Testing Basics - Germ Warfare Prep
- Core Objectives:
- Ensure food safety & quality (consumer protection).
- Detect pathogens (e.g., Salmonella, Listeria) & spoilage organisms.
- Verify regulatory compliance (FSSAI standards).
- Sample Handling (Critical Steps):
- Aseptic collection: Prevents external contamination. 📌 Always Sterile Sampling Prevents Problems.
- Representative portion of food item.
- Transport: Rapid, maintain temperature (typically 2-8°C).
- Initial Lab Procedures:
- Homogenization: Releases microbes from food matrix (e.g., using a stomacher).
- Serial Dilution: Systematically reduces microbial density for accurate plate counts (e.g., $1:10$ or $10^{-1}$ dilutions).
⭐ Total Viable Count (TVC) or Aerobic Plate Count (APC) gives a general estimate of the bacterial population, indicating overall hygiene.
oka
Old School Counts - Culture Club Rules
Traditional methods for quantifying microbes in food.
- Standard Plate Count (SPC) / Aerobic Plate Count (APC)
- Enumerates viable aerobes/facultative.
- Methods: Pour/Spread plate.
- Medium: PCA (Plate Count Agar).
- Incubation: 35°C, 24-48 hrs.
- Units: CFU/g or /mL.
- Limit: Underestimates (VBNC, anaerobes).
- Most Probable Number (MPN)
- Statistical estimate: low counts/specific groups (e.g., coliforms).
- Liquid media replicates (e.g., 3-tube).
- Results via MPN tables.
- Dye Reduction Tests (e.g., Methylene Blue, Resazurin)
- Assess metabolic activity; faster dye reduction = ↑ load.
- For milk quality.
- 📌 Methylene Blue Reduces Time with More Bugs.
- Direct Microscopic Count (DMC)
- Counts total cells (live/dead) by microscopy (Breed's smear).
- Rapid; less sensitive; debris interference.
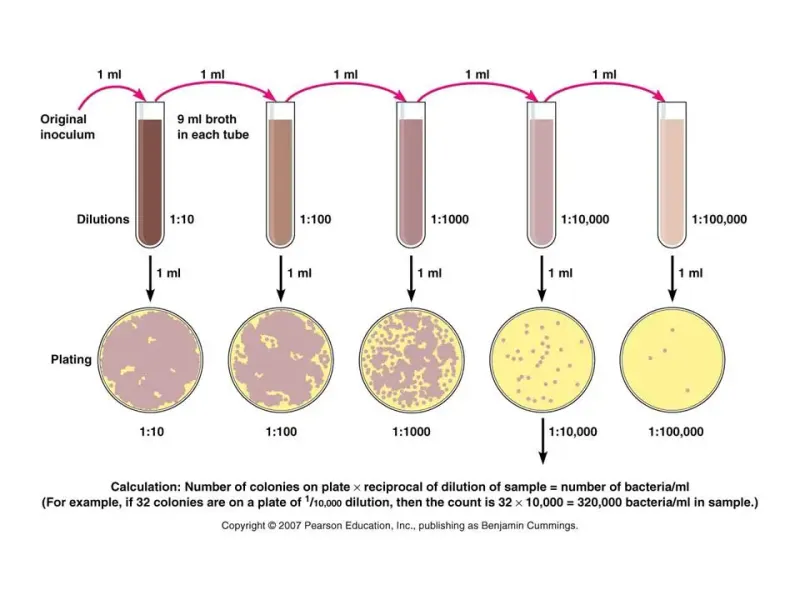
⭐ SPC is the most common method for determining the total number of viable aerobic bacteria in a food sample.
Rapid Roundup - Modern Microbe Detectives
Modern diagnostics bypass lengthy culture, offering swift, specific microbial detection in food.
- Immunological Assays: Antigen-antibody binding.
- ELISA: Sensitive for toxins/pathogens. High throughput.
- Lateral Flow Assays (LFAs): User-friendly strips. Rapid (minutes), point-of-need.
- Molecular Techniques: Target microbial nucleic acids.
- PCR: Amplifies DNA/RNA. Highly sensitive.
- Real-Time PCR (qPCR): Quantitative, live monitoring. Faster.
- Multiplex PCR: Detects multiple targets.
- NGS: Genomic insight for source tracking & pathogen ID.
- PCR: Amplifies DNA/RNA. Highly sensitive.
- Other Advanced Methods:
- MALDI-TOF MS: Rapid microbial ID via protein "fingerprints".
- Biosensors: Real-time detection via biological recognition & signal transduction.
⭐ MALDI-TOF MS identifies bacteria/yeasts in minutes (typically 2-10 min) from culture, much faster than biochemical tests.
Signposts & Safety - Rules of the Road
- Indicator Organisms: Signal poor hygiene or contamination.
- E. coli: Faecal contamination.
- Coliforms: General hygiene indicator.
- Enterobacteriaceae: Broader hygiene indicator.
- Pathogen Detection: Zero tolerance for key pathogens.
- Salmonella, Listeria monocytogenes, E. coli O157:H7, Campylobacter.
- Spoilage Organisms: Affect quality; may not be safety hazards.
- Yeasts, molds, Lactic Acid Bacteria.
- Microbiological Standards: FSSAI guidelines define limits.
- n, c, m, M values in sampling plans.
⭐ Listeria monocytogenes can grow at refrigeration temperatures (4°C), making it a persistent food safety challenge.
- HACCP Principles: Proactive food safety system.
High‑Yield Points - ⚡ Biggest Takeaways
- Indicator organisms (e.g., E. coli) signal fecal contamination and potential pathogen presence.
- Standard Plate Count (SPC) estimates total viable aerobic bacteria, reflecting overall hygiene.
- Most Probable Number (MPN) statistically enumerates coliforms in liquids like water/milk.
- Alkaline Phosphatase Test confirms milk pasteurization efficacy (enzyme inactivation).
- Dye Reduction Tests (Methylene Blue) rapidly assess microbial quality of raw milk.
- Key pathogen detection: Salmonella, Listeria monocytogenes, E. coli O157:H7.
- Aflatoxin screening (e.g., ELISA) is vital for mycotoxins from Aspergillus species.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

