Headache Basics - Pinpointing Pain Patterns
- Primary: No structural cause (Migraine, TTH, TACs).
- Secondary: Symptom of underlying pathology.
- Pain Patterns: Assess Onset, Location, Duration, Character, Aggravating/Relieving factors, Timing, Severity (OLD CARTS).
- 📌 Red Flags (SNOOPP): Systemic sx, Neuro deficits, Sudden Onset, Older (>50), Pattern change, Papilledema.
⭐ IHS Primary Headache Classification:
- Migraine
- Tension-Type Headache (TTH)
- Trigeminal Autonomic Cephalalgias (TACs)
- Other Primary Headaches
Migraine - Throbbing Trouble

- Episodic, often unilateral, pulsating headache; duration 4-72 hrs.
- 📌 POUND mnemonic: Pulsating, One-day duration (untreated: 4-72 hrs), Unilateral, Nausea/vomiting, Disabling intensity.
- Aura: Reversible neurological symptoms (visual, sensory, speech) preceding or accompanying headache.
- Triggers: Stress, hormonal changes (menses), certain foods (chocolate, cheese), alcohol, sleep disturbances.
⭐ Diagnostic Criteria (Migraine without Aura):
- At least 5 attacks fulfilling criteria.
- Headache duration: 4-72 hours.
- Headache has ≥2 of: unilateral, pulsating, moderate/severe pain, aggravation by routine physical activity.
- During headache, ≥1 of: nausea and/or vomiting; photophobia and phonophobia.
- Acute Management:
- Mild-Moderate: NSAIDs (Ibuprofen), Paracetamol.
- Moderate-Severe: Triptans (Sumatriptan 50-100mg PO), Gepants (Ubrogepant).
- Antiemetics (Metoclopramide) if nausea/vomiting prominent.
- Prophylaxis (if ≥4 attacks/month, disabling, or triptan overuse):
- Beta-blockers (Propranolol), TCAs (Amitriptyline), Anticonvulsants (Topiramate, Valproate), CGRP mAbs.
- Chronic Migraine: ≥15 headache days/month for >3 months (≥8 days with migraine features).
Tension-Type Headache - The Daily Grind
- Most common primary headache; bilateral, non-pulsating, pressing/tightening quality.
- Mild to moderate intensity; not aggravated by routine activity.
- No nausea/vomiting; photophobia or phonophobia may be present (not both).
- Types:
- Infrequent episodic: <1 day/month.
- Frequent episodic: 1-14 days/month.
- Chronic: ≥15 days/month for >3 months.
- Pathophysiology: Peripheral (myofascial tenderness) and central mechanisms.
⭐ Tension-Type Headache is characterized by bilateral, pressing/tightening (non-pulsating) quality, mild to moderate intensity, and not aggravated by routine physical activity.
- Management: Analgesics (NSAIDs, paracetamol), amitriptyline for prophylaxis in chronic TTH.
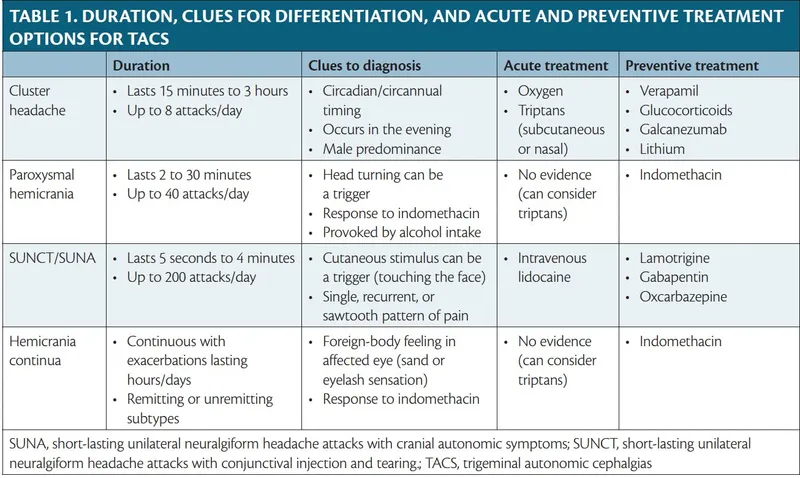
Trigeminal Autonomic Cephalalgias - TACs Attack!
Unilateral headache, ipsilateral cranial autonomic symptoms.
- Cluster Headache (CH)
- Severe orbital/temporal pain; 15-180 min; 1 qod to 8/day.
- Autonomic features, restlessness.
- Acute: 100% O2, SC Sumatriptan (6mg). Prophylaxis: Verapamil.
- Paroxysmal Hemicrania (PH)
- Severe pain; shorter (2-30 min), frequent (>5/day).
- Autonomic features.
- Key: Responds to Indomethacin (25-75mg TID).
- SUNCT/SUNA
- Short (1-600 sec) stabbing pain; very frequent.
- SUNCT: Conjunctival injection & Tearing. SUNA: Other autonomic features.
- Rx: Lamotrigine.
⭐ Acute treatment for Cluster Headache: 100% oxygen (12-15 L/min), SC sumatriptan (6mg).
Secondary Headaches & Red Flags - Danger Signals
- Headaches from underlying pathology; prompt ID vital.
- 📌 SNOOP4 Red Flags:
- Systemic: Fever, wt loss, cancer.
- Neurologic: Focal deficits, seizures, AMS.
- Onset: Sudden (thunderclap); New >50 yrs.
- Ps: Pattern change, Progressive, Papilledema, Positional, Precipitated (cough/Valsalva).
- Key Causes:
- SAH: Thunderclap. CT (LP if neg).
- Meningitis: Fever, nuchal rigidity. LP.
- GCA: Age >50, jaw claudication, ESR >50 mm/hr. Biopsy.
- Tumor: Progressive, focal. Neuroimaging.
- IIH: Papilledema, LP opening pressure >25 cm $H_2O$.
⭐ The SNOOP4 mnemonic (Systemic symptoms, Neurologic signs, Onset sudden, Older age, Pattern change, Papilledema, Positional, Precipitated by cough/exertion, Progressive) helps identify red flags for secondary headaches.
High‑Yield Points - ⚡ Biggest Takeaways
- Migraine prophylaxis includes Propranolol, Topiramate, and Amitriptyline.
- Triptans are first-line for acute migraine; avoid in CAD.
- Cluster headache: Unilateral, periorbital pain, autonomic signs; acute: 100% O2/Sumatriptan; prophylaxis: Verapamil.
- Tension-type headache: Bilateral, "band-like" pressure; treat with NSAIDs.
- MOH: From frequent acute drug use; stop offending drug.
- Secondary headache red flags: SNOOP (Systemic, Neuro, Onset, Older, Pattern).
- Trigeminal neuralgia: Lancinating facial pain; Carbamazepine is DOC.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

