Arthrology and Infections

On this page
🦠 Microbial Siege: The Joint Invasion Landscape
Joints are sterile sanctuaries until microbes breach their defenses, transforming them into inflamed battlegrounds where cartilage destruction unfolds in hours and permanent disability looms without swift intervention. You'll master how bacteria invade synovial spaces, distinguish septic arthritis from mimics through targeted diagnostics, deploy antibiotics and drainage strategically, and build prevention protocols that protect vulnerable patients. This lesson equips you to recognize joint infections early, act decisively, and preserve function when every hour counts.
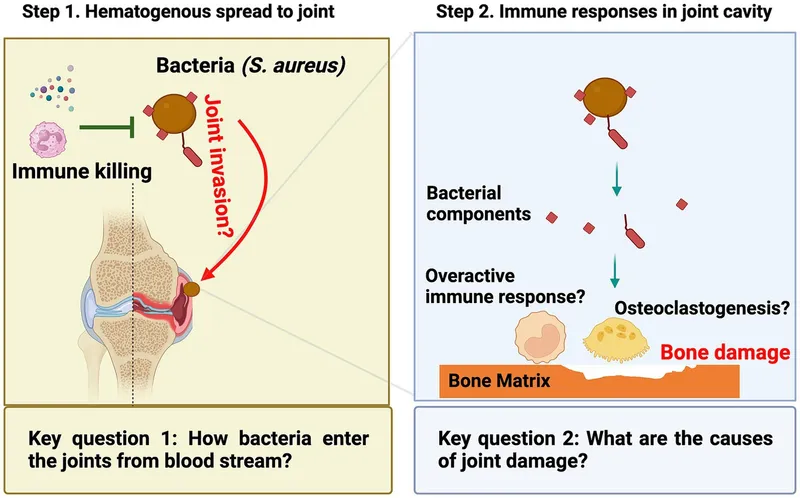
📌 Remember: SHIP - Septic arthritis, Hematogenous spread, Iatrogenic introduction, Penetrating trauma. These four pathways account for >95% of joint infections, with hematogenous spread responsible for 60% of cases in children and 40% in adults.
The microbial spectrum varies dramatically by patient demographics and infection pathway. Staphylococcus aureus dominates across all age groups, causing 70% of septic arthritis cases in adults and 80% in children over 2 years. Methicillin-resistant strains (MRSA) now account for 25-30% of hospital-acquired joint infections, with mortality rates reaching 15-20% compared to 5% for methicillin-sensitive strains.
| Organism | Age Predilection | Joint Preference | Mortality Rate | Antibiotic Resistance |
|---|---|---|---|---|
| S. aureus | All ages | Knee (45%), Hip (25%) | 5-15% | MRSA: 25-30% |
| Streptococcus | Elderly, DM | Multiple joints | 8-12% | Penicillin: <5% |
| N. gonorrhoeae | 15-40 years | Wrist, ankle | <1% | Fluoroquinolone: 30% |
| Gram-negative | Immunocompromised | Axial skeleton | 20-25% | ESBL: 15-20% |
| Kingella kingae | <2 years | Hip, knee | <2% | Ampicillin: 10% |
The pathophysiology follows a predictable cascade once microorganisms establish synovial presence. Initial bacterial adhesion triggers complement activation and neutrophil recruitment within 2-4 hours. Neutrophil degranulation releases proteolytic enzymes, particularly elastase and collagenase, which begin cartilage matrix destruction. Simultaneously, bacterial toxins and inflammatory mediators stimulate synovial cells to produce matrix metalloproteinases (MMPs), accelerating cartilage breakdown.
-
Acute Phase (0-24 hours)
- Bacterial adhesion and initial complement activation
- Neutrophil recruitment: 10,000-50,000 cells/μL in synovial fluid
- Early cytokine release: IL-1β, TNF-α, IL-6
- IL-1β levels: >1000 pg/mL (normal: <10 pg/mL)
- TNF-α elevation: 50-100x baseline within 6 hours
-
Destructive Phase (24-72 hours)
- Peak enzyme activity and cartilage destruction
- Synovial fluid glucose: <50% of serum levels
- Protein concentration: >4.5 g/dL (normal: <2.5 g/dL)
- Lactate levels: >7.5 mmol/L indicate severe infection
- pH depression: <7.30 correlates with poor outcomes
💡 Master This: Cartilage destruction is irreversible after 72 hours of untreated infection. The "golden window" for joint preservation requires recognition within 24 hours and drainage within 48 hours of symptom onset.
