Degenerative Disorders

On this page
🧬 The Cartilage Catastrophe: Molecular Foundations of Joint Failure
Osteoarthritis emerges not from passive wear-and-tear but from active biological failure of the entire joint organ. The articular cartilage-a 2-4 mm thick avascular tissue composed of 70% water, 20% type II collagen, and 10% proteoglycans-loses its biomechanical resilience through a cascade of enzymatic destruction and failed repair.

The Proteoglycan Collapse
Healthy cartilage maintains a fixed charge density of 150-300 mEq/L through aggrecan molecules, creating osmotic swelling pressure that resists compression. In early OA, aggrecanases (ADAMTS-4 and ADAMTS-5) cleave aggrecan at specific sites, reducing proteoglycan content by 30-50% within the superficial zone. This loss decreases the tissue's aggregate modulus from 0.5-0.9 MPa to <0.2 MPa, rendering cartilage vulnerable to mechanical injury.
📌 Remember: ADAM Destroys Cartilage - ADAMTS-4 and ADAMTS-5, Degrade Aggrecan, causing Mechanical failure through proteoglycan depletion and osmotic pressure loss.
- Collagen Network Disruption
- Type II collagen provides tensile strength (5-25 MPa)
- Matrix metalloproteinases (MMP-1, MMP-13) cleave collagen triple helix
- Collagenase activity increases 5-10 fold in OA cartilage
- Fibrillation begins at superficial zone, propagating to deep zones
- Vertical clefts extend perpendicular to surface
- Horizontal cleavage creates delamination
- Full-thickness defects expose subchondral bone
⭐ Clinical Pearl: 50% of patients with cartilage fibrillation visible on MRI progress to full-thickness defects within 3 years, making early detection critical for disease-modifying interventions.
The Inflammatory Amplification Loop
Damaged cartilage releases matrix fragments (fibronectin, collagen fragments) that activate synovial macrophages through toll-like receptors (TLR-2, TLR-4). These cells produce interleukin-1β (IL-1β) and tumor necrosis factor-α (TNF-α), which upregulate chondrocyte production of MMPs and aggrecanases while suppressing collagen and proteoglycan synthesis.
💡 Master This: The self-perpetuating inflammatory cycle-where mechanical damage triggers cytokine release, which amplifies matrix destruction-explains why 70% of OA patients experience intermittent synovitis and why anti-inflammatory strategies provide only temporary relief without addressing the underlying catabolic drive.
| Mediator | Source | Primary Action | Fold Increase in OA | Clinical Correlation |
|---|---|---|---|---|
| IL-1β | Synovial macrophages, chondrocytes | ↑ MMP-1, MMP-13, ADAMTS-5 | 10-50× | Synovial fluid levels correlate with pain severity |
| TNF-α | Synovial macrophages | ↑ MMP expression, ↓ collagen synthesis | 5-20× | Elevated in erosive OA subtypes |
| IL-6 | Chondrocytes, synovium | ↑ VEGF, osteophyte formation | 3-10× | Predicts radiographic progression |
| PGE₂ | Chondrocytes (via COX-2) | ↑ Pain sensitization, ↑ MMP | 5-15× | Target of NSAID therapy |
| Nitric oxide | Chondrocytes (via iNOS) | ↓ Proteoglycan synthesis, chondrocyte apoptosis | 10-100× | Marker of cartilage catabolism |
Subchondral Bone Remodeling
The subchondral bone plate-normally 0.2-1.0 mm thick-thickens to >2 mm in advanced OA through increased osteoblast activity driven by transforming growth factor-β (TGF-β) released from degraded cartilage. This sclerosis reduces the bone's shock-absorbing capacity, increasing peak cartilage stress by 15-30% and accelerating surface damage.
- Bone Marrow Lesions (BMLs)
- Visualized as high signal on T2-weighted MRI
- Represent microfractures, edema, fibrosis, necrosis
- Present in 60-80% of symptomatic knee OA
- Size correlates with pain severity (r = 0.45-0.65)
- BMLs >1 cm² predict 3-fold higher risk of cartilage loss
- Dynamic lesions fluctuate with mechanical loading
- Persistent BMLs indicate ongoing structural damage
⭐ Clinical Pearl: Patients with large BMLs (>2 cm²) experience 40% greater pain than those with similar cartilage loss but no BMLs, explaining why radiographic severity poorly predicts symptoms in 30-40% of cases.
