Neurology

On this page
🧠 The Neural Command Center: Decoding Brain Architecture
The nervous system orchestrates every thought, movement, and sensation through an intricate network of electrical signals and anatomical pathways. You'll master how to decode brain architecture, trace neural highways, and recognize clinical patterns that pinpoint lesions with precision. By integrating diagnostic reasoning with evidence-based interventions, you'll transform complex neurological presentations into confident clinical decisions. This lesson builds your ability to think like a neurologist-connecting anatomy to physiology, symptoms to localization, and diagnosis to targeted treatment.
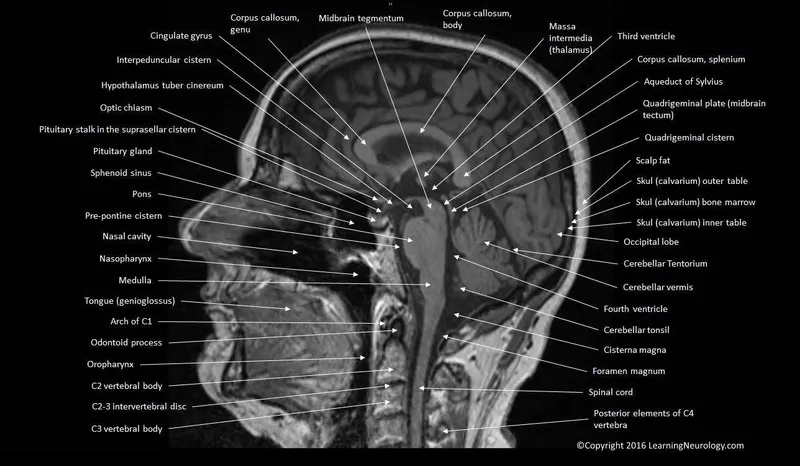
The central nervous system represents medicine's most sophisticated territory, where 2% of body weight consumes 20% of total energy and processes information at speeds reaching 120 meters per second. Understanding neuroanatomy unlocks the logic behind every neurological presentation, from subtle cognitive changes to devastating strokes.
Neuroanatomical Foundation Matrix
The brain's hierarchical organization follows predictable patterns that guide clinical localization:
-
Cerebrum (85% of brain weight)
- Frontal lobe: Executive function, motor control (40% of cortical volume)
- Parietal lobe: Sensory integration, spatial processing (20% of cortical volume)
- Temporal lobe: Memory, language, auditory processing (22% of cortical volume)
- Hippocampus: Memory consolidation (95% of new memories)
- Wernicke's area: Language comprehension (dominant hemisphere)
- Occipital lobe: Visual processing (18% of cortical volume)
- Primary visual cortex: 130 million photoreceptors input processing
-
Brainstem (4% of brain weight, 100% critical functions)
- Midbrain: Eye movements, pupillary reflexes
- Pons: Facial sensation, sleep regulation
- Medulla: Cardiovascular control, respiratory drive
-
Cerebellum (11% of brain weight, 50% of total neurons)
- Motor coordination, balance, cognitive modulation
