Adrenal Physiology in Pregnancy - Hormonal Hullabaloo
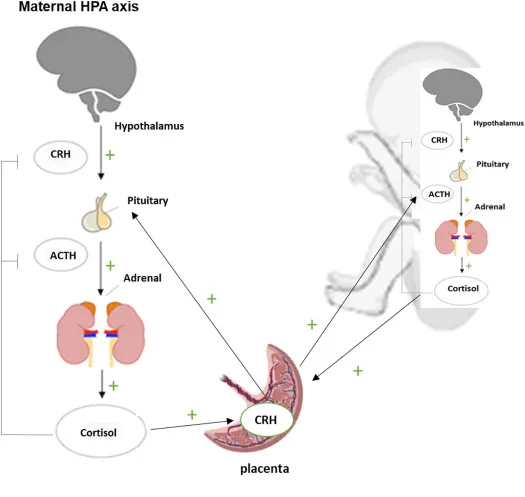
- HPA Axis: Negative feedback largely intact. Placental CRH ↑, especially in late pregnancy.
- Cortisol: Total cortisol ↑ significantly (2-3x) due to estrogen-driven ↑ Cortisol Binding Globulin (CBG). Free cortisol remains normal or slightly ↑. Diurnal rhythm is maintained but blunted.
- CBG (Transcortin): ↑ due to estrogen, leading to ↑ total cortisol carrying capacity.
- Aldosterone: ↑ progressively (RAAS activation; progesterone antagonism). Levels can be 5-10x non-pregnant values by term.
- DHEAS: ↓ during pregnancy, partly due to ↑ placental clearance and conversion to estrogens.
⭐ Pregnancy is a state of physiologic hypercortisolism due to increased estrogen stimulating Cortisol Binding Globulin (CBG) production, leading to higher total cortisol but normal or slightly elevated free cortisol.
Cushing's Syndrome in Pregnancy - Cortisol Chaos
- Etiology: Adrenal adenoma most common; pituitary (Cushing's disease) rare.
- Clinical Features: Overlap with pregnancy (weight gain, striae). Specific: proximal myopathy, easy bruising, facial plethora, HTN, new glucose intolerance.
- Diagnostic Challenges & Tests (Interpretation in Pregnancy):
- 24-hr UFC: Normal pregnancy (mild ↑); Cushing's (markedly ↑, >3x non-preg ULN).
- Late-night salivary cortisol: Normal pregnancy (stable/slight ↑); Cushing's (significantly ↑).
- LDDST (1mg): Normal pregnancy (variable suppression); Cushing's (no suppression, cortisol >1.8 µg/dL or 50 nmol/L).
- ACTH: Low in adrenal adenoma.
- Maternal Complications: GDM, preeclampsia, infections.
- Fetal Complications: IUGR, preterm birth, neonatal adrenal suppression.
- Management: Surgery (adrenalectomy, 2nd tri. ideal for adenoma) or Metyrapone (preferred).
⭐ The most common cause of Cushing's syndrome during pregnancy is an adrenal adenoma; pituitary causes (Cushing's disease) are rare.

Adrenal Insufficiency in Pregnancy - Energy Emergency
- Types & Causes:
- Primary (Addison's): Autoimmune, TB.
- Secondary: Pituitary dysfunction, chronic steroid withdrawal.
- Clinical Features: Hypotension, fatigue, nausea/vomiting, weight loss. Hyperpigmentation (primary, may be subtle if recent onset).
- Diagnosis: ↓AM cortisol, ↑ACTH (primary). ACTH stimulation test: post-ACTH cortisol <18-20 mcg/dL or <500 nmol/L.
- Management:
- Glucocorticoid (e.g., Hydrocortisone) & Mineralocorticoid (Fludrocortisone for primary) replacement.
- Stress Doses: Crucial for labor/delivery/illness. Hydrocortisone 50-100mg IV/IM q6-8h during labor.
- Adrenal Crisis: Precipitated by stress/infection. Severe hypotension, shock, hypoglycemia.
- Manage: IV fluids (Normal Saline), IV Hydrocortisone 100mg stat, then q6-8h.
- Maternal/Fetal Effects (Poor Control): Maternal crisis, IUGR, preterm labor.
⭐ Women with known adrenal insufficiency require parenteral stress doses of corticosteroids (e.g., hydrocortisone 100mg IM/IV every 6-8 hours) throughout labor and delivery, and in the immediate postpartum period.
Pheochromocytoma in Pregnancy - Adrenaline Attack
- Rare catecholamine-secreting tumor. "Rule of 10s" (e.g., 10% malignant) less typical in pregnancy.
- Clinical Presentation:
- Classic Triad: Paroxysmal Hypertension, Palpitations, Headaches.
- Diaphoresis is also key.
- 📌 P.H.E.O. Mnemonic: Palpitations, Headache, Episodic sweating, Others (anxiety/tremor).
- Diagnosis:
Test Type Method Biochemical 24hr urinary fractionated metanephrines & catecholamines; Plasma free metanephrines Localization MRI (preferred over CT) - Management:
- Maternal/Fetal Risks: Extremely high if undiagnosed (↑↑ mortality).
⭐ Undiagnosed pheochromocytoma in pregnancy can lead to maternal and fetal mortality rates as high as 50%; thus, prompt diagnosis and management with alpha-adrenergic blockade are crucial.
High-Yield Points - ⚡ Biggest Takeaways
- Physiological hypercortisolism can mask Cushing's syndrome in pregnancy.
- Cushing's syndrome: ↑maternal/fetal risks (preeclampsia, GDM, IUGR); surgery (2nd tri) or metyrapone.
- Addison's disease: ↑steroid dose in labor/stress; continue fludrocortisone.
- CAH: Dexamethasone to mother for at-risk female fetus (virilization).
- Pheochromocytoma: Alpha-blockade (e.g., phenoxybenzamine) then beta-blockade; surgery pre-16 weeks/postpartum.
- Primary aldosteronism: Often improves; spironolactone contraindicated; use amiloride/nifedipine for severe HTN_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

