Cartilage Types & Basics - The Cartilage Crew
- Specialized connective tissue: avascular, aneural, alymphatic.
- Cells: Chondrocytes (reside in lacunae).
- Extracellular Matrix (ECM):
- Water (~75% by weight).
- Collagens (mainly Type II for hyaline & elastic; Type I & II for fibrocartilage).
- Proteoglycans (e.g., aggrecan, which binds hyaluronan).
- Three Main Types:
- Hyaline Cartilage (Type II collagen): Most abundant. Found in articular surfaces, nose, larynx, trachea, costal cartilages. Provides smooth, low-friction surfaces.
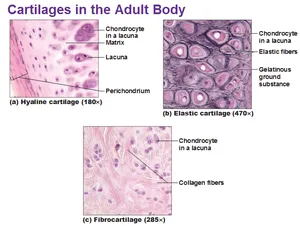
- Elastic Cartilage (Type II collagen + Elastin fibers): Provides flexible support. Found in external ear, epiglottis, Eustachian tube.
- Fibrocartilage (Type I & Type II collagen): Resists compression and shear forces.
⭐ Fibrocartilage, characterized by Type I and Type II collagen, is found in intervertebral discs, pubic symphysis, and menisci of the knee.
- Hyaline Cartilage (Type II collagen): Most abundant. Found in articular surfaces, nose, larynx, trachea, costal cartilages. Provides smooth, low-friction surfaces.
Hyaline Cartilage Structure - Articular Ace
- Primary Cell: Chondrocytes (in lacunae).
- Extracellular Matrix (ECM):
- Fibers: Mainly Type II collagen (tensile strength).
- Ground Substance:
- Proteoglycans (Aggrecan, Hyaluronic Acid).
- 80% water (resilience).
- Key Features: Avascular, Alymphatic, Aneural. Nutrition by diffusion (synovial fluid).
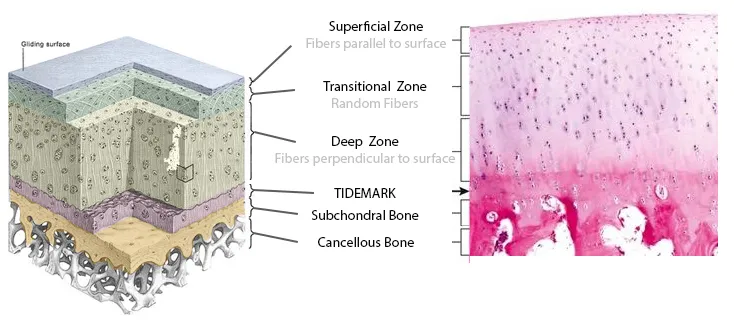
- Articular Cartilage Zones (Superficial to Deep):
- Superficial (Tangential): Flat chondrocytes; parallel collagen (shear resistance).
- Middle (Transitional): Round chondrocytes; random collagen.
- Deep (Radial): Columnar chondrocytes; perpendicular collagen (compression resistance).
- Calcified Zone: Tidemark; anchors to bone.
⭐ Aggrecan, a large proteoglycan in hyaline cartilage, binds to hyaluronic acid and is responsible for the tissue's osmotic properties and compressive stiffness.
Cartilage Metabolism & Nutrition - Chondrocyte Chow
⭐ Cartilage is avascular, aneural, and alymphatic; chondrocytes receive nutrition primarily via diffusion from synovial fluid, facilitated by joint loading.
- Nutrient Delivery:
- Mainly from synovial fluid (glucose, amino acids, O₂).
- Diffusion through matrix, enhanced by intermittent joint loading ("sponge effect").
- Chondrocyte Energy Source:
- Predominantly anaerobic glycolysis due to low O₂ tension: $Glucose \rightarrow Pyruvate \rightarrow Lactate + ATP$.
- ECM Balance (Turnover):
- Anabolism (Synthesis): Chondrocytes produce Type II collagen, aggrecan. Key stimulators: TGF-β, IGF-1.
- Catabolism (Degradation): Mediated by MMPs & ADAMTS enzymes. Key inducers: IL-1, TNF-α.
Cartilage Biomechanics & Repair - Stress & Distress
- Biomechanics: Articular cartilage is a specialized connective tissue designed to withstand and distribute loads.
- Type II collagen: Provides tensile strength and structural integrity.
- Aggrecan (proteoglycan): Confers compressive stiffness by binding $H_2O$, creating turgor pressure.
- Viscoelasticity: Exhibits creep (deformation under constant load) and stress-relaxation (stress reduction under constant deformation), crucial for shock absorption.
- Lubrication: Boundary (lubricin) and fluid-film mechanisms minimize friction.
- Repair Limitations: Cartilage has a very limited capacity for self-repair.
- Avascular, aneural, and alymphatic nature restricts access to progenitor cells and nutrients.
- Chondrocytes: Low mitotic activity and are fixed within the matrix, preventing migration to injury sites.
- Partial-thickness defects: Generally do not heal.
- Full-thickness defects: May heal with fibrocartilage (Type I collagen), which is mechanically inferior to native hyaline cartilage (Type II).
- Stress & Distress (Degeneration):
- Physiological loading: Essential for maintaining cartilage health and matrix homeostasis.
- Abnormal/excessive loading or trauma: Leads to chondrocyte apoptosis, increased matrix metalloproteinases (MMPs) activity, and net matrix degradation, progressing to Osteoarthritis (OA).
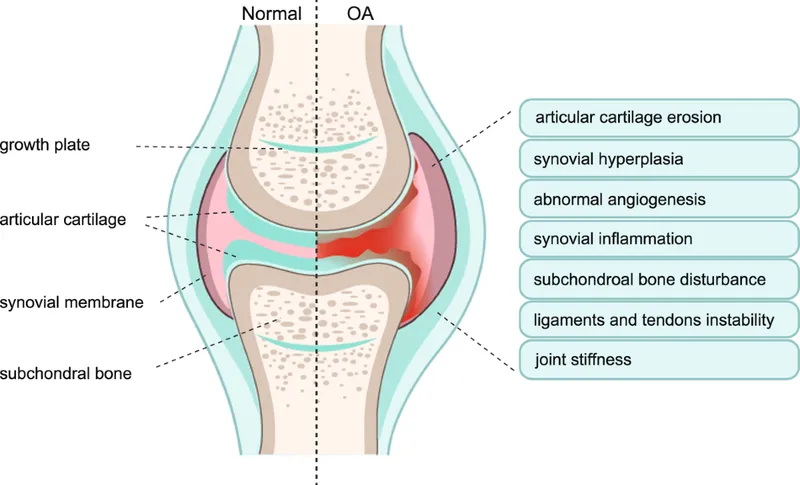
⭐ The limited repair capacity of articular cartilage is primarily due to its avascular nature and the inability of chondrocytes to migrate to defect sites and proliferate effectively.
High‑Yield Points - ⚡ Biggest Takeaways
- Articular cartilage is hyaline, with Type II collagen (tensile strength) and aggrecan (compressive strength).
- It's avascular, aneural, alymphatic; nutrition via diffusion from synovial fluid.
- Chondrocytes are the sole cells, maintaining the extracellular matrix (ECM).
- Limited repair capacity due to avascularity and low chondrocyte division.
- Four zones: Superficial (tangential fibers), Middle, Deep (radial fibers, highest proteoglycans), Calcified.
- The tidemark separates deep uncalcified from calcified cartilage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

