Urogynecology

On this page
🏥 The Urogynecology Command Center: Mastering Pelvic Floor Medicine
The pelvic floor is medicine's most underappreciated architectural marvel-a dynamic support system where anatomy, biomechanics, and neural control converge to maintain continence and organ position. You'll master how this intricate scaffold fails, learn to decode the clinical patterns of prolapse and incontinence, and build a systematic approach to match each patient with the right diagnostic tools and treatments. By integrating structural knowledge with functional assessment, you'll transform complex urogynecologic complaints into clear therapeutic pathways that restore quality of life.
📌 Remember: SUPPORT - Sacral nerves, Urethra, Pubococcygeus, Puborectalis, Obturator internus, Rectum, Triangular ligament. These seven structures form the foundation of pelvic floor competency, with 85% of urogynecologic conditions involving dysfunction in at least three of these components.
The specialty encompasses four primary domains: stress urinary incontinence (affecting 23% of women over 40), pelvic organ prolapse (present in 41% of women over 50), overactive bladder syndrome (impacting 16.9% of the adult female population), and genitourinary fistulas (occurring in 0.1-0.2% of gynecologic surgeries in developed countries).
| Condition Category | Prevalence (%) | Peak Age Range | Primary Risk Factors | Surgical Success Rate (%) | Conservative Success Rate (%) |
|---|---|---|---|---|---|
| Stress Incontinence | 23-45 | 45-65 years | Vaginal delivery, obesity | 85-95 | 60-70 |
| Pelvic Prolapse | 41-50 | 50-70 years | Multiparity, aging | 90-95 | 45-60 |
| Overactive Bladder | 16.9-20 | 40-60 years | Neurologic, idiopathic | 70-80 | 65-75 |
| Genitourinary Fistula | 0.1-0.2 | 30-50 years | Surgical trauma | 95-98 | Not applicable |
| Mixed Incontinence | 30-35 | 50-70 years | Combined factors | 80-90 | 50-65 |
- Anatomical Precision Requirements
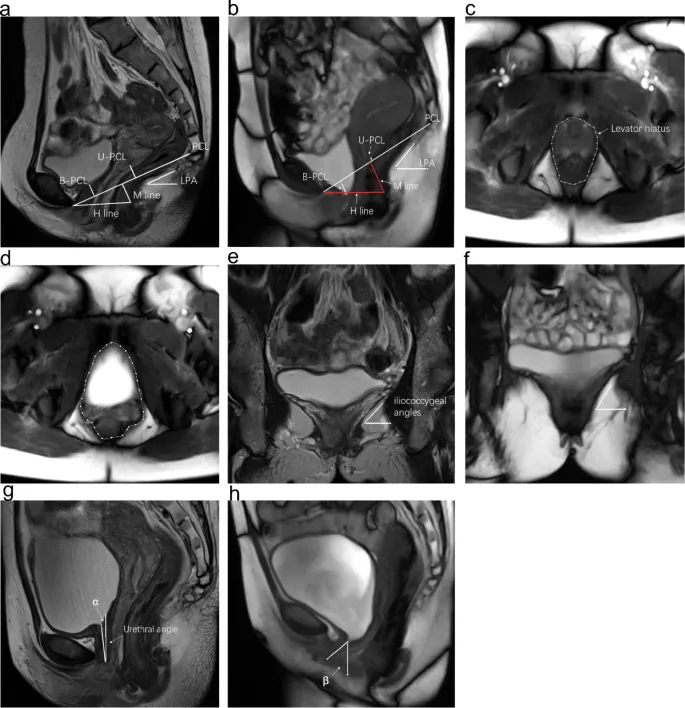
- Urethrovesical angle: 100-110 degrees (normal continent position)
- Posterior urethrovesical angle: 90-100 degrees (critical for stress continence)
- Levator hiatus area: <25 cm² (normal), >30 cm² (prolapse risk)
- Puborectalis muscle thickness: >8mm (adequate support)
- Pubovisceral muscle integrity: >75% (functional competence)
💡 Master This: Understanding the three-level support system (DeLancey's model) predicts 90% of prolapse patterns. Level I (cardinal-uterosacral complex) provides apical suspension, Level II (arcus tendineus fasciae pelvis) offers lateral attachment, and Level III (urogenital diaphragm) creates distal support. Failure patterns follow predictable sequences based on which level fails first.
