Gut Microbiome: Composition - Meet the Micro-Managers
- Gut Microbiota: Community of microorganisms (bacteria, viruses, fungi, archaea) in the gastrointestinal tract (GIT).
- Gut Microbiome: Collective genetic material of the microbiota.
- Dominant Phyla: Firmicutes, Bacteroidetes. Key Genera: Lactobacillus, Bifidobacterium, Escherichia, Clostridium.
- Eubiosis: Normal, balanced microbial community. Dysbiosis: Imbalance, associated with disease.
- Microbial Density: Increases distally; Stomach/Duodenum (low, 101-103 cells/mL) → Colon (high, 1011-1012 cells/g).
⭐ The Firmicutes/Bacteroidetes (F/B) ratio is often altered in obesity (typically an increased F/B ratio).
Gut Microbiome: Influencers - Who Shapes Your Gut?

- Diet:
- High fiber (prebiotics) ↑ diversity.
- High fat/protein diets alter composition.
- Artificial sweeteners may cause dysbiosis.
- Age:
- Infancy: Crucial colonization period (breast vs. formula milk).
- Elderly: Typically ↓ diversity, altered stability.
- Mode of Birth:
- Vaginal: Acquires maternal vaginal/fecal flora.
- C-section: Colonized by skin flora, environmental microbes.
- Antibiotics:
- Cause ↓ diversity, dysbiosis; promote antibiotic resistance.
⭐ Broad-spectrum antibiotics can severely reduce gut flora diversity, predisposing to opportunistic infections like C. difficile.
- Host Genetics: Influences microbial composition and host response.
- Geography & Lifestyle: Local diet, sanitation, environment.
- Stress: Chronic stress negatively impacts gut-brain-microbiota axis.
- Hygiene Hypothesis: Reduced early life microbial exposure linked to ↑ immune disorders.
Gut Microbiome: Functions - The Symbiotic Symphony
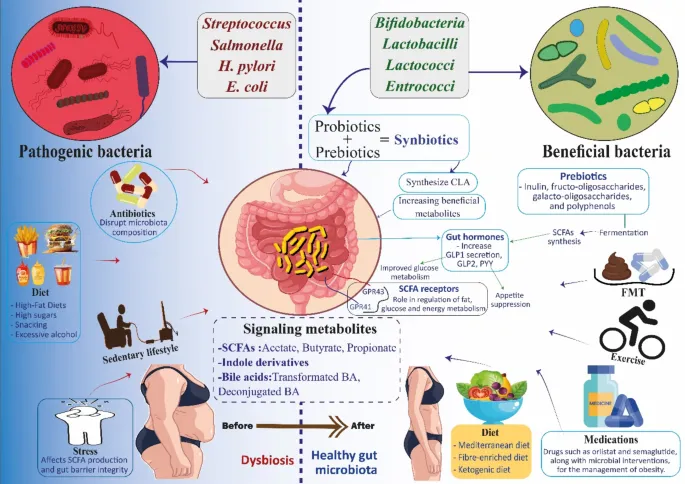
- Metabolic Functions:
- Vitamin Synthesis: Critical vitamins K, B-group (B12, folate).
- SCFA Production: Digests complex carbs (fiber) $\rightarrow$ SCFAs (Butyrate, Acetate, Propionate).
- Bile Acid Metabolism: Modifies primary to secondary bile acids.
- Protective Functions:
- Colonization Resistance: Competes with/inhibits pathogens.
- Gut Barrier Integrity: Strengthens mucus layer, tight junctions.
- Immune System Modulation:
- Development & Regulation: Influences $\uparrow$ IgA production, Treg cell differentiation.
⭐ Butyrate, a key SCFA produced by gut bacteria from fiber, is the primary energy source for colonocytes and has potent anti-inflammatory effects.
Gut Microbiome: Dysbiosis - When Microbes Go Rogue
Dysbiosis: Qualitative & quantitative changes in gut microbiota relative to eubiosis, causing imbalance.
- Associated GI Diseases:
- Inflammatory Bowel Disease (IBD): Crohn's, Ulcerative Colitis
- Irritable Bowel Syndrome (IBS)
- Clostridioides difficile infection (CDI)
- Associated Systemic/Metabolic Diseases:
- Obesity, Type 2 Diabetes Mellitus (T2DM)
- Non-Alcoholic Fatty Liver Disease (NAFLD)
- Cardiovascular Disease (CVD) (e.g., TMAO pathway)
- Gut-Brain Axis Links:
- Anxiety, depression, Autism Spectrum Disorder (ASD).
⭐ Recurrent Clostridioides difficile infection (CDI) is a prime example of severe dysbiosis, often refractory to standard antibiotics but highly responsive to Fecal Microbiota Transplantation (FMT).
Gut Microbiome: Modulation - Tuning Inner Ecosystem
- Dietary Interventions:
- High-fiber diet (promotes diversity).
- Prebiotics (e.g., inulin, FOS, GOS): Feed beneficial bacteria.
- Probiotics:
- Live microorganisms (Lactobacillus, Bifidobacterium) conferring health benefits.
- Indications: Antibiotic-associated diarrhea (AAD), Irritable Bowel Syndrome (IBS).
- Synbiotics: Probiotics + Prebiotics combination for synergistic effect.
- Fecal Microbiota Transplantation (FMT):
- Indication: Recurrent Clostridioides difficile infection (rCDI).
- Mechanism: Restores eubiosis.
> ⭐ Fecal Microbiota Transplantation (FMT) has a high success rate (often >**90%**) for treating recurrent *Clostridioides difficile* infection.
High‑Yield Points - ⚡ Biggest Takeaways
- Gut microbiome composition: influenced by diet, genetics, environment.
- Dominant phyla: Firmicutes & Bacteroidetes; their ratio is crucial.
- Functions: SCFA production (e.g., butyrate), immune modulation, pathogen protection.
- Dysbiosis (imbalance) linked to IBD, obesity, diabetes, mental health disorders.
- Probiotics (beneficial bacteria) & prebiotics (fiber) modulate gut flora.
- FMT is effective for recurrent C. difficile infection.
- Gut-brain axis: Bidirectional communication between gut microbiota and CNS.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

