Menstrual Cycle: Definitions & Phases - Cycle Rhythms
- Normal Menstrual Cycle (Eumenorrhea):
- Interval: 21-35 days (average 28 days).
- Duration of flow: 2-7 days (average 4-5 days).
- Volume of blood loss: 20-80 mL (average 35 mL). >80 mL is menorrhagia.
- Cycle Phases (Interlinked):
- Ovarian Cycle:
- Follicular Phase (variable): Follicle growth, estrogen ↑.
- Ovulation: LH surge, oocyte release (Day 14 in 28-day cycle).
- Luteal Phase (fixed 14 days): Corpus luteum, progesterone ↑.
- Uterine (Endometrial) Cycle:
- Menstrual Phase: Endometrial shedding.
- Proliferative Phase: Endometrial regrowth (estrogen-driven).
- Secretory Phase: Endometrial maturation (progesterone-driven).
- Ovarian Cycle:
- Rhythm: Infradian (cycle >24h), orchestrated by HPO axis.
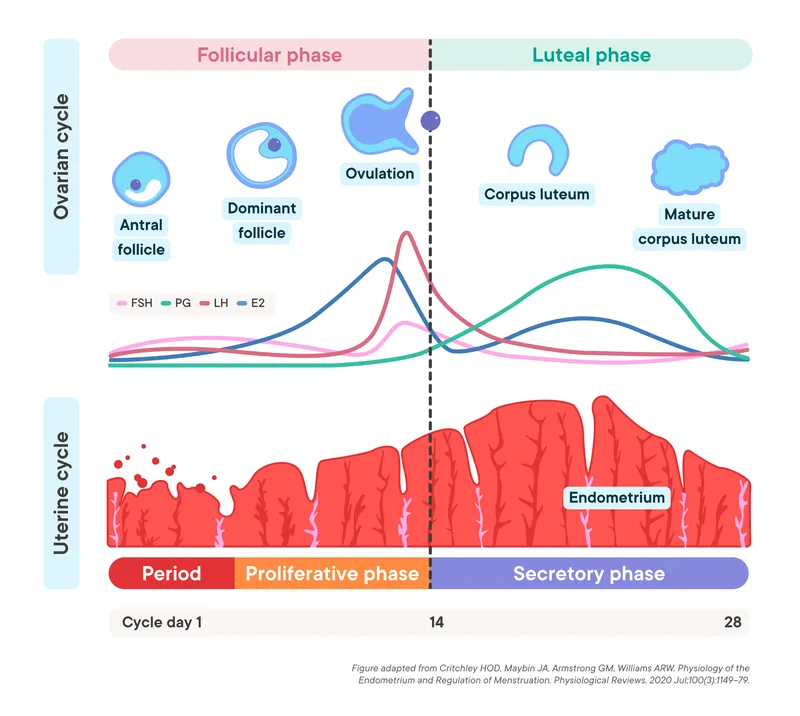
⭐ The luteal phase is consistently 14 days; variations in cycle length are primarily due to follicular phase duration.
HPO Axis: Regulation & Feedback - Brain-Ovary Chat
- Orchestration: Hypothalamus-Pituitary-Ovarian (HPO) axis governs menstrual cycle.
- Hypothalamus: Pulsatile Gonadotropin-Releasing Hormone (GnRH).
- Slow pulses favor FSH release.
- Fast pulses favor LH release.
- Anterior Pituitary: GnRH stimulates secretion of:
- FSH: Ovarian follicle growth, estrogen (E2) production.
- LH: Ovulation, corpus luteum, progesterone (P4) production.
- Ovarian Hormones & Feedback:
- Estrogen (E2):
- Low/moderate levels: Negative feedback on Hypothalamus/Pituitary (↓GnRH, ↓FSH, ↓LH).
- Sustained high levels (pre-ovulatory): Positive feedback on Pituitary → LH surge.
- Progesterone (P4): Negative feedback on Hypothalamus/Pituitary.
- Inhibin (from granulosa cells): Selectively ↓FSH secretion from pituitary.
- Activin (from granulosa cells): Stimulates ↑FSH secretion from pituitary.