The field demands integration of urodynamic parameters (detrusor pressure >15 cmH₂O, maximum flow rate >15 mL/sec, post-void residual <100 mL), imaging findings (bladder neck descent >10mm, cervical descent >6cm below ischial spines), and functional assessments (Pelvic Floor Distress Inventory scores >95, quality of life impact scores >33).

Connect these foundational principles through anatomical mastery to understand how structural relationships determine functional outcomes.
🏥 The Urogynecology Command Center: Mastering Pelvic Floor Medicine
🏗️ Architectural Blueprints: The Pelvic Support Matrix
📌 Remember: LEVEL - Level I (cardinal-uterosacral), Endopelvic fascia, Vaginal apex, Elevation mechanism, Level II (lateral attachments). Level I provides vertical suspension, Level II offers lateral stabilization, Level III creates distal closure. Each level failure produces distinct prolapse patterns with predictable symptoms.
Level I Support Architecture operates through the cardinal-uterosacral ligament complex, providing vertical suspension for the upper two-thirds of the vagina. These ligaments contain smooth muscle fibers (40% of total composition) and dense collagen bundles (35% type I collagen, 25% type III collagen) that maintain tensile strength up to 45 Newtons of force.

| Support Level | Primary Structures | Mechanical Function | Failure Pattern | Clinical Presentation | Repair Success Rate (%) |
|---|---|---|---|---|---|
| Level I | Cardinal-uterosacral complex | Vertical suspension | Apical descent | Uterine/vault prolapse | 90-95 |
| Level II | Arcus tendineus fasciae pelvis | Lateral stabilization | Paravaginal defects | Cystocele, rectocele | 85-90 |
| Level III | Urogenital diaphragm | Distal closure | Perineal weakness | Urethrocele, perineal | 80-85 |
| Combined I+II | Multiple level failure | Loss of suspension + lateral | Central defect | Severe prolapse | 85-90 |
| Combined II+III | Lateral + distal failure | Anterior/posterior weakness | Compartment prolapse | Bulge symptoms | 80-85 |
- Level II Lateral Support Mechanics
- Arcus tendineus fasciae pelvis: bilateral attachment from pubic bone to ischial spine
- Supports middle third of vagina through lateral fusion
- Paravaginal defects occur in 85% of anterior prolapse cases
- Unilateral defects: 45% of cases (usually right-sided)
- Bilateral defects: 40% of cases (severe prolapse)
- Central defects: 15% of cases (fascial weakness)
Level III Distal Support involves the urogenital diaphragm and perineal body, creating the final barrier against prolapse. The perineal body measures 3-4 cm in length and 2-3 cm in width, containing eight distinct muscle insertions that must maintain coordinated contraction during increased intra-abdominal pressure.
💡 Master This: The "Hammock Hypothesis" explains stress incontinence through Level II support failure. When paravaginal attachments weaken, the urethrovesical junction loses its stable backstop, preventing effective urethral compression during stress maneuvers. Repair must restore lateral support to achieve continence rates >85%.
- Integrated Support Failure Patterns
- Sequential failure: Level I → Level II → Level III (60% of cases)
- Combined failure: Multiple levels simultaneously (25% of cases)
- Isolated failure: Single level defect (15% of cases)
- Level I only: 5% (post-surgical)
- Level II only: 8% (paravaginal defects)
- Level III only: 2% (perineal trauma)
⭐ Clinical Pearl: Collagen composition changes predict prolapse risk. Type I:Type III collagen ratio decreases from 4:1 (normal) to 2:1 (prolapse patients). Matrix metalloproteinase activity increases 3-fold in prolapse tissue, accelerating fascial degradation and recurrence risk.
Connect this architectural understanding through functional mechanisms to understand how support failure translates into clinical symptoms and treatment targets.