Risk stratification reveals distinct vulnerability patterns across patient populations. Immunocompromised states increase infection risk by 5-10 fold, with diabetes mellitus conferring 3-4x higher risk due to impaired neutrophil function and delayed wound healing. Rheumatoid arthritis patients face 8-10x increased risk, particularly those receiving TNF-α inhibitors or methotrexate therapy.
⭐ Clinical Pearl: Prosthetic joints alter the infection landscape dramatically. Biofilm formation occurs within 6-8 hours of bacterial seeding, creating 1000x increased antibiotic resistance. Early infections (<3 months) typically involve S. aureus or gram-negative organisms, while late infections (>24 months) favor coagulase-negative staphylococci.
Understanding this microbial siege framework enables rapid pathogen prediction based on clinical presentation patterns. Connect these foundational concepts through diagnostic approaches to master the systematic evaluation of suspected joint infections.
🦠 Microbial Siege: The Joint Invasion Landscape
🔬 Pathogen Profiles: The Bacterial Rogues Gallery
📌 Remember: GNATS for gonococcal arthritis - Genital symptoms, Neisseria culture, Asymmetric joint involvement, Tenosynovitis, Skin lesions. This constellation occurs in 80% of disseminated gonococcal infections, with 60% showing skin manifestations.
Staphylococcus aureus dominates the pathogen landscape through multiple virulence mechanisms. Protein A binds immunoglobulin Fc regions, preventing opsonization and phagocytosis. Alpha-toxin creates membrane pores in synovial cells, while hyaluronidase breaks down joint matrix components. MRSA strains carry additional resistance genes, with mecA conferring methicillin resistance and vanA providing vancomycin resistance in rare cases.
| Pathogen | Onset Pattern | Joint Distribution | Synovial WBC | Glucose Ratio | Mortality |
|---|---|---|---|---|---|
| S. aureus | Acute (12-24h) | Monoarticular (90%) | >100,000/μL | <0.25 | 10-15% |
| Streptococcus | Subacute (2-7d) | Monoarticular (80%) | 50,000-100,000/μL | 0.25-0.50 | 5-8% |
| N. gonorrhoeae | Migratory→Localized | Polyarticular→Mono | 30,000-80,000/μL | >0.50 | <1% |
| Gram-negative | Variable | Axial preference | >75,000/μL | <0.30 | 20-25% |
| Anaerobes | Indolent (weeks) | Large joints | 20,000-50,000/μL | 0.40-0.60 | 8-12% |
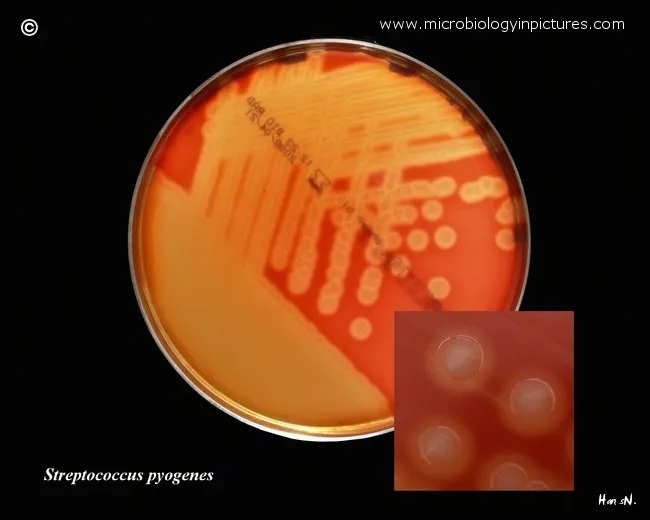
Streptococcal arthritis follows distinct epidemiological patterns. Group A Streptococcus (S. pyogenes) causes aggressive infections in healthy individuals, often following pharyngitis or cellulitis. Group B Streptococcus (S. agalactiae) predominantly affects neonates and elderly patients with diabetes. Viridans group streptococci typically infect abnormal joints or patients with endocarditis.
