Insomnia: Intro & Types - Defining Dream Deficits
- Insomnia: Persistent difficulty with sleep initiation, duration, consolidation, or quality, despite adequate opportunity. Leads to daytime impairment.
- Types based on duration:
- Short-term (Acute) Insomnia: Symptoms < 3 months. Often stress-related.
- Chronic Insomnia:
⭐ Chronic insomnia is defined as symptoms (difficulty initiating/maintaining sleep, or early awakening) lasting ≥ 3 months occurring ≥ 3 times/week, causing significant distress or impairment.
- Other Insomnia: Specific type, not meeting criteria for short-term or chronic.
Insomnia: Causes & Culprits - The Sleep Stealers
- Medical Conditions: Chronic pain, asthma/COPD, GERD, hyperthyroidism, RLS, heart failure.
- Psychiatric Disorders: Depression, anxiety disorders, PTSD, bipolar disorder.
- Medications/Substances: Stimulants (caffeine, nicotine), alcohol (disrupts sleep), decongestants, corticosteroids, some antidepressants.
- Situational/Environmental: Poor sleep hygiene, shift work, jet lag, stress, noise, light.

⭐ The '3P Model' (Predisposing, Precipitating, Perpetuating factors) is a key framework for understanding the development and persistence of chronic insomnia.
Insomnia: Diagnosis & Detective Work - Night's Unraveling
- Core Tools:
- Detailed Sleep History: Pattern, duration, daytime impact; medical/psychiatric/substance Hx.
- Sleep Diary: 1-2 weeks; records bedtime, sleep latency, awakenings, TST.
- Actigraphy: Objective sleep-wake pattern.
- Questionnaires:
- Insomnia Severity Index (ISI): Score ≥15 = clinical insomnia.
- Epworth Sleepiness Scale (ESS): Assesses daytime sleepiness.
- Polysomnography (PSG):
- Not routine. Indicated if OSA, PLMD, narcolepsy, or refractory insomnia suspected.
⭐ A thorough sleep history and a 1-2 week sleep diary are cornerstone diagnostic tools for insomnia; Polysomnography (PSG) is NOT routinely indicated unless other sleep disorders like OSA or PLMD are suspected.

Insomnia: Treatment Tango - Restoration Roadmap
⭐ Cognitive Behavioral Therapy for Insomnia (CBT-I) is the first-line recommended treatment for chronic insomnia and has demonstrated superior long-term efficacy compared to pharmacotherapy.
-
Non-Pharmacological (First-Line)
- CBT-I: Multi-component therapy.
- 📌 CBT-I Components (SLeep REST):
- Stimulus control
- Leep restriction (focus on sleep efficiency)
- Relaxation techniques
- Education (about sleep & healthy practices)
- Sleep hygiene (reinforcement)
- Thought restructuring (cognitive therapy)
- 📌 CBT-I Components (SLeep REST):
- Sleep Hygiene:
- Consistent sleep-wake schedule.
- Avoid stimulants (caffeine, nicotine) & alcohol near bedtime.
- Optimize sleep environment: dark, quiet, cool.
- Limit daytime naps to <30 mins.
- Avoid heavy meals/excess fluids before bed.
- CBT-I: Multi-component therapy.
-
Pharmacological (Second-Line / Adjunctive)
- Consider if CBT-I fails, is unavailable, or for short-term relief.
- Principles: Lowest effective dose, shortest duration possible, monitor side effects (e.g., dependence, rebound insomnia), taper on discontinuation.