- Purkinje cells: 200,000 synaptic inputs per neuron
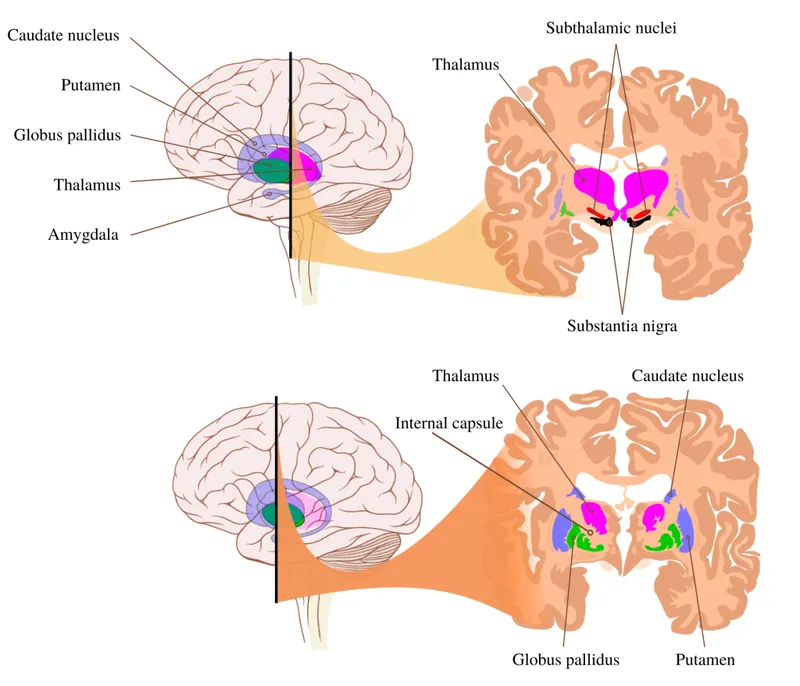
📌 Remember: FLOPT for cerebral lobes - Frontal (executive), Limbic (emotion), Occipital (vision), Parietal (sensation), Temporal (memory). Each lobe's dysfunction creates predictable clinical syndromes with specific percentages of presentation patterns.
Vascular Territory Architecture
| Territory | Artery | Cortical Area | Clinical Deficit | Stroke Frequency |
|---|---|---|---|---|
| Anterior | ACA | Medial frontal/parietal | Leg weakness, personality | 8% of strokes |
| Middle | MCA | Lateral hemisphere | Arm/face weakness, aphasia | 70% of strokes |
| Posterior | PCA | Occipital, temporal | Visual field cuts, memory | 15% of strokes |
| Vertebrobasilar | VA/BA | Brainstem, cerebellum | Dizziness, ataxia, diplopia | 7% of strokes |
💡 Master This: Blood-brain barrier breakdown occurs within 6-24 hours of stroke onset, creating the therapeutic window for thrombolysis. Understanding vascular territories predicts both deficit patterns and recovery potential, with collateral circulation determining final infarct size in 60% of cases.
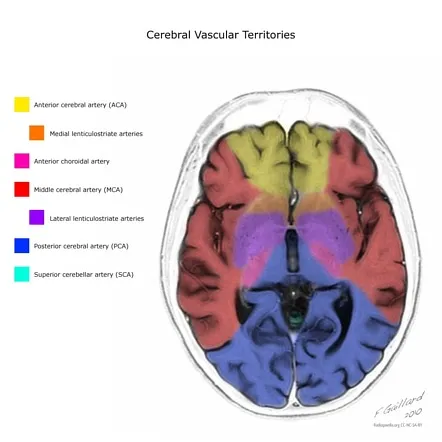
The brain's dual blood supply - anterior circulation (80% of flow) and posterior circulation (20% of flow) - creates predictable clinical patterns. Circle of Willis variations occur in 70% of population, affecting stroke risk and collateral compensation. Autoregulation maintains constant perfusion between 50-150 mmHg mean arterial pressure, failing at extremes and creating watershed infarcts.
📌 Remember: FAST-ED for stroke recognition - Face drooping, Arm weakness, Speech difficulty, Time critical, Eye deviation, Deny/neglect. Each component increases stroke probability: 1 sign = 72%, 2 signs = 85%, 3+ signs = 95% likelihood.
Understanding this neural architecture provides the foundation for recognizing how specific lesions create predictable clinical presentations, setting the stage for mastering the functional systems that transform anatomical knowledge into diagnostic precision.
