Sexual Dysfunction

On this page
🔬 Sexual Dysfunction: The Intimate Physiology Breakdown
Sexual dysfunction affects up to 43% of women and 31% of men, yet remains underdiagnosed because it sits at the crossroads of vascular health, neurochemistry, psychology, and endocrinology. You'll learn to decode the physiological cascade behind arousal and orgasm, recognize distinct clinical patterns that point to specific etiologies, and build systematic approaches to differentiate organic from psychogenic causes. By mastering the neurohormonal command center and evidence-based treatment algorithms, you'll gain confidence addressing this sensitive yet critical dimension of patient health that impacts quality of life, relationships, and often signals underlying systemic disease.
📌 Remember: HOPES for sexual function assessment - Hormonal status, Orgasmic capacity, Pain presence, Emotional factors, System medications. Each component requires quantitative evaluation with specific thresholds for normal vs. dysfunction.
The sexual response cycle involves 4 distinct phases with measurable physiological parameters. During arousal, vaginal blood flow increases 3-8 fold, heart rate elevates 20-40 bpm, and genital sensitivity increases 200-400% through complex neurovascular mechanisms. These quantifiable changes provide objective markers for dysfunction assessment.
-
Desire Phase Markers
- Testosterone levels: >15 ng/dL (women), >300 ng/dL (men)
- Sexual thoughts frequency: >2-3 times weekly (normal range)
- Spontaneous arousal: Present in 60-80% of healthy individuals
- Psychological component: 70% of desire originates centrally
- Hormonal influence: 30% testosterone-dependent in both sexes
-
Arousal Phase Parameters
- Vaginal lubrication onset: 10-30 seconds (normal response)
- Clitoral engorgement: 2-3 fold increase in diameter
- Penile tumescence: >60% rigidity for functional penetration
- Vascular requirements: 25-30 mL/min arterial inflow
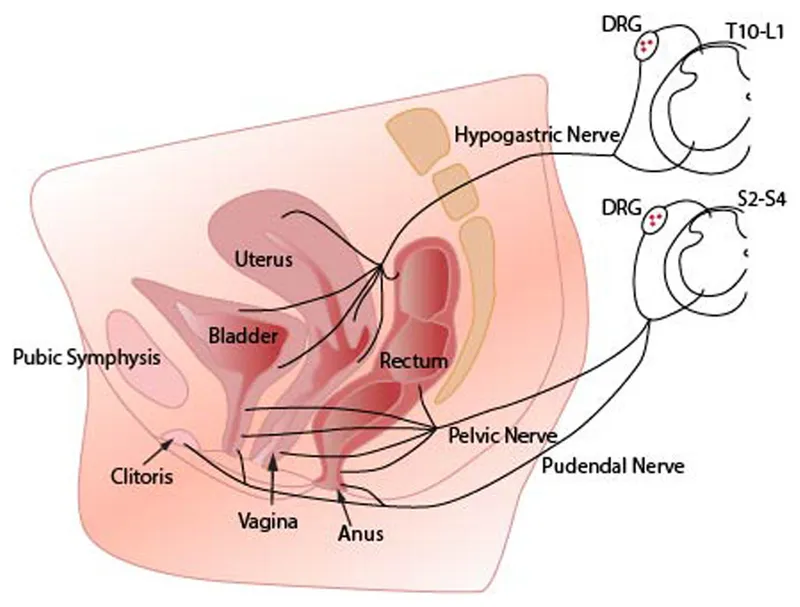
- Neurological pathway: S2-S4 parasympathetic dominance
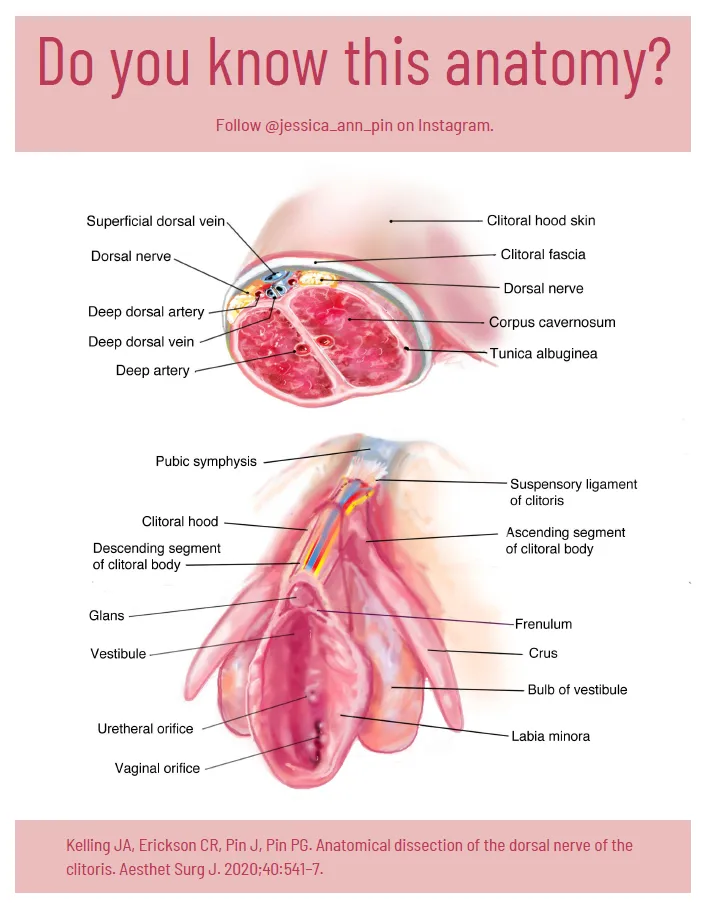
⭐ Clinical Pearl: Arousal disorders affect 12-22% of women and correlate with cardiovascular risk factors in 85% of cases. Clitoral blood flow serves as early marker for systemic endothelial dysfunction, often preceding cardiac symptoms by 2-5 years.
| Parameter | Normal Response | Mild Dysfunction | Moderate Dysfunction | Severe Dysfunction | Clinical Threshold |
|---|---|---|---|---|---|
| Lubrication Time | <30 seconds | 30-60 seconds | 1-3 minutes | >3 minutes | >2 minutes abnormal |
