Microbiome & Immune Kickstart - Gut Feeling Genesis
- Microbiome: Diverse microbial communities (bacteria, archaea, fungi, viruses) in/on the body; gut is a major reservoir.
- Immune System Priming:
- Early life exposure is critical for immune system education and tolerance.
- Drives development of Gut-Associated Lymphoid Tissue (GALT).
- Essential for distinguishing commensals from pathogens.
- Key Interactions & Molecules:
- Commensals: Stimulate secretory IgA (sIgA), enhance gut barrier function, compete with pathogens.
- Microbial metabolites: Short-Chain Fatty Acids (SCFAs) e.g., butyrate (from dietary fiber fermentation) nourish colonocytes, promote T-regulatory (Treg) cell development, and have anti-inflammatory effects.
- Microbe-Associated Molecular Patterns (MAMPs) are recognized by host Pattern Recognition Receptors (PRRs) like Toll-like Receptors (TLRs).
- Dysbiosis: Imbalance in microbiome composition; linked to allergies, autoimmune diseases, and Inflammatory Bowel Disease (IBD).

⭐ Segmented Filamentous Bacteria (SFB), while often unculturable, are potent specific inducers of Th17 cells and secretory IgA in the mammalian gut, significantly shaping mucosal immunity.
Innate Immunity's Tiny Trainers - First Line Friends
- Barrier Reinforcement: Strengthen epithelial tight junctions (occludin, claudins); promote robust mucus layer.
- Resource Competition: Outcompete pathogens for nutrients & adhesion sites on mucosa.
- Direct Antagonism: Secrete bacteriocins, defensins, SCFAs (e.g., butyrate) to inhibit pathogens.
- Innate Cell Priming & Maturation:
- MAMPs (LPS, PGN) sensed by PRRs (TLRs, NLRs) on innate cells.
- Primes macrophages, neutrophils, DCs; enhances phagocytosis, cytokine release (TNF-α, IL-6).
- GALT Development: Crucial for Gut-Associated Lymphoid Tissue development and function.
⭐ Commensal bacteria-derived Short-Chain Fatty Acids (SCFAs), like butyrate, fuel colonocytes and enhance macrophage antimicrobial activity.

Adaptive Immunity's Microbial Mentors - T&B Cell Tutors
- Microbiome shapes adaptive immunity, tutoring T & B cells.
- T-Cell Development & Differentiation:
- Commensals guide T-cell lineage in Gut-Associated Lymphoid Tissue (GALT).
- Segmented Filamentous Bacteria (SFB): key for Th17 induction. 📌 Mnemonic: SFB for Seventeen.
- Clostridia (clusters IV, XIVa) promote Regulatory T cells (Tregs) via butyrate.
- Th17/Treg balance: vital for mucosal homeostasis, prevents autoimmunity.
- B-Cell Maturation & Antibody Production:
- Microbial components stimulate B-cells for IgA production.
- IgA: crucial for mucosal defense.
- Microbiota influences germinal centers in Peyer's patches.
- Antigen Presenting Cell (APC) Priming:
- Microbial PAMPs (e.g., LPS) mature Dendritic Cells (DCs).
- Mature DCs effectively prime naive T-cells.
⭐ Segmented Filamentous Bacteria (SFB) are potent inducers of Th17 cells in the gut lamina propria, critical for defense against extracellular pathogens but also linked to autoimmune conditions when dysregulated.

Dysbiosis & Disease Drama - When Bugs Go Bad
- Dysbiosis: Microbial imbalance (composition/function) in gut; loss of beneficial microbes, ↑ pathobionts.
- Triggers:
- Antibiotics (📌 "Anti-Bio-sis" = against life, can disrupt gut life).
- Diet: ↓Fiber, ↑Fat/Sugar (Western diet).
- Infections, chronic stress, host genetics.
- Pathways to Pathology:
- ↑ Gut permeability ("Leaky Gut" syndrome).
- Altered immune responses (e.g., imbalance of ↑Th17, ↓Treg cells).
- ↓ Production of Short-Chain Fatty Acids (SCFAs like butyrate).
- ↑ Systemic endotoxemia (e.g., Lipopolysaccharide - LPS).
- Associated Diseases:
- GIT: Inflammatory Bowel Disease (IBD - Crohn's, Ulcerative Colitis), Irritable Bowel Syndrome (IBS), Clostridioides difficile infection (CDI), colorectal cancer.
- Metabolic: Obesity, Type 2 Diabetes Mellitus, Non-Alcoholic Fatty Liver Disease (NAFLD).
- Immune-mediated: Allergies, asthma, autoimmune disorders (e.g., Rheumatoid Arthritis, Multiple Sclerosis).
- Neuropsychiatric: Anxiety, depression, Autism Spectrum Disorder (via Gut-Brain Axis).
⭐ Clostridioides difficile infection (CDI), particularly pseudomembranous colitis, is a hallmark example of severe disease triggered by antibiotic-induced dysbiosis.
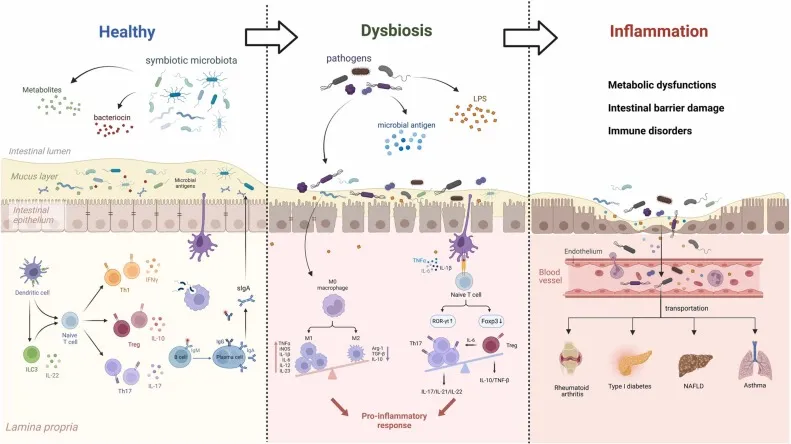
High‑Yield Points - ⚡ Biggest Takeaways
- Gut microbiome is crucial for immune system maturation and function.
- Dysbiosis is linked to autoimmune diseases, allergies, and inflammatory bowel disease (IBD).
- SCFAs (e.g., butyrate) from bacterial fermentation possess anti-inflammatory properties and promote Treg cell development.
- Microbiota educate innate immune cells and modulate adaptive immune responses, including Th1/Th2/Th17 balance.
- Segmented Filamentous Bacteria (SFB) strongly induce Th17 cells in the gut.
- Early microbial colonization influences oral tolerance and long-term immune health, underpinning the Hygiene Hypothesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

