FSD Overview - Defining Desire's Dip
- Female Sexual Dysfunction (FSD): Clinically significant disturbance in a woman's ability to respond sexually or experience sexual pleasure.
- Key Criteria: Causes personal distress; present for ≥ 6 months (not solely due to nonsexual mental disorder, severe relationship distress, other significant stressors, or effects of a substance/medication).
- DSM-5 Major Types:
- Female Sexual Interest/Arousal Disorder (FSIAD): Absent/reduced sexual interest, thoughts, fantasies, initiation, pleasure, or arousal (genital/non-genital).
- Female Orgasmic Disorder: Marked difficulty, infrequency, or absence of orgasm; or markedly reduced intensity of orgasmic sensations.
- Genito-Pelvic Pain/Penetration Disorder (GPPPD): Persistent/recurrent difficulties with one or more: vaginal penetration, vulvovaginal/pelvic pain during intercourse, fear/anxiety about pain, or pelvic floor muscle tensing during attempted penetration.

⭐ FSIAD is the most commonly diagnosed FSD, characterized by a significant lack of, or reduction in, sexual interest and/or arousal for at least 6 months, causing clinically significant distress to the individual.
Etiology of FSD - Unraveling the Knots
- Biological Factors:
- Hormonal: ↓Estrogen (e.g., menopause, lactation), ↓androgens, ↑prolactin, thyroid dysfunction.
- Vascular: Atherosclerosis, peripheral vascular disease (PVD) → ↓genital blood flow.
- Neurological: Multiple sclerosis (MS), diabetes (neuropathy), spinal cord injuries.
- Medications: SSRIs, antihypertensives (β-blockers, diuretics), OCPs, antiandrogens.
- Chronic illness: Diabetes mellitus, CKD. Pelvic surgery/trauma (e.g., hysterectomy).
- Psychological Factors:
- Mental health: Depression, anxiety disorders (GAD, panic), PTSD.
- Stress, negative body image, history of sexual trauma/abuse.
- Interpersonal Factors:
- Relationship discord, poor communication, partner's sexual dysfunction or health issues.
- Sociocultural Factors:
- Restrictive cultural/religious norms, lack of comprehensive sex education, societal pressures.
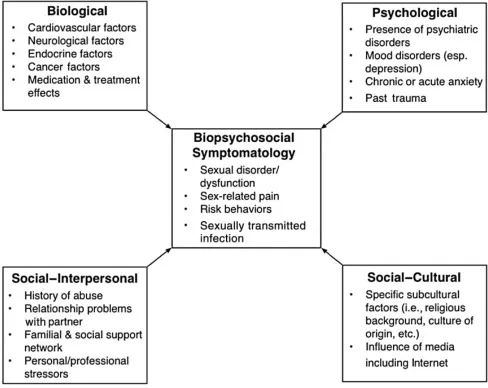
- Restrictive cultural/religious norms, lack of comprehensive sex education, societal pressures.
⭐ SSRI-induced sexual dysfunction is common; consider bupropion or mirtazapine as alternatives if FSD develops and psychiatric stability allows a switch or augmentation strategy under guidance.
History Taking in FSD - The Patient's Story
- Sexual History (DAPO 📌):
- Desire (↓libido), Arousal (↓subjective/physical), Pain (dyspareunia, vaginismus), Orgasm (anorgasmia).
- Onset, duration, severity, context.
- Partner factors: health, sexual function, relationship.
- Medical/Surgical History:
- Illnesses: DM, HTN, thyroid, neuro, depression/anxiety.
- Meds: Antihypertensives, OCPs.
⭐ SSRIs are a common iatrogenic cause of FSD, particularly affecting orgasm and libido.
- Surgeries: Pelvic, GYN, breast.
- Obstetric/Gynecologic History:
- Menopause, childbirth (trauma), lactation.
- Contraception, STIs, endometriosis.
- Psychosocial History:
- Mood disorders, stress, relationship dynamics.
- History of abuse, body image concerns.
Exam & Investigations - Clues & Corroboration
- Physical Examination:
- General: BMI, BP; signs of systemic illness (thyroid, diabetes, androgen excess).
- Pelvic Exam:
- External Genitalia: Atrophy (thinning, pallor, loss of rugae), lesions, clitoral health.
- Vaginal Mucosa: Dryness, pallor, petechiae (Genitourinary Syndrome of Menopause - GSM), discharge, pH.
- Tenderness: Q-tip test (vestibulodynia), Pelvic Floor Muscle (PFM) palpation for trigger points.
- PFM Function: Tone (hyper/hypo), Kegel strength, relaxation.
- Masses, prolapse, structural issues.
- Investigations (Guided by Findings):
- Hormonal Profile (if indicated):
- Estradiol, FSH (suspected menopause/hypoestrogenism).
- Testosterone (total & free for persistent low libido).
- TSH, Prolactin (thyroid/pituitary screen).
- Validated Questionnaires:
- Female Sexual Function Index (FSFI): Assesses 6 domains (desire, arousal, lubrication, orgasm, satisfaction, pain).
⭐ FSFI score < 26.55 strongly suggests FSD.
- Female Sexual Function Index (FSFI): Assesses 6 domains (desire, arousal, lubrication, orgasm, satisfaction, pain).
- Others (as indicated): Glucose/HbA1c, Pap smear, wet mount/cultures, pelvic USG.
- Hormonal Profile (if indicated):
High‑Yield Points - ⚡ Biggest Takeaways
- FSD evaluation uses a biopsychosocial approach for its multifactorial nature.
- Thorough history (sexual, medical, psychosocial, relationship) is key for diagnosis.
- Validated tools like FSFI (Female Sexual Function Index) quantify sexual function and distress.
- Focused physical exam detects pelvic pathology, atrophy, or pain triggers.
- Hormonal tests (estrogen, androgens, thyroid) for low libido or menopausal signs.
- Diagnosis follows DSM-5 criteria for specific disorders like FSIAD, FOD, GPPPD.
- Screen for drug side effects (e.g., SSRIs) and comorbidities (diabetes, depression).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