-
Group A Streptococcus
- Peak incidence: Winter months (pharyngitis season)
- Joint involvement: Knee (45%), ankle (25%), shoulder (15%)
- Complications: Necrotizing fasciitis in 10-15% of cases
- Mortality with necrotizing fasciitis: 30-40%
- Requires immediate surgical debridement
-
Group B Streptococcus
- Risk factors: Diabetes (60%), malignancy (25%), immunosuppression (40%)
- Presentation: Subacute onset over 3-7 days
- Bacteremia: Present in 80% of cases
- Blood culture positive: 24-48 hours
- Synovial culture positive: 48-72 hours
Neisseria gonorrhoeae creates a unique clinical syndrome requiring specialized recognition. Disseminated gonococcal infection (DGI) affects 1-3% of patients with untreated gonorrhea, predominantly young, sexually active individuals. The classic presentation includes migratory polyarthralgia, tenosynovitis, and dermatitis before localizing to 1-2 joints.
💡 Master This: Gonococcal arthritis diagnosis relies on clinical syndrome recognition rather than synovial fluid culture. Joint fluid cultures are positive in only 25-50% of cases, while urogenital cultures yield organisms in 80-90% of patients with DGI.
Gram-negative arthritis represents the highest mortality category, particularly in immunocompromised hosts. Pseudomonas aeruginosa shows predilection for fibrocartilaginous joints (sacroiliac, sternoclavicular, symphysis pubis) and injection drug users. Escherichia coli and Klebsiella species typically arise from urinary tract sources in elderly patients with diabetes or chronic kidney disease.
-
Pseudomonas aeruginosa
- Risk factors: IV drug use (70%), immunosuppression (50%)
- Joint preference: Sternoclavicular (40%), sacroiliac (30%)
- Antibiotic resistance: Carbapenem resistance in 15-25%
- Requires combination therapy: β-lactam + aminoglycoside
- Treatment duration: 6-8 weeks minimum
-
Enterobacteriaceae
- Source: Urinary tract (60%), intra-abdominal (25%)
- Demographics: Age >65 (80%), diabetes (70%)
- ESBL production: 15-20% of isolates
- Carbapenem therapy required for ESBL producers
- Mortality with ESBL: 25-30% vs 15% for susceptible strains
⭐ Clinical Pearl: Kingella kingae in children under 24 months requires prolonged culture incubation and PCR confirmation. Standard cultures miss 40% of cases due to fastidious growth requirements and prior antibiotic exposure.
Understanding pathogen-specific patterns enables targeted empirical therapy while awaiting culture results. Connect these bacterial profiles through diagnostic algorithms to master the systematic approach to joint infection evaluation.
🔬 Pathogen Profiles: The Bacterial Rogues Gallery
🎯 Diagnostic Precision: The Clinical Detective Framework
📌 Remember: FLUID for synovial analysis priorities - Fluid appearance, Leukocyte count, Under polarized light (crystals), Infection markers, Differential count. This sequence ensures systematic evaluation without missing critical findings.
Clinical presentation patterns provide the initial diagnostic framework. Acute monoarthritis in a previously healthy joint carries 80% probability of bacterial infection when accompanied by fever and elevated inflammatory markers. Polyarticular involvement reduces bacterial probability to 20-30% but increases consideration for gonococcal, viral, or crystal arthropathy.
| Clinical Feature | Bacterial Probability | Viral Probability | Crystal Probability | Autoimmune Probability |
|---|---|---|---|---|
| Acute monoarthritis + fever | 80-85% | 5-10% | 10-15% | <5% |
| Subacute monoarthritis | 40-50% | 20-25% | 25-30% | 10-15% |
| Acute polyarthritis | 20-30% | 40-50% | 15-20% | 20-25% |
| Chronic polyarthritis | <5% | <5% | 10-15% | 75-80% |
| Migratory arthritis | 60-70% (GC) | 15-20% | <5% | 15-20% |
Synovial fluid analysis provides the diagnostic gold standard through multiple parameters. Cell count and differential offer immediate bacterial probability assessment, while glucose ratio and lactate levels provide metabolic evidence of infection. Gram stain yields rapid pathogen identification in 60-80% of bacterial cases.