| Arousal Intensity | 7-10/10 scale | 5-6/10 scale | 3-4/10 scale | 0-2/10 scale | <5/10 concerning |
| Frequency Satisfaction | >75% encounters | 50-75% encounters | 25-50% encounters | <25% encounters | <50% diagnostic |
| Distress Level | Minimal | Mild concern | Moderate distress | Severe impact | Moderate+ = disorder |
| Duration Symptoms | Occasional | <3 months | 3-6 months | >6 months | >6 months = chronic |
The biopsychosocial model explains 90% of sexual dysfunction cases through interconnected factors. Biological components (hormones, vascular, neurological) account for 40-50%, psychological factors (anxiety, depression, trauma) contribute 30-40%, and social elements (relationship quality, cultural factors) influence 20-30% of presentations.

Understanding sexual dysfunction's multifactorial nature enables targeted assessment strategies that identify specific system failures and guide evidence-based interventions for optimal therapeutic outcomes.
🔬 Sexual Dysfunction: The Intimate Physiology Breakdown
🧬 Neurohormonal Command Center: The Chemical Orchestra
📌 Remember: SANTA controls sexual neurochemistry - Serotonin (inhibits), Acetylcholine (parasympathetic arousal), Norepinephrine (sympathetic orgasm), Testosterone (desire), Androgens (genital sensitivity). Balance disruption in any neurotransmitter creates specific dysfunction patterns.
-
Central Nervous System Control
- Hypothalamic nuclei: Paraventricular and supraoptic regions coordinate hormonal release
- Limbic system: Amygdala (emotional processing), hippocampus (memory integration)
- Cortical areas: Anterior cingulate (40% activation during arousal), insula (interoceptive awareness)
- Dopamine pathways: Mesolimbic reward system drives sexual motivation
- Serotonin modulation: 5-HT2A receptors (inhibitory at >80% occupancy)
-
Peripheral Autonomic Mechanisms
- Parasympathetic dominance: S2-S4 sacral nerves control arousal/lubrication
- Sympathetic activation: T11-L2 thoracolumbar manages orgasmic contractions
- Pudendal nerve: S2-S4 provides somatic sensation to external genitalia
- Nitric oxide synthesis: eNOS activation increases cGMP levels 5-10 fold
- Smooth muscle relaxation: Calcium channel modulation enables vascular engorgement
⭐ Clinical Pearl: SSRI-induced sexual dysfunction occurs in 60-70% of patients through 5-HT2A receptor overstimulation. Onset timing: 2-6 weeks after initiation. Recovery pattern: 2-4 weeks after discontinuation, but 10-15% experience persistent dysfunction lasting >3 months.