- Estrogen (E2):
⭐ LH surge (for ovulation) needs sustained high E2 (>200 pg/mL for ~48-50 hrs).
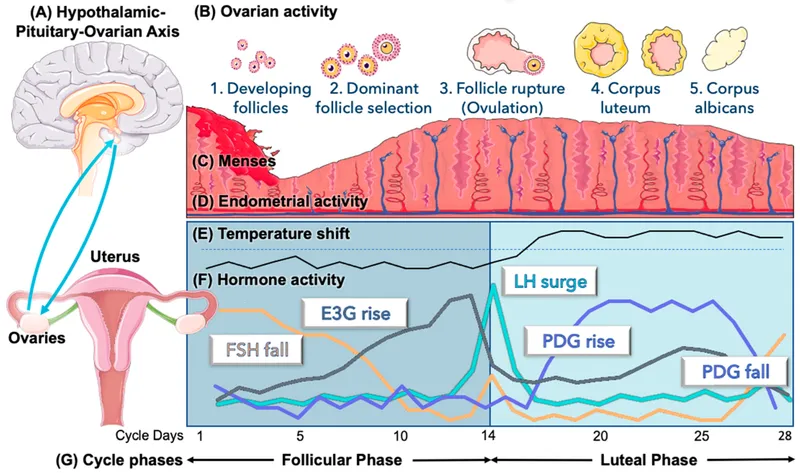
Ovarian Cycle: Folliculogenesis & Luteinization - Egg's Big Show
- Folliculogenesis (FSH-driven):
- Primordial follicle → Primary → Secondary → Graafian (mature) follicle.
- Granulosa cells: convert androgens (from LH-stimulated theca cells) to estrogen (E2).
- One dominant follicle emerges.
- Ovulation (LH surge-triggered):
- Caused by sustained ↑E2 from dominant follicle (positive feedback).
- Oocyte released ~10-12 hrs post-LH peak, 24-36 hrs post-E2 peak.
- ⭐ > The LH surge is essential for final oocyte maturation (meiosis I completion) and ovulation.
- Luteinization (LH maintains):
- Corpus Luteum (CL) forms from follicle remnants.
- Produces progesterone (P4; dominant) & estrogen. P4 prepares endometrium.
- CL lifespan: ~14 days. If no pregnancy → luteolysis (corpus albicans) → ↓P4, E2 → menses.
- If pregnancy: hCG rescues CL.
Endometrial Cycle: Proliferation & Secretion - Monthly Makeover

-
Cyclical endometrial changes driven by ovarian hormones. Two main phases post-menstruation:
-
1. Proliferative Phase (Days ~5-14; Follicular Phase)
- Hormone: ↑ Estrogen.
- Endometrium: Regenerates stratum functionalis; thickness ↑ to 3.5-5 mm.
- Glands: Straight, tubular; mitoses.
- Arteries: Spiral arteries lengthen.
-
2. Secretory Phase (Days ~15-28; Luteal Phase)
- Hormone: ↑ Progesterone (Estrogen present).
- Endometrium: Thickens to 5-6 mm (up to 14 mm).
- Glands: Tortuous ("saw-tooth"), dilated; secrete glycogen.
- Stroma: Edematous; predecidual changes.
- Arteries: Spiral arteries coil.
- 📌 Progesterone = Prepares for Pregnancy.
⭐ Peak endometrial receptivity for implantation: days 20-24 (6-10 days post-ovulation).
-
Menstruation: If no implantation, ↓ Estrogen & Progesterone → spiral artery spasm → ischemia → shedding of stratum functionalis (superficial 2/3rds).
High‑Yield Points - ⚡ Biggest Takeaways
- The Hypothalamic-Pituitary-Ovarian (HPA) axis orchestrates the menstrual cycle.
- Pulsatile GnRH from hypothalamus stimulates pituitary FSH and LH.
- FSH promotes follicular maturation and estrogen synthesis, causing endometrial proliferation.
- A mid-cycle LH surge is the critical trigger for ovulation.
- The corpus luteum, post-ovulation, secretes progesterone for secretory endometrium.
- Menstruation results from progesterone withdrawal if no pregnancy.
- Normal cycle: 21-35 days; menses: 2-7 days; blood loss: <80 mL.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