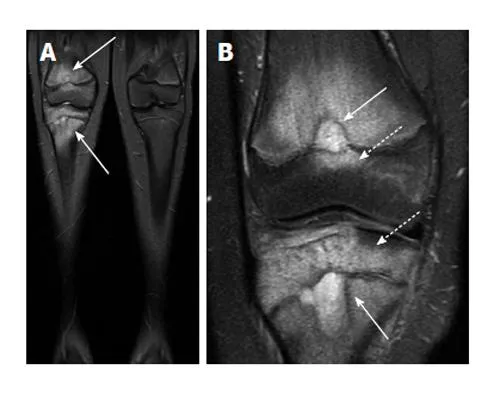
Osteophyte Formation
Marginal osteophytes develop through endochondral ossification at the joint periphery, where synovium meets periosteum. TGF-β and bone morphogenetic proteins (BMPs) induce mesenchymal stem cells to differentiate into chondrocytes, forming cartilaginous outgrowths that subsequently ossify. While historically considered compensatory, osteophytes contribute to joint stiffness and may impinge on surrounding structures.
📌 Remember: BONE Spurs Grow - BMPs and TGF-beta drive Osteophyte formation through eNdochondral ossification at joint Edges, creating Spurs that Progressively limit Uniform joint motion and cause Restricted range and Grating pain.
Connect these molecular mechanisms through to understand how therapeutic targets emerge from understanding the catabolic cascade.
🧬 The Cartilage Catastrophe: Molecular Foundations of Joint Failure
🎯 Pattern Recognition Arsenal: Clinical Phenotypes and Diagnostic Frameworks
Osteoarthritis manifests through distinct clinical patterns that guide diagnosis and predict progression. Recognizing these phenotypes-from mechanical knee pain in obese patients to inflammatory erosive hand OA-enables targeted management and prognostication.
The Mechanical Pain Pattern
OA pain follows a characteristic temporal pattern: worsening with activity, improving with rest, morning stiffness <30 minutes, and end-of-day exacerbation. This contrasts sharply with inflammatory arthritis (morning stiffness >60 minutes, improvement with activity). The pain originates not from cartilage (which lacks nociceptors) but from:
-
Periosteal Irritation
- Osteophyte traction on periosteum
- Subchondral microfractures
- Bone marrow lesion-associated edema
- Accounts for 40-50% of OA pain intensity
-
Synovial Inflammation
- Intermittent synovitis in 50-70% of patients
- Effusion distends joint capsule (pain threshold: 20-30 mL in knee)
- Inflammatory mediators sensitize nociceptors
- Explains episodic pain flares superimposed on chronic ache
-
Capsular and Ligamentous Strain
- Joint instability from cartilage loss and ligament laxity
- Abnormal loading patterns stress capsular attachments
- Muscle spasm attempts to stabilize joint
- Contributes to "giving way" sensation in 30-40% of knee OA
💡 Master This: The "use-related pain with rest relief" pattern has 85% sensitivity and 90% specificity for OA when combined with age >50 years and morning stiffness <30 minutes, allowing clinical diagnosis without imaging in most cases.
Joint-Specific Clinical Signatures
| Joint | Key Symptom | Classic Sign | Functional Impact | Prevalence in OA | Progression Rate |
|---|---|---|---|---|---|
| Knee | Stair-climbing pain | Crepitus, effusion, varus/valgus deformity | Walking distance ↓ 50% | 40-50% symptomatic >60 yr | 4-6%/yr cartilage loss |
| Hip | Groin pain radiating to knee | Restricted internal rotation (<15°) | Difficulty with shoes/socks | 10-15% symptomatic >60 yr | 2-3%/yr joint space narrowing |
| Hand | DIP/PIP swelling | Heberden's/Bouchard's nodes, squaring of thumb base | Grip strength ↓ 30-40% | 60-70% radiographic >65 yr | 10-15% develop erosive subtype |
| Spine | Axial pain, radiculopathy | Paraspinal tenderness, reduced flexion | Spinal stenosis in 30% | 80-90% radiographic >65 yr | 5-10%/yr disc height loss |
| Shoulder | Night pain, overhead limitation | Painful arc 60-120°, AC joint tenderness | Difficulty with hair/back | 5-10% symptomatic >60 yr | Variable, often post-traumatic |
⭐ Clinical Pearl: Groin pain is the hallmark of hip OA-present in 90% of cases-while lateral hip or buttock pain suggests trochanteric bursitis or lumbar radiculopathy. Always assess hip internal rotation; <15° predicts radiographic OA with 95% specificity.

