Ovulation Induction: Basics & Workup - Sparking the Start
- Goal: Induce follicular development & ovulation for conception.
- Indications:
- Anovulation (e.g., WHO Groups I, II)
- Unexplained infertility
- Controlled Ovarian Stimulation (COS) for ART (IUI/IVF)
- Essential Workup:
- History (menstrual, medical), BMI
- Hormonal: Day 2/3 FSH, LH, E2; Prolactin, TSH, AMH (ovarian reserve)
- Transvaginal Ultrasound (TVS): Antral Follicle Count (AFC), uterine/adnexal pathology
- Semen analysis (partner)
- Tubal patency tests (e.g., HSG, HyCoSy)
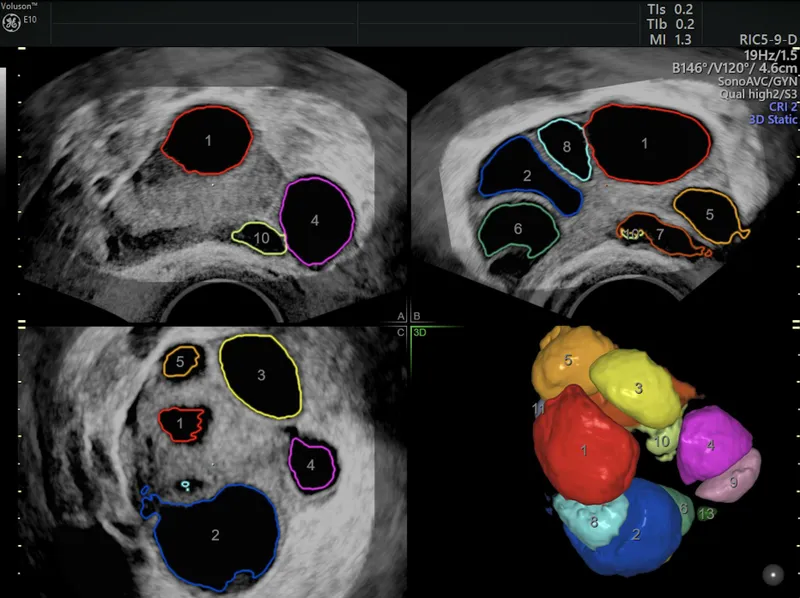
⭐ WHO Group II anovulation (e.g., Polycystic Ovary Syndrome - PCOS) is the most common cause of anovulatory infertility and typically responds well to first-line oral ovulation induction agents like clomiphene citrate or letrozole.
Ovulation Induction: Key Drugs - The Ovary Orchestra
| Drug | MOA | Typical Regimen | Key Pointers |
|---|---|---|---|
| Clomiphene Citrate | SERM, ↑FSH/LH | 50-150mg/d x 5d (start D2-5) | Hot flashes; visual disturbances (stop); multiple pregnancy ~5-10%; thin endometrium |
| Letrozole | Aromatase Inhibitor, ↓E₂ → ↑FSH | 2.5-7.5mg/d x 5d (start D2-5) | Preferred in PCOS; monofollicular; better endometrial profile; arthralgia |
| Gonadotropins (FSH) | Direct ovarian stimulation | Variable, SC/IM | CC failure, hypogonadotropic hypogonadism; Higher OHSS & multiple pregnancy risk |
| hCG | LH surge mimic | 5000-10000IU IM/SC (follicle 18-20mm) | Triggers ovulation; given post follicular maturation |
Ovulation Induction: Protocols & Monitoring - The Ovulation Roadmap
- Protocols:
- Clomiphene Citrate (CC): 50-100 mg/day x 5 days (from Day 2-5).
- Letrozole: 2.5-5 mg/day x 5 days (from Day 2-5); preferred in PCOS.
- Gonadotropins (FSH, hMG): Step-up/Step-down protocols; dose individualized.
- Monitoring:
- Transvaginal Sonography (TVS): Follicular growth (serial), endometrial thickness (target ≥7-8 mm).
- Serum E2 levels: Assess follicular response.
- Ovulation Trigger (hCG/GnRH Agonist):
- Criteria: Dominant follicle 18-22 mm, adequate endometrium.
- hCG: 5,000-10,000 IU IM/SC.

⭐ Letrozole is often the first-line agent for ovulation induction in PCOS women, associated with higher live birth rates and lower multiple pregnancy rates compared to clomiphene.
Ovulation Induction: Complications & Nuances - Navigating the Hurdles
- Ovarian Hyperstimulation Syndrome (OHSS):
- ⚠️ Risks: PCOS, young, high AMH/AFC, E2 >3500 pg/mL.
- Features: Ovarian enlargement, ascites, hemoconcentration (Hct >45%).
- Prevention: GnRH antagonist, cabergoline, "freeze-all".
- Management: Supportive, IV fluids, albumin, paracentesis.
- Multiple Pregnancies:
- Risk with all agents; highest with gonadotropins.
- Mitigation: Low-dose protocols, cycle cancellation, SET (IVF).
- Resistant Cases:
- Clomiphene Resistance (~15-40%): No ovulation with 150mg/day.
- Options: Letrozole, gonadotropins, ovarian drilling (PCOS).
- PCOS & Monitoring:
- Letrozole: First-line in PCOS. Metformin adjunct.
⭐ Letrozole is superior to clomiphene for ovulation induction in PCOS, with higher live birth rates. 💡 Crucial: Monitor follicular growth (USG) & E2 to prevent OHSS/multiples.
 oka
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Clomiphene Citrate (CC) is first-line for WHO Group II anovulation (e.g., PCOS).
- Letrozole, an aromatase inhibitor, is often preferred for PCOS; higher live birth rates, monofollicular development.
- Gonadotropins (hMG, rec-FSH) for WHO Group I anovulation or CC/Letrozole resistance.
- hCG injection mimics LH surge, triggering final oocyte maturation and ovulation.
- Ovarian Hyperstimulation Syndrome (OHSS): key risk with gonadotropins and hCG trigger.
- Pulsatile GnRH: physiological for WHO Group I anovulation, but less common_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

