Knee Arthroscopy - Scope & Staples
- Scope:
- Diagnostic: Visualize menisci, ligaments (ACL/PCL), cartilage, synovium.
- Therapeutic: Multiple options.
- Meniscal tears: Meniscectomy (partial/total), meniscal repair (all-inside, inside-out, outside-in techniques).
- Ligament injuries: ACL/PCL reconstruction (BTB, hamstring grafts).
- Cartilage lesions: Chondroplasty, microfracture, OATS.
- Synovial pathology: Synovectomy (e.g., PVNS).
- Loose body removal.
- Patellofemoral: Lateral release, patellar debridement.
- Fluid Management: Saline for distension & visualization.
- Key Fixation ("Staples"):
- Meniscal Repair: Sutures, bioabsorbable anchors (all-suture, PEEK), darts.
- ACL/PCL Reconstruction:
- Fixation: Interference screws (metal/bio), suspensory devices (Endobutton), cross-pins.
- Graft tensioning vital.
- Cartilage Repair (OATS): Press-fit plugs, scaffold fixation.
- Portals & Risks:
- Portals: Std. AL (anterolateral), AM (anteromedial); accessory as needed.
- Risks: Infection, DVT, nerve injury, stiffness, instrument breakage.
⭐ The "terrible triad" (O'Donoghue's triad) involves injury to the ACL, MCL, and medial meniscus, often requiring arthroscopic intervention for ACL and meniscal components.
Shoulder Arthroscopy - Rotator & Repair
- Indications: Symptomatic rotator cuff tears (RCTs) failing >3-6 months conservative therapy; acute traumatic tears in active patients.
- RCT Overview:
- Muscles (SITS): Supraspinatus (most common), Infraspinatus, Teres minor, Subscapularis.
- Types: Partial (articular/bursal-sided), Full-thickness. Patterns: Crescent, U-shaped, L-shaped. Massive tears: >5 cm or involving ≥2 tendons.
- Repair Principles:
- Debridement of tear margins, footprint preparation (bleeding bone bed for healing).
- Anchors: Metal, bioabsorbable, PEEK, all-suture types.
- Constructs: Single-Row (SR); Double-Row (DR) for ↑biomechanical strength & potentially ↓re-tear rates in larger tears; Suture-bridge techniques.
- Common Adjuncts: Subacromial decompression (SAD)/acromioplasty for impingement; biceps tenotomy/tenodesis if biceps pathology present.
- Post-operative: Sling immobilization (4-6 weeks), structured, phased physiotherapy crucial for outcomes.
- Complications: Stiffness (adhesive capsulitis), re-tear (most common), infection, anchor pull-out, deltoid dysfunction, nerve injury (axillary n.).
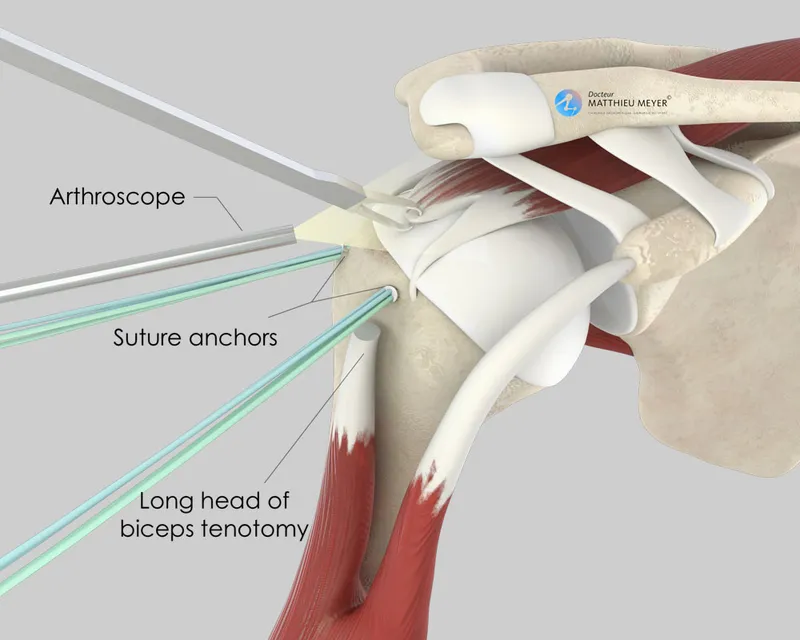
⭐ The "critical zone" (Codman's critical zone) of the supraspinatus tendon, a hypovascular region approximately 1 cm proximal to its insertion on the greater tuberosity, is the most common location for degenerative tears and subsequent failure of repair due to poor healing potential.