🏗️ Architectural Blueprints: The Pelvic Support Matrix
⚙️ Functional Dynamics: The Continence Control System
📌 Remember: CONTINENCE - Coordination (neurologic), Outlet resistance, Neurologic reflexes, Tissue compliance, Intra-abdominal pressure, Neurologic control, External sphincter, Neurologic integration, Closure pressure, Elevation mechanisms. These ten components must function synchronously to maintain continence rates >99% during normal activities.
Neurologic Control Architecture operates through three hierarchical levels: spinal reflexes (S2-S4), pontine coordination (brainstem), and cortical modulation (frontal cortex). The pontine micturition center processes bladder filling signals every 50-100 milliseconds, maintaining storage reflexes until voluntary voiding is appropriate.

| Control Level | Neural Pathways | Response Time (ms) | Primary Function | Dysfunction Pattern | Clinical Manifestation |
|---|---|---|---|---|---|
| Cortical | Frontal-pontine | 200-500 | Voluntary control | Stroke, dementia | Urge incontinence |
| Pontine | Brainstem coordination | 50-100 | Storage/voiding switch | Multiple sclerosis | Detrusor-sphincter dyssynergia |
| Spinal | Sacral reflexes (S2-S4) | 10-50 | Basic reflexes | Spinal injury | Neurogenic bladder |
| Peripheral | Autonomic/somatic | 5-20 | Muscle activation | Diabetes, surgery | Mixed dysfunction |
| Local | Tissue mechanoreceptors | 1-10 | Pressure sensing | Aging, prolapse | Sensory urgency |
- Urethral Closure Mechanisms
- Intrinsic sphincter deficiency: urethral closure pressure <20 cmH₂O
- Anatomical support failure: urethrovesical junction hypermobility >30 degrees
- Combined mechanisms: both factors present in 45% of stress incontinence cases
- Valsalva leak point pressure: <60 cmH₂O (severe ISD), 60-90 cmH₂O (moderate), >90 cmH₂O (hypermobility)
- Maximum urethral closure pressure: <20 cmH₂O (ISD), 20-40 cmH₂O (borderline), >40 cmH₂O (normal)
Muscular Coordination Patterns require precise timing between detrusor relaxation and urethral contraction during storage, then coordinated reversal during voiding. The external urethral sphincter maintains tonic contraction at 15-25 cmH₂O, increasing to 80-120 cmH₂O during stress maneuvers.
💡 Master This: The "Integral Theory" explains stress incontinence through ligamentous laxity affecting muscle vector forces. When pubourethral ligaments stretch, the external urethral sphincter loses mechanical advantage, reducing closure pressure by 40-60% despite normal muscle strength. This explains why pelvic floor exercises alone fail in 30-40% of stress incontinence cases.
- Tissue Compliance Factors
- Collagen cross-linking: decreases 25% per decade after menopause
- Elastin content: reduces 40% in prolapse patients vs. controls
- Smooth muscle density: decreases 30% in aging urethral tissue
- Estrogen receptors: α and β subtypes present in urethral smooth muscle
- Estrogen deficiency: reduces urethral closure pressure by 20-30%
- Hormone replacement: improves tissue compliance but not continence rates
⭐ Clinical Pearl: Mixed incontinence represents dual pathophysiology: anatomical stress incontinence plus neurologic urge incontinence. Treatment must address both mechanisms - surgical correction for stress component achieves 85% success, while anticholinergic therapy for urge component adds additional 60-70% improvement in urgency symptoms.
Connect these functional mechanisms through pattern recognition frameworks to understand how pathophysiology translates into recognizable clinical presentations and diagnostic approaches.
⚙️ Functional Dynamics: The Continence Control System
🔍 Pattern Recognition Mastery: Clinical Presentation Decoding
📌 Remember: SYMPTOMS - Stress leakage, Yearning to void (urgency), Mixed patterns, Prolapse sensations, Tissue bulging, Obstructive voiding, Micturation frequency, Sexual dysfunction. These eight symptom categories create distinct patterns that predict specific anatomical defects with >85% accuracy.