The Kellgren-Lawrence Grading System
This radiographic classification remains the standard for OA severity assessment, correlating with symptoms and guiding surgical timing:
-
Grade 0: Normal
- No radiographic features of OA
- Joint space >3 mm in knee, >4 mm in hip
-
Grade 1: Doubtful
- Minute osteophytes, doubtful significance
- 10-15% progress to symptomatic OA over 10 years
-
Grade 2: Mild
- Definite osteophytes, possible joint space narrowing
- Joint space 2-3 mm in knee
- 30-40% symptomatic at this stage
- Conservative management typically successful
- 20-25% progress to Grade 3 within 5 years
-
Grade 3: Moderate
- Moderate joint space narrowing (1-2 mm)
- Multiple osteophytes, subchondral sclerosis
- 60-70% experience significant symptoms
- Surgical consideration in younger, active patients
- 40-50% progress to Grade 4 within 5 years
-
Grade 4: Severe
- Marked joint space narrowing (<1 mm or bone-on-bone)
- Large osteophytes, severe sclerosis, deformity
- >90% have severe symptoms limiting function
- Arthroplasty typically indicated
📌 Remember: K-L Grades Build Pain - K-L Grade 1 = minute osteophytes (Little concern), Grade 2 = Bigger spurs with space narrowing (conservative care), Grade 3 = severe Pain with moderate narrowing (surgery considered), Grade 4 = bone-on-bone (Arthroplasty time), Grade 5 = doesn't exist (Ignore if listed), Grade 6+ = Nonsense.
Advanced Imaging Modalities
While plain radiographs suffice for most OA diagnosis, advanced imaging reveals early changes and guides interventional therapies:
-
MRI Assessment
- Detects cartilage loss 2-3 years before radiographic changes
- Quantifies cartilage thickness (normal knee: 2.0-2.5 mm)
- Identifies bone marrow lesions, meniscal tears, ligament injury
- WORMS (Whole-Organ MRI Score) predicts progression
- Score >20 indicates 3-fold higher risk of arthroplasty within 5 years
-
Ultrasound Utility
- Detects effusions as small as 5 mL (vs 20 mL clinically)
- Assesses synovial hypertrophy (>4 mm suggests inflammation)
- Guides intra-articular injections with 90% accuracy vs 70% blind
- Evaluates osteophytes and cartilage surface irregularities
⭐ Clinical Pearl: MRI is not routinely indicated for OA diagnosis but becomes essential when considering joint-preserving surgery (osteotomy, cartilage repair) or when symptoms seem disproportionate to radiographic findings-situations occurring in 15-20% of cases.

Explore joint-specific presentations through , , , and for detailed pattern recognition frameworks.
🎯 Pattern Recognition Arsenal: Clinical Phenotypes and Diagnostic Frameworks
🛡️ The Conservative Arsenal: Non-Surgical Management Strategies
Conservative management forms the foundation of OA treatment, achieving 50-70% symptom control in mild-to-moderate disease and delaying arthroplasty by 5-10 years when implemented systematically. The approach combines mechanical unloading, pharmacological pain control, and functional restoration.
Weight Reduction: The Most Potent Intervention
Every kilogram of weight loss reduces knee joint load by 4 kg during walking due to ground reaction forces. A 5% body weight reduction (e.g., 5 kg in a 100 kg patient) decreases knee OA pain by 20-30% and improves function scores by 15-25% within 3-6 months.
💡 Master This: Weight loss represents the only intervention that simultaneously reduces pain, slows structural progression (demonstrated by 30% less cartilage loss over 4 years in patients losing >10% body weight), and improves cardiovascular comorbidities affecting 60-70% of OA patients.
