Image-Guided Surgery - Guiding the Cut
- Goal: Uses patient-specific image data (CT, MRI) to guide surgical instruments in real-time, enhancing precision and safety. "Surgical GPS."
- Key Steps (Workflow):
- Imaging: Pre-operative scans (CT, MRI) create a 3D anatomical model.
- Registration: Crucial step; aligns the virtual image model to the actual patient's anatomy on the operating table.
- Tracking: Monitors instruments and patient anatomy using optical (reflective markers) or electromagnetic systems.
- Navigation: Software displays tracked instruments overlaid on the patient's images, guiding the surgeon.
- Benefits: ↑ Accuracy, ↓ invasiveness, ↓ radiation exposure (to staff), potentially improved outcomes.

⭐ Accurate registration is paramount; errors at this stage directly compromise surgical precision and patient safety.
Image-Guided Surgery - The Surgeon's GPS
Image-Guided Surgery (IGS) acts like a GPS for surgeons, enhancing precision by providing real-time, 3D visualization of patient anatomy and instrument position relative to it.
- Core Components:
- Hardware:
- Imaging Modalities:
- Pre-operative: CT, MRI (create detailed 3D patient model).
- Intra-operative: Fluoroscopy (C-arm), O-arm, intra-op CT/MRI (provide real-time anatomical updates).
- Tracking Systems: Monitor instrument and patient position.
- Optical Trackers: Use infrared cameras & passive/active reflective markers (require clear line-of-sight).
- Electromagnetic (EM) Trackers: Use EM fields & sensor coils (no line-of-sight issues; potential metal interference).
- Computer Workstation & Display: Processes data, displays navigation views.
- Tracked Instruments: Surgical tools with attached markers or sensors.
- Imaging Modalities:
- Software:
- Image Processing & Segmentation: Defining anatomical structures from image data.
- Registration: Aligning pre-operative images with the patient's intra-operative anatomy (the crucial link).
- Navigation & Visualization Interface: Displays instrument trajectory overlaid on patient images.
- Hardware:
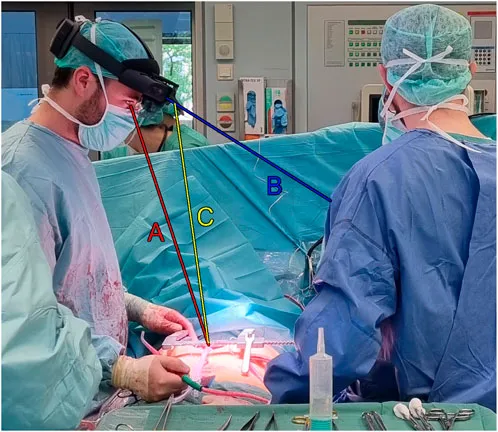
⭐ IGS systems aim for sub-millimetric accuracy, often achieving precision within 1-2 mm, crucial for procedures like pedicle screw placement or joint replacement component alignment, thereby reducing complications and improving outcomes.
Image-Guided Surgery - Precision Ortho Ops
Image-Guided Surgery (IGS) utilizes computer systems to track surgical instruments in real-time relative to patient anatomy, enhancing operative precision.
IGS Workflow:
Core Components:
- Imaging: CT, MRI, Fluoroscopy
- Tracking Systems: Optical (infrared cameras), Electromagnetic (EM)
- Software: Planning & real-time navigation interface
- Tracked surgical instruments
Key Orthopaedic Applications:
- Joint Arthroplasty (TKA, THA): Component alignment, sizing, leg length restoration.
- Spine Surgery: Pedicle screw placement, osteotomies, decompression.
- Trauma: Fracture reduction, complex intra-articular fixation.
- Tumor Resection: Precise margin definition.

Advantages:
- ↑ Accuracy & precision in implant placement
- ↓ Component malalignment & outliers
- Potential for improved long-term outcomes
- Facilitates Minimally Invasive Surgery (MIS)
Disadvantages:
- ↑ Initial cost & operative time
- Radiation exposure (with CT/fluoroscopy-based systems)
- Steep learning curve
- Potential for registration inaccuracies
⭐ IGS significantly improves acetabular cup placement accuracy in Total Hip Arthroplasty (THA), aiming for optimal inclination (e.g., 40°±10°) and anteversion (e.g., 15°±10°) to reduce dislocation risk (Lewinnek's safe zone).
Image-Guided Surgery - Hurdles & Horizons
- Hurdles
- Accuracy: Registration errors, soft-tissue shift (brain shift).
- Cost: High capital investment, maintenance.
- Learning Curve: Steep for surgical team.
- Radiation: Patient/staff exposure (CT/fluoro).
- Workflow: Integration issues, potential OR time ↑.
- Horizons
- AI & Robotics: Automated planning, precision.
- AR/VR: Intuitive overlays, 3D visualization.
- Radiation-free imaging: Advanced US, iMRI.
⭐ Major Limitation: Intraoperative "brain shift" or tissue deformation compromises IGS accuracy.
High‑Yield Points - ⚡ Biggest Takeaways
- IGS employs preoperative (CT/MRI) or intraoperative (fluoroscopy) imaging for precise surgical navigation.
- Significantly improves accuracy in implant placement (e.g., TKR, THR, pedicle screws).
- Relies on patient-to-image registration as a critical step for aligning data.
- Utilizes tracking systems (optical or electromagnetic) to monitor instrument position.
- Reduces component malalignment and improves functional outcomes in arthroplasty.
- Considerations include ↑ operative time, learning curve, and potential radiation exposure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

