Sleep Medicine

On this page
🌙 Sleep Medicine: The Nocturnal Neuroscience Mastery
Sleep is not merely rest-it's a dynamic neurobiological process orchestrating memory consolidation, metabolic regulation, and immune function across precisely timed cycles. You'll master the architecture of sleep stages, decode circadian mechanisms driven by suprachiasmatic nucleus signaling, and develop pattern recognition skills to diagnose disorders from insomnia to narcolepsy. By integrating sleep pathology with cardiovascular, psychiatric, and metabolic comorbidities, you'll command evidence-based therapeutics that transform patient outcomes. This lesson builds your clinical reasoning from cellular clockwork to bedside decision-making, equipping you to address one of medicine's most underrecognized yet pervasive domains.
Sleep disorders affect 70 million Americans annually, with 22 million suffering from sleep apnea alone. Master these nocturnal networks, and you unlock the diagnostic keys to fatigue, cognitive dysfunction, cardiovascular disease, and psychiatric comorbidities that plague modern medicine.
🌙 Sleep Medicine: The Nocturnal Neuroscience Mastery
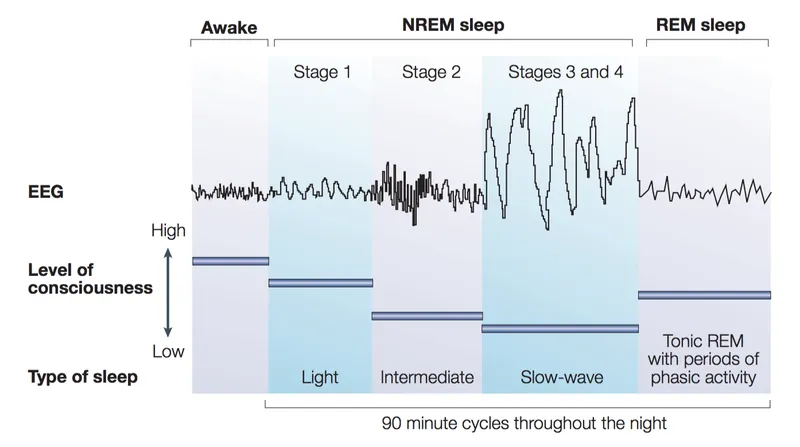
🧠 Sleep Architecture: The Brain's Nightly Symphony
NREM Sleep Stages: The Restorative Foundation
-
Stage N1 (Light Sleep)
- Duration: 2-5% of total sleep time
- EEG: 4-7 Hz theta waves replace alpha rhythm
- Physiological changes: 10-15% decrease in heart rate and blood pressure
- Muscle tone gradually decreases
- Eye movements become slow and rolling
- Hypnagogic hallucinations may occur (5-10% of population)
-
Stage N2 (Stable Sleep)
- Duration: 45-55% of total sleep time
- EEG hallmarks: Sleep spindles (12-14 Hz) and K-complexes
- Sleep spindles generated by thalamic reticular nucleus at 12-14 Hz frequency
- K-complexes: high-amplitude waves lasting >0.5 seconds
- Temperature regulation begins to diminish
- Arousal threshold increases significantly
-
Stage N3 (Deep Sleep/Slow Wave Sleep)
- Duration: 15-20% of total sleep time (decreases with age)
- EEG: Delta waves <4 Hz comprise >20% of epoch
- Critical functions: Growth hormone release (75% of daily secretion)
- Memory consolidation and synaptic homeostasis
- Glymphatic system activation for brain detoxification
- Highest arousal threshold - difficult to wake
📌 Sleep Spindle Memory: Spindles Signal Stable Sleep - Stage N2 with Sleep Spindles at 12-14 Hz, Signaling Synaptic Stabilization
REM Sleep: The Cognitive Processor
-
REM Characteristics
- Duration: 20-25% of total sleep time
- EEG: Mixed frequency, low-amplitude waves resembling wakefulness
- Physiological paradox: Brain activation with muscle atonia
- Rapid eye movements in burst patterns
- Dreams occur 80-90% of REM awakenings
- Temperature regulation completely absent
-
REM Physiology
- Cholinergic activation from pontine tegmentum
- Norepinephrine and serotonin activity suppressed
- Muscle atonia mediated by glycinergic neurons in medulla
- Blood pressure and heart rate variability increase
- Respiratory rate becomes irregular
- Penile erections occur (90% of REM periods)
⭐ Clinical Pearl: REM sleep latency <15 minutes suggests narcolepsy, depression, or sleep deprivation. Normal REM latency is 60-120 minutes in healthy adults.