- Mechanical Unloading Strategies
- Knee bracing: Valgus-directing brace reduces medial compartment load by 10-15%
- Effective in mild-moderate medial OA (KL Grade 2-3)
- Improves pain in 60-70% of compliant users
- Requires 6-8 hours/day wear for benefit
- Lateral wedge insoles: Shift load from medial to lateral compartment
- 5-10° wedge reduces medial load by 5-8%
- Benefit modest; 30-40% report improvement
- Best in varus alignment <5°
- Walking aids: Cane in contralateral hand reduces hip load by 20-30%
- Underutilized; only 15-20% of eligible patients use
- Proper height: wrist crease level with arm relaxed
- Immediate pain reduction in 70-80% of users
- Knee bracing: Valgus-directing brace reduces medial compartment load by 10-15%
Exercise: The Analgesic Without Side Effects
Structured exercise programs reduce OA pain by 40-50% and improve function by 30-40%-effects comparable to NSAIDs but sustained long-term. The mechanism involves muscle strengthening (reducing joint stress), proprioception enhancement (improving stability), and endorphin release (modulating pain perception).
| Exercise Type | Primary Benefit | Frequency | Pain Reduction | Function Improvement | Adherence Rate |
|---|---|---|---|---|---|
| Resistance training | Quadriceps strength ↑ 30-50% | 3×/week, 8-12 reps | 30-40% | 25-35% | 60-70% at 6 months |
| Aerobic (walking, cycling) | Cardiovascular fitness, weight control | 5×/week, 30 min | 25-35% | 20-30% | 50-60% at 6 months |
| Aquatic therapy | Reduced joint loading, improved ROM | 2-3×/week, 45 min | 35-45% | 30-40% | 70-80% at 6 months |
| Tai Chi | Balance, proprioception, mental health | 2-3×/week, 60 min | 30-40% | 25-35% | 65-75% at 6 months |
| Yoga | Flexibility, strength, stress reduction | 2-3×/week, 60 min | 25-35% | 20-30% | 55-65% at 6 months |
📌 Remember: WATER Exercises Win - Weight-bearing reduced through buoyancy, Aerobic conditioning improved, Temperature warmth soothes joints, Endurance built without impact, Range of motion enhanced-making aquatic therapy ideal for moderate-severe OA with 70-80% adherence.
Pharmacological Pain Management Ladder
OA pharmacotherapy follows a stepwise approach balancing efficacy, safety, and cost:
-
Step 1: Topical NSAIDs and Acetaminophen
- First-line for mild-moderate OA per all guidelines
- Topical diclofenac gel: 30-40% pain reduction, minimal systemic absorption
- Apply 4 g to knee 4×/day
- Effective in 50-60% of patients
- GI/renal risk <5% (vs 20-30% oral NSAIDs)
- Acetaminophen: 1000 mg TID-QID (max 4000 mg/day)
- Pain reduction 15-25% (less than NSAIDs)
- Hepatotoxicity risk with chronic use, alcohol
- Consider in patients with NSAID contraindications
-
Step 2: Oral NSAIDs
- Reserve for inadequate response to topicals
- Ibuprofen 400-800 mg TID, naproxen 500 mg BID, celecoxib 200 mg daily
- Pain reduction 40-50% in 60-70% of patients
- GI bleeding risk 2-4%/year (↑ with age >65, prior ulcer)
- Cardiovascular risk: 20-30% ↑ with all NSAIDs except naproxen
- Renal impairment in 10-15% of elderly patients
- Always co-prescribe PPI in high-risk patients (age >65, prior GI bleed, anticoagulation)
⭐ Clinical Pearl: Topical NSAIDs provide 80-90% of the efficacy of oral NSAIDs for knee OA with <10% of systemic side effects, yet are prescribed in only 20-30% of eligible patients-a major opportunity for safer pain management.
- Step 3: Intra-Articular Injections
- Corticosteroids: Triamcinolone 40 mg or methylprednisolone 40-80 mg
- Rapid onset (24-48 hours), peak effect 1-2 weeks
- Duration 4-12 weeks in 60-70% of patients
- Limit to 3-4 injections/year (cartilage toxicity concern)
- Best for acute flares with effusion
- Hyaluronic acid: 3-5 weekly injections of various molecular weights
- Delayed onset (2-4 weeks), duration 3-6 months
- Modest effect size (20-30% pain reduction)
- Controversial efficacy; 40-50% placebo response
- Consider in corticosteroid non-responders
- Corticosteroids: Triamcinolone 40 mg or methylprednisolone 40-80 mg
💡 Master This: Corticosteroid injections provide superior short-term relief (50-60% pain reduction at 4 weeks) compared to hyaluronic acid (30-40% at 4 weeks), but HA may offer longer duration (3-6 months vs 6-12 weeks)-making steroids ideal for acute flares and HA for sustained relief in selected patients.