-
Synovial Fluid Parameters
- Normal values: WBC <200/μL, PMN <25%, glucose ratio >0.75
- Inflammatory: WBC 2,000-50,000/μL, PMN 50-75%, glucose ratio 0.50-0.75
- Septic: WBC >50,000/μL, PMN >75%, glucose ratio <0.50
- Highly septic: WBC >100,000/μL, glucose ratio <0.25
- Lactate >7.5 mmol/L indicates severe infection
-
Diagnostic Accuracy
- WBC >50,000/μL: Sensitivity 90%, Specificity 85% for bacterial infection
- PMN >75%: Sensitivity 85%, Specificity 90% for bacterial infection
- Glucose ratio <0.50: Sensitivity 80%, Specificity 95% for bacterial infection
- Combined parameters: Sensitivity 95%, Specificity 98%
- Lactate >5.5 mmol/L: Sensitivity 92%, Specificity 89%
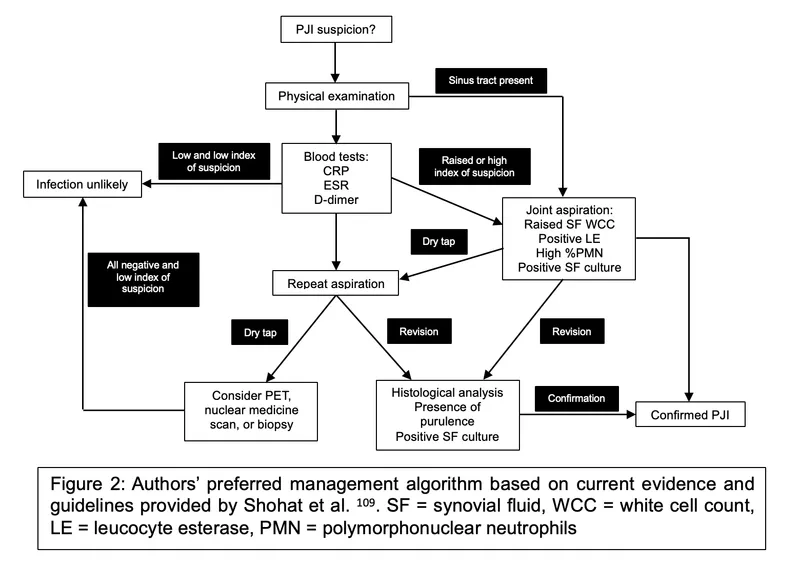
💡 Master This: Synovial fluid lactate >7.5 mmol/L predicts bacterial infection with 95% accuracy and correlates with cartilage destruction severity. This parameter remains elevated even after antibiotic therapy initiation, unlike glucose levels which normalize within 24-48 hours.
Advanced diagnostic techniques enhance detection accuracy in challenging cases. Synovial fluid PCR identifies fastidious organisms and culture-negative infections with 85-90% sensitivity. Next-generation sequencing detects polymicrobial infections and antibiotic-resistant organisms within 24-48 hours.
Imaging modalities provide complementary diagnostic information and surgical planning guidance. Plain radiographs remain the initial study but show changes only after 7-14 days of infection. Ultrasound detects joint effusions and guides aspiration with 95% accuracy. MRI reveals early bone marrow edema and soft tissue involvement within 24-48 hours.
-
Imaging Timeline
- Ultrasound: Effusion detection within 2-4 hours
- MRI: Bone marrow edema within 24-48 hours
- Plain radiographs: Joint space narrowing at 7-14 days
- Bone erosions: Visible at 2-4 weeks
- Osteomyelitis: Cortical destruction at 10-14 days
-
Advanced Imaging
- CT: Bone destruction and sequestra identification
- Nuclear medicine: Tc-99m bone scan sensitivity 95%, specificity 78%
- PET/CT: Sensitivity 90%, specificity 85% for prosthetic infections
- SUV max >2.5 suggests active infection
- Dual-time imaging improves specificity to 92%
⭐ Clinical Pearl: MRI with gadolinium shows synovial enhancement patterns that distinguish bacterial from crystal arthropathy with 88% accuracy. Thick, irregular enhancement suggests bacterial infection, while thin, smooth enhancement indicates crystal disease.
