Management Approaches to Menstrual Disorders - Charting the Chaos
- Initial Assessment: Detailed history (menstrual, medical, family), physical exam (general, pelvic).
- Investigations:
- Lab: CBC, TSH, PRL, hCG. Consider coagulation profile, androgens if indicated.
- Imaging: Pelvic USG (transvaginal preferred).
- Hysteroscopy/Endometrial biopsy: If structural pathology suspected or >45 yrs / risk factors for endometrial hyperplasia/cancer.
- General Management:
- Lifestyle: Weight management, stress reduction, exercise.
- Symptomatic relief: NSAIDs for dysmenorrhea.
- Medical Management (Hormonal):
- Combined Oral Contraceptives (COCs)
- Progestins (oral, injectable, IUD - Mirena)
- GnRH agonists (with add-back therapy)
- Medical Management (Non-Hormonal):
- Tranexamic acid (for HMB)
- NSAIDs (Mefenamic acid)
- Surgical Management: Indicated for structural lesions or failed medical therapy.
- Hysteroscopic procedures (polypectomy, myomectomy)
- Endometrial ablation
- Hysterectomy (definitive)

⭐ Levonorgestrel-releasing IUD (Mirena) is highly effective for heavy menstrual bleeding (HMB), reducing blood loss by up to 80-95% and providing contraception. (📌 Mirena: Manages Increased REd Nuisance Amounts!)
Management Approaches to Menstrual Disorders - Pill & Potion Power
Medical management is tailored to the specific disorder, severity, and patient preference.
- Key Medications:
- 📌 HMB Meds: "Treat Heavy Menses Now" (Tranexamic acid, Hormonal [COCs, Progestogens], Mirena [LNG-IUS], NSAIDs)
- NSAIDs:
- Mefenamic Acid: 500mg TDS (HMB, Dysmenorrhea)
- Ibuprofen: 400-600mg TDS (Dysmenorrhea)
- Antifibrinolytics:
- Tranexamic Acid: 1g TDS (or 10-15mg/kg TDS) for HMB. Max 4g/day.
⭐ LNG-IUS (Mirena) is highly effective for HMB, reducing blood loss by up to 80-95% within 3-6 months.
- Tranexamic Acid: 1g TDS (or 10-15mg/kg TDS) for HMB. Max 4g/day.
- Combined Oral Contraceptives (COCs):
- Cyclic or continuous use for HMB, Dysmenorrhea, Cycle regulation, PMS.
- Progestogens:
- Norethisterone: 5mg TDS (days 5-26 for HMB; or luteal phase for 10-14 days).
- Medroxyprogesterone Acetate (MPA): Oral or depot.
- LNG-IUS (Mirena): HMB, contraception.
- SSRIs:
- Fluoxetine, Sertraline for PMS/PMDD (continuous or luteal phase).
- GnRH Agonists:
- Severe HMB/Endometriosis (e.g., Leuprolide, Goserelin) with add-back therapy (to mitigate hypoestrogenic side effects).
Management Approaches to Menstrual Disorders - Precision Procedures
- Dilation & Curettage (D&C)
- Diagnostic: endometrial sampling for AUB.
- Therapeutic: retained products, temporary HMB relief.
- Hysteroscopy
- Gold standard for intrauterine pathology (polyps, fibroids).
- Operative: polypectomy, submucosal myomectomy, adhesiolysis.
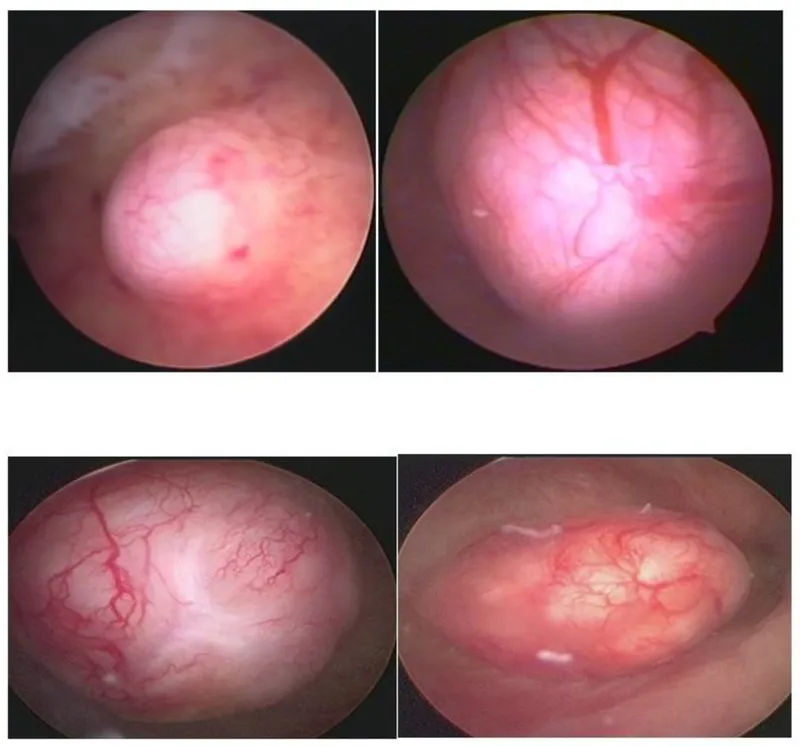
- Endometrial Ablation
- For HMB; fertility not desired.
- Techniques: thermal, radiofrequency, cryoablation.
- Avoid if endometrial hyperplasia/cancer.
- Uterine Artery Embolization (UAE)
- Minimally invasive for symptomatic fibroids (HMB).
- Myomectomy
- Surgical fibroid removal; preserves uterus & fertility.
- Hysterectomy
- Definitive for severe/refractory AUB, large fibroids, cancer.
⭐ Hysteroscopy is the gold standard for diagnosing and treating intrauterine abnormalities like polyps or submucous fibroids causing AUB.
High‑Yield Points - ⚡ Biggest Takeaways
- NSAIDs (Mefenamic acid) are first-line for dysmenorrhea & reducing HMB.
- COCs regulate cycles, ↓ HMB, & manage PCOS irregularities.
- Progestins are key for anovulatory bleeding, HMB, & endometrial protection.
- LNG-IUS is highly effective for HMB & long-term contraception.
- GnRH agonists treat severe endometriosis/fibroids by inducing temporary menopause.
- Tranexamic acid is effective for HMB if hormones are contraindicated.
- Surgery (ablation, hysterectomy) for refractory cases or structural issues_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