⚡ The Electrical Highway: Neural Signal Mastery
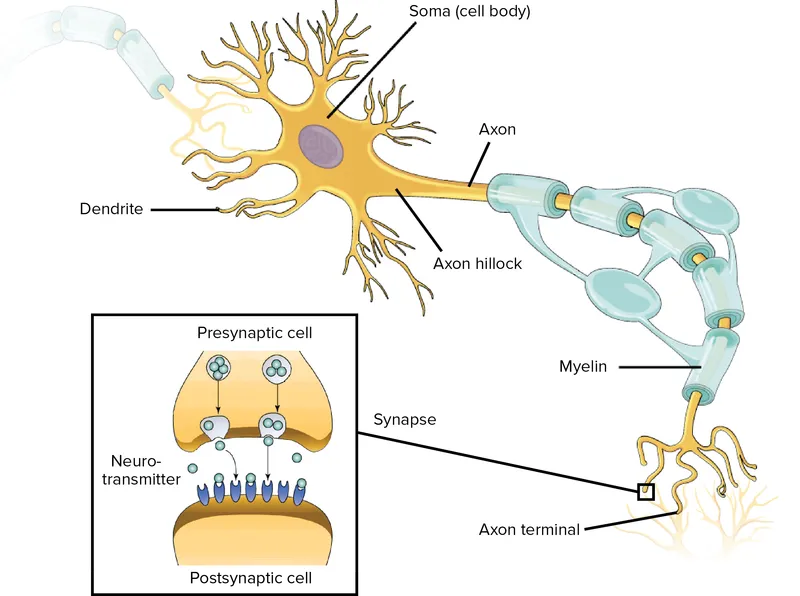
Neural signal transmission operates through precisely orchestrated electrical and chemical events, where resting potential of -70mV creates the foundation for action potential generation. Understanding these mechanisms reveals why neurological diseases create specific patterns of dysfunction and guides therapeutic interventions.
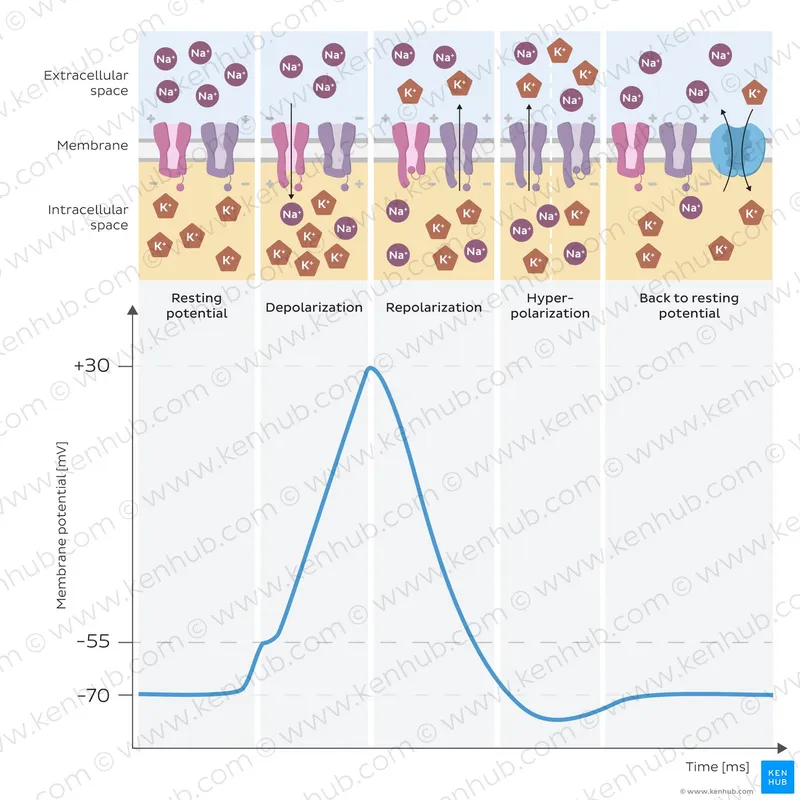
Action Potential Cascade Mechanics
The neural signal represents a carefully choreographed sequence of ionic movements:
-
Resting State (-70mV baseline)
- Na+/K+ ATPase maintains 3:2 exchange ratio
- 140mM K+ intracellular vs 5mM extracellular
- 10mM Na+ intracellular vs 145mM extracellular
- Energy cost: 40% of neuronal ATP consumption
- Pump density: 100-200 pumps per μm² membrane
-
Depolarization Phase (threshold -55mV)
- Voltage-gated Na+ channels open (<1 millisecond)
- 500-fold increase in Na+ permeability
- Membrane potential reaches +30mV peak
- Channel density: 100-200 channels per μm²
- Conduction velocity: 0.5-120 m/s depending on myelination
-
Repolarization Recovery (2-4 milliseconds)
- K+ efflux restores negative potential
- Absolute refractory period: 1-2ms (no new action potential)
- Relative refractory period: 3-4ms (higher threshold required)
📌 Remember: SNAP-K for action potential sequence - Stimulus reaches threshold, Na+ channels open, Action potential peaks, Potassium efflux, K+ restores resting state. Each phase has specific timing: Na+ influx <1ms, K+ efflux 2-4ms, total duration 3-5ms.