Nutraceuticals: Evidence and Expectations
Glucosamine and chondroitin sulfate remain popular despite conflicting evidence. Meta-analyses show small-to-moderate pain reduction (10-20%) with high heterogeneity. The GAIT trial (Glucosamine/Chondroitin Arthritis Intervention Trial) found no benefit in the overall population but possible benefit in moderate-severe OA subgroup (60-70% response vs 50% placebo).
- Dosing: Glucosamine sulfate 1500 mg/day, chondroitin sulfate 800-1200 mg/day
- Onset: 2-3 months for maximum effect
- Safety: Excellent; GI upset in 5-10%, rare allergic reactions
- Cost-effectiveness: Questionable given modest benefits
⭐ Clinical Pearl: Recommend 3-month trial of glucosamine/chondroitin for motivated patients with mild-moderate OA; if no benefit, discontinue. Avoid in shellfish allergy (glucosamine source) and monitor glucose in diabetics (theoretical concern, rarely significant).
Detailed conservative strategies are explored in , , and .
🛡️ The Conservative Arsenal: Non-Surgical Management Strategies
⚙️ Rehabilitation Mastery: Functional Restoration and Disability Prevention
Rehabilitation transforms OA management from passive symptom control to active functional optimization. Structured programs reduce pain by 30-50%, improve physical function by 30-40%, and delay arthroplasty by 5-10 years through neuromuscular re-education, strengthening, and biomechanical correction.
The Quadriceps Paradox
Quadriceps weakness develops early in knee OA-20-40% strength deficit even in mild disease-creating a vicious cycle: weakness → increased joint stress → cartilage damage → pain → disuse → further weakness. Breaking this cycle requires targeted strengthening.
- Quadriceps Strengthening Protocol
- Isometric exercises: Quad sets, straight leg raises
- Safe in acute pain; no joint motion
- Hold 5-10 seconds, 10-15 reps, 3 sets/day
- Strength gain 15-25% in 6-8 weeks
- Isotonic exercises: Leg extensions, squats (0-60° only)
- Progress when isometric pain-free
- 8-12 reps, 3 sets, 3×/week
- Strength gain 30-50% in 12 weeks
- Functional exercises: Step-ups, sit-to-stand
- Mimics daily activities
- Improves proprioception and balance
- Reduces fall risk by 30-40% in elderly
- Isometric exercises: Quad sets, straight leg raises
💡 Master This: Every 10% increase in quadriceps strength reduces knee OA pain by 10-15% and improves function by 10-12%-a dose-response relationship that makes strengthening the most evidence-based rehabilitation intervention with NNT of 4-5 for clinically meaningful improvement.
| Rehabilitation Modality | Mechanism | Pain Reduction | Function Improvement | Evidence Quality | Cost |
|---|---|---|---|---|---|
| Therapeutic exercise | Muscle strengthening, proprioception | 30-50% | 30-40% | High (multiple RCTs) | Low |
| Manual therapy | Joint mobilization, soft tissue release | 20-30% | 15-25% | Moderate | Medium |
| TENS (Transcutaneous Electrical Nerve Stimulation) | Gate control theory, endorphin release | 15-25% | 10-15% | Low-Moderate | Low |
| Ultrasound therapy | Deep heat, tissue extensibility | 10-20% | 5-15% | Low | Medium |
| Pulsed electromagnetic fields | Chondrocyte metabolism, anti-inflammatory | 15-25% | 10-20% | Moderate | High |
| Acupuncture | Neuromodulation, placebo | 20-30% | 15-20% | Moderate | Medium |
Gait Retraining and Biomechanical Optimization
Abnormal gait patterns in OA increase joint loading and accelerate cartilage loss. The knee adduction moment (KAM)-a surrogate for medial compartment load-is 20-40% higher in medial knee OA and predicts progression.