Stress Incontinence Recognition Patterns present with activity-related leakage during coughing, sneezing, lifting, or exercise. The "Stress Test Triad" includes immediate leakage with cough stress test, positive Q-tip test (>30-degree deflection), and demonstrable urethral hypermobility on pelvic examination.
| Symptom Pattern | Primary Mechanism | Physical Findings | Diagnostic Accuracy (%) | First-Line Treatment | Success Rate (%) |
|---|---|---|---|---|---|
| Pure stress leakage | Urethral hypermobility | Q-tip >30°, mobile urethra | 90-95 | Pelvic floor therapy | 60-70 |
| Stress + low pressure | Intrinsic sphincter deficiency | Fixed urethra, low MUCP | 85-90 | Surgical intervention | 85-95 |
| Mixed stress/urge | Combined mechanisms | Variable findings | 80-85 | Staged treatment | 70-80 |
| Positional leakage | Severe prolapse | Visible prolapse | 95-98 | Prolapse repair | 90-95 |
| Coital incontinence | Urethral instability | Normal examination | 70-75 | Behavioral therapy | 50-60 |
- Urgency Incontinence Pattern Recognition
- Sudden, intense urge followed by involuntary leakage
- Frequency >8 voids/day, nocturia >2 episodes/night
- Key triggers: running water, cold weather, key-in-lock syndrome
- Detrusor overactivity: present in 70% of urgency cases
- Sensory urgency: 30% of cases with normal detrusor function
- Neurogenic patterns: associated conditions in 40% of patients
Prolapse Presentation Algorithms follow anatomical compartment patterns. Anterior prolapse (cystocele) presents with pelvic pressure, incomplete bladder emptying, and manual reduction to void. Posterior prolapse (rectocele) causes obstructed defecation, splinting maneuvers, and incomplete evacuation.
💡 Master This: The "Bulge Symptom Rule" states that patient-reported bulge symptoms correlate with prolapse severity better than physician examination in 75% of cases. Women who report "something coming down" have Stage II or greater prolapse in >90% of cases, making this the most reliable screening symptom.
- Advanced Pattern Recognition Strategies
- "See prolapse, think occult incontinence": 30-40% prevalence
- "See mixed symptoms, think staged treatment": address most bothersome first
- "See recurrent UTIs, think incomplete emptying": post-void residual >100 mL
- Functional obstruction: prolapse-related in 60% of cases
- Neurogenic retention: diabetes, medications in 25% of cases
- Anatomical obstruction: urethral stricture in 15% of cases
⭐ Clinical Pearl: "Red flag symptoms" require immediate evaluation: gross hematuria (rule out malignancy), recurrent UTIs (>3 per year), new-onset urgency in women >50 (neurologic causes), pelvic pain with voiding (interstitial cystitis), and continuous leakage (fistula). These patterns have <5% prevalence but >95% positive predictive value for serious pathology.
- Examination Pattern Correlations
- POP-Q Stage 0-I: rarely symptomatic (<10% bulge symptoms)
- POP-Q Stage II: symptomatic in 40-60% of patients
- POP-Q Stage III-IV: symptomatic in >90% of patients
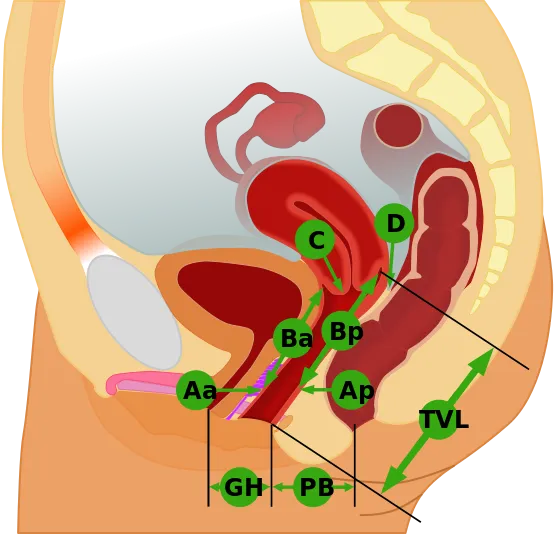
- Anterior compartment: Ba ≥0 correlates with bulge symptoms (85% sensitivity)
- Posterior compartment: Bp ≥0 correlates with defecatory dysfunction (80% sensitivity)
- Apical compartment: C ≥-3 correlates with pressure symptoms (75% sensitivity)
Connect these recognition patterns through systematic discrimination frameworks to understand how similar presentations require different treatment approaches based on underlying mechanisms.