Culture optimization maximizes pathogen recovery through proper specimen handling and processing techniques. Blood culture bottles for synovial fluid improve recovery rates by 15-20% compared to standard culture media. Prolonged incubation for 5-7 days captures fastidious organisms like Kingella and HACEK group bacteria.
Understanding this diagnostic precision framework enables rapid, accurate joint infection diagnosis. Connect these evaluation principles through treatment algorithms to master the therapeutic management of joint infections.
🎯 Diagnostic Precision: The Clinical Detective Framework
⚔️ Treatment Battleground: The Therapeutic Arsenal
📌 Remember: DRAIN for surgical indications - Delay >48 hours, Recurrent effusion, Antibiotic failure, Inaccessible location, Necrotic tissue. Any of these factors mandates surgical intervention beyond simple aspiration.
Antibiotic selection follows pathogen-directed principles with consideration for synovial penetration and biofilm activity. β-lactam antibiotics achieve 60-80% of serum concentrations in inflamed synovial fluid, while fluoroquinolones and clindamycin reach 80-100% penetration. Vancomycin penetration improves from 20% in normal joints to 60-70% with inflammation.
| Antibiotic Class | Synovial Penetration | Biofilm Activity | MRSA Coverage | Gram-Negative Coverage |
|---|---|---|---|---|
| Penicillins | 60-80% | Poor | No | Limited |
| Cephalosporins | 70-85% | Poor | No (except ceftaroline) | Good |
| Fluoroquinolones | 80-100% | Good | Variable | Excellent |
| Vancomycin | 60-70% | Poor | Excellent | No |
| Linezolid | 90-100% | Good | Excellent | No |
| Daptomycin | 70-80% | Good | Excellent | No |
Empirical antibiotic regimens target likely pathogens based on patient demographics and clinical presentation. Healthy adults receive anti-staphylococcal therapy, while immunocompromised patients require broad-spectrum coverage. Prosthetic joint infections demand biofilm-active agents from treatment initiation.
-
Empirical Regimens by Population
- Healthy adults: Cefazolin 2g IV q8h OR Clindamycin 600mg IV q8h
- MRSA risk factors: Vancomycin 15-20mg/kg IV q12h (target trough 15-20 μg/mL)
- Immunocompromised: Vancomycin + Ceftazidime 2g IV q8h
- Pseudomonas risk: Add Tobramycin 5-7mg/kg IV daily
- Anaerobe coverage: Metronidazole 500mg IV q8h
-
Prosthetic Joint Infections
- Early (<3 months): Vancomycin + Rifampin 600mg PO BID
- Late (>24 months): Vancomycin + Rifampin + Fluoroquinolone
- Biofilm disruption: Rifampin essential for staphylococcal infections
- Never use rifampin monotherapy - resistance develops in 48-72 hours
- Combination therapy reduces resistance to <5%
Surgical management follows a staged approach based on infection severity and joint type. Native joints undergo arthroscopic drainage for accessible locations and open drainage for deep joints. Prosthetic joints require implant retention vs removal decisions based on timing and organism characteristics.
Duration of therapy varies by pathogen, joint type, and surgical intervention. Native joint infections typically require 2-4 weeks of IV therapy followed by 2-4 weeks oral therapy. Prosthetic joint infections demand 6-12 weeks total therapy with rifampin continuation for 3-6 months.
-
Treatment Duration Guidelines
- S. aureus native joint: 4 weeks IV + 2 weeks PO
- Streptococcus native joint: 2 weeks IV + 2 weeks PO
- Gram-negative native joint: 3 weeks IV + 3 weeks PO
- Pseudomonas: 6 weeks IV therapy minimum
- ESBL producers: 4 weeks IV + 2 weeks PO
-
Prosthetic Joint Duration
- DAIR procedure: 6 weeks IV + 6 weeks PO
- Two-stage exchange: 6 weeks between stages + 6 weeks post-reimplantation
- Rifampin therapy: Continue 3-6 months for staphylococcal infections
- Biofilm eradication: Requires prolonged therapy
- Relapse rates: 15-20% without adequate duration
💡 Master This: Oral antibiotic transition requires clinical improvement, afebrile >48 hours, and decreasing inflammatory markers. Fluoroquinolones provide excellent oral bioavailability for gram-negative infections, while linezolid or clindamycin cover gram-positive organisms.