Synaptic Transmission Architecture
| Synapse Type | Neurotransmitter | Response Time | Duration | Clinical Significance |
|---|---|---|---|---|
| Excitatory | Glutamate | 0.5ms | 10-20ms | 80% of brain synapses |
| Inhibitory | GABA | 1-2ms | 20-100ms | 20% of brain synapses |
| Cholinergic | Acetylcholine | 0.5ms | 2-5ms | NMJ, autonomic |
| Dopaminergic | Dopamine | 50-100ms | 200-500ms | Movement, reward |
| Serotonergic | Serotonin | 100-300ms | 1-5 seconds | Mood, sleep |
💡 Master This: Myelination increases conduction velocity 50-fold while reducing energy consumption 100-fold. Saltatory conduction between nodes of Ranvier (1-2μm gaps every 150-300μm) explains why demyelinating diseases create conduction blocks and why temperature elevation worsens symptoms in multiple sclerosis patients.
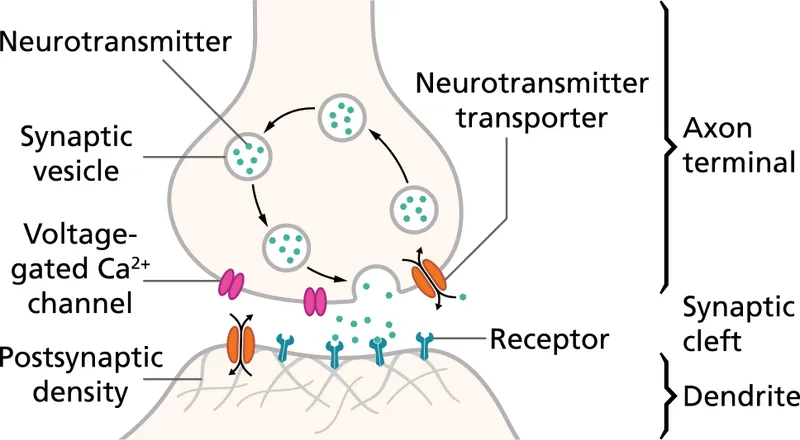
Neurotransmitter synthesis and degradation follow specific pathways that become therapeutic targets. Acetylcholine synthesis requires choline acetyltransferase, while degradation by acetylcholinesterase occurs within 1-2ms. GABA synthesis from glutamate via glutamic acid decarboxylase creates the brain's primary inhibitory system, with benzodiazepines enhancing GABA effectiveness 2-5 fold.
📌 Remember: AGED for cholinesterase inhibition effects - Acetylcholine accumulation, GI hypermotility, Excessive secretions, Depolarizing block. Organophosphate poisoning creates irreversible inhibition lasting weeks to months, while reversible inhibitors (physostigmine) last 2-6 hours.
These electrical and chemical mechanisms create the foundation for understanding how neural networks process information, leading to the pattern recognition systems that enable clinical diagnosis and therapeutic intervention.
🎯 Pattern Recognition Mastery: Clinical Localization Framework
Clinical neurology transforms anatomical knowledge into diagnostic precision through systematic pattern recognition. Upper motor neuron vs lower motor neuron distinction guides 90% of motor complaints, while cortical vs subcortical patterns predict recovery potential and treatment response.