| Sleep Stage | Duration (%) | EEG Pattern | Key Functions | Clinical Significance |
|---|---|---|---|---|
| N1 | 2-5% | 4-7 Hz theta | Sleep transition | Increased in sleep disorders |
| N2 | 45-55% | Spindles, K-complexes | Memory processing | Reduced in aging |
| N3 | 15-20% | <4 Hz delta waves | Growth hormone, restoration | Decreased in depression |
| REM | 20-25% | Mixed frequency | Dreams, memory consolidation | Altered in psychiatric disorders |
| Wake | <5% | 8-13 Hz alpha | Consciousness | Increased in insomnia |
💡 Master This: Sleep architecture changes predictably with age - N3 decreases from 20% in young adults to <10% after age 60, while wake time increases from 2% to 15-20%. This explains why elderly patients report lighter, more fragmented sleep.
Understanding sleep architecture provides the foundation for recognizing pathological patterns in polysomnography and correlating sleep disturbances with clinical presentations.
🧠 Sleep Architecture: The Brain's Nightly Symphony
⚡ Circadian Rhythms: The Master Clock Mechanics
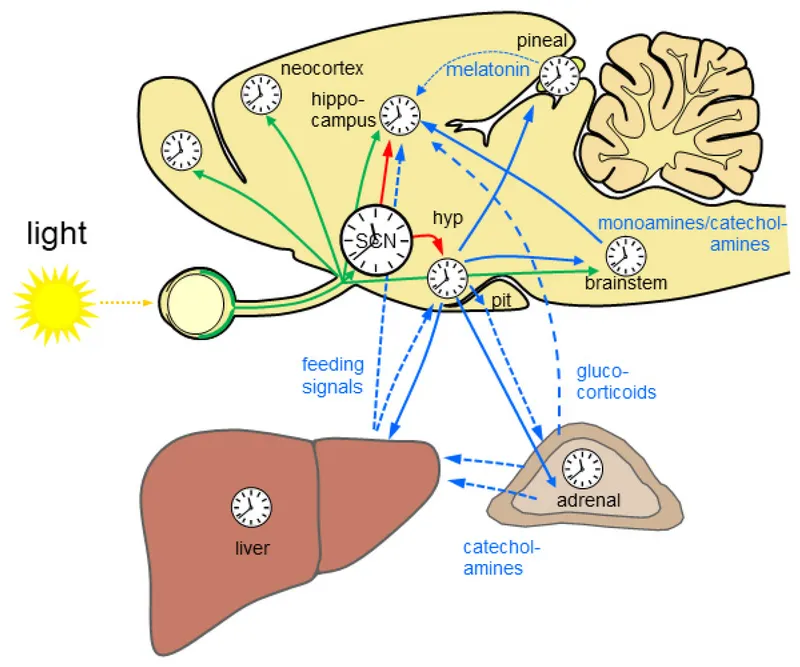
Circadian disruption underlies numerous sleep disorders and medical conditions. Master these temporal mechanisms, and you predict treatment responses and optimize therapeutic timing.