| Hormone | Normal Range | Sexual Function Role | Dysfunction Threshold | Clinical Impact | Replacement Efficacy |
|---|---|---|---|---|---|
| Testosterone (Women) | 15-70 ng/dL | Desire, arousal | <15 ng/dL | 70% libido loss | 60-80% improvement |
| Testosterone (Men) | 300-1000 ng/dL | All phases | <300 ng/dL | Progressive decline | 85-95% restoration |
| Estradiol | 30-400 pg/mL | Lubrication, tissue | <30 pg/mL | Atrophy, pain | 90% symptom relief |
| Prolactin | <25 ng/mL | Inhibitory when high | >25 ng/mL | Desire suppression | Normalize = recovery |
| DHEA-S | 35-430 μg/dL | Arousal support | <35 μg/dL | Reduced sensitivity | 40-60% benefit |
The neurotransmitter balance determines sexual response quality through opposing systems. Dopamine and norepinephrine (facilitatory) compete with serotonin and GABA (inhibitory). Medication effects predictably alter this balance-antidepressants increase serotonin (dysfunction in 60-70%), antipsychotics block dopamine (dysfunction in 40-60%).
This neurohormonal foundation provides the biochemical substrate for sexual response, setting the stage for understanding how vascular and psychological factors integrate to create functional or dysfunctional patterns in clinical presentations.
🧬 Neurohormonal Command Center: The Chemical Orchestra
🎯 Pattern Recognition Mastery: Clinical Dysfunction Signatures
Clinical pattern recognition transforms sexual dysfunction evaluation from lengthy questionnaires into efficient diagnostic frameworks. Master clinicians recognize dysfunction signatures within 5-10 minutes of focused assessment, identifying primary vs. secondary causes and system-specific failures that guide evidence-based treatment selection.
📌 Remember: DISCO pattern recognition - Duration (acute vs. chronic), Intensity (mild/moderate/severe), Situation (global vs. situational), Course (progressive vs. stable), Onset (gradual vs. sudden). Each pattern suggests different etiological pathways and treatment approaches.
-
Primary vs. Secondary Dysfunction Patterns
- Primary (lifelong): Never achieved satisfactory function, suggests anatomical/developmental causes
- Secondary (acquired): Previous normal function, indicates medical/psychological triggers
- Global vs. situational: All circumstances vs. specific situations/partners
- Global dysfunction: 80% medical etiology (hormonal, vascular, neurological)
- Situational dysfunction: 70% psychological etiology (relationship, anxiety, trauma)
-
Onset Pattern Significance
- Sudden onset (<1 month): Medication changes (60% of cases), acute stressors (25%), medical events (15%)
- Gradual onset (>6 months): Hormonal decline (40%), chronic disease (35%), relationship issues (25%)
- Progressive worsening: Vascular disease (50%), neurological conditions (30%), hormonal deficiency (20%)
- Age-related patterns: <30 years = psychological (70%), >50 years = medical (75%)
⭐ Clinical Pearl: Medication-induced dysfunction has characteristic timing patterns. SSRIs: 2-8 weeks onset, dose-dependent severity. Antihypertensives: Variable timing (days to months), beta-blockers worst (40-50% incidence). Antihistamines: Immediate anticholinergic effects on lubrication/erection.
