Probiotics & Microbiome Mod. - Gut Garden Intro
- Microbiome: Trillions of microbes (bacteria, fungi, viruses) in/on the human body; gut is the primary, most diverse site.
- Eubiosis: A balanced, healthy state of the gut microbial community.
- Dysbiosis: An imbalanced state; linked to various diseases (e.g., IBD, obesity, allergies, autoimmune disorders).
- Influencing Factors: Diet, antibiotics, age, mode of birth, stress, host genetics.

- Probiotics: Live microorganisms that, when administered in adequate amounts, confer a health benefit on the host (e.g., Lactobacillus, Bifidobacterium).
⭐ The human gut microbiome contains approximately 100 trillion microorganisms, outnumbering human cells by a factor of 10:1.
Probiotics & Microbiome Mod. - Friendly Flora Force
- Probiotics: Live microorganisms; confer health benefits when given in adequate amounts. Typical dose: 109-1010 CFU/day.
- Mechanisms: Pathogen exclusion, barrier integrity, immune modulation (↑IgA), antimicrobial production.
- Key Probiotics:
- Lactobacillus spp.
- Bifidobacterium spp.
- Saccharomyces boulardii (a yeast)

- Clinical Applications:
- Antibiotic-Associated Diarrhea (AAD).
- Infectious diarrhea (e.g., rotaviral).
- Irritable Bowel Syndrome (IBS).
- Necrotizing Enterocolitis (NEC) in preterm infants.
⭐ Saccharomyces boulardii, a yeast probiotic, is particularly effective in preventing and treating antibiotic-associated diarrhea (AAD).
- Other Microbiome Modulators:
- Prebiotics: Non-digestible food components selectively stimulating beneficial gut flora (e.g., FOS, GOS, inulin).
- Synbiotics: Probiotic + Prebiotic.
- Fecal Microbiota Transplantation (FMT): For recurrent Clostridioides difficile infection (rCDI).
Probiotics & Microbiome Mod. - Fueling the Good
- Probiotics: Live beneficial microbes (e.g., Lactobacillus, Bifidobacterium); confer health benefits.
- Prebiotics: Non-digestible fibers; selectively feed beneficial gut bacteria.
- Examples: Inulin, FOS, GOS.
- Mechanism: Fermented to SCFAs (e.g., acetate $CH_3COOH$, propionate $CH_3CH_2COOH$, butyrate $CH_3CH_2CH_2COOH$).
⭐ Prebiotics like inulin and fructooligosaccharides (FOS) selectively stimulate the growth of beneficial gut bacteria such as Bifidobacteria and Lactobacilli, leading to increased short-chain fatty acid (SCFA) production.
- Synbiotics: Probiotic + Prebiotic combination; synergistic effect.
- Postbiotics: Bioactive compounds from probiotics (e.g., SCFAs); health benefits.
- FMT (Fecal Microbiota Transplant): Stool transfer for recurrent C. difficile.

Probiotics & Microbiome Mod. - Gut Reset & Beyond
- Probiotics: Live beneficial microbes (e.g., Lactobacillus, Bifidobacterium) aiding gut health.
- Prebiotics: Non-digestible fibers (e.g., FOS, inulin) fueling beneficial gut bacteria.
- Synbiotics: Probiotic + Prebiotic combination for synergistic effect.
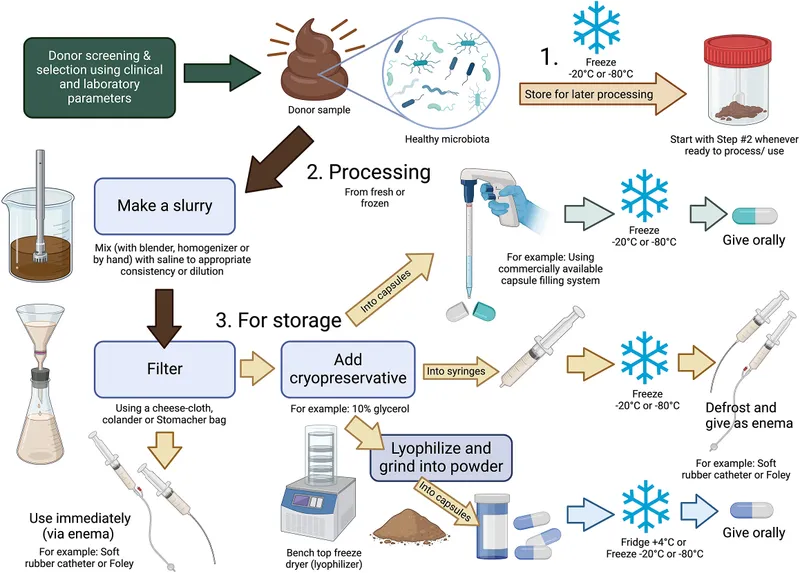
- **Fecal Microbiota Transplantation (FMT):
- Transfer of rigorously screened donor fecal microbiota to recipient.
- Primary indication: Recurrent Clostridioides difficile infection (rCDI).
⭐ Fecal Microbiota Transplantation (FMT) demonstrates high efficacy rates (often >80-90%) in treating recurrent Clostridioides difficile infection (rCDI) refractory to standard antibiotic therapies.
- Investigational uses: IBD, IBS, metabolic disorders.
- Modulation Strategies: Diet, judicious antibiotics, probiotics, prebiotics, FMT.
High‑Yield Points - ⚡ Biggest Takeaways
- Probiotics: Live microorganisms (e.g., Lactobacillus, Bifidobacterium) offering health benefits.
- Prebiotics: Non-digestible fibers (e.g., inulin, FOS, GOS) that fuel beneficial gut bacteria.
- Synbiotics: Probiotic + Prebiotic combinations for synergistic gut health effects.
- Fecal Microbiota Transplantation (FMT): Highly effective for recurrent Clostridioides difficile infection (CDI).
- Probiotic mechanisms: Competitive exclusion, immune modulation, improved gut barrier function.
- Microbiome modulation targets: IBD, IBS, obesity, allergies, mental health.
- Dysbiosis: Gut microbiota imbalance linked to chronic diseases and inflammation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

