Muscle Fundamentals - Mighty Machines
- Muscle Fiber (Cell): Basic structural unit; multinucleated. Contains myofibrils.
- Myofibril: Composed of repeating sarcomeres, the functional contractile units.
- Sarcomere: Z-disc to Z-disc.
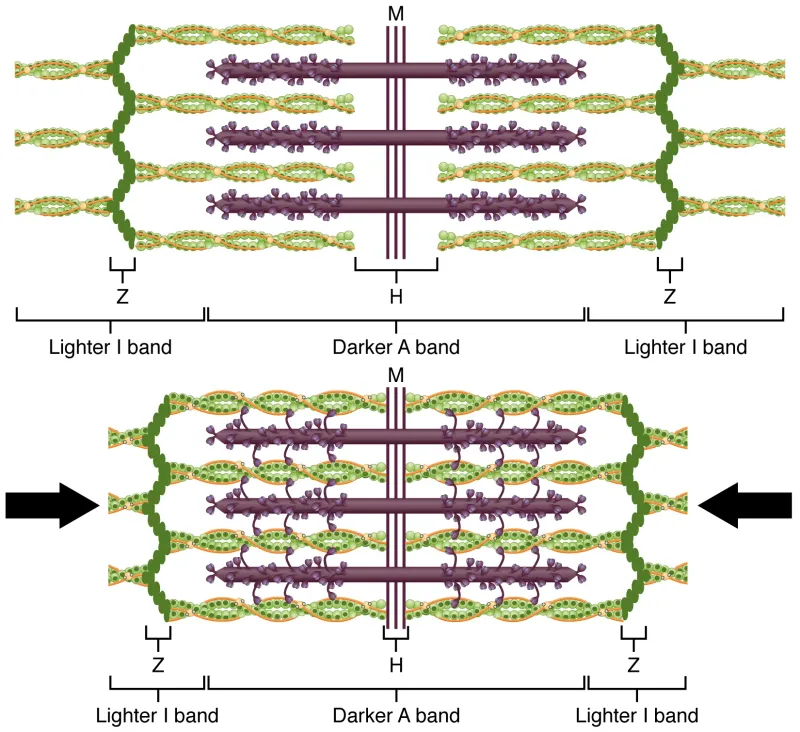
- A-band: Anisotropic (dArk); contains Myosin ± Actin. Length constant during contraction.
- I-band: Isotropic (lIght); Actin only. Shortens during contraction.
- H-zone: Myosin only. Shortens during contraction.
- M-line: Midpoint of sarcomere; anchors Myosin. and thin (actin) filaments, titin, and nebulin)
- Sarcomere: Z-disc to Z-disc.
- Motor Unit: A single α-motor neuron and all the muscle fibers it innervates. Obeys "all-or-none" law.
- Muscle Fiber Types:
 , Type IIA (fast oxidative glycolytic), Type IIX/B (fast glycolytic) detailing contraction speed, fatigue resistance, color, mitochondria, myoglobin, capillary density, and primary metabolic pathway)
, Type IIA (fast oxidative glycolytic), Type IIX/B (fast glycolytic) detailing contraction speed, fatigue resistance, color, mitochondria, myoglobin, capillary density, and primary metabolic pathway)
⭐ Titin is a giant protein responsible for passive elasticity of muscle and stabilizing myosin filaments within the sarcomere. It's the largest known protein in the human body!
Contraction Action - Sliding Story
-
NMJ Activation: AP → Ca²⁺ influx → ACh release → ACh binds receptors → EPP → Muscle AP.
-
Excitation-Contraction Coupling:
- Sliding Filament Mechanism:
- Ca²⁺ binds Troponin C → Tropomyosin shifts, exposing actin sites.
- Myosin head (energized by ATP hydrolysis: $ATP \rightarrow ADP + P_i$) binds actin (cross-bridge).
- Power Stroke: Myosin pulls actin; ADP and $P_i$ are released.
- New ATP binds myosin → detachment.
- Cycle repeats if Ca²⁺ & ATP are present.
- Sarcomere shortens: H & I bands ↓; A band constant. 📌 Mnemonic: "HI" disappears (H and I bands shorten).
- Relaxation: Ca²⁺ pumped back to SR (SERCA pump, ATP-dependent) → Tropomyosin covers actin sites.
⭐ Rigor mortis occurs due to ATP depletion, preventing myosin head detachment from actin.
Tendon Tidbits - Tough Connectors
-
Function: Transmit muscle force to bone; enable movement & stability.
-
Composition:
- Cells: Tenocytes & tenoblasts (synthesize/maintain ECM).
- ECM: Primarily Type I collagen (~95%), elastin, proteoglycans (e.g., decorin).
-
Structure: Hierarchical: Collagen molecule → microfibril → fibril → fascicle → tendon.
- Endotenon: Connective tissue around fascicles.
- Epitenon: Connective tissue sheath covering entire tendon.
- Paratenon: Outer loose connective tissue layer (if present, aids gliding).

-
Vascularity: Limited; supplied by musculotendinous junction (MTJ), osteotendinous junction (OTJ) & paratenon/synovial sheath.
-
Innervation: Golgi Tendon Organs (GTOs - proprioception), mechanoreceptors (Ruffini, Pacinian), nociceptors (free nerve endings).
-
Biomechanics: Viscoelastic properties (creep, stress relaxation).
- Stress-Strain Curve: Toe region (crimp unfolds), linear region (elastic), plastic region (microfailure), ultimate failure point.
-
Healing: Slow due to ↓ vascularity; often results in mechanically inferior scar tissue.
⭐ Type I collagen is the predominant collagen type in tendons, providing their characteristic high tensile strength.
Healing & Hurt - Repair & Rebuild
- Muscle Injury:
- Strain (indirect), Contusion (direct).
- Grades: 1 (mild, <5% fibers, min. loss), 2 (moderate, partial tear, pain, ↓strength), 3 (severe, complete tear, defect).
- Tendon Injury:
- Tendinopathy, Rupture.
- Healing Phases (Muscle & Tendon):
- Inflammation (0-7d): Hematoma, necrosis, phagocytosis. Cells: neutrophils, macrophages.
- Proliferation (1-6w): Fibroblasts, myoblasts active. Collagen III. Angiogenesis.
- Remodeling (>3w-yrs): Collagen III→I. Cross-linking, alignment, scar matures. Strength regains.
⭐ Tendon healing primarily forms scar tissue. Early Type III collagen is replaced by stronger Type I, but final tensile strength rarely matches the original, uninjured tendon.

- Key Points: RICE/PRICE acutely. Controlled mobilization is vital for optimal healing. Scar tissue is biomechanically inferior.
High‑Yield Points - ⚡ Biggest Takeaways
- Sarcomere: Basic contractile unit; actin-myosin interaction drives contraction.
- Calcium (Ca²⁺) binding to troponin C initiates muscle contraction.
- ATP is vital for cross-bridge cycling (contraction) and detachment (relaxation).
- Motor unit: A single motor neuron and all muscle fibers it innervates.
- Tendons: Primarily Type I collagen, ensuring high tensile strength.
- Golgi Tendon Organs sense muscle tension; Muscle Spindles sense muscle length/stretch.
- Henneman's size principle: Smaller motor units are recruited before larger ones during muscle activation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