| Dysfunction Type | Key Distinguishing Features | Primary Etiology | Response to Treatment | Diagnostic Clues | Prognosis |
|---|---|---|---|---|---|
| Desire Disorders | Low interest, absent fantasy | Hormonal (60%), psychological (40%) | 70-80% improvement | Morning testosterone <15 ng/dL | Excellent with HRT |
| Arousal Disorders | Poor lubrication/erection | Vascular (50%), neurological (30%) | 60-75% improvement | Cardiovascular risk factors | Good if reversible cause |
| Orgasmic Disorders | Delayed/absent climax | Medication (40%), psychological (35%) | 80-90% improvement | SSRI use, performance anxiety | Excellent if drug-induced |
| Pain Disorders | Dyspareunia, vaginismus | Anatomical (45%), inflammatory (35%) | 85-95% improvement | Physical exam findings | Excellent with specific treatment |
| Mixed Disorders | Multiple phase involvement | Complex multifactorial | 50-70% improvement | Multiple risk factors | Variable, requires comprehensive approach |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | |||||
| flowchart TD |
Start["🩺 Sexual Dysfunction
• Patient presentation• Initial assessment"]
Onset{"📋 Onset Pattern
• Identify timing• Sudden vs gradual"}
MedReview["💊 Medication Review
• Check new drugs• Dosage changes"]
MedScreen["🔬 Medical Screening
• Physical exam• Lab workup"]
Recent{"📋 Recent Changes
• New prescriptions• Life stressors"}
Age{"📋 Age Group
• Patient age• Risk factors"}
DrugInd["🩺 Drug-Induced
• Secondary to meds• Temporal relation"]
Stressor["🩺 Acute Stressor
• Brief duration• Situation-based"]
Psych["🩺 Psych Focus
• Mental health• Performance anxiety"]
MedFocus["🩺 Medical Focus
• Chronic issues• Comorbidities"]
MedAdj["💊 Med Adjustment
• Dose reduction• Switch agents"]
Counsel["💊 Therapy
• CBT or sex therapy• Counseling"]
Workup["🔬 Detailed Workup
• Hormonal levels• Vascular studies"]
Start --> Onset Onset -->|Sudden <1mo| MedReview Onset -->|Gradual >6mo| MedScreen MedReview --> Recent Recent -->|Yes| DrugInd Recent -->|No| Stressor MedScreen --> Age Age -->|<30 years| Psych Age -->|>50 years| MedFocus DrugInd --> MedAdj Psych --> Counsel MedFocus --> Workup
style Start fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Onset fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style MedReview fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style MedScreen fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style Recent fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Age fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style DrugInd fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Stressor fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Psych fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style MedFocus fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style MedAdj fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style Counsel fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style Workup fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C
> 💡 **Master This**: **"See sudden onset, think medication"** - **>80% of acute sexual dysfunction** relates to **new medications** or **dose changes**. **"See gradual onset in >50 years, think medical"** - **Hormonal decline**, **vascular disease**, or **chronic conditions** dominate. **"See situational pattern, think psychological"** - **Relationship issues** or **performance anxiety** create **context-dependent dysfunction**.
**Severity assessment** uses **validated scales** with **clinical correlation**. **Female Sexual Function Index (FSFI)**: **Total score <26.55** indicates **dysfunction** (sensitivity **85%**, specificity **90%**). **International Index of Erectile Function (IIEF)**: **Erectile domain <25** suggests **ED** (correlation **r=0.84** with objective measures).
These **pattern recognition frameworks** enable **rapid triage** of sexual dysfunction presentations, identifying **high-yield diagnostic pathways** that maximize **therapeutic success** while minimizing **unnecessary testing** and **treatment delays**.
🎯 Pattern Recognition Mastery: Clinical Dysfunction Signatures
🔍 Differential Diagnosis Architecture: Systematic Discrimination
Systematic differential diagnosis prevents misattribution of sexual dysfunction to single causes when multifactorial etiologies dominate >70% of presentations. Expert clinicians use hierarchical assessment frameworks that identify primary drivers while recognizing contributing factors that require concurrent management.
📌 Remember: PRIME differential framework - Psychological (anxiety, depression, trauma), Relationship (communication, conflict, intimacy), Iatrogenic (medications, procedures), Medical (hormonal, vascular, neurological), Environmental (stress, lifestyle, cultural). Most cases involve 2-3 categories requiring integrated treatment.
-
Organic vs. Psychogenic Discrimination
- Organic indicators: Gradual onset, global dysfunction, medical comorbidities, absent nocturnal erections
- Psychogenic indicators: Sudden onset, situational dysfunction, normal morning erections, relationship stressors
- Mixed presentations: >60% of cases show both components requiring dual approach
- Nocturnal penile tumescence: >60% rigidity suggests intact vascular function
- Partner-specific dysfunction: Strong psychological component likely
-
Hormonal vs. Vascular Differentiation
- Hormonal patterns: Decreased desire primary, preserved arousal if stimulated, global symptoms
- Vascular patterns: Arousal difficulties primary, preserved desire, cardiovascular risk factors
- Neurological patterns: Sensation changes, orgasmic difficulties, medical history of diabetes/MS
- Testosterone <300 ng/dL (men) or <15 ng/dL (women): Hormonal likely
- Cardiovascular disease present: Vascular component >80% probability
⭐ Clinical Pearl: Medication-induced dysfunction affects >40% of patients on psychotropic medications. SSRIs: Orgasmic delay (60-70%), decreased desire (40-50%). Antihypertensives: Erectile dysfunction (20-40%), beta-blockers worst. Antihistamines: Lubrication problems through anticholinergic effects.
