Urogenital Atrophy - Estrogen's Adieu
- Definition (GSM): Genitourinary Syndrome of Menopause: collection of symptoms/signs from $\downarrow$ estrogen & other sex steroid changes affecting labia, clitoris, vestibule/introitus, vagina, urethra, bladder.
- Epidemiology: Affects up to 50-70% of postmenopausal women; often underreported and undertreated.
- Pathophysiology: Estrogen decline $\rightarrow$
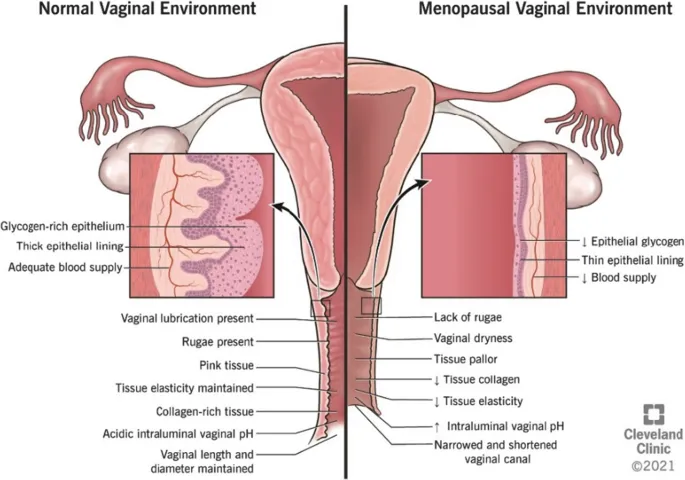
- Thinned vaginal epithelium: $\downarrow$ glycogen, $\downarrow$ superficial cells, $\uparrow$ parabasal cells.
- $\downarrow$ Collagen & elastin, $\downarrow$ vascularity.
- $\uparrow$ Vaginal pH (>5.0).
- Altered vaginal microbiota: $\downarrow$ Lactobacilli.
- Urinary Tract Effects: Similar atrophic changes in urethra and bladder trigone $\rightarrow$ urgency, dysuria, recurrent UTIs.
⭐ GSM is preferred over 'vulvovaginal atrophy' or 'atrophic vaginitis' as it better reflects the full spectrum of genitourinary involvement.
Clinical Features - Dry Spells & Drips
📌 Mnemonic: SAD LIPS (Sexual dysfunction, Atrophy, Dryness, Lubrication decrease, Itching, Pain, Soreness).
- Symptoms:
- Genital: Dryness (most common), burning, irritation, itching, dyspareunia (superficial/entry), postcoital bleeding.
- Urinary (LUTs): Dysuria, frequency, urgency, nocturia, recurrent UTIs, stress incontinence (may worsen).
- Sexual: ↓ lubrication, pain/discomfort, arousal difficulties, ↓ libido (often secondary).
⭐ Dyspareunia is a hallmark symptom of GSM, significantly impacting quality of life.
- Signs on Examination:
- Vulva: Loss of labial fat/turgor, sparse pubic hair, introital stenosis/narrowing.
- Vagina: Pale, dry, smooth (loss of rugae) mucosa; friability, petechiae; prominent parabasal cells on wet mount.
- Urethra: Urethral caruncle, eversion, prolapse; meatal tenderness.
 oka
oka
Diagnosis & Differentials - Spotting the Signs
- Clinical: Symptoms (dryness, dyspareunia, urinary) + signs (pale, thin mucosa) in postmenopausal women (not on ET).
- Supportive Tests (often not needed):
- Vaginal pH: > 5.0 (Normal premenopausal: $3.5-4.5$)
- Vaginal Maturation Index (VMI): <5% superficial cells, ↑parabasal cells.
- Wet Mount: Rules out infection; shows ↑WBCs, ↑parabasal cells.
- Urine culture: If UTI symptoms.
⭐ A vaginal pH > 5.0 in a postmenopausal woman is highly suggestive of Genitourinary Syndrome of Menopause (GSM).
Differential Diagnoses (DDx):
- Infections: Candidiasis, Bacterial Vaginosis (BV), Trichomoniasis.
- Dermatoses: Lichen sclerosus, Lichen planus, Eczema.
- Irritant/Allergic dermatitis.
- Vulvodynia/Vestibulodynia.
- Desquamative Inflammatory Vaginitis (DIV).
- Neoplasia (VIN, VaIN; rare, persistent/atypical symptoms).
Management - Oasis Restoration
Goals: Relieve symptoms, restore urogenital physiology, improve Quality of Life (QoL).
- Non-Hormonal (First-line for mild symptoms):
- Vaginal moisturizers: Regular use (e.g., polycarbophil, hyaluronic acid).
- Vaginal lubricants: Coitally/as needed (water, silicone, oil-based).
- Lifestyle: Continued sexual activity, avoid irritants, pelvic floor PT.
- Hormonal Therapy (Most effective for moderate-severe GSM):
- Local Estrogen Therapy (LET) - Preferred for isolated GSM:
- Forms: Creams (conjugated estrogens 0.625mg/g, estradiol 0.01%), tablets (estradiol 10mcg, 4mcg), rings (estradiol 7.5mcg/day).
- Dosing: Initial daily for 1-2 weeks, then maintenance 2-3 times/week. (e.g., Estradiol 10mcg vaginal tablet).
- Minimal systemic absorption; progestin generally NOT required with low-dose LET (uterus intact).
- Systemic Estrogen Therapy (ET/HT): If concomitant vasomotor symptoms. Requires progestin if uterus intact.
- Local Estrogen Therapy (LET) - Preferred for isolated GSM:
- Other FDA-Approved Therapies:
- Ospemifene: Oral SERM (60mg daily). Estrogen agonist on vagina. Risks: hot flushes, VTE.
- Prasterone (Intrarosa®): Intravaginal DHEA (6.5mg daily). Local conversion.
- Emerging: Laser (CO2, Er:YAG), Radiofrequency - evidence evolving.

⭐ Low-dose vaginal estrogen therapy is the gold standard for symptomatic GSM and has an excellent safety profile with minimal systemic absorption.
High‑Yield Points - ⚡ Biggest Takeaways
- Urogenital atrophy (UGA), also known as Genitourinary Syndrome of Menopause (GSM), is primarily caused by estrogen deficiency post-menopause.
- Common symptoms include vaginal dryness, dyspareunia, pruritus, urinary urgency, dysuria, and recurrent UTIs.
- Clinical signs: pale, thin, dry vaginal mucosa, loss of rugae, and petechiae.
- Vaginal pH is elevated (typically > 5.0), reflecting altered flora.
- Microscopy shows an increased proportion of parabasal cells and a decrease in superficial cells.
- First-line treatment is low-dose topical estrogen; vaginal moisturizers and lubricants offer symptomatic relief.
- It is a chronic and progressive condition if left untreated, significantly impacting quality of life.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