Motor System Localization Matrix
-
Upper Motor Neuron Patterns (cortical/subcortical lesions)
- Spastic weakness: velocity-dependent resistance
- Hyperreflexia: 3+ to 4+ deep tendon reflexes
- Pathological reflexes: Babinski positive in 95% of cases
- Clonus: >5 beats sustained ankle clonus
- Hoffman sign: finger flexion with middle finger flick
- No fasciculations: muscle bulk preserved initially
- Disuse atrophy: develops after 6-12 weeks
-
Lower Motor Neuron Patterns (anterior horn/peripheral nerve)
- Flaccid weakness: constant reduced tone
- Hyporeflexia: 0 to 1+ deep tendon reflexes
- Fasciculations: visible muscle twitching in 80% of cases
- Muscle atrophy: begins within 2-3 weeks
- Fibrillations: EMG detection before clinical atrophy
- Normal plantar response: no pathological reflexes
📌 Remember: UMNLMN comparison - Upper has More tone, No atrophy initially; Lower has Muscle wasting, No reflexes. UMN lesions show spasticity developing over days to weeks, while LMN lesions show immediate flaccidity with atrophy beginning within 2-3 weeks.
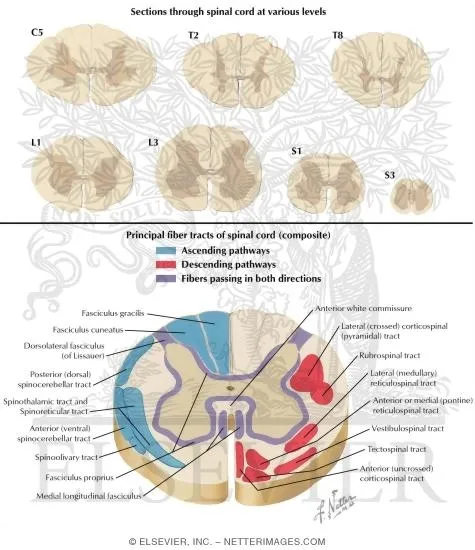
Sensory Localization Patterns
| Location | Pain/Temperature | Vibration/Position | Light Touch | Pattern Name |
|---|---|---|---|---|
| Thalamus | Contralateral loss | Contralateral loss | Contralateral loss | Pure sensory |
| Parietal | Mild deficit | Severe loss | Cortical signs | Cortical sensory |
| Brainstem | Crossed pattern | Variable | Crossed pattern | Alternating |
| Spinal cord | Contralateral | Ipsilateral | Variable | Dissociated |
| Peripheral | Stocking-glove | Distal loss | Length-dependent | Peripheral |
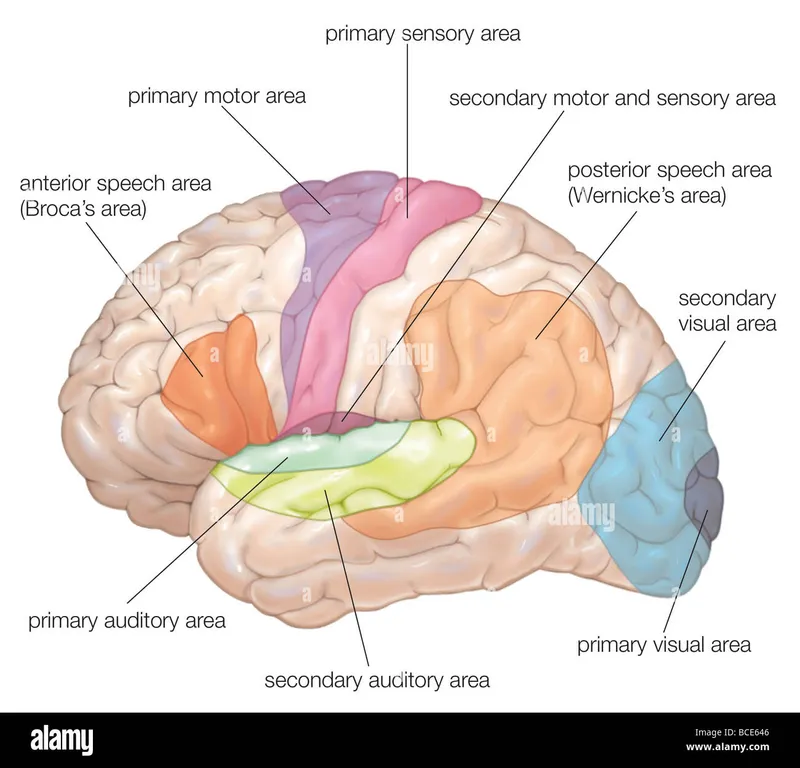
Language Localization Framework
-
Broca's Aphasia (frontal lobe, area 44/45)
- Non-fluent speech: <50 words per minute
- Comprehension preserved: >80% accuracy
- Repetition impaired: telegraphic output
- Associated findings: right hemiparesis in 85% of cases
- Prognosis: moderate recovery in 60% of patients
-
Wernicke's Aphasia (temporal lobe, area 22)
- Fluent speech: >100 words per minute
- Comprehension impaired: <50% accuracy
- Paraphasic errors: semantic and phonemic substitutions
- Associated findings: right visual field cut in 70% of cases
- Prognosis: limited recovery in 30% of patients
-
Conduction Aphasia (arcuate fasciculus)
- Fluent speech: preserved
- Comprehension preserved: >90% accuracy
- Repetition severely impaired: <20% accuracy
- Phonemic paraphasias: prominent during repetition tasks