🔍 Pattern Recognition Mastery: Clinical Presentation Decoding
⚖️ Diagnostic Discrimination: The Clinical Decision Matrix
📌 Remember: DISCRIMINATE - Detrusor function, Intrinsic sphincter, Support anatomy, Compliance factors, Residual urine, Imaging findings, Mobility testing, Incontinence severity, Neurologic status, Anatomical defects, Tissue quality, Estrogen status. These twelve parameters create diagnostic matrices that differentiate conditions with >90% accuracy.
Stress Incontinence Subtype Discrimination separates urethral hypermobility from intrinsic sphincter deficiency using quantitative parameters. This distinction determines surgical approach and predicts success rates with >90% accuracy.
| Diagnostic Parameter | Urethral Hypermobility | Intrinsic Sphincter Deficiency | Mixed Pattern | Normal Values | Clinical Significance |
|---|---|---|---|---|---|
| Q-tip Test (degrees) | >30 | <30 | Variable | <30 | Anatomical support |
| MUCP (cmH₂O) | >20 | <20 | 15-25 | >40 | Sphincter function |
| VLPP (cmH₂O) | >90 | <60 | 60-90 | >150 | Severity assessment |
| Urethral Mobility (mm) | >10 | <10 | Variable | <10 | Support integrity |
| Leak Point Pressure | High | Low | Intermediate | None | Treatment selection |
- Prolapse Severity Discrimination Criteria
- POP-Q measurements: objective staging with millimeter precision
- Functional impact: symptom severity vs. anatomical stage
- Quality of life: validated questionnaires with threshold scores
- PFDI-20 score >95: significant functional impact
- PFIQ-7 score >33: quality of life impairment
- UDI-6 score >33: urinary distress threshold
Urgency Syndrome Discrimination distinguishes detrusor overactivity, sensory urgency, and neurogenic bladder using urodynamic parameters and clinical patterns. This differentiation guides treatment selection and predicts response rates with 85% accuracy.
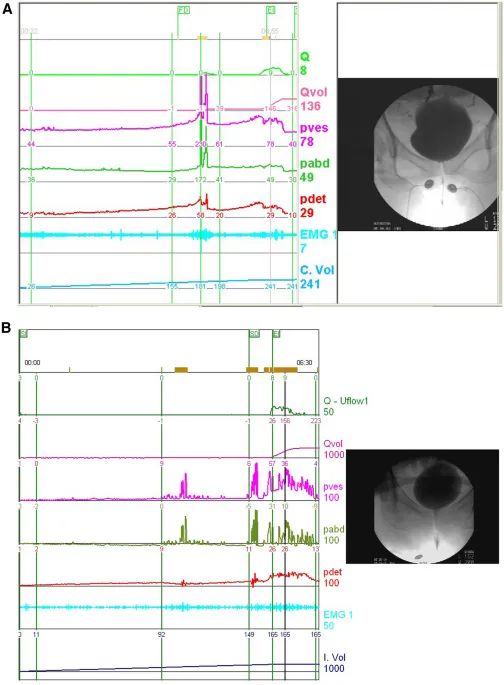
💡 Master This: Detrusor overactivity shows involuntary contractions >15 cmH₂O during filling phase, while sensory urgency demonstrates normal detrusor function with increased sensation. Neurogenic patterns exhibit detrusor-sphincter dyssynergia with elevated post-void residuals >100 mL. Treatment success rates: detrusor overactivity 75%, sensory urgency 60%, neurogenic 45%.