| Etiology Category | Prevalence | Key Discriminators | Diagnostic Tests | Treatment Response | Recovery Timeline |
|---|---|---|---|---|---|
| Hormonal | 25-35% | Low desire, global symptoms | Testosterone, estradiol, prolactin | 70-85% improvement | 4-12 weeks |
| Vascular | 30-40% | Arousal difficulties, CV risk | Doppler, cardiovascular assessment | 60-75% improvement | 6-16 weeks |
| Neurological | 10-15% | Sensation changes, medical history | Neurological exam, EMG | 40-60% improvement | Variable |
| Psychological | 40-50% | Situational, relationship issues | Clinical interview, questionnaires | 80-90% improvement | 8-20 weeks |
| Iatrogenic | 35-45% | Temporal relationship to medications | Medication review, trial discontinuation | 85-95% improvement | 2-8 weeks |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | |||||
| flowchart TD |
Start["🍆 Sexual Dysfunction
• Patient concern• Initial intake"]
GlobalSit["📋 Activity Pattern
• Global vs Sit.• Classify context"]
Psych["🧠 Psych Assessment
• Stress/Anxiety• Relationship focus"]
Onset["⏱️ Onset Pattern
• Sudden vs Gradual• Timing check"]
MedReview["💊 Medication Review
• Check current meds• Side effect scan"]
AgeGroup["👥 Age Group
• Risk stratify• Likely causes"]
Recent["❓ Recent Changes
• New dosing• Temporal link"]
DrugInd["⚠️ Drug-Induced
• Iatrogenic cause• Dose adjustment"]
Acute["🩺 Acute Medical
• Sudden vascular• Stat evaluation"]
MedWork["🔬 Medical Workup
• Lab testing• Exam vascular"]
Hormonal["🔬 Hormonal Screen
• Endocrine check• Lab evaluation"]
VascNeuro["🩺 Vasc/Neuro
• Vascular health• Nerve status"]
TestoEstra["🧪 Serum Levels
• Testosterone• Estradiol"]
Start --> GlobalSit GlobalSit -->|Situational| Psych GlobalSit -->|Global| Onset Onset -->|Sudden| MedReview Onset -->|Gradual| AgeGroup MedReview --> Recent Recent -->|Yes| DrugInd Recent -->|No| Acute AgeGroup -->|>= 50 years| MedWork AgeGroup -->|< 50 years| Hormonal MedWork --> VascNeuro Hormonal --> TestoEstra
style Start fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style GlobalSit fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Psych fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1 style Onset fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style MedReview fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style AgeGroup fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Recent fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style DrugInd fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Acute fill:#FDF4F3, stroke:#FCE6E4, stroke-width:1.5px, rx:12, ry:12, color:#B91C1C style MedWork fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style Hormonal fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style VascNeuro fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style TestoEstra fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252
> 💡 **Master This**: **Temporal relationships** provide **diagnostic clarity**. **Dysfunction onset** within **2-8 weeks** of **medication initiation** = **>90% iatrogenic**. **Progressive worsening** over **months-years** = **medical etiology** likely. **Sudden onset** with **relationship stressor** = **psychological** component dominant. **Always assess** for **multiple contributing factors**.
**Comorbidity patterns** guide **differential diagnosis**. **Diabetes mellitus**: **Neurological dysfunction** in **35-50%**, **vascular involvement** in **60-75%**. **Depression**: **Decreased desire** in **70-80%**, **medication effects** in **60-70%**. **Cardiovascular disease**: **Erectile dysfunction** precedes **cardiac events** by **2-5 years** in **65% of cases**.
This **systematic discrimination framework** enables **accurate diagnosis** of **complex presentations**, ensuring **appropriate treatment selection** and **optimal therapeutic outcomes** through **evidence-based assessment protocols**.
🔍 Differential Diagnosis Architecture: Systematic Discrimination
⚖️ Treatment Algorithm Mastery: Evidence-Based Intervention Pathways
Treatment algorithms transform sexual dysfunction management from trial-and-error approaches into systematic interventions with predictable outcomes. Success rates improve from 40-50% with generic approaches to 75-90% with etiology-specific treatments guided by evidence-based protocols.
