Cardiovascular Health in Menopause - Heart's Hormonal Shift
- Menopause: Defined as the permanent cessation of menstruation resulting from the loss of ovarian follicular activity. Typically confirmed after 12 consecutive months of amenorrhea.
- Average Age of Onset (India): 46-47 years (Global average: ~51 years).
- Increased CVD Risk: Post-menopause sees a significant ↑ in cardiovascular disease (CVD) risk.
- Key contributor: Estrogen withdrawal, which adversely impacts:
- Lipid profiles (↑LDL, ↑Total Cholesterol; ↓HDL)
- Endothelial function & vascular tone
- Inflammatory markers (e.g., ↑CRP)
- Blood pressure & coagulation factors
- Key contributor: Estrogen withdrawal, which adversely impacts:
- Primary Mortality Cause:
⭐ Cardiovascular disease (CVD) is the leading cause of mortality in postmenopausal women, surpassing all cancers combined.
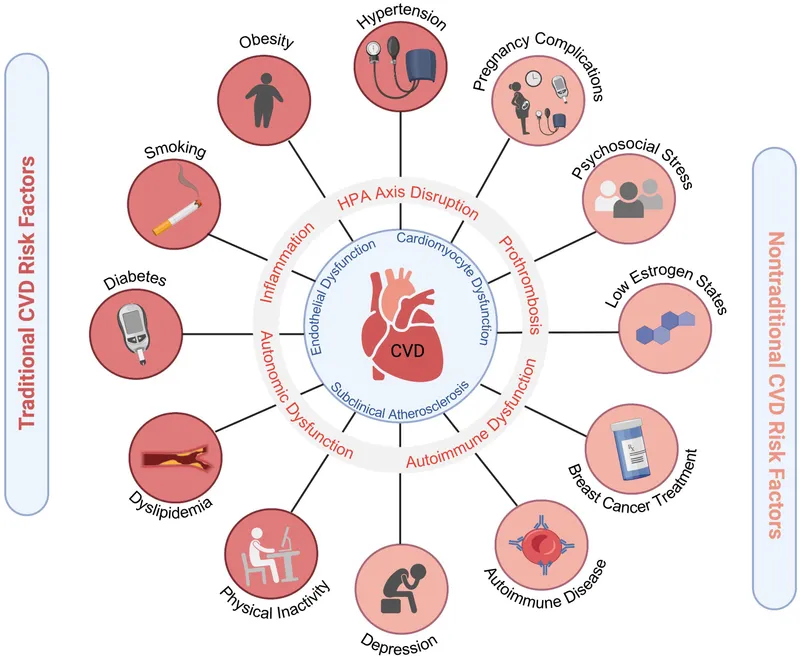
Cardiovascular Health in Menopause - Vessel Vulnerability

-
Impact of ↓Estrogen:
- Endothelial Dysfunction: ↓ $NO$, ↑ Endothelin-1.
- Vascular Inflammation: ↑ CRP, ↑ cytokines.
- Coagulation: Prothrombotic changes.
- Arterial Stiffness: ↑ (e.g., ↑ pulse wave velocity).
-
Lipid Profile Alterations:
Lipid Parameter Change Post-Menopause Total Cholesterol ↑ LDL-C ("Bad") ↑ HDL-C ("Good") ↓ Triglycerides (TG) ↑
⭐ Estrogen withdrawal leads to a more atherogenic lipid profile, characterized by increased LDL-C and decreased HDL-C.
📌 Mnemonic: Estrogen LOW = Lipids HIGH, Vessels STIFF.
Cardiovascular Health in Menopause - Danger Signals & Screening
Menopause significantly ↑ cardiovascular disease (CVD) risk. Early identification of danger signals & proactive screening is crucial.
Key Risk Factors:
| Category | Risk Factors | Implication |
|---|---|---|
| Traditional (Amplified) | Hypertension (BP > 130/80 mmHg), Diabetes, Dyslipidemia (LDL > 100 mg/dL, HDL < 50 mg/dL), Smoking, Obesity (BMI > 23 kg/m² for South Asians), Family Hx (premature CVD) | Estrogen withdrawal worsens these pre-existing or new-onset factors. |
| Menopause-Specific | Premature menopause (<40 yrs), Early menopause (40-45 yrs), Severe/frequent Vasomotor Symptoms (VMS), PCOS history, Adverse pregnancy outcomes (GDM, preeclampsia) | Directly linked to hormonal changes & earlier/accelerated vascular aging. |
- Regularly screen for traditional CVD risk factors.