💡 Master This: Dominant hemisphere (usually left) controls language in 95% of right-handed and 70% of left-handed individuals. Non-dominant hemisphere controls prosody, spatial attention, and emotional content. Crossed aphasia (right hemisphere language) occurs in <5% of right-handed patients.
📌 Remember: FLAW for aphasia types - Fluency (Wernicke's preserved), Language comprehension (Broca's preserved), Arcuate fasciculus (conduction aphasia), Writing (agraphia patterns). Each type has specific recovery patterns and rehabilitation approaches with evidence-based outcomes.
These localization patterns create the diagnostic framework for systematic neurological assessment, enabling precise lesion localization that guides both acute management and long-term prognosis prediction.
🔬 Diagnostic Precision: The Neurological Detective System
Systematic neurological evaluation transforms clinical suspicion into diagnostic certainty through evidence-based discrimination. Sensitivity and specificity values guide test selection, while likelihood ratios quantify diagnostic probability changes with each positive or negative finding.
Diagnostic Test Performance Matrix
| Test | Sensitivity | Specificity | PPV | NPV | Clinical Application |
|---|---|---|---|---|---|
| MRI Brain | 95% | 85% | Variable | 98% | Structural lesions |
| CT Head | 85% | 95% | 90% | 92% | Acute hemorrhage |
| Lumbar Puncture | 90% | 80% | Variable | 95% | Infectious/inflammatory |
| EEG | 70% | 90% | 85% | 80% | Seizure disorders |
| EMG/NCS | 85% | 95% | 92% | 90% | Peripheral neuropathy |
Cerebrospinal Fluid Analysis Framework
-
Normal CSF Parameters
- Cell count: <5 cells/μL (all lymphocytes)
- Protein: 15-45 mg/dL (lumbar), 15-25 mg/dL (ventricular)
- Glucose: 50-80 mg/dL (CSF:serum ratio >0.6)
- Opening pressure: 70-180 mmH2O (lateral decubitus)
- Volume: 150mL total, 500mL daily production
-
Bacterial Meningitis Pattern
- Cell count: >1000 cells/μL (>80% neutrophils)
- Protein: >100 mg/dL (often 200-500 mg/dL)
- Glucose: <40 mg/dL (CSF:serum ratio <0.4)
- Gram stain positive: 60-90% depending on organism
- Culture positive: 70-85% if antibiotics not started
-
Viral Meningitis Pattern
- Cell count: 50-1000 cells/μL (>50% lymphocytes)
- Protein: 50-100 mg/dL (mildly elevated)
- Glucose: >45 mg/dL (normal CSF:serum ratio)
- PCR testing: 85-95% sensitivity for common viruses
📌 Remember: PING for CSF interpretation - Pressure (elevated in bacterial), Inflammatory cells (PMNs vs lymphocytes), Nutrients (glucose low in bacterial), Gram stain (immediate bacterial identification). Bacterial meningitis shows glucose <40 mg/dL in 80% of cases, while viral maintains normal glucose in 90% of cases.
