Hypertensive Disorders - Pressure Cooker Pregs
- Types:
- Chronic HTN: BP $\ge$ 140/90 mmHg <20 wks.
- Gestational HTN (GHTN): BP $\ge$ 140/90 mmHg >20 wks, no proteinuria.
- Preeclampsia (PE): GHTN + Proteinuria (PCR $\ge$ 0.3 or $\ge$300mg/24h) OR end-organ damage.
- Severe features: BP $\ge$ 160/110 mmHg, Plt <100k, $\uparrow$LFTs, Cr >1.1mg/dL, pulm edema, neuro sx.
- Eclampsia: PE + Seizures.
- HELLP Syndrome: Hemolysis, Elevated Liver enzymes, Low Platelets.
- Management:
- Antihypertensives: Labetalol, Nifedipine, Methyldopa. ⚠️ Avoid ACEi/ARBs.
- Severe PE/Eclampsia: MgSO4 (IV 4-6g load, 1-2g/hr maint.). Delivery.
⭐ Therapeutic range for MgSO4 in preeclampsia/eclampsia is 4.8-8.4 mg/dL (4-7 mEq/L). Loss of patellar reflex (DTRs) occurs at ~10 mEq/L (toxicity).
Diabetes in Pregnancy - Sweet Baby Saga
- Types: Pregestational (PGDM), Gestational (GDM - onset in pregnancy).
- GDM Screening (24-28 wks):
- DIPSI (India): 75g OGTT (non-fasting); 2hr PG ≥140 mg/dL.
- IADPSG: 75g OGTT (fasting). Dx if: FPG ≥92 OR 1hr PG ≥180 OR 2hr PG ≥153 mg/dL.
- Glycemic Targets: FPG <95; 1hr PP <140; 2hr PP <120 mg/dL. $HbA_{1c}$ <6-6.5%.
- Management Algorithm:
- Maternal Risks: Preeclampsia, polyhydramnios, infections, ↑CS rate.
- Fetal Risks:
- PGDM (early exposure): Congenital anomalies (cardiac, caudal regression).
- GDM/PGDM: Macrosomia, RDS, neonatal hypoglycemia, hypocalcemia.

⭐ GDM mothers: significantly increased risk of future Type 2 DM. Postpartum screening & lifestyle modification are vital counseling points.
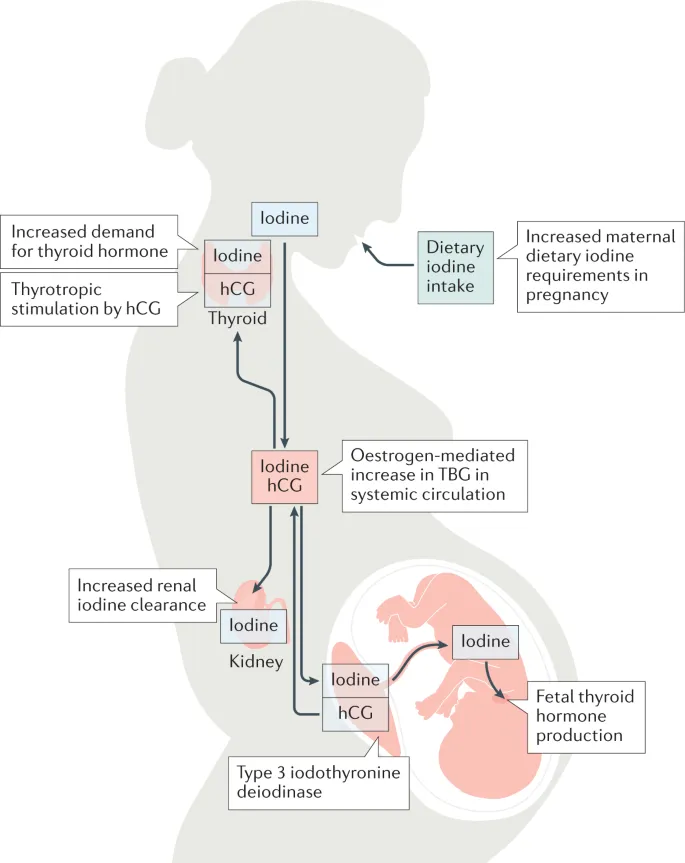
Thyroid Disorders - Gland Central Drama
- Physiology: ↑TBG, ↑Total T4/T3. hCG → transient ↓TSH (1st tri).
- Hypothyroidism:
- Screen high-risk. TSH goals: <2.5 $mIU/L$ (1st tri), <3.0 $mIU/L$ (2nd/3rd).
- Rx: Levothyroxine; ↑ dose 25-30%. Monitor TSH.
- Risks: Cretinism, preeclampsia.
- Hyperthyroidism (Graves'):
- ↓TSH, ↑FT4. TRAb+.
- Rx: 📌 PTU (1st tri - Pregnant Trimester Use), then MMI. See flowchart. Goal: High-normal FT4.
- Risks: IUGR, preterm, storm.
- Radioactive iodine: NO.
- Postpartum Thyroiditis: Transient hyper/hypo.
⭐ Universal screening for thyroid dysfunction in pregnancy is controversial; targeted screening for high-risk women is widely accepted.
Anemia & VTE - Blood Tales Trouble
-
Anemia in Pregnancy:
- WHO: Hb <11 g/dL (1st/3rd trimesters), <10.5 g/dL (2nd). Physiological hemodilution.
- Iron Deficiency Anemia (IDA) most common. Screen: Booking & 28 weeks.
- Rx IDA: Oral iron (e.g., Ferrous sulfate 200mg TID). Folic acid 0.4mg daily; 5mg if high-risk (e.g., prior NTD, antiepileptics).
- Parenteral iron if severe/intolerant.
-
Venous Thromboembolism (VTE):
- ↑Risk: Virchow's triad (hypercoagulability, stasis, endothelial injury). Peak risk: Postpartum (first 6 weeks).
- 📌 Key RFs (POTIMAS): Previous VTE, Obesity (BMI >30), Thrombophilia, Immobility, Multiparity, Age >35, Surgery (esp. C-section).
- Prophylaxis (high-risk): LMWH (e.g., Enoxaparin 40mg SC OD).
- Treatment: Therapeutic LMWH (e.g., Enoxaparin 1mg/kg SC BD). Warfarin contraindicated.
⭐ LMWH is the anticoagulant of choice in pregnancy as it does not cross the placenta and has a better safety profile than unfractionated heparin.
High‑Yield Points - ⚡ Biggest Takeaways
- Intrahepatic Cholestasis of Pregnancy (ICP): Ursodeoxycholic acid (UDCA) is the drug of choice.
- Gestational Diabetes Mellitus (GDM): Insulin is preferred; Metformin can be used. OGTT for diagnosis.
- Hypertension in Pregnancy: Labetalol, Nifedipine, Methyldopa are safe. ACE inhibitors/ARBs are contraindicated.
- Thyroid Disorders: PTU in 1st trimester for hyperthyroidism, then Methimazole. Levothyroxine for hypothyroidism, dose often ↑.
- Epilepsy in Pregnancy: Levetiracetam, Lamotrigine are safer. High-dose folic acid (5mg) is crucial.
- Asthma in Pregnancy: Inhaled corticosteroids (ICS) like Budesonide are safe and preferred for control; avoid exacerbations.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