- Gait Modification Strategies
- Toe-out gait: Increase foot progression angle by 5-10°
- Reduces KAM by 5-10%
- Simple, no equipment required
- Effective in 50-60% of patients
- Trunk sway: Lateral trunk lean over affected limb
- Reduces KAM by 10-15%
- Requires practice; 4-6 weeks to automate
- May increase hip/back stress
- Walking poles: Nordic walking technique
- Reduces knee load by 15-20%
- Improves cardiovascular fitness
- Enhances balance and confidence
- Toe-out gait: Increase foot progression angle by 5-10°
📌 Remember: GAIT Changes Help - Gait retraining reduces joint load, Abnormal patterns accelerate damage, Increase toe-out angle 5-10°, Trunk sway over affected side reduces stress, Consistent practice needed 4-6 weeks, Helps 50-60% of patients, Effect size 10-15% load reduction, Long-term adherence challenging, Poles (walking) add stability.
Proprioception and Balance Training
Proprioceptive deficits occur in 60-80% of knee OA patients, impairing joint position sense and neuromuscular control. This increases fall risk (2-3 fold higher than age-matched controls) and contributes to "giving way" episodes.
- Proprioceptive Training Components
- Single-leg stance: Progress from eyes open to eyes closed
- Goal: 30 seconds stable without support
- Improves balance confidence by 30-40%
- Wobble board exercises: Multidirectional perturbations
- Enhances dynamic stability
- 10-15 minutes, 3×/week for 8-12 weeks
- Perturbation training: Unexpected pushes/pulls
- Trains reactive balance strategies
- Reduces fall risk by 40-50%
- Single-leg stance: Progress from eyes open to eyes closed
⭐ Clinical Pearl: Combining strengthening with proprioceptive training provides additive benefits-60-70% improvement in function vs 40-50% with strengthening alone-because OA impairs both muscle force production and neuromuscular control, requiring dual-targeted rehabilitation.

The Rehabilitation Prescription
A comprehensive OA rehabilitation program integrates multiple modalities:
-
Phase 1 (Weeks 1-4): Pain Control and ROM
- Modalities: Ice, TENS, gentle ROM exercises
- Goals: Reduce pain 30-40%, achieve full passive ROM
- Frequency: Daily home program, 2×/week supervised
-
Phase 2 (Weeks 5-12): Strengthening and Endurance
- Isometric → isotonic → functional exercises
- Aerobic conditioning: 30 minutes, 5×/week
- Goals: 30-50% strength gain, 20-30% endurance improvement
- Frequency: 3×/week supervised, daily home program
-
Phase 3 (Weeks 13+): Maintenance and Progression
- Advanced functional exercises, sport-specific training
- Gait retraining, proprioception drills
- Goals: Return to desired activities, prevent progression
- Frequency: 2-3×/week independent, periodic reassessment
💡 Master This: Rehabilitation success requires minimum 12 weeks of consistent participation-60-70% of benefits accrue by 8-10 weeks, but long-term adherence (>6 months) is achieved in only 30-40% of patients, making behavioral strategies (goal-setting, self-monitoring, group classes) as important as exercise prescription.
Explore comprehensive rehabilitation frameworks in for detailed protocols and outcome measures.
⚙️ Rehabilitation Mastery: Functional Restoration and Disability Prevention
🔬 Surgical Decision-Making: When Conservative Measures Fail
Surgical intervention becomes necessary when conservative management fails to maintain acceptable quality of life despite 6-12 months of optimal non-operative treatment. The decision balances symptom severity, functional limitation, radiographic findings, patient expectations, and surgical risk.
Indications for Surgical Referral
Absolute Indications (surgery strongly recommended):
- Severe pain (VAS >7/10) despite maximal medical management
- Significant functional limitation (unable to walk >2-3 blocks, difficulty with ADLs)
- Radiographic severity (KL Grade 4, bone-on-bone)
- Failed conservative therapy >6-12 months
- Progressive deformity affecting adjacent joints
Relative Indications (consider surgery in appropriate candidates):
- Moderate pain (VAS 5-7/10) with activity-limiting symptoms
- Younger age (<60 years) with focal cartilage defects amenable to joint preservation
- Mechanical symptoms (locking, catching) from loose bodies or meniscal tears
- Psychological impact (depression, social withdrawal) from pain/disability
⭐ Clinical Pearl: The "night pain" criterion-pain severe enough to wake patient from sleep and requiring >2 analgesic doses/night-predicts 80-90% satisfaction with arthroplasty and should lower the threshold for surgical referral even in moderate radiographic disease.
