Pain Control - The Ache Avengers
-
Assessment: Use validated scales (NRS, VAS). Identify pain type: Nociceptive (somatic/visceral) vs. Neuropathic.
-
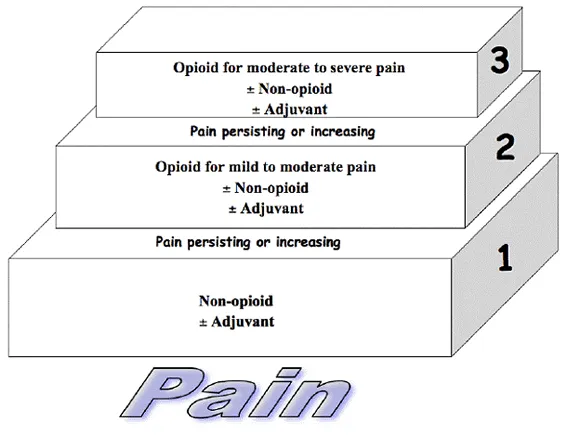
WHO Analgesic Ladder: Foundational approach.
-
Opioids: Start low, titrate to effect. Morphine (gold standard). Fentanyl patch (stable chronic pain). Breakthrough pain dose: 10-15% of total 24-hour dose.
-
Adjuvants:
- Neuropathic: Amitriptyline, Gabapentin, Pregabalin.
- Bone pain: NSAIDs, Bisphosphonates, Radiotherapy.
-
Opioid Side Effects:
- Constipation: Universal! Prescribe prophylactic laxatives (stimulant + softener). 📌
- Nausea/Vomiting: Antiemetics (e.g., Haloperidol).
- Sedation: Usually transient; dose reduction if persistent.
⭐ In renal impairment, morphine metabolites (M6G, M3G) accumulate; prefer fentanyl or methadone, or use morphine with caution and dose adjustment.
Dyspnea & Cough - Breathless Battles
-
Dyspnea: Subjective breathlessness.
- Management:
- Non-Pharmacological: Cool air (fan), positioning, pursed-lip breathing.
- Pharmacological:
- Opioids: Morphine (oral 2.5-5 mg, SC/IV 1-2 mg q4h PRN) cornerstone. Titrate.
- Anxiolytics: Lorazepam (0.5-1 mg) for anxiety component.
- Corticosteroids: e.g., COPD, tumor.
- Oxygen: Only if SpO2 < 90%.
- 📌 "PAM O2" for Dyspnea: Positioning, Airflow, Morphine, O2 (if hypoxic).
- Management:
-
Cough:
- Treat underlying cause.
- Non-Pharmacological: Honey, hydration, lozenges.
- Pharmacological:
- Opioids: Codeine, Morphine.
- Dextromethorphan.
- Refractory: Nebulized Lidocaine.
⭐ Opioids are effective for dyspnea even in non-hypoxic patients by reducing air hunger perception.
GI Distress - Gut Grumbles Gone
-
Nausea & Vomiting (N&V)
- Assessment: Identify cause (opioids, chemo, metabolic, obstruction, ↑ICP).
- Management:
- Non-pharmacological: Small meals, hydration.
- Pharmacological:
- Dopamine (D2) antag: Metoclopramide¹ (10mg TDS), Haloperidol (0.5-1.5mg OD-BD).
- Serotonin (5-HT3) antag: Ondansetron (4-8mg BD/TDS) - esp. chemo/radio.
- Antihistamine (H1): Cyclizine (50mg TDS) - motion, bowel obstruction.
- Anticholinergic: Hyoscine butylbromide (20mg QID) - colic, secretions.
- Steroids: Dexamethasone (4-8mg OD) - ↑ICP, MBO.
- Refractory: Levomepromazine.
⭐ Metoclopramide¹ is generally avoided in complete bowel obstruction or Parkinson's disease.
-
Constipation
- Opioid-Induced Constipation (OIC) is common; prophylaxis vital!
- Rx:
- Lifestyle: Fluids, fiber (cautiously in MBO).
- Laxatives:
- Stimulant (Senna, Bisacodyl) + Softener (Docusate). 📌 MUSH & PUSH.
- Osmotic (Lactulose, Macrogol/PEG).
- Peripheral opioid antagonist: Methylnaltrexone (SC) if refractory OIC.
-
Malignant Bowel Obstruction (MBO)
- Medical management: Analgesia, antiemetics (Haloperidol, Cyclizine), antisecretory (Octreotide 100-600 mcg/24h SC/CSCI, Hyoscine Butylbromide 60-120mg/24h CSCI), Dexamethasone.
Neuropsychiatric Issues - Mind Menders
-
Delirium
- Acute onset, fluctuating course, inattention, disorganized thinking, altered consciousness.
- Causes: 📌 I WATCH DEATH (Infection, Withdrawal, Acute metabolic, Trauma, CNS, Hypoxia, Deficiencies, Endocrinopathies, Acute vascular, Toxins, Heavy metals).
- Management:
- Non-pharm: Reorient, calm environment, sleep, hydration.
- Pharm:
- Haloperidol 0.5-1 mg PO/SC/IV.
- Risperidone 0.25-0.5 mg PO.
- Olanzapine 2.5-5 mg PO/SL/IM.
- ⚠️ Avoid benzodiazepines (except alcohol/benzo withdrawal).
⭐ Haloperidol is first-line for delirium in palliative care; use atypicals (e.g., risperidone) or avoid in Parkinson's/LBD.
-
Agitation/Restlessness
- Assess reversible causes (pain, bladder/bowel issues).
- Delirium-related: Antipsychotics.
- Anxiety-related: Lorazepam 0.5-1 mg.
- Terminal: Midazolam SC 10-30 mg/24h; Levomepromazine.
-
Depression/Anxiety
- Depression: SSRIs (e.g., Sertraline).
- Anxiety: Benzodiazepines (e.g., Lorazepam, short-term).
- Psychostimulants (Methylphenidate) for rapid effect: fatigue, apathy, depression.
High‑Yield Points - ⚡ Biggest Takeaways
- Opioids (e.g., morphine) are cornerstone for cancer pain; titrate to effect.
- Dyspnea: manage with low-dose morphine, oxygen (if hypoxic), anxiolytics.
- Nausea/Vomiting: target cause; use metoclopramide, ondansetron, or haloperidol.
- Opioid-induced constipation: requires prophylactic stimulant + softener laxatives.
- Delirium: treat reversible causes; haloperidol for severe agitation.
- Terminal agitation: consider midazolam or phenobarbital for sedation.
- WHO analgesic ladder: guides pain management strategy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

