Palliative Care: Core Concepts & Initiation - Gentle Beginnings
- Definition: Active, total care for patients with life-limiting illnesses; primary goal is improving Quality of Life (QoL).
- Core Goals:
- Prevent & relieve suffering (physical, psychosocial, spiritual).
- Support patient autonomy & informed decision-making.
- Enhance QoL for patients & families.
- When to Initiate:
- Early in the course of illness, ideally at diagnosis of advanced cancer.
- Concurrently with curative or life-prolonging treatments.
- Not restricted to end-of-life care.
- Key Principles:
- Patient-centered & family-oriented.
- Holistic: addresses physical, emotional, social, spiritual needs.
- Interdisciplinary team approach.
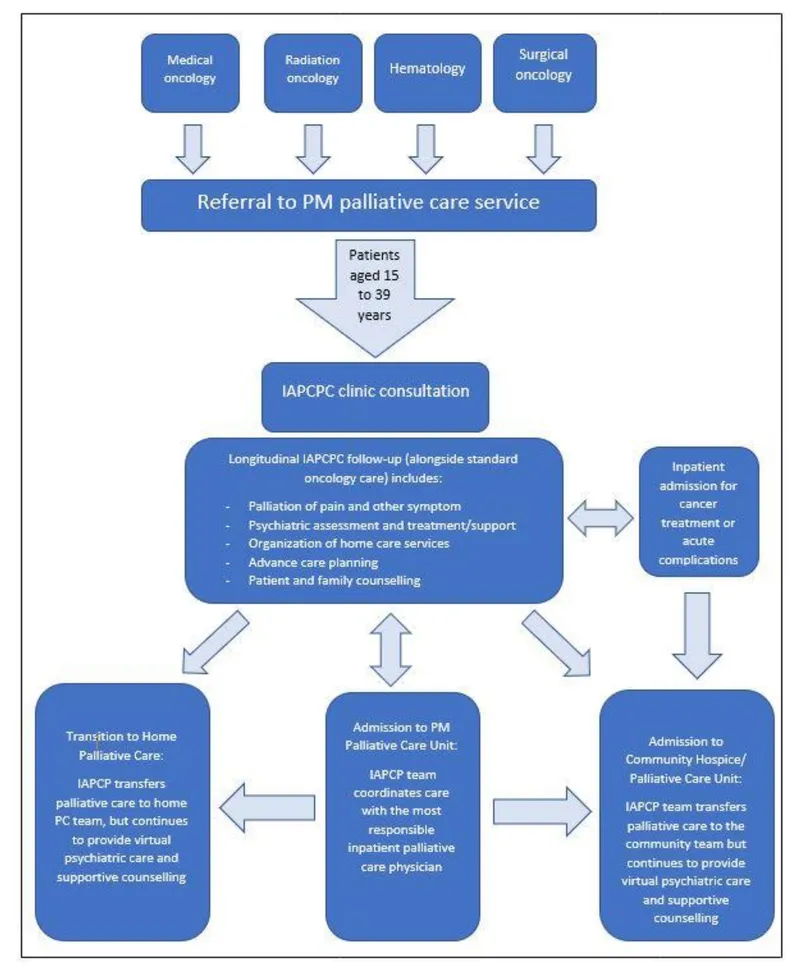
⭐ Early palliative care integration (within 8 weeks of advanced cancer diagnosis) improves QoL, reduces depression, and may prolong survival (NEJM, 2010).
Oncologic Symptom Management - Comfort Commandos
- Goal: Maximize Quality of Life (QoL) by managing distressing symptoms.
- Key Symptoms & Approaches:
- Pain:
- Assess: PQRST. Use WHO Analgesic Ladder.
- Opioids: Morphine, Fentanyl. Titrate dose.
- Adjuvants: NSAIDs, Corticosteroids, Gabapentin/Pregabalin for neuropathic pain.
- Nausea/Vomiting (N&V):
- Antiemetics: Ondansetron (5-HT3 antag.), Metoclopramide (D2 antag.), Dexamethasone.
- Dyspnea:
- Low-dose Morphine (2.5-5 mg PO q4h PRN). Oxygen if hypoxic.
- Constipation:
- Prophylaxis with opioids. Laxatives (Senna, Docusate). Methylnaltrexone for Opioid-Induced Constipation (OIC).
- Fatigue:
- Energy conservation. Treat reversible causes.
- Cachexia:
- Megestrol acetate. Nutritional support.
- Pain:

⭐ For opioid-induced constipation (OIC), peripherally acting mu-opioid receptor antagonists (PAMORAs) like methylnaltrexone are effective and preserve analgesia.
📌 PAIN Mnemonic - "LADDER" (for WHO ladder application):
- Look for cause
- Add adjuvants
- Dose regularly (not just PRN for chronic pain)
- Details (document assessment & response)
- Explain to patient & family
- Review regularly & re-assess
Communication & Ethical Aspects in Oncology Palliative Care - Heartfelt Huddles
Effective Communication (SPIKES Model):
Core Ethical Considerations:
- Core Principles: Autonomy (patient choice), Beneficence (do good), Non-maleficence (no harm), Justice (fairness).
- Informed Consent: Patient understands diagnosis, prognosis, options (risks/benefits) to decide.
- Advance Care Planning: Respect documented wishes (living will, proxy).
- End-of-Life (EOL) Decisions:
- Withhold/Withdraw Life-Sustaining Treatment (LST) (futile/patient wish).
- 📌 Doctrine of Double Effect (DDE): Symptom relief intent justifies unintended life shortening if primary goal is palliation.
- Confidentiality: Uphold patient privacy.
- Shared Decision-Making: Collaborative patient/family care planning.
⭐ Withholding/withdrawing futile life-sustaining treatment, with informed consent or a valid advance directive, is ethically & legally permissible in India.
End-of-Life Care (EOLC) in Oncology - Peaceful Passages
- Goal: Maximize comfort, dignity, and quality of life (QoL) during the terminal phase of illness.
- Symptom Management:
- Pain: Opioids (morphine); titrate effectively.
- Dyspnea: Opioids, oxygen, anxiolytics.
- Terminal Delirium: Haloperidol, midazolam. Exclude reversible causes.
- Death Rattle: Anticholinergics (hyoscine, glycopyrrolate). Reposition.
- Communication: Open discussions on prognosis, patient preferences, Advance Care Planning (ACP), Do Not Attempt Resuscitation (DNAR).
- Anticipatory Prescribing: Medications for predictable EOL symptoms.
- Family Support: Psychosocial, spiritual needs; bereavement care.
⭐ The "death rattle" occurs in 25-50% of dying patients; managed with anticholinergics and repositioning.
High‑Yield Points - ⚡ Biggest Takeaways
- Palliative care enhances quality of life through symptom control in serious illnesses.
- The WHO analgesic ladder is pivotal for cancer pain management; morphine is key.
- Address common symptoms: pain, dyspnea, nausea/vomiting, cachexia, and delirium.
- Effective communication (e.g., SPIKES for breaking bad news) is essential.
- Palliative radiotherapy treats bone pain, brain metastases, and cord compression.
- Prophylactically manage opioid-induced constipation; monitor other side effects.
- Palliative care can be concurrent with curative treatment, unlike hospice_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