Suprachiasmatic Nucleus: The Central Pacemaker
-
SCN Architecture
- Location: Anterior hypothalamus above optic chiasm
- Cell population: ~20,000 neurons with intrinsic rhythmicity
- Input pathways: Retinohypothalamic tract for light entrainment
- Intergeniculate leaflet for non-photic cues
- Raphe nuclei for serotonergic modulation
- Intrinsic period: 24.2 ± 0.2 hours without external cues
-
Molecular Clock Mechanism
- CLOCK/BMAL1 transcription factors drive circadian gene expression
- Period (PER) and Cryptochrome (CRY) proteins provide negative feedback
- ~24-hour cycle of protein synthesis and degradation
- Light exposure resets molecular clocks via CRY protein degradation
- Temperature cycles provide secondary entrainment
- Genetic polymorphisms affect chronotype preferences
📌 Circadian Memory: CLOCK Controls Circadian Cycles - CRY and CLOCK proteins Create Cellular Chronometry with Constant Cycling
Melatonin: The Darkness Signal
-
Melatonin Physiology
- Pineal gland synthesis from tryptophan → serotonin → melatonin
- Sympathetic innervation controls nocturnal production
- Peak levels: 100-200 pg/mL at 2-4 AM
- Daytime suppression: <10 pg/mL with light exposure
- Blue light (460-480 nm) most suppressive
- Half-life: 30-50 minutes after oral administration
-
Melatonin Functions
- Phase-shifting: Advances circadian rhythms when given in evening
- Soporific effects: Promotes sleep initiation at 0.5-3 mg doses
- Antioxidant properties: Scavenges free radicals
- Seasonal affective disorder treatment
- Jet lag prevention and treatment
- Delayed sleep phase syndrome management
⭐ Clinical Pearl: Melatonin timing determines effect - morning administration delays circadian rhythms, while evening doses advance them. Optimal timing is 2-3 hours before desired bedtime for phase advancement.
| Circadian Marker | Peak Time | Nadir Time | Clinical Application | Normal Range |
|---|---|---|---|---|
| Core Temperature | 6-8 PM | 4-6 AM | Chronotype assessment | 36.1-37.2°C |
| Melatonin | 2-4 AM | 12-2 PM | Phase evaluation | 100-200 pg/mL |
| Cortisol | 6-8 AM | 11 PM-2 AM | HPA axis function | 10-25 μg/dL |
| Growth Hormone | 10 PM-2 AM | 10 AM-6 PM | Sleep quality | 1-5 ng/mL |
| Alertness | 10 AM, 6 PM | 2-4 AM | Performance timing | Subjective scale |
Circadian mastery enables precise treatment of shift work disorder, jet lag, and delayed/advanced sleep phase syndromes through evidence-based chronotherapy approaches.
⚡ Circadian Rhythms: The Master Clock Mechanics
🔍 Sleep Disorder Recognition: Pattern-Based Diagnostics
Hypersomnia Pattern Recognition
-
Narcolepsy Type 1 (with Cataplexy)
- Excessive daytime sleepiness with irresistible sleep attacks
- Cataplexy: sudden muscle weakness triggered by emotions (70% of patients)
- Sleep paralysis and hypnagogic hallucinations (60-80%)
- HLA-DQB1*06:02 positive in >95% of cases
- CSF hypocretin-1 <110 pg/mL (diagnostic threshold)
- MSLT: Mean sleep latency <8 minutes with ≥2 SOREMPs
-
Narcolepsy Type 2 (without Cataplexy)
- Excessive daytime sleepiness without cataplexy
- Normal CSF hypocretin-1 levels (>110 pg/mL)
- MSLT criteria: <8 minutes mean latency, ≥2 SOREMPs
- HLA association less consistent (40-60% positive)
- Sleep paralysis and hallucinations may occur
- Risk of progression to Type 1: 10-15% over 10 years
-
Idiopathic Hypersomnia
- Prolonged nocturnal sleep (>10 hours) with unrefreshing naps
- Sleep drunkenness: difficulty awakening with confusion
- MSLT: Mean sleep latency <8 minutes with <2 SOREMPs
- No cataplexy or REM sleep abnormalities
- Normal CSF hypocretin-1 levels
- Clarithromycin may provide therapeutic benefit
📌 Hypersomnia Memory: Narcolepsy Needs Naps - No Normal Night sleep, Numerous Nap Needs, Neurological Nature with Neurotransmitter (hypocretin) Needs
Sleep-Disordered Breathing Patterns
-
Obstructive Sleep Apnea (OSA)
- Apnea-Hypopnea Index (AHI): ≥5 events/hour with symptoms
- Severity classification: Mild (5-14), Moderate (15-29), Severe (≥30)
- Risk factors: BMI >30, neck circumference >17 inches (men), >16 inches (women)
- Mallampati score III-IV predicts OSA risk
- Epworth Sleepiness Scale >10 suggests excessive sleepiness
- STOP-BANG score ≥3 indicates high OSA probability
-
Central Sleep Apnea (CSA)
- Central apneas >50% of total respiratory events
- Heart failure association: CSA prevalence 40-50%
- Cheyne-Stokes breathing pattern with crescendo-decrescendo ventilation
- Opioid-induced CSA increasingly common
- High-altitude CSA occurs above 8,000 feet
- Treatment-emergent CSA in 5-15% of OSA patients on CPAP
⭐ Clinical Pearl: Complex sleep apnea (CompSA) emerges when central apneas develop during OSA treatment with CPAP. Occurs in 5-15% of OSA patients and may require adaptive servo-ventilation or bilevel PAP therapy.