Electrodiagnostic Discrimination Patterns
-
Demyelinating Neuropathy (Guillain-Barré, CIDP)
- Conduction velocity: <80% of normal (usually <40 m/s)
- Distal latency: >125% of normal
- F-wave latency: >125% of normal
- Conduction block: >20% amplitude drop between sites
- Temporal dispersion: >15% duration increase
-
Axonal Neuropathy (diabetic, toxic)
- Amplitude reduction: >50% below normal
- Conduction velocity: mildly reduced (>80% of normal)
- Distal latency: normal or mildly prolonged
- Fibrillations: present in 70% of cases
- Positive sharp waves: denervation markers
-
Myopathic Pattern (muscular dystrophy, inflammatory)
- Small amplitude: <5mV compound muscle action potential
- Short duration: <8ms motor unit potentials
- Early recruitment: >5 motor units with minimal effort
- Normal conduction: velocities preserved
- CK elevation: 5-50x normal in inflammatory myopathy
💡 Master This: Nerve conduction studies differentiate demyelinating (slow conduction) from axonal (low amplitude) neuropathies with 90% accuracy. EMG detects denervation within 2-3 weeks of nerve injury, while reinnervation potentials appear 3-6 months later, predicting recovery potential.
⭐ Clinical Pearl: Carpal tunnel syndrome shows median nerve distal latency >4.5ms with normal ulnar nerve conduction in 95% of cases. Ulnar neuropathy at elbow demonstrates conduction velocity <50 m/s across the elbow segment with >10 m/s slowing compared to forearm segment.
These diagnostic frameworks enable systematic differentiation between neurological conditions, transforming clinical suspicion into evidence-based diagnosis that guides targeted therapeutic interventions.
💊 Therapeutic Precision: Evidence-Based Neurological Interventions
Evidence-based neurology integrates pathophysiology with pharmacokinetics to optimize therapeutic outcomes. Therapeutic drug monitoring, biomarker tracking, and outcome measurement guide treatment adjustments, while combination therapies address multiple pathogenic mechanisms simultaneously.
Antiepileptic Drug Optimization Framework
| Drug | Mechanism | Therapeutic Level | Half-life | Monitoring | Efficacy Rate |
|---|---|---|---|---|---|
| Phenytoin | Na+ channel block | 10-20 μg/mL | 12-36 hours | Free levels | 60-70% |
| Carbamazepine | Na+ channel block | 4-12 μg/mL | 8-20 hours | CBC, LFTs | 65-75% |
| Valproate | Multiple mechanisms | 50-100 μg/mL | 8-20 hours | LFTs, platelets | 70-80% |
| Levetiracetam | SV2A modulation | Not established | 6-8 hours | Renal function | 50-60% |
| Lamotrigine | Na+ channel block | 3-14 μg/mL | 12-60 hours | Rash monitoring | 55-65% |
Stroke Intervention Protocols
-
Acute Ischemic Stroke (<4.5 hour window)
- Alteplase (tPA): 0.9 mg/kg (max 90mg)
- 10% as bolus, 90% over 60 minutes
- Symptomatic ICH risk: 6.4% vs 0.6% placebo
- Excellent outcome (mRS 0-1): 39% vs 26% placebo
- Mechanical thrombectomy: <6 hours (selected cases <24 hours)
- TICI 2b-3 recanalization: 85-90% success rate
- Number needed to treat: 2.6 for functional independence
- Alteplase (tPA): 0.9 mg/kg (max 90mg)
-
Secondary Prevention (post-stroke)
- Antiplatelet therapy: Aspirin 81mg daily
- Clopidogrel 75mg: if aspirin intolerant
- Dual therapy: 21 days for minor stroke/TIA
- Statin therapy: Atorvastatin 80mg daily
- LDL target: <70 mg/dL (<55 mg/dL if high risk)
- Stroke reduction: 16% relative risk reduction
- Antiplatelet therapy: Aspirin 81mg daily
📌 Remember: FAST-ED for stroke treatment windows - Fibrinolysis (<4.5 hours), Anticoagulation reversal (immediate), Surgery consideration (<6-24 hours), Thrombectomy (<6 hours standard), Endovascular (<24 hours selected), Dual antiplatelet (21 days minor stroke). Each intervention has specific inclusion/exclusion criteria and outcome expectations.