📌 Remember: TREAT algorithm - Target primary etiology, Review medications, Educate patient/partner, Address psychological factors, Time-limited trial with objective monitoring. Sequential approach maximizes success rates while minimizing adverse effects and treatment costs.
-
First-Line Interventions by Etiology
- Hormonal dysfunction: Testosterone replacement (70-85% success), estrogen therapy (85-95% for atrophy)
- Vascular dysfunction: PDE5 inhibitors (60-80% success), lifestyle modifications (40-60% improvement)
- Psychological dysfunction: Cognitive-behavioral therapy (80-90% success), mindfulness training (70-85% improvement)
- Combination therapy: >90% success when multiple etiologies addressed simultaneously
- Treatment duration: 8-16 weeks for psychological, 4-12 weeks for medical interventions
-
Medication Management Protocols
- SSRI-induced dysfunction: Dose reduction (40% success), drug holiday (60% success), adjunctive therapy (70% success)
- Antihypertensive optimization: ACE inhibitors/ARBs preferred (<10% dysfunction), avoid beta-blockers (40% dysfunction)
- Hormonal replacement: Bioidentical preferred, lowest effective dose, regular monitoring
- Testosterone therapy: Start 50-100 mg weekly, target 400-600 ng/dL
- Estrogen therapy: Local preferred for genital symptoms, systemic for global effects
⭐ Clinical Pearl: PDE5 inhibitor optimization requires proper education. Timing: 30-60 minutes before activity. Food effects: High-fat meals reduce absorption by 30-40%. Dose escalation: Start lowest dose, increase if <50% improvement after 4-6 attempts. Success rate: 60-80% with proper use.
| Treatment Category | First-Line Options | Success Rate | Time to Effect | Monitoring Required | Cost Considerations |
|---|---|---|---|---|---|
| Hormonal | Testosterone, estrogen | 70-85% | 4-8 weeks | Labs every 3-6 months | Moderate, insurance variable |
| Vascular | PDE5 inhibitors, lifestyle | 60-80% | 30-60 minutes | Blood pressure, cardiac | High, often not covered |
| Psychological | CBT, mindfulness therapy | 80-90% | 8-16 weeks | Symptom scales | High, limited coverage |
| Combination | Multi-modal approach | >90% | Variable | Comprehensive | Highest, best outcomes |
| Device-Based | Vacuum devices, dilators | 50-70% | Immediate | Proper technique | Moderate, one-time cost |
Second-line interventions for refractory cases include intracavernosal injections (80-90% success for ED), topical anesthetics for premature ejaculation (60-70% improvement), pelvic floor therapy for pain disorders (85-95% success). Surgical options reserved for anatomical abnormalities or failed medical management.

Treatment monitoring uses validated outcome measures and objective parameters. FSFI scores should improve >5 points, IIEF scores >4 points for clinically meaningful change. Patient-reported outcomes combined with relationship satisfaction measures provide comprehensive assessment of treatment efficacy.
This evidence-based treatment framework ensures optimal therapeutic outcomes through systematic intervention selection, appropriate monitoring, and timely adjustment of treatment protocols based on objective response measures.
⚖️ Treatment Algorithm Mastery: Evidence-Based Intervention Pathways
🔗 Multisystem Integration Hub: The Interconnected Web
Multisystem integration explains why >70% of sexual dysfunction cases involve multiple etiologies requiring comprehensive assessment and coordinated treatment approaches. Understanding system interactions enables prediction of treatment responses and identification of hidden contributing factors that limit therapeutic success.
📌 Remember: WEAVE integration model - Women's hormonal cycles, Endothelial function, Autonomic balance, Vascular health, Emotional regulation. Disruption in any system affects all others through shared pathways and feedback mechanisms. Optimal function requires system harmony.