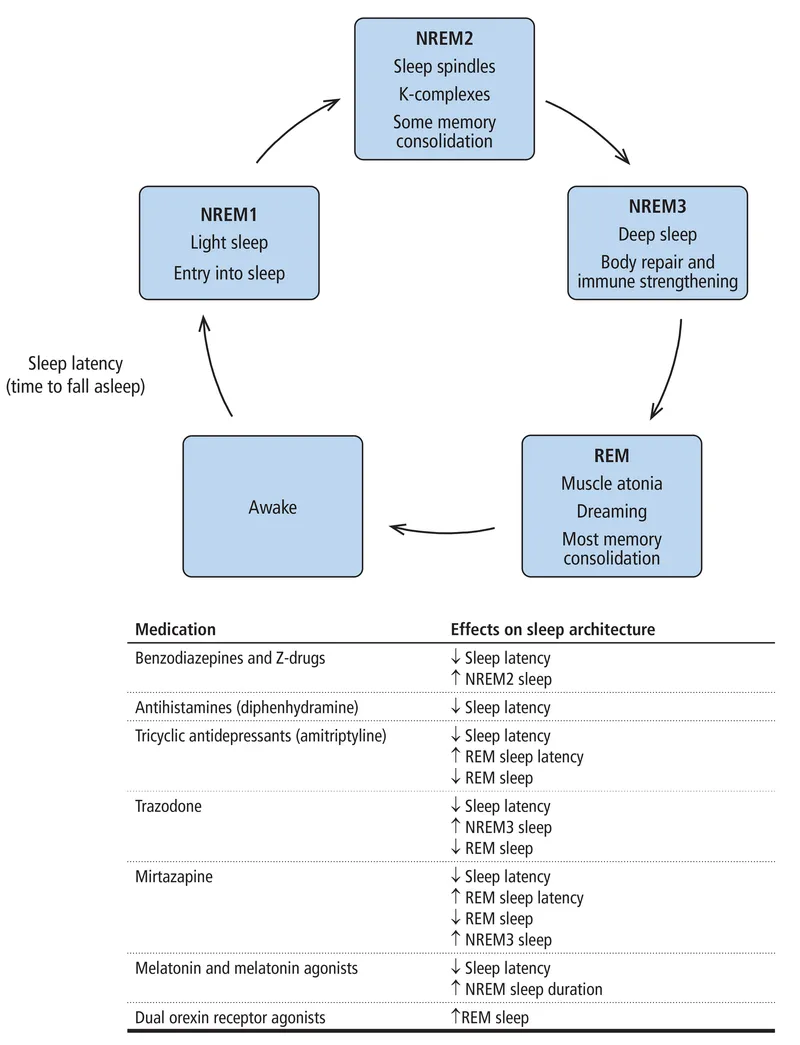
- Common Classes:
- Benzodiazepine Receptor Agonists (BzRAs):
- Benzodiazepines (e.g., Lorazepam, Temazepam)
- Non-Benzodiazepines / Z-drugs (e.g., Zolpidem, Eszopiclone) - generally preferred over BZDs for insomnia.
- Melatonin Receptor Agonists (e.g., Ramelteon) - good for sleep-onset insomnia, no abuse potential.
- Orexin Receptor Antagonists (e.g., Suvorexant, Lemborexant).
- Sedating Antidepressants (low-dose, off-label): Trazodone, Doxepin.
- Benzodiazepine Receptor Agonists (BzRAs):
- ⚠️ Caution: Elderly, history of substance abuse, comorbid respiratory conditions, pregnancy.
High‑Yield Points - ⚡ Biggest Takeaways
- Insomnia: Difficulty initiating/maintaining sleep or non-restorative sleep, causing daytime impairment.
- Chronic insomnia: Symptoms last ≥3 months, occurring ≥3 times/week.
- CBT-I (Cognitive Behavioral Therapy for Insomnia) is first-line treatment, superior to drugs long-term.
- Pharmacotherapy (e.g., Z-drugs, short-acting Benzodiazepines) is for short-term use; be wary of dependence.
- Sleep hygiene is important but often insufficient alone for chronic cases.
- Always rule out secondary causes: depression, anxiety, pain, or substance use.
- Polysomnography (PSG) is generally not indicated for primary insomnia diagnosis unless other disorders are suspected_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