| Sleep Disorder | Key Features | Diagnostic Criteria | Treatment Response | Prevalence |
|---|---|---|---|---|
| OSA | Snoring, witnessed apneas | AHI ≥5 with symptoms | CPAP 85-95% effective | 15-30% adults |
| CSA | Heart failure, opioids | Central events >50% | ASV for heart failure | 0.4-3.7% adults |
| Narcolepsy Type 1 | Cataplexy, sleep attacks | CSF hypocretin <110 | Stimulants + sodium oxybate | 0.02-0.18% |
| Idiopathic Hypersomnia | Long sleep, unrefreshing | MSLT <8 min, <2 SOREMPs | Modafinil, clarithromycin | 0.005-0.3% |
| RLS | Evening leg discomfort | Urge to move legs | Dopamine agonists | 5-15% adults |
Pattern recognition in sleep disorders enables rapid triage and appropriate diagnostic testing, leading to targeted treatments that dramatically improve patient outcomes and quality of life.
🔍 Sleep Disorder Recognition: Pattern-Based Diagnostics
⚖️ Treatment Algorithms: Evidence-Based Sleep Therapeutics
OSA Treatment Algorithm
CPAP Optimization Protocol
-
Initial Pressure Titration
- Starting pressure: 4-6 cmH2O for auto-titrating devices
- Target AHI: <5 events/hour for optimal control
- Pressure range: 4-20 cmH2O for most patients
- 90th percentile pressure from auto-CPAP determines fixed pressure
- Leak compensation: Modern devices adjust for <24 L/min unintentional leak
- Ramp time: 0-45 minutes to improve comfort
-
Adherence Optimization
- Medicare compliance: ≥4 hours/night for ≥70% of nights
- Optimal adherence: ≥6 hours/night for maximum benefit
- Mask fitting: Critical for <24 L/min leak rates
- Heated humidification reduces nasal congestion
- Pressure relief (C-Flex, EPR) improves comfort
- Behavioral interventions increase long-term adherence
📌 CPAP Memory: CPAP Cures Cardiovascular Complications - Consistent Compliance Creates Clinical Changes with Complete Control
Insomnia Treatment Hierarchy
-
First-Line: CBT-I (Cognitive Behavioral Therapy for Insomnia)
- Sleep restriction: Limit time in bed to sleep efficiency >85%
- Stimulus control: Bed only for sleep and sex
- Sleep hygiene: Cool temperature (65-68°F), dark environment
- Cognitive restructuring: Address dysfunctional sleep beliefs
- Relaxation training: Progressive muscle relaxation, mindfulness
- Response rates: 70-80% with sustained benefits
-
Pharmacological Interventions
- Short-term use: <4 weeks to prevent dependence
- Z-drugs: Zolpidem (5-10 mg), eszopiclone (1-3 mg)
- Melatonin receptor agonists: Ramelteon (8 mg), tasimelteon (20 mg)
- Orexin antagonists: Suvorexant (10-20 mg), lemborexant (5-10 mg)
- Avoid benzodiazepines: Risk of dependence and cognitive impairment
- Taper protocols: 25% reduction weekly to prevent rebound
⭐ Clinical Pearl: CBT-I demonstrates superior long-term outcomes compared to pharmacotherapy, with sustained improvements at 12-month follow-up and no risk of dependence. Should be first-line treatment for chronic insomnia.