-
Cardiovascular-Sexual Function Interface
- Endothelial dysfunction: Shared pathophysiology with erectile dysfunction and female arousal disorders
- Nitric oxide pathway: Critical for both cardiac and genital vascular function
- Risk factor overlap: Diabetes (50% sexual dysfunction), hypertension (40%), dyslipidemia (35%)
- Erectile dysfunction predicts cardiac events with 65% sensitivity
- Female arousal disorders correlate with cardiovascular risk (r=0.72)
-
Endocrine-Neurological Integration
- Testosterone effects: Neural plasticity, neurotransmitter synthesis, receptor sensitivity
- Estrogen functions: Neuroprotection, serotonin modulation, tissue maintenance
- Stress hormone impact: Cortisol elevation suppresses HPG axis and sexual response
- Chronic stress: 30-40% reduction in testosterone production
- Depression: Bidirectional relationship with sexual dysfunction (r=0.68)
⭐ Clinical Pearl: Metabolic syndrome creates perfect storm for sexual dysfunction. Insulin resistance reduces nitric oxide bioavailability (40-50% decrease), abdominal obesity increases aromatase activity (testosterone conversion to estrogen), chronic inflammation impairs endothelial function. Weight loss of >10% improves sexual function in 60-70% of cases.
| System Interaction | Mechanism | Clinical Impact | Assessment Markers | Intervention Strategy | Success Predictors |
|---|---|---|---|---|---|
| Cardio-Sexual | Shared NO pathway | ED predicts CAD | Flow-mediated dilation | Lifestyle + PDE5i | CV risk reduction |
| Neuro-Endocrine | Hormone-receptor modulation | Mood affects libido | Testosterone + mood scales | Combined HRT + therapy | Hormone normalization |
| Psycho-Somatic | Stress-hormone axis | Anxiety impairs arousal | Cortisol + anxiety measures | Stress reduction + medical | Stress management success |
| Metabolic-Vascular | Insulin resistance effects | Diabetes complications | HbA1c + lipid profile | Glycemic control + statins | Metabolic improvement |
| Inflammatory-Neural | Cytokine-mediated damage | Chronic disease impact | CRP + inflammatory markers | Anti-inflammatory approach | Inflammation reduction |
Aging effects demonstrate multisystem integration complexity. Testosterone decline (1-2% annually after age 30) affects muscle mass, bone density, mood, and sexual function. Estrogen deficiency impacts cardiovascular health, cognitive function, bone metabolism, and genital tissues. Replacement therapy provides multisystem benefits beyond sexual function improvement.
Medication effects illustrate system interconnections. Antidepressants affect serotonin (sexual inhibition), autonomic function (arousal impairment), and hormonal regulation (prolactin elevation). Antihypertensives influence vascular function (erectile capacity), autonomic balance (arousal response), and energy levels (desire motivation).
Treatment integration requires coordinated approaches addressing multiple systems simultaneously. Lifestyle interventions (exercise, nutrition, stress management) provide broad benefits across all systems. Targeted therapies (hormonal, vascular, psychological) address specific deficits while supporting overall function.
This multisystem perspective transforms sexual dysfunction management from symptom treatment into comprehensive health optimization, achieving superior outcomes through integrated care approaches that address root causes and system interactions.
🔗 Multisystem Integration Hub: The Interconnected Web
🎯 Clinical Mastery Arsenal: Rapid Assessment & Intervention Tools
Clinical mastery transforms complex sexual dysfunction presentations into manageable assessment frameworks that maximize diagnostic accuracy while minimizing patient discomfort and consultation time. Expert practitioners achieve >85% diagnostic accuracy within 10-15 minutes using systematic approaches and validated tools.
📌 Remember: RAPID assessment framework - Review medications/medical history, Assess relationship/psychological factors, Perform focused physical exam, Identify primary etiology, Develop targeted treatment plan. Each component provides specific diagnostic information guiding evidence-based interventions.
-
Essential Clinical Arsenal
- 5-minute screening: FSFI-6 (women) or IIEF-5 (men) for rapid dysfunction identification
- Medication review: Focus on psychotropics (60-70% dysfunction), antihypertensives (20-40%), antihistamines (variable)
- Targeted history: Onset pattern, situational factors, relationship quality, medical comorbidities
- Red flags: Sudden onset + medication change, progressive worsening + cardiovascular risk
- Green flags: Situational dysfunction + relationship stressor, preserved morning erections
-
Physical Examination Priorities
- Cardiovascular: Blood pressure, peripheral pulses, cardiac rhythm (vascular dysfunction screening)
- Genital: Anatomical abnormalities, tissue quality, sensation testing (organic pathology identification)
- Neurological: Reflexes, sensation, muscle tone (neurological dysfunction assessment)
- Time investment: <5 minutes for focused exam vs. 15-20 minutes for comprehensive assessment
- Diagnostic yield: Abnormal findings in 25-30% guide specific interventions
⭐ Clinical Pearl: Laboratory efficiency maximizes diagnostic yield. Essential tests: Total testosterone (morning), HbA1c (diabetes screening), lipid panel (cardiovascular risk). Additional tests based on clinical suspicion: Prolactin (decreased desire), TSH (fatigue/mood), PSA (men >50). Cost-effective approach: $200-300 vs. $800-1200 for comprehensive panels.
