Physiological Thyroid Changes - Hormonal High Jinks
- Estrogen ↑ → Thyroxine-Binding Globulin (TBG) ↑ → Total T4 & T3 ↑. Free T4/T3 usually normal.
- hCG (TSH-like activity): Stimulates thyroid → T4/T3 ↑; transient TSH ↓ (esp. 1st trimester, nadir 10-12 wks).
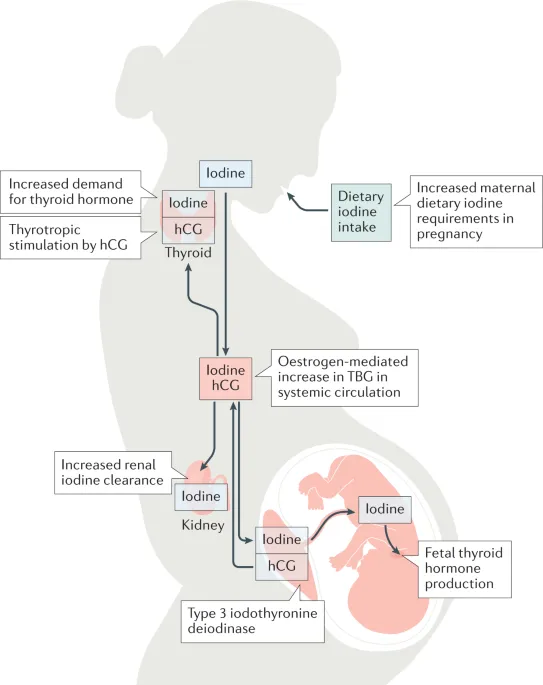
- Iodine: Demand ↑ (due to ↑ renal clearance & fetal needs).
- Placenta: ↑ Deiodinase activity (converts T4 to rT3).
- Net effect: Euthyroid state maintained by ↑ thyroid hormone production. Gland may ↑ size by 10-15%.
⭐ Trimester-specific TSH reference ranges are crucial: 1st trimester <2.5 mIU/L, 2nd <3.0 mIU/L, 3rd <3.0-3.5 mIU/L.
Maternal Hypothyroidism - Slow Mo Mama
- Definition: Inadequate thyroid hormone production during pregnancy.
- Screening: TSH in 1st trimester or early pregnancy.
- TSH > 2.5 mIU/L (1st trimester).
- TSH > 3.0 mIU/L (2nd/3rd trimester).
- Causes: Hashimoto's thyroiditis (most common, Anti-TPO Ab+), iodine deficiency, prior thyroidectomy/radioiodine.
- Risks (Maternal): Miscarriage, preeclampsia, placental abruption, PPH.
- Risks (Fetal/Neonatal): Preterm birth, LBW, neurodevelopmental impairment (↓IQ).
- Management:
- Levothyroxine (L-T4).
- Pre-existing Rx: ↑ L-T4 dose by 30-50% upon pregnancy confirmation.
- New diagnosis: Start L-T4 (e.g., overt: 1-2 mcg/kg/day; subclinical: 25-75 mcg/day).
- Target TSH: < 2.5 mIU/L (1st tri), < 3.0 mIU/L (2nd/3rd tri).
- Monitor TSH every 4-6 weeks.
⭐ Untreated maternal hypothyroidism is associated with an increased risk of neurodevelopmental deficits in the offspring, including lower IQ.
Maternal Hyperthyroidism - Speedy Spurt
- Most common: Graves' disease (TRAb). Also: Gestational Transient Thyrotoxicosis (hCG).
- Risks:
- Mother: Miscarriage, preeclampsia, preterm labor, heart failure, thyroid storm.
- Fetus: IUGR, prematurity, goiter, fetal/neonatal hyperthyroidism (TRAb).
- Dx: ↓TSH, ↑FT4/FT3. TRAb+ in Graves'.
- Goal: FT4 upper normal range (maternal euthyroidism).
- ATD Therapy:
- 1st Trimester: Propylthiouracil (PTU) (100-300 mg/day).
- 2nd/3rd Trimesters: Methimazole (MMI) (5-20 mg/day).
- Adjunct: Propranolol for symptoms.
- Surgery (thyroidectomy): 2nd trimester if ATDs fail/CI.
- ⚠️ Radioiodine (RAI) contraindicated.
- Thyroid Storm: PTU, Iodides, β-blockers, Steroids.
- Postpartum: Monitor for flares.
⭐ Propylthiouracil (PTU) is preferred in the first trimester due to MMI's risk of embryopathy (e.g., aplasia cutis, choanal/esophageal atresia). MMI is preferred in 2nd/3rd trimesters due to lower risk of PTU-induced hepatotoxicity.
Postpartum Thyroiditis & Iodine - Aftermath & Essentials
- Postpartum Thyroiditis (PPT): Autoimmune thyroiditis, 1-12 months post-delivery.
- Often triphasic: thyrotoxicosis → hypothyroidism → euthyroidism.
- Management: β-blockers (thyrotoxic), Levothyroxine (hypothyroid if TSH >10/symptomatic).
- Risk factors: T1DM, prior PPT, TPOAb+.
- Iodine: Essential for fetal neurodevelopment.
- RDA: Pregnancy 250 mcg/day, Lactation 290 mcg/day.
- Sources: Iodized salt, seafood, dairy.
⭐ Postpartum thyroiditis typically presents with a triphasic course: transient hyperthyroidism, followed by hypothyroidism, and then usually euthyroidism, though permanent hypothyroidism can occur in 20-30% of cases.
High‑Yield Points - ⚡ Biggest Takeaways
- Physiological changes: ↑TBG, ↑Total T4/T3. TSH ↓ in 1st trimester (hCG effect).
- Hypothyroidism (Hashimoto's): ↑Levothyroxine dose by ~30%. TSH goal <2.5 mIU/L (1st tri), <3.0 mIU/L (later).
- Untreated maternal hypothyroidism risks cretinism and adverse obstetric outcomes.
- Hyperthyroidism (Graves'): PTU (1st tri), MMI (2nd/3rd tri). Risk of thyroid storm.
- Postpartum thyroiditis: Occurs within 1 year postpartum, often triphasic.
- Iodine requirements are significantly ↑ during pregnancy; screen high-risk women for dysfunction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