| Treatment Modality | Efficacy Rate | Time to Effect | Duration of Benefit | Side Effects |
|---|---|---|---|---|
| CBT-I | 70-80% | 2-4 weeks | >12 months | Minimal |
| CPAP for OSA | 85-95% | 1-2 weeks | Ongoing with use | Mask discomfort |
| Zolpidem | 60-70% | 30 minutes | 6-8 hours | Dependence risk |
| Melatonin | 40-60% | 1-2 hours | 6-8 hours | Minimal |
| Modafinil | 70-85% | 1-2 hours | 8-12 hours | Headache, nausea |
Evidence-based treatment algorithms maximize therapeutic success while minimizing adverse effects, creating sustainable improvements in sleep quality and daytime functioning.
⚖️ Treatment Algorithms: Evidence-Based Sleep Therapeutics
🔗 Sleep-Medical Comorbidity Integration: Systems Interconnection
Cardiovascular-Sleep Integration
-
OSA-Cardiovascular Pathophysiology
- Intermittent hypoxia triggers sympathetic activation and oxidative stress
- Intrathoracic pressure swings increase cardiac afterload and venous return
- Inflammatory cascade: ↑CRP, ↑IL-6, ↑TNF-α levels
- Endothelial dysfunction with ↓nitric oxide bioavailability
- Accelerated atherosclerosis and plaque instability
- Arrhythmia risk: Atrial fibrillation prevalence 2-4x higher
-
Quantitative Cardiovascular Risks
- Hypertension: OSA increases risk by 200-300%
- Coronary artery disease: RR 2.38 (95% CI: 1.89-2.99)
- Stroke: RR 2.24 (95% CI: 1.57-3.19)
- Heart failure: OSA prevalence 40-50% in HF patients
- Sudden cardiac death: 2.6x increased risk with severe OSA
- CPAP treatment: 30-40% reduction in cardiovascular events
📌 Cardio-Sleep Memory: Heart Hates Hypoxia - Hypertension, Heart failure, Heart attacks Happen with Hypoxic Halts (apneas)
Metabolic-Sleep Interconnections
-
Sleep-Metabolic Pathways
- Sleep restriction (<6 hours) increases ghrelin by 28%, decreases leptin by 18%
- Glucose tolerance impaired with single night of sleep deprivation
- Insulin sensitivity decreases 25% after 4 nights of 4-hour sleep
- Cortisol dysregulation with evening elevation
- Growth hormone secretion reduced by 50%
- Inflammatory markers elevated: ↑IL-6, ↑CRP
-
Diabetes-Sleep Bidirectional Relationship
- OSA prevalence: 58% in Type 2 diabetes patients
- Diabetes risk: 37% increased with <5 hours sleep nightly
- HbA1c improvement: 0.4-0.8% reduction with CPAP therapy
- Diabetic neuropathy worsens sleep quality
- Nocturnal hypoglycemia fragments sleep architecture
- Sleep medications may affect glucose control
⭐ Clinical Pearl: Sleep duration shows U-shaped mortality curve - both <6 hours and >9 hours increase all-cause mortality by 10-15%. Optimal sleep duration is 7-8 hours for most adults.
| Medical Condition | Sleep Disorder Prevalence | Bidirectional Risk | Treatment Impact | Screening Recommendation |
|---|---|---|---|---|
| Heart Failure | OSA: 40-50% | 2-3x increased mortality | CPAP reduces events 30-40% | All HF patients |
| Type 2 Diabetes | OSA: 58% | 37% increased diabetes risk | HbA1c improves 0.4-0.8% | BMI >30 or symptoms |
| Depression | Insomnia: 75% | 2x increased depression risk | CBT-I improves mood | All depression patients |
| Hypertension | OSA: 30-40% | 2-3x increased HTN risk | CPAP reduces BP 5-10 mmHg | Resistant hypertension |
| Stroke | OSA: 60-70% | 2.2x increased stroke risk | CPAP improves recovery | All stroke patients |
Sleep-medical comorbidity integration reveals sleep as a modifiable risk factor that, when optimized, provides substantial benefits across multiple organ systems and disease states.