Monitoring parameters guide therapy adjustments and detect complications. C-reactive protein normalizes over 2-4 weeks with successful therapy, while ESR remains elevated for 6-8 weeks. Synovial fluid parameters improve within 48-72 hours of appropriate therapy.
- Response Monitoring
- Clinical improvement: 48-72 hours (fever resolution, pain reduction)
- CRP normalization: 2-4 weeks (50% reduction by day 7)
- ESR normalization: 6-8 weeks (slower than CRP)
- Persistent elevation: Consider treatment failure or complications
- Rising levels: Suggests inadequate therapy or resistance
⭐ Clinical Pearl: Procalcitonin levels >0.5 ng/mL suggest bacterial infection with 85% sensitivity and normalize within 72 hours of effective therapy. This marker helps distinguish bacterial from crystal arthropathy when synovial fluid analysis is inconclusive.
Understanding this therapeutic arsenal enables optimal treatment selection and monitoring. Connect these management principles through prevention strategies to master the comprehensive approach to joint infection care.
⚔️ Treatment Battleground: The Therapeutic Arsenal
🛡️ Prevention Fortress: The Protective Shield Strategy
📌 Remember: ARMOR for infection prevention - Antibiotic prophylaxis, Risk factor modification, Minimally invasive techniques, Operating room protocols, Rapid intervention. These five layers provide comprehensive protection against joint infections.
Risk stratification enables targeted prevention strategies based on patient factors and procedure complexity. Diabetes mellitus increases infection risk by 3-4 fold, while rheumatoid arthritis with immunosuppressive therapy confers 8-10 fold increased risk. Revision procedures carry 2-3 times higher infection rates than primary surgeries.
| Risk Factor | Relative Risk | Modifiable | Intervention | Risk Reduction |
|---|---|---|---|---|
| Diabetes (HbA1c >8%) | 3.5x | Yes | Glycemic control | 40-50% |
| Obesity (BMI >35) | 2.8x | Partially | Weight loss | 25-30% |
| Smoking | 2.2x | Yes | Cessation >4 weeks | 35-40% |
| RA + MTX | 4.5x | Partially | Drug holiday | 20-25% |
| Prior infection | 6.8x | No | Enhanced surveillance | 15-20% |
| Revision surgery | 2.5x | No | Extended prophylaxis | 30-35% |
Antibiotic prophylaxis follows timing, selection, and duration principles based on procedure type and patient factors. Cefazolin remains first-line for most orthopedic procedures, while vancomycin is reserved for MRSA risk factors or β-lactam allergies. Prophylaxis timing within 60 minutes of incision optimizes tissue concentrations.
-
Standard Prophylaxis Protocols
- Cefazolin: 2g IV (3g if weight >120kg) within 60 minutes of incision
- Vancomycin: 15mg/kg IV over 60-120 minutes, start 120 minutes pre-incision
- Clindamycin: 600mg IV for β-lactam allergic patients
- Redosing intervals: Cefazolin q4h, Vancomycin q12h during surgery
- Duration: Single dose for most procedures, 24 hours for implants
-
High-Risk Modifications
- MRSA colonization: Vancomycin + Cefazolin combination
- Gram-negative risk: Cefazolin + Gentamicin 5mg/kg
- Prolonged procedures (>4 hours): Redose primary antibiotic
- Tourniquet use: Administer before inflation
- Blood loss >1500mL: Consider additional dosing
Intraoperative protocols minimize contamination through environmental controls and sterile techniques. Laminar airflow reduces airborne contamination by 90%, while body exhaust suits further decrease bacterial shedding. Skin preparation with chlorhexidine-alcohol solutions provides superior antimicrobial activity compared to povidone-iodine.
Postoperative surveillance enables early detection and intervention when infections develop. Wound monitoring for erythema, drainage, and dehiscence continues for 30 days after surgery. Patient education regarding warning signs facilitates prompt reporting of concerning symptoms.
