Quality Improvement & Patient Safety - Oops Prevention 101
- Quality Improvement (QI): Systematic efforts to enhance care processes & outcomes.
- Patient Safety (PS): Preventing harm to patients during medical care.
- Medical Error Types:
- Slip: Action not as planned (e.g., wrong drug dose drawn up).
- Lapse: Memory failure (e.g., forgetting a step in a procedure).
- Mistake: Incorrect plan (e.g., misdiagnosis leading to wrong treatment).
- Violation: Deliberate deviation from safe procedures.
- 📌 Mnemonic (Error Types): Silly Little Monkeys Vex.
- Adverse Event (AE): Harm from medical care, not underlying disease.
- Near Miss: Error with harm potential, but no harm occurred (chance/intervention).
- Sentinel Event: Unexpected event causing death, serious injury, or risk thereof.
- Swiss Cheese Model: (Reason) Errors occur when flaws in multiple system layers align, like holes in cheese slices.
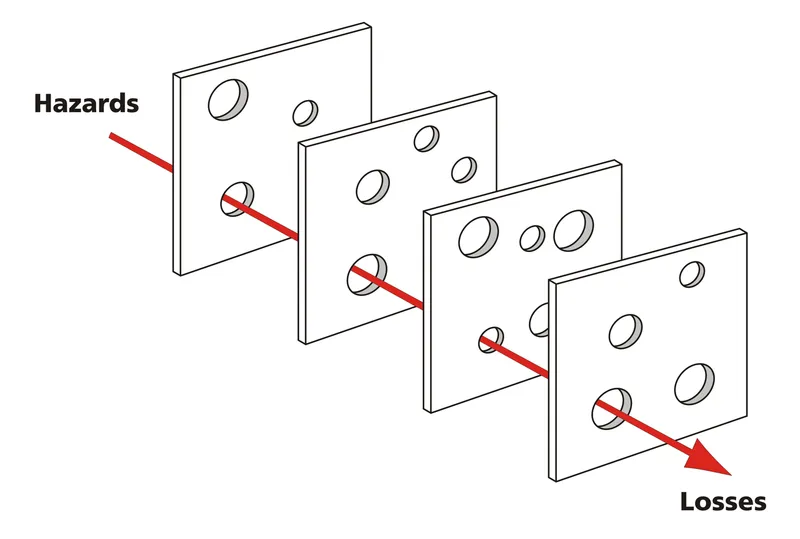
⭐ The majority of medical errors stem from systemic issues rather than individual incompetence.
Quality Improvement & Patient Safety - Cycle Savvy QI
- PDSA Cycle (Plan-Do-Study-Act): Core QI tool for iterative testing of changes. Purpose: To test a change on a small scale, learn, and refine before broader implementation.
- Lean Methodology: Aims to maximize patient value by eliminating waste (non-value-added activities).
- Key principle: Waste reduction (📌 TIM WOODS: Transportation, Inventory, Motion, Waiting, Overproduction, Over-processing, Defects, Skills underutilized).
- Six Sigma: Data-driven strategy to reduce defects (goal: <3.4 defects per million opportunities) and improve outcomes.
- Framework: 📌 DMAIC (Define, Measure, Analyze, Improve, Control) for systematic process improvement.
⭐ The PDSA cycle is fundamental for iterative testing and implementation of changes in healthcare quality improvement.
Quality Improvement & Patient Safety - Error Detective Kit
Essential tools for identifying, analyzing, and preventing patient safety incidents:
- Root Cause Analysis (RCA): Retrospective analysis; methods: Fishbone (Ishikawa) diagram, 5 Whys.
- Failure Modes and Effects Analysis (FMEA): Prospective risk assessment to prevent failures.
| Feature | Root Cause Analysis (RCA) | Failure Modes and Effects Analysis (FMEA) |
|---|---|---|
| Timing | Retrospective (after event) | Prospective (before system/process use) |
| Objective | Identify underlying causes | Identify potential failures & effects |
| Focus | Why did it happen? | What could go wrong? |
- Incident Reporting Systems: Collect and analyze data on errors and near misses for system improvement.
⭐ Root Cause Analysis (RCA) is a retrospective approach to error investigation, while FMEA is a prospective risk assessment tool.

Quality Improvement & Patient Safety - Safety Speak Up
- Patient Safety Culture:
- Promotes blame-free reporting of errors and near-misses.
- Focuses on system improvements, not individual blame.
⭐ A 'Just Culture' encourages error reporting by distinguishing between human error, at-risk behavior, and reckless conduct.
- Teamwork & Communication:
- 📌 SBAR: Standardized communication (Situation, Background, Assessment, Recommendation).
- Closed-loop communication: Ensures message accuracy by sender confirming receiver's understanding.
- Structured handoffs: Critical for continuity of care (e.g., I-PASS).
- Audits & Feedback:
- Regular audits to monitor safety practices (e.g., infection control, medication administration).
- Provides data-driven feedback for continuous improvement cycles.
- WHO Patient Safety Solutions (India Focus):
- Medication safety (e.g., managing Look-Alike Sound-Alike (LASA) drugs).
- Surgical Safety Checklist adherence.
- Hand hygiene to prevent Healthcare-Associated Infections (HAIs).

High‑Yield Points - ⚡ Biggest Takeaways
- PDSA cycle (Plan-Do-Study-Act) is fundamental for QI initiatives.
- Root Cause Analysis (RCA) is critical for analyzing sentinel events.
- Sentinel events (e.g., wrong-site surgery) require immediate investigation and reporting.
- Never Events are serious, largely preventable patient safety incidents.
- Key patient safety practices include hand hygiene and medication reconciliation.
- A Just Culture encourages error reporting to enhance system safety.
- Six Sigma aims to minimize defects and improve process efficiency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

