Definition & Physiology - Androgen Excess 101
- Hyperandrogenism: Clinical (e.g., hirsutism, acne, alopecia) or biochemical evidence of elevated androgen levels.
- Principal Androgens & Sources:
- Testosterone (T): Primarily ovarian & adrenal; potent.
- DHEAS (Dehydroepiandrosterone sulfate): Exclusively adrenal; weak androgen, but good marker.
- Androstenedione (A4): Ovarian & adrenal; precursor to T.
- Peripheral conversion in skin/adipose tissue also contributes to active androgens.
⭐ 5α-reductase converts testosterone to dihydrotestosterone (DHT), a more potent androgen, primarily in target tissues like hair follicles and skin.
Etiology & Clinical Features - Causes & Hairy Signs
Common Causes & Differentiating Features:
| Feature | PCOS | Late-Onset CAH | Androgen-Secreting Tumor |
|---|---|---|---|
| Onset | Peri-pubertal, gradual | Peri-pubertal, gradual | Rapid, any age (post-pubertal) |
| Virilization | Usually absent/mild hirsutism | Mild-moderate hirsutism | Often severe, rapid |
| Key Lab | ↑LH/FSH, ↑Testo (mild-mod) | ↑17-OHP (baseline/post-ACTH) | Markedly ↑Testo or DHEAS |
Other Etiologies:
- Adrenal: Cushing's Syndrome
- Drugs: Danazol, Valproate, Steroids
- Endocrine: Hyperprolactinemia, Hypothyroidism
- Idiopathic Hirsutism: Normal androgens, ↑skin sensitivity
Clinical Features (Spectrum of Androgen Excess):
- Hirsutism:
- Excess terminal hair (male pattern: face, chest, back)
- Ferriman-Gallwey score >8.
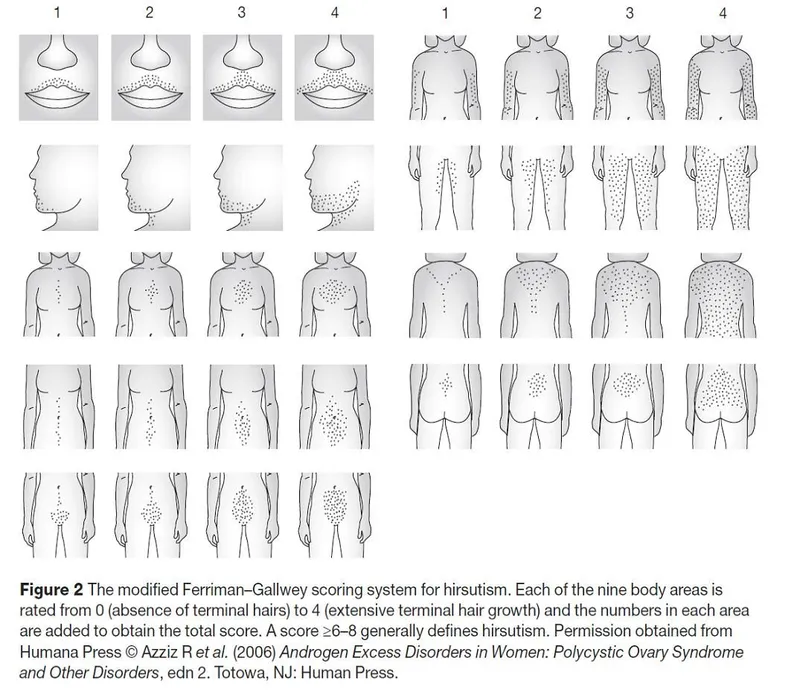
- Cutaneous Signs:
- Acne, Seborrhea
- Androgenic alopecia (temporal, vertex thinning)
- Menstrual Dysfunction:
- Oligo/amenorrhea
- Virilization (Red Flag: Tumor/Severe Excess):
- Clitoromegaly (>10mm length)
- Voice deepening
- ↑Muscle mass, male habitus
- Breast atrophy
Diagnostic Workup - Unmasking the Source
-
History & Exam: Assess symptom onset/progression (hirsutism, acne, alopecia). Note signs of virilization (clitoromegaly, voice deepening, muscle mass ↑).
-
Initial Key Labs:
- Total Testosterone (T)
- DHEA-S (Adrenal marker)
- 17-hydroxyprogesterone (17-OHP) (early morning, follicular phase)
-
Diagnostic Algorithm:
-
Further Tests (if indicated): Prolactin, TSH, Cushing's screen (e.g., 1mg overnight dexamethasone suppression test).
⭐ Basal 17-OHP >200 ng/dL warrants an ACTH stimulation test for Non-Classical Congenital Adrenal Hyperplasia (NCAH); a post-ACTH 17-OHP level >1000-1500 ng/dL is diagnostic.
Management Approaches - Taming the Hormones
- Lifestyle Modification: Weight loss (≥5% of body weight) in PCOS improves insulin sensitivity & hyperandrogenism.
- Cosmetic Measures: For hirsutism (e.g., laser, electrolysis, eflornithine cream).
- Pharmacological Therapy:
- Oral Contraceptive Pills (OCPs): First-line for menstrual regulation & hirsutism. Suppress LH, ↑SHBG.
- Anti-androgens: Added if OCP response is inadequate after 6 months.
- Spironolactone: 50-200 mg/day. Androgen receptor blocker. ⚠️ Monitor K+.
- Finasteride: 5 mg/day. 5α-reductase inhibitor (Type 2).
- Metformin: For PCOS with metabolic syndrome, impaired glucose tolerance (IGT), or Type 2 Diabetes Mellitus (T2DM).
- GnRH Agonists: (e.g., Leuprolide) For severe refractory hyperandrogenism (e.g., ovarian hyperthecosis).
⭐ Combined oral contraceptives (OCPs) are the first-line medical therapy for both hirsutism and menstrual cycle disturbances in women with Polycystic Ovary Syndrome (PCOS).
High‑Yield Points - ⚡ Biggest Takeaways
- PCOS is the most common cause; use Rotterdam criteria (2 of 3) for diagnosis.
- Manifests as hirsutism (Ferriman-Gallwey), acne, alopecia, and menstrual irregularity.
- Key labs: total testosterone, DHEAS; 17-OHP to exclude late-onset CAH.
- Rapid virilization (clitoromegaly, voice change) signals possible androgen-secreting tumor.
- Treatment: lifestyle changes, OCPs (first-line), spironolactone or other anti-androgens.
- Insulin resistance is a frequent comorbidity, especially with PCOS.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