| Assessment Tool | Time Required | Diagnostic Accuracy | Clinical Application | Cost | Interpretation Threshold |
|---|---|---|---|---|---|
| FSFI-6 | 2-3 minutes | 85% sensitivity | Female screening | Free | <19 suggests dysfunction |
| IIEF-5 | 2-3 minutes | 90% sensitivity | Male screening | Free | <22 suggests dysfunction |
| Medication Review | 3-5 minutes | 95% for iatrogenic | All patients | Free | Temporal relationship key |
| Focused Exam | 5-8 minutes | 70% for organic | Suspected pathology | Minimal | Abnormal findings significant |
| Basic Labs | 1 day results | 80% for hormonal | Age >40 or symptoms | $200-300 | Reference range dependent |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | |||||
| flowchart TD |
Start["👤 Patient Intake
• Patient presents• Initial evaluation"]
Screening["⏱️ Screening
• 5-min screening• Quick assessment"]
Decision{"❓ Positive?
• Screen results• Check criteria"}
Reassurance["✅ Reassurance
• Provide education• Patient comfort"]
Assessment["📋 Assessment
• Focused review• Clinical status"]
MedReview["💊 Med Review
• Current drugs• Check interactions"]
History["📖 History
• Targeted details• Medical record"]
PhysExam["🩺 Physical Exam
• Focused exam• Clinical signs"]
Labs["🔬 Lab Tests
• Order diagnostics• Review results"]
TxPlan["🏥 Treatment Plan
• Finalize therapy• Next steps"]
Start --> Screening Screening --> Decision Decision -->|No| Reassurance Decision -->|Yes| Assessment Assessment --> MedReview MedReview --> History History --> PhysExam PhysExam --> Labs Labs --> TxPlan
style Start fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Screening fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Decision fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Reassurance fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252 style Assessment fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style MedReview fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534 style History fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style PhysExam fill:#F7F5FD, stroke:#F0EDFA, stroke-width:1.5px, rx:12, ry:12, color:#6B21A8 style Labs fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style TxPlan fill:#F1FCF5, stroke:#BEF4D8, stroke-width:1.5px, rx:12, ry:12, color:#166534
> 💡 **Master This**: **Treatment monitoring** requires **objective measures**. **Baseline scores** (FSFI/IIEF) establish **dysfunction severity**. **4-week follow-up**: **Assess tolerance** and **early response**. **12-week evaluation**: **Measure efficacy** using **validated scales**. **Success criteria**: **>5-point FSFI improvement** or **>4-point IIEF improvement** indicates **clinically meaningful change**.
**Rapid intervention protocols** optimize **treatment efficiency**. **First-line approaches**: **Medication adjustment** (iatrogenic), **hormone replacement** (deficiency), **PDE5 inhibitors** (vascular), **counseling referral** (psychological). **Response timeline**: **2-4 weeks** (medications), **4-8 weeks** (hormones), **8-16 weeks** (therapy).
**Clinical decision support** tools enhance **diagnostic accuracy**. **Smartphone apps** with **validated questionnaires**, **drug interaction checkers**, and **treatment algorithms** provide **point-of-care assistance**. **Electronic health records** with **embedded screening tools** and **automated reminders** improve **assessment consistency**.
**Patient education resources** accelerate **treatment success**. **Standardized handouts** explaining **normal sexual function**, **common causes** of **dysfunction**, and **treatment options** reduce **consultation time** while **improving understanding**. **Online resources** and **support groups** provide **ongoing education** and **peer support**.
This **clinical mastery arsenal** enables **efficient**, **accurate**, and **comprehensive** sexual dysfunction management, achieving **optimal patient outcomes** through **systematic assessment**, **evidence-based treatment**, and **objective monitoring** of **therapeutic responses**.
🎯 Clinical Mastery Arsenal: Rapid Assessment & Intervention Tools
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




