🔗 Sleep-Medical Comorbidity Integration: Systems Interconnection
🎯 Sleep Medicine Mastery: Clinical Command Center
Essential Clinical Arsenal
-
Rapid Assessment Tools
- Epworth Sleepiness Scale: >10 suggests pathological sleepiness
- STOP-BANG Questionnaire: ≥3 indicates high OSA risk
- Insomnia Severity Index: >14 indicates moderate-severe insomnia
- Pittsburgh Sleep Quality Index: >5 suggests poor sleep quality
- Morningness-Eveningness Questionnaire: Identifies chronotype preferences
- Sleep diary: 2-week minimum for circadian pattern assessment
-
Critical Diagnostic Thresholds
- AHI severity: Mild (5-14), Moderate (15-29), Severe (≥30)
- MSLT criteria: <8 minutes mean latency, ≥2 SOREMPs for narcolepsy
- REM latency: <15 minutes suggests narcolepsy or depression
- Sleep efficiency: <85% indicates sleep maintenance problems
- Total sleep time: <6 hours associated with health risks
- Wake after sleep onset: >30 minutes suggests fragmented sleep
📌 Mastery Memory: Sleep Specialists Systematically Screen - STOP-BANG Scores, Sleepiness Scales, Sleep Studies Solve Sleep Syndromes
Advanced Integration Framework
-
Polysomnography Interpretation Mastery
- Sleep architecture analysis: Stage percentages and REM latency
- Respiratory event classification: Obstructive vs central patterns
- Arousal index: >15/hour indicates fragmented sleep
- Periodic limb movement index: >15/hour with arousals pathological
- Sleep spindle density: Marker of sleep quality and memory consolidation
- Delta power: Quantitative measure of deep sleep intensity
-
Treatment Optimization Protocols
- CPAP titration: Target AHI <5, leak <24 L/min, usage >6 hours
- CBT-I implementation: Sleep restriction + stimulus control + cognitive restructuring
- Medication management: Lowest effective dose, shortest duration, taper protocols
- Combination therapy: CPAP + weight loss, CBT-I + short-term medications
- Comorbidity management: Cardiovascular, metabolic, psychiatric optimization
- Long-term monitoring: Annual follow-up, objective measures, quality of life
| Clinical Scenario | First-Line Diagnostic | Treatment Priority | Success Metrics | Follow-up Interval |
|---|---|---|---|---|
| Loud snoring + witnessed apneas | Home sleep test or PSG | CPAP therapy | AHI <5, usage >6h | 1-3 months |
| Excessive daytime sleepiness | PSG + MSLT | Stimulant medications | ESS <10, functional improvement | 1-2 months |
| Chronic insomnia | Sleep diary + clinical assessment | CBT-I | Sleep efficiency >85% | 2-4 weeks |
| Shift work complaints | Actigraphy + work schedule | Light therapy + melatonin | Improved alertness | 2-4 weeks |
| REM behavior disorder | Video PSG | Melatonin + safety measures | Injury prevention | 3-6 months |
💡 Master This: Sleep optimization represents one of the highest-yield interventions in medicine - improving cardiovascular outcomes, metabolic control, cognitive function, and quality of life across diverse patient populations through evidence-based, systematic approaches.
Sleep medicine mastery transforms clinical practice by recognizing sleep as a fundamental pillar of health, enabling comprehensive care that addresses root causes rather than isolated symptoms, ultimately optimizing patient outcomes across all medical specialties.
🎯 Sleep Medicine Mastery: Clinical Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app























