Understanding Pain - The Palliative Puzzle
- Pain: Unpleasant sensory & emotional experience linked to actual/potential tissue damage (WHO).
- Total Pain (Cicely Saunders): Physical, psychological, social, spiritual dimensions. Holistic approach vital.
- Types & Characteristics:
- Nociceptive:
- Somatic: Localized, aching, throbbing (e.g., bone mets).
- Visceral: Diffuse, cramping, gnawing (e.g., organ distension).
- Neuropathic: Nerve injury; burning, shooting, tingling, "pins & needles".
- Nociceptive:
- Assessment: Self-report is gold standard 💡. Use scales (NRS, VAS, Faces Pain Scale).
⭐ "Total Pain" (Saunders): physical, psychological, social, spiritual dimensions; crucial for holistic palliative care.
Assessing Agony - Detective Work
- Core Principle: Pain is subjective; patient's report is key.
- Systematic Assessment:
- History: Patient's words. 📌 SOCRATES: Site, Onset, Character, Radiation, Assoc. symptoms, Timing, Exacerb/Relief, Severity.
- Impact: On daily activities, sleep, mood.
- Physical Exam: Source, tenderness, neuro signs.
- Pain Scales:
- NRS (Numeric Rating Scale): 0-10.
- VAS (Visual Analog Scale): 100mm line.
- Wong-Baker FACES: Children ≥3 yrs, cognitive/verbal impair.
- VDS (Verbal Descriptor Scale): Mild, moderate, severe.
- BPS/CPOT (Behavioral Pain Scale/Critical-Care Pain Observation Tool): Non-verbal/ICU.
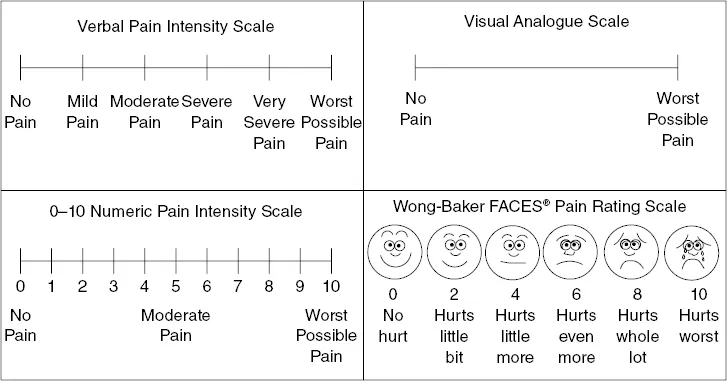
⭐ Wong-Baker FACES Scale: validated for children ≥3 yrs; preferred if unable to use numeric scales.
The Analgesic Arsenal - Step by Step
- WHO Ladder Principles: 📌 By Mouth, By Clock, By Ladder, Individualized Dosing.
- Non-Opioids (Step 1):
- Paracetamol: Max 4g/day (adults).
- NSAIDs (e.g., Ibuprofen, Diclofenac): GI & renal risk. COX-2 inhibitors (Etoricoxib) safer for GI.
- Weak Opioids (Step 2):
- Tramadol: 50-100mg q4-6h (max 400mg/day). Seizure risk.
- Codeine: Often with paracetamol. Constipation.
- Strong Opioids (Step 3):
- Morphine (oral): Start 5-10mg q4h for opioid-naive.
- Fentanyl (patch): For stable, chronic pain. Not for acute pain or opioid-naive.
- Adjuvant Analgesics (All Steps):
- Neuropathic pain: Gabapentin, Pregabalin, Amitriptyline.
- Bone pain: Corticosteroids (Dexamethasone), Bisphosphonates.
⭐ Morphine is the gold standard and first-line strong opioid for moderate to severe cancer pain management according to WHO guidelines; initiate with immediate-release oral morphine.
Opioid Power - Taming the Beast
- Principle: WHO Ladder Step 2 (weak) & 3 (strong) for moderate-severe pain.
- Weak: Tramadol, Codeine.
- Strong: Morphine (Gold Standard), Fentanyl, Methadone, Oxycodone.
- Titration: "Start Low, Go Slow".
- Breakthrough Pain (BTP): Rescue dose 10-15% of 24-hr total, q1-4h PRN.
- Opioid Rotation: For poor efficacy or intolerable side effects.
- Use equianalgesic doses; reduce new opioid by 25-50% (incomplete cross-tolerance).
- Key Side Effects & Management:
- Constipation: Universal. Prophylactic laxatives (stimulant + softener).
- Nausea/Vomiting: Common. Antiemetics (Metoclopramide).
- Sedation: Usually transient.
- Respiratory Depression: Rare. Antidote: Naloxone (0.4mg IV/IM).
- 📌 Mnemonic (Common): Constipation, Nausea, Sedation (CNS).

- Important Notes:
- Fentanyl patch: For stable pain, not opioid-naïve. Change q72h.
- Methadone: Long half-life, good for neuropathic pain. Careful initiation.
⭐ Oral morphine is the first-line strong opioid for cancer pain management as per WHO guidelines, valued for its efficacy and multiple administration routes.
High‑Yield Points - ⚡ Biggest Takeaways
- Pain assessment is key; use scales like NRS or VAS.
- The WHO analgesic ladder guides stepwise management, starting with non-opioids.
- Morphine is the gold standard strong opioid; titrate dose carefully.
- Proactively manage opioid side effects: constipation (laxatives), nausea (antiemetics).
- Use adjuvant analgesics like gabapentin for neuropathic pain or NSAIDs.
- Address breakthrough pain with short-acting opioids.
- Recognize total pain: physical, psychological, social, spiritual aspects_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