- Inquire about menopause-specific risk factors.
- Be vigilant for atypical CVD symptoms in women: fatigue, dyspnea, nausea, indigestion, jaw/neck/back pain. These differ from classic angina.
⭐ Women experiencing premature menopause (before age 40) have a significantly higher risk of developing coronary heart disease.
Cardiovascular Health in Menopause - Guardian Guidelines
- Lifestyle Modification is Key:
- Diet: Emphasize DASH or Mediterranean patterns.
- Exercise: Regular, moderate-intensity activity.
- Smoking cessation; achieve/maintain healthy weight.
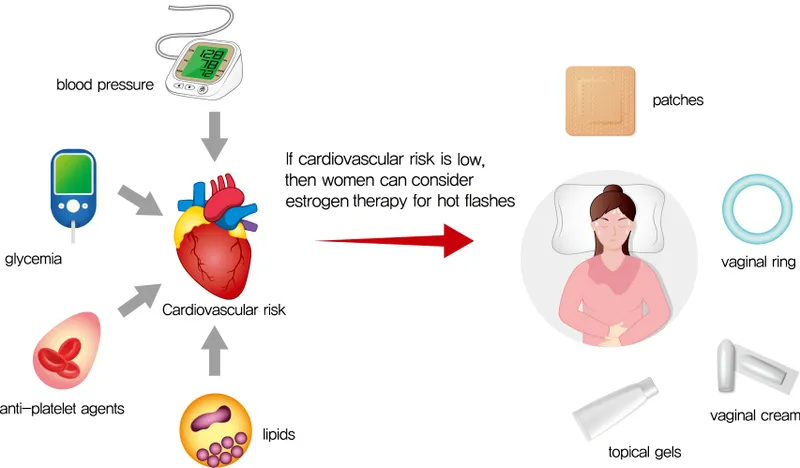
- Hormone Replacement Therapy (HRT):
- 📌 HRT Timing: Early Bird gets the Benefit (for CV).
- 'Window of opportunity': Initiate if <60 years old OR within 10 years of menopause for Vasomotor Symptom (VMS) relief & potential CV benefits/neutrality. Later start may ↑risk.
- Risks: Venous Thromboembolism (VTE), breast cancer (type/duration dependent).
- Contraindications: History of breast/endometrial cancer, VTE, active liver disease, undiagnosed vaginal bleeding, established Coronary Artery Disease (CAD).
- Non-Hormonal Options for VMS: SSRIs, SNRIs, gabapentin.
- Cardiovascular Risk Factor Management:
- Dyslipidemia: Statins as indicated.
- Hypertension: ACE inhibitors (ACEi) / Angiotensin II Receptor Blockers (ARBs) often first-line.
- Diabetes: Optimal glycemic control.
- Aspirin: For primary/secondary prevention based on individual risk assessment and guidelines.
⭐ The 'timing hypothesis' suggests that HRT initiated early in menopause (e.g., within 10 years of onset and/or age <60) may have cardiovascular benefits or be neutral, while later initiation might be harmful.
High‑Yield Points - ⚡ Biggest Takeaways
- Estrogen withdrawal at menopause adversely affects cardiovascular physiology, increasing risk.
- Risk of Coronary Artery Disease (CAD), myocardial infarction, and stroke significantly ↑.
- Unfavorable lipid profile: ↑Total Cholesterol, ↑LDL, ↑Triglycerides, and often ↓HDL.
- Increased incidence of hypertension, endothelial dysfunction, and arterial stiffness.
- Metabolic syndrome prevalence rises, compounding overall cardiovascular disease (CVD) risk.
- Hormone Therapy (HT) for CVD prevention is complex; timing hypothesis is key.
- Primary prevention via lifestyle changes (diet, exercise, no smoking) is crucial.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