-
Surveillance Parameters
- Daily wound assessment: First 72 hours post-surgery
- Temperature monitoring: >38.5°C warrants evaluation
- Pain assessment: Increasing pain after initial improvement
- Wound drainage: Any purulent or malodorous discharge
- Systemic symptoms: Fever, chills, malaise after day 3
-
Early Intervention Triggers
- Wound erythema >2cm from incision
- Persistent drainage beyond 48 hours
- Wound dehiscence or fluctuance
- Laboratory markers: CRP >100 mg/L or rising trend
- Imaging findings: Fluid collections or gas in tissues
💡 Master This: Surgical site infections present within 30 days in 80% of cases, but prosthetic joint infections can manifest months to years later. Late infections often present with subtle symptoms requiring high clinical suspicion.
Special populations require modified prevention strategies based on unique risk profiles. Immunocompromised patients need extended prophylaxis and enhanced surveillance. Pediatric patients require weight-based dosing and age-appropriate monitoring protocols.
-
Immunocompromised Modifications
- Extended prophylaxis: 24-48 hours post-surgery
- Broader spectrum: Consider gram-negative coverage
- Enhanced surveillance: Weekly follow-up for 6 weeks
- TNF-α inhibitor patients: Hold therapy 1-2 weeks pre/post-surgery
- Steroid therapy: Stress dose coverage perioperatively
-
Pediatric Considerations
- Weight-based dosing: Cefazolin 30mg/kg (max 2g)
- Age-specific pathogens: Consider Kingella kingae in <2 years
- Family education: Caregiver training for symptom recognition
- Behavioral changes: Irritability or feeding difficulties
- Physical signs: Limping or refusal to bear weight
⭐ Clinical Pearl: Nasal decolonization with mupirocin for 5 days preoperatively reduces S. aureus surgical site infections by 60% in colonized patients. Universal screening and targeted decolonization provides cost-effective prevention.
Understanding this prevention fortress enables comprehensive risk reduction across all patient populations. Connect these protective strategies through outcome optimization to master the complete spectrum of joint infection management.
🛡️ Prevention Fortress: The Protective Shield Strategy
🎖️ Mastery Command Center: The Clinical Excellence Arsenal
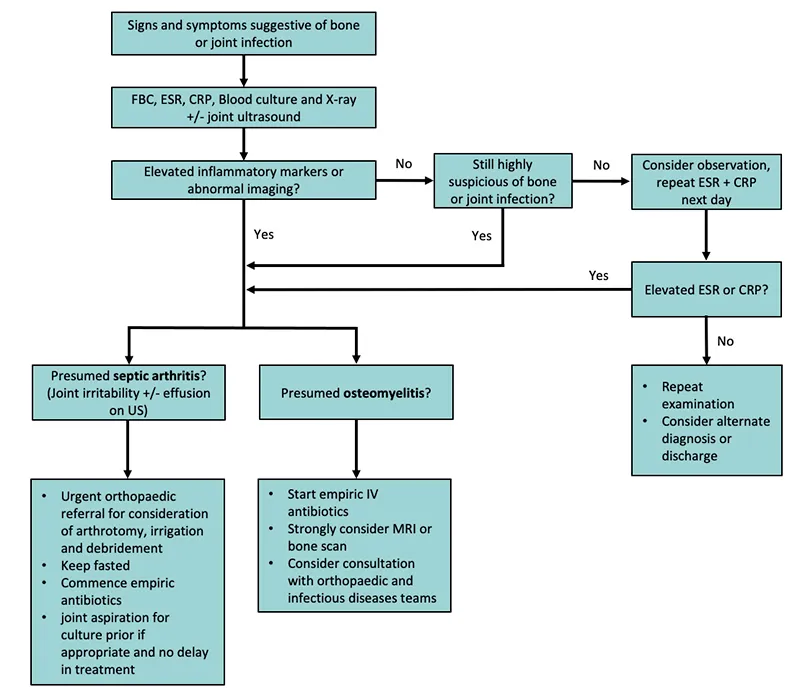
📌 Remember: MASTER framework - Monitor continuously, Assess systematically, Stratify risk, Treat aggressively, Evaluate outcomes, Refine protocols. This cycle ensures continuous improvement and optimal patient care.
