Introduction & Principles - Print Perfect Bones
3D printing, or Additive Manufacturing (AM), creates patient-specific orthopaedic implants and surgical guides from digital models (CT/MRI scans). This allows for complex geometries, aiming for reduced OR time and improved surgical accuracy.
- Process: Layer-by-layer material deposition (e.g., SLS, FDM, DMLS).
- Input: CT/MRI data converted to STL (Standard Tessellation Language) files.
- Design: Using CAD (Computer-Aided Design) software.
- Benefits: High patient-specificity, fabrication of intricate structures, potential for ↓OR time & ↑accuracy.
⭐ STL (Standard Tessellation Language) is the most common file format used to convert 3D CAD models into data for 3D printers.
Materials & Anatomical Models - Crafty Cartilage Creators
- Key 3D Printing Materials:
- Metals: Titanium alloys (e.g., Ti6Al4V - strong, biocompatible), Co-Cr alloys (wear-resistant for joints).
- Polymers: PEEK (bone-like modulus, radiolucent for cages), PLA (biodegradable scaffolds).
- Ceramics: Hydroxyapatite (HA - osteoconductive, for implant coatings).
- Bio-inks: Hydrogels with cells for tissue engineering (e.g., cartilage).
- Anatomical Models:
- Patient-specific physical replicas from CT/MRI data.
- Uses: Surgical planning, procedure simulation, education, patient communication.

⭐ Titanium alloys, particularly Ti6Al4V, are extensively used for 3D-printed orthopaedic implants due to their excellent biocompatibility, corrosion resistance, and mechanical strength similar to bone.
Patient-Specific Solutions - Custom Cut Cures
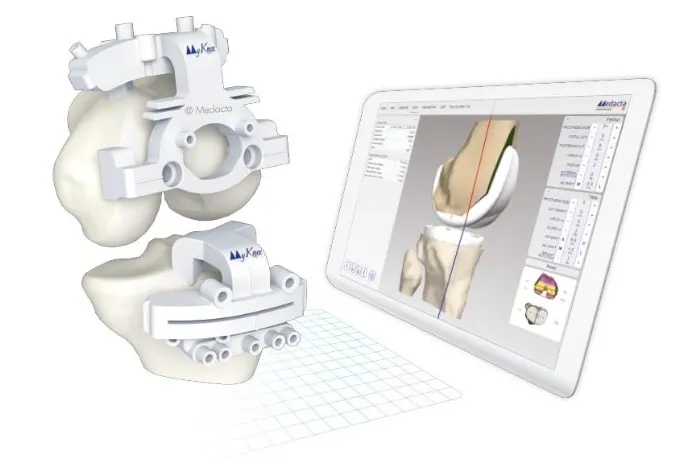
- Patient-Specific Instruments (PSIs): Custom-made surgical guides, 3D printed from patient's CT/MRI scans.
- Key Applications:
- Total Knee Arthroplasty (TKA): For precise femoral & tibial cuts.
- Total Hip Arthroplasty (THA): Aids acetabular cup & femoral stem positioning.
- Spine Surgery: Improves accuracy of pedicle screw placement.
- Advantages: ↑Surgical precision, potentially ↓operative time, ↓instrument trays.
- Key Applications:
- Custom Implants: Individually designed implants for complex anatomical challenges.
- Trauma:
- Complex fractures: e.g., comminuted articular fractures, malunions.
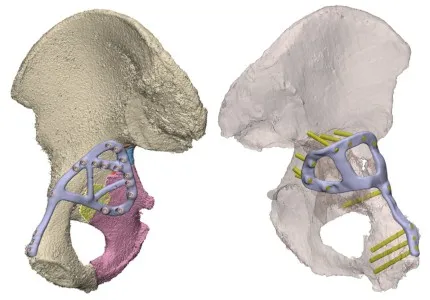
- Pelvic & acetabular reconstruction: For intricate defects.
- Oncology:
- Tumor resection & reconstruction: e.g., limb salvage with custom megaprostheses after bone sarcoma.
- Arthroplasty:
- Custom acetabular components: For significant bone loss or deformity (e.g., Paprosky type III defects, protrusio acetabuli).
- Revision components: Addressing failed previous arthroplasty.
- Osteotomies:
- Patient-specific cutting jigs for accurate deformity correction (e.g., high tibial osteotomy, femoral osteotomy).
- Trauma:
⭐ 3D-printed patient-specific implants are particularly valuable in complex oncological reconstructions and revision arthroplasty where standard implants may not suffice.
Challenges & Innovations - Printing New Paths
- Current Hurdles (Limitations):
- High costs & manufacturing time.
- Steep learning curve for surgeons.
- Rigorous regulatory approval.
- Material biocompatibility/strength constraints.
- Limited long-term clinical data.
- Future Horizons (Innovations):
- Bioprinting: Tissue scaffolds with cells, growth factors.
- 4D Printing: Implants adapting shape/function over time.
- Point-of-Care (POC) Manufacturing: On-site implant creation.

⭐ While promising, bioprinting of functional tissues for orthopaedic applications faces significant hurdles, including achieving adequate vascularization and long-term cell viability.
High‑Yield Points - ⚡ Biggest Takeaways
- Patient-Specific Implants (PSIs) offer superior fit and osseointegration.
- 3D-printed surgical guides boost accuracy in osteotomies and implant placement.
- Anatomical models are vital for pre-op planning in complex cases.
- Common materials: Titanium alloys, PEEK, and bioabsorbable polymers.
- Key benefits: Reduced OR time, improved precision, and better patient outcomes.
- Widely used in complex trauma, arthroplasty, spine, and orthopaedic oncology.
- Facilitates custom porous designs for enhanced bone ingrowth.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