The Joint Preservation vs. Replacement Decision
Patient age, activity level, and disease pattern determine whether joint-preserving procedures or arthroplasty is appropriate:
| Procedure | Ideal Candidate | Contraindications | Success Rate | Durability | Return to Activity |
|---|---|---|---|---|---|
| High Tibial Osteotomy | Age <60, active, isolated medial OA, varus <15° | KL Grade 4, inflammatory arthritis, obesity (BMI >35) | 70-80% good-excellent | 10-year survival 65-75% | High-impact sports 60-70% |
| Unicompartmental Knee Arthroplasty | Age >60, isolated medial/lateral OA, intact ACL | Inflammatory arthritis, fixed deformity >15°, patellofemoral OA | 85-90% good-excellent | 10-year survival 85-90% | Low-impact activities 80-90% |
| Total Knee Arthroplasty | Age >60, tricompartmental OA, any severity | Active infection, extensor mechanism dysfunction | 90-95% good-excellent | 15-year survival 90-95% | Low-impact activities 90-95% |
| Hip Resurfacing | Age <60, male, good bone quality, large femoral head | Osteoporosis, cysts >1 cm, renal disease | 85-90% good-excellent | 10-year survival 85-90% | High-impact sports 70-80% |
| Total Hip Arthroplasty | Age >60, any severity hip OA | Active infection, abductor insufficiency | 95-98% good-excellent | 20-year survival 85-90% | Low-impact activities 95-98% |
📌 Remember: OSTEOTOMY Saves Joints - Older than 60? Consider replacement; younger? Salvage possible, Tibial osteotomy for varus knee, Excellent for active patients, Only works in isolated compartment OA, Time-limited (10-15 years), Obesity (BMI >35) = contraindication, Mechanical axis correction key, Young males ideal candidates.
Arthroscopic Debridement: The Discredited Procedure
Landmark trials (Moseley 2002, Kirkley 2008) demonstrated arthroscopic debridement and lavage for knee OA provide no benefit beyond placebo/sham surgery. Current guidelines strongly recommend against arthroscopic surgery for OA without mechanical symptoms (true locking from loose bodies, displaced meniscal tears).
- Appropriate Arthroscopic Indications
- Mechanical locking (not pseudo-locking from pain/stiffness)
- Loose body removal in young patients with focal defects
- Meniscal repair (not debridement) in salvageable tears
- Diagnostic arthroscopy when diagnosis uncertain
⭐ Clinical Pearl: Despite strong evidence against benefit, arthroscopic debridement for OA remains overutilized in 20-30% of eligible patients-a $3 billion/year expenditure in the US alone. Educating patients about lack of efficacy and potential harm (10-15% complication rate) is essential.
Arthroplasty Outcomes and Patient Selection
Total joint arthroplasty ranks among the most successful surgical interventions, with 90-95% patient satisfaction and dramatic improvements in pain and function. However, 5-10% experience persistent pain or dissatisfaction, often related to inappropriate patient selection.
- Predictors of Poor Arthroplasty Outcome
- Psychological factors: Depression, anxiety, catastrophizing
- Present in 20-30% of TKA candidates
- 2-3 fold higher risk of persistent pain
- Screen with PHQ-9, GAD-7 before surgery
- Unrealistic expectations: Expecting 100% pain relief, return to high-impact sports
- 15-20% of patients have unrealistic expectations
- Preoperative counseling reduces dissatisfaction by 30-40%
- Mild radiographic disease: KL Grade 2-3 with disproportionate symptoms
- 30-40% dissatisfaction rate (vs 5-10% in Grade 4)
- Consider alternative diagnoses before surgery
- Young age: <50 years at time of TKA
- Higher revision rates (15-20% at 10 years vs 5-8% in older patients)
- Consider joint preservation when possible
- Psychological factors: Depression, anxiety, catastrophizing
💡 Master This: The "triple threat" of depression, obesity (BMI >40), and unrealistic expectations predicts 60-70% risk of dissatisfaction after TKA-10-fold higher than patients without these factors-making preoperative optimization and psychological screening as important as surgical technique.