- Advanced Discrimination Algorithms
- Occult stress incontinence detection: pessary reduction testing
- Voiding dysfunction assessment: pressure-flow studies
- Neurologic screening: post-void residual, anal wink reflex
- Diabetes screening: HbA1c >7% increases neurogenic risk 3-fold
- Medication review: anticholinergics, alpha-blockers, diuretics
- Cognitive assessment: dementia increases urgency incontinence risk 5-fold
⭐ Clinical Pearl: "The 3-Day Voiding Diary Rule" provides more accurate diagnosis than clinical history alone in 70% of cases. Frequency >8 voids/day, nocturia >2 episodes, and urgency episodes >3/day predict detrusor overactivity with 85% sensitivity and 75% specificity. Volume patterns distinguish polyuria (>3L/day) from bladder dysfunction.
- Tissue Quality Assessment Parameters
- Estrogen status: vaginal pH >5.0 indicates deficiency
- Collagen integrity: clinical assessment of tissue friability
- Healing capacity: smoking status, diabetes control, nutrition
- Smoking: reduces healing by 40%, increases complications 2-fold
- Diabetes: HbA1c >8% doubles infection risk
- BMI >35: increases failure rates by 25-30%
Connect these discrimination frameworks through evidence-based treatment algorithms to understand how accurate diagnosis translates into optimal therapeutic outcomes.
⚖️ Diagnostic Discrimination: The Clinical Decision Matrix
🎯 Treatment Optimization: The Therapeutic Decision Engine
📌 Remember: OPTIMIZE - Objective assessment, Patient preferences, Tissue quality, Invasiveness hierarchy, Mechanism targeting, Individualized approach, Zero complications goal, Evidence-based selection. These eight principles guide treatment decisions that achieve optimal outcomes with minimal morbidity.
Conservative Management Optimization achieves success rates of 60-70% for stress incontinence and 65-75% for overactive bladder when properly implemented. The "Conservative First Rule" mandates 6-month trial before surgical intervention unless severe symptoms or patient preference dictate otherwise.
| Treatment Modality | Success Rate (%) | Time to Effect | Duration of Benefit | Patient Selection | Cost-Effectiveness |
|---|---|---|---|---|---|
| Pelvic Floor Therapy | 60-70 | 6-12 weeks | 2-5 years | Motivated patients | High |
| Bladder Training | 65-75 | 4-8 weeks | 1-3 years | Cognitive intact | High |
| Pessary Management | 70-85 | Immediate | Ongoing use | Anatomical fit | Moderate |
| Pharmacotherapy | 50-65 | 2-4 weeks | Ongoing use | No contraindications | Moderate |
| Combination Conservative | 75-85 | 8-16 weeks | 3-7 years | Compliant patients | High |
- Pharmacological Optimization Strategies
- Anticholinergic selection: based on side effect profile and patient factors
- Beta-3 agonists: mirabegron for anticholinergic intolerance
- Combination therapy: improves efficacy by 15-20% over monotherapy
- Solifenacin + mirabegron: superior efficacy with acceptable tolerability
- Dose optimization: start low, titrate slowly to minimize side effects
- Monitoring parameters: post-void residual, cognitive function, constipation

Surgical Treatment Optimization requires mechanism-specific approaches that achieve success rates >90% for appropriately selected patients. The "Right Surgery, Right Patient, Right Time" principle guides procedure selection based on anatomical defects, tissue quality, and patient factors.
💡 Master This: Retropubic midurethral slings achieve 85-95% success rates for urethral hypermobility, while transobturator slings show 80-90% success with lower voiding dysfunction rates (5% vs. 15%). Patient factors (age >70, prior surgery, tissue quality) influence approach selection and predict outcomes with >85% accuracy.
- Prolapse Repair Optimization Principles
- Apical support restoration: mandatory for durable repair
- Compartment-specific techniques: match repair to defect
- Mesh considerations: benefits vs. complications analysis
- Native tissue repair: 80-85% success, low complications
- Synthetic mesh: 90-95% success, higher complication risk
- Biologic grafts: intermediate outcomes, higher cost
⭐ Clinical Pearl: "The Apical Rule" mandates apical support restoration in all prolapse repairs to prevent recurrence. Uterosacral ligament suspension achieves 90-95% apical success, while sacrospinous fixation shows 85-90% success with higher anterior recurrence rates (15% vs. 8%).