Essential Clinical Thresholds provide immediate decision points for critical interventions. Synovial fluid WBC >50,000/μL mandates immediate antibiotic therapy, while glucose ratio <0.25 indicates severe infection requiring surgical drainage. CRP >100 mg/L suggests bacterial infection with 90% probability.
| Parameter | Normal | Inflammatory | Septic | Action Required |
|---|---|---|---|---|
| Synovial WBC | <200/μL | 2,000-50,000/μL | >50,000/μL | Immediate antibiotics |
| PMN % | <25% | 50-75% | >75% | Surgical consultation |
| Glucose ratio | >0.75 | 0.50-0.75 | <0.50 | Urgent drainage |
| Lactate | <2.5 mmol/L | 2.5-5.5 mmol/L | >7.5 mmol/L | ICU consideration |
| CRP | <3 mg/L | 10-100 mg/L | >100 mg/L | Blood cultures |
Rapid Assessment Protocol enables systematic evaluation within 30 minutes of presentation. Clinical scoring combined with point-of-care testing provides immediate risk stratification. Ultrasound-guided aspiration yields diagnostic fluid within 15 minutes.
-
30-Minute Assessment Protocol
- Minutes 0-5: Clinical history and examination
- Minutes 5-10: Laboratory orders (CBC, CRP, blood cultures)
- Minutes 10-20: Joint aspiration (ultrasound-guided if needed)
- Minutes 20-25: Synovial fluid analysis (cell count, gram stain)
- Minutes 25-30: Treatment decision and antibiotic initiation
-
Point-of-Care Testing
- Synovial fluid lactate: <5 minutes for results
- Gram stain: 10 minutes for preliminary identification
- Leukocyte esterase: 2 minutes for WBC estimation
- Sensitivity: 85% for bacterial infection
- Specificity: 90% when combined with clinical assessment
💡 Master This: Antibiotic stewardship requires culture-directed therapy within 48-72 hours. De-escalation from empirical broad-spectrum to targeted therapy reduces resistance development and adverse effects while maintaining efficacy.
Treatment Success Metrics guide therapy optimization and outcome assessment. Clinical improvement within 48-72 hours indicates appropriate therapy, while CRP reduction >50% by day 7 predicts successful treatment. Functional outcomes at 6 months determine long-term success.
Quality Improvement Framework ensures continuous enhancement of care delivery. Infection rates, time-to-treatment, and functional outcomes serve as key performance indicators. Multidisciplinary rounds optimize care coordination and resource utilization.
-
Key Performance Indicators
- Time-to-diagnosis: Target <6 hours from presentation
- Time-to-antibiotics: Target <1 hour from diagnosis
- Surgical drainage: Target <24 hours when indicated
- Culture positivity: Target >80% for bacterial infections
- Antibiotic appropriateness: Target >95% culture-directed therapy
-
Outcome Metrics
- 30-day mortality: Target <5% for native joints
- Functional preservation: Target >85% return to baseline
- Recurrence rates: Target <10% at 1 year
- Patient satisfaction: Target >90% with care experience
- Length of stay: Benchmark against national standards
⭐ Clinical Pearl: Multidisciplinary teams including orthopedic surgery, infectious disease, and pharmacy reduce treatment failures by 30% and length of stay by 2-3 days through coordinated care and protocol standardization.
This mastery command center provides the essential framework for transforming joint infection challenges into systematic clinical successes through evidence-based protocols and continuous quality improvement.
🎖️ Mastery Command Center: The Clinical Excellence Arsenal
Continue reading on Oncourse
Sign up for free to access the full lesson, plus unlimited questions, flashcards, AI-powered notes, and more.
CONTINUE READING — FREEor get the app
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Practice Questions: Arthrology and Infections
Test your understanding with these related questions
A 12 year old girl was brought with fever, malaise, and migrating polyarthritis. She had a history of recurrent throat infections in the past. Elevated erythrocyte sedimentation rate is noted. Which among the following is NOT a major Jones criteria for diagnosis of acute rheumatic fever?