Other Joints & Complications - Wider View & Watchouts
- Elbow Arthroscopy:
- Uses: Loose bodies, osteochondritis dissecans (OCD), synovitis, capsular release.
- Nerve at risk: Posterior interosseous n. (PIN).
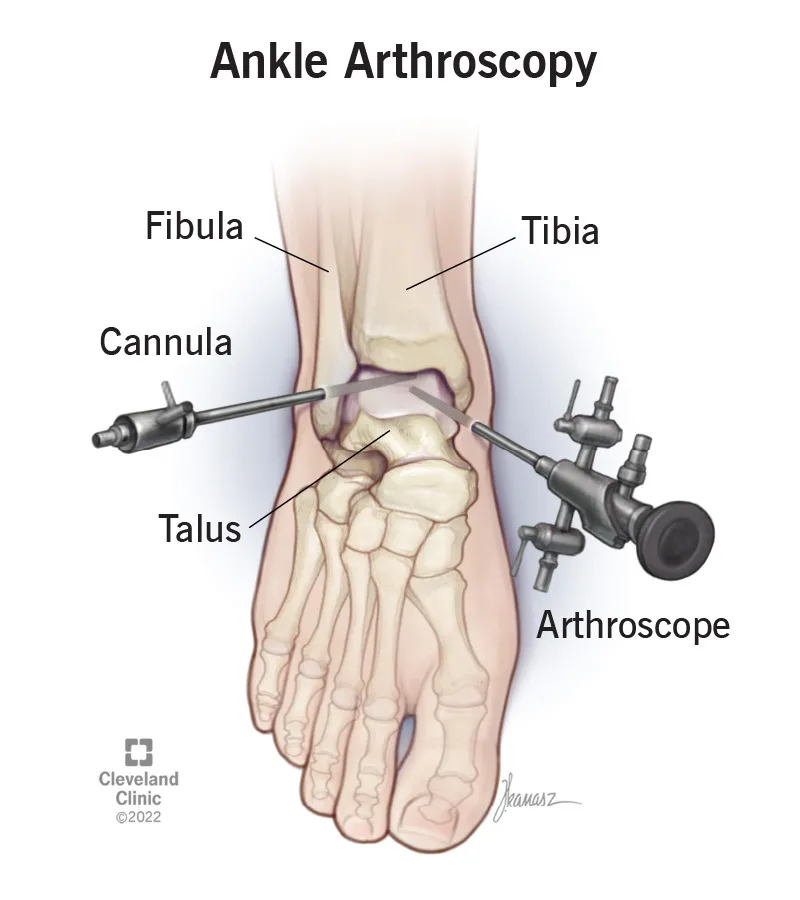
- Ankle Arthroscopy:
- Uses: Talar OCD, impingement (anterior/posterior), synovitis.
- Nerves at risk: Superficial peroneal n., sural n.
- Hip Arthroscopy:
- Uses: Femoroacetabular impingement (FAI), labral tears, loose bodies. Traction needed.
- Nerves at risk: Lateral femoral cutaneous n., sciatic n.
- Wrist Arthroscopy:
- Uses: Triangular Fibrocartilage Complex (TFCC) tears, ganglion removal, diagnostic.
- Common portals: 3-4, 4-5 (radiocarpal).
- General Arthroscopy Complications:
- Intra-op: Instrument breakage, chondral injury, neurovascular damage, fluid extravasation (⚠️ compartment syndrome risk, esp. ankle/elbow).
- Post-op: Infection (septic arthritis <1%), Deep Vein Thrombosis/Pulmonary Embolism (DVT/PE), stiffness/arthrofibrosis, Complex Regional Pain Syndrome (CRPS), portal issues (neuroma, sinus).
⭐ Pudendal nerve neurapraxia can occur in hip arthroscopy due to perineal post traction.
High‑Yield Points - ⚡ Biggest Takeaways
- Partial meniscectomy is preferred over total for degenerative tears to prevent early osteoarthritis.
- ACL reconstruction commonly uses hamstring autografts (semitendinosus-gracilis).
- Rotator cuff repair is indicated for full-thickness tears to restore shoulder function.
- Bankart repair addresses recurrent anterior shoulder dislocation by fixing the anteroinferior labrum.
- SLAP lesion repair targets tears of the Superior Labrum Anterior to Posterior.
- Loose body removal prevents joint locking and further cartilage damage.
- Microfracture for cartilage defects stimulates fibrocartilage formation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