- Complication Prevention Strategies
- Preoperative optimization: diabetes control, smoking cessation, weight management
- Surgical technique: tissue handling, hemostasis, infection prevention
- Postoperative care: early mobilization, bladder management, follow-up protocols
- Infection rates: <2% with prophylactic antibiotics
- Bleeding complications: <1% with meticulous technique
- Voiding dysfunction: <5% with appropriate sling tension
Connect these optimization principles through mastery frameworks to understand how systematic approaches create reproducible excellent outcomes in clinical practice.
🎯 Treatment Optimization: The Therapeutic Decision Engine
🏆 Clinical Mastery Arsenal: The Expert's Toolkit
📌 Remember: MASTERY - Mechanisms understood, Assessment systematic, Selection evidence-based, Technique optimized, Expertise applied, Results measured, Yield maximized. These seven principles create reproducible excellence in urogynecologic practice.
Rapid Assessment Protocol enables complete evaluation in 15-20 minutes while maintaining >95% diagnostic accuracy. The "5-Minute Rule" states that focused history and targeted examination identify primary pathology in >90% of cases.
| Assessment Component | Time Allocation (min) | Key Elements | Diagnostic Yield (%) | Clinical Decision Impact |
|---|---|---|---|---|
| Focused History | 5 | Symptom patterns, severity, impact | 85 | Treatment selection |
| Physical Examination | 8 | POP-Q, stress test, neurologic | 90 | Surgical planning |
| Basic Testing | 5 | PVR, urinalysis, cough test | 75 | Mechanism identification |
| Patient Counseling | 7 | Options, expectations, preferences | 95 | Treatment compliance |
| Documentation | 3 | Standardized forms, coding | 100 | Quality metrics |
- Expert Decision Algorithms
- Conservative vs. Surgical: symptom severity, quality of life impact, patient preference
- Surgical approach selection: mechanism, anatomy, tissue quality, prior surgery
- Complication management: early recognition, prompt intervention, outcome optimization
- Mesh complications: recognition patterns, management algorithms
- Voiding dysfunction: temporary vs. permanent, intervention thresholds
- Recurrence patterns: mechanism analysis, revision strategies
Technical Excellence Standards define performance benchmarks that achieve optimal outcomes. The "Zero Preventable Complications" goal requires systematic attention to every detail of perioperative care.
💡 Master This: "The 90-5-2 Rule" defines expert-level outcomes: >90% success rates, <5% minor complications, <2% major complications. Achieving these benchmarks requires systematic protocols, continuous monitoring, and outcome analysis with immediate feedback loops.
- Outcome Optimization Metrics
- Success definitions: objective and subjective measures
- Patient satisfaction: validated questionnaires, quality of life scores
- Complication tracking: standardized definitions, severity grading
- Clavien-Dindo classification: standardized complication grading
- Patient-reported outcomes: PFDI-20, PFIQ-7, UDI-6 scores
- Objective measures: POP-Q staging, urodynamic parameters
⭐ Clinical Pearl: "The Learning Curve Reality" shows that surgical outcomes improve significantly with experience: first 20 cases achieve 75-80% success, cases 21-50 reach 85-90%, and >50 cases achieve >90% success rates. Mentorship and structured training accelerate this progression by 40-50%.
- Quality Assurance Framework
- Outcome tracking: prospective databases, long-term follow-up
- Complication analysis: root cause identification, system improvements
- Continuous improvement: protocol refinement, technique evolution
- Benchmark comparisons: national databases, peer networks
- Patient feedback: satisfaction surveys, quality metrics
- Professional development: continuing education, skill maintenance
This comprehensive mastery toolkit provides the foundation for expert-level urogynecologic practice, enabling optimal patient outcomes through systematic excellence and evidence-based care.
🏆 Clinical Mastery Arsenal: The Expert's Toolkit
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