Multiple Sclerosis Disease-Modifying Therapy
-
First-line Therapies (relapsing-remitting MS)
- Interferon β-1a: 30 μg IM weekly or 44 μg SC 3x/week
- Relapse reduction: 30-35%
- MRI lesion reduction: 50-70%
- Flu-like symptoms: 60-80% of patients initially
- Glatiramer acetate: 20mg SC daily
- Relapse reduction: 29%
- Injection site reactions: 90% of patients
- Immediate post-injection reaction: 15% (benign)
- Interferon β-1a: 30 μg IM weekly or 44 μg SC 3x/week
-
High-efficacy Therapies (active disease)
- Natalizumab: 300mg IV monthly
- Relapse reduction: 68%
- PML risk: 1:1000 overall, 1:100 high-risk patients
- JC virus monitoring: every 6 months
- Fingolimod: 0.5mg daily
- Relapse reduction: 54%
- First-dose monitoring: 6 hours (bradycardia risk)
- Macular edema: 0.4% incidence
- Natalizumab: 300mg IV monthly
💡 Master This: Disease-modifying therapy should begin immediately after MS diagnosis, as early treatment reduces long-term disability by 30-40%. Escalation therapy to high-efficacy agents is indicated for breakthrough disease (≥1 relapse or ≥2 new T2 lesions annually) or highly active disease at presentation.
⭐ Clinical Pearl: JC virus antibody status stratifies PML risk with natalizumab: seronegative patients have <1:10,000 risk, while seropositive patients with prior immunosuppression and >24 infusions have 1:100 risk. Risk mitigation includes extended interval dosing (every 6-8 weeks) reducing PML risk by 94%.
These evidence-based therapeutic frameworks enable precision medicine approaches in neurology, optimizing treatment selection and monitoring to achieve maximal efficacy while minimizing adverse effects through individualized patient care.
🌐 Neural Network Integration: Advanced Connectivity Mastery
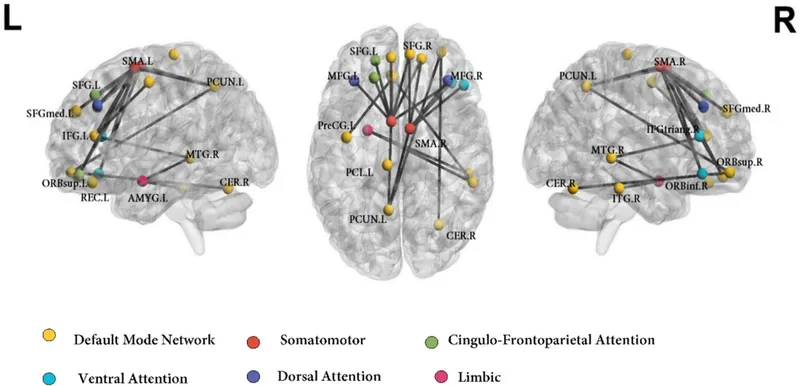
Advanced neuroscience reveals the brain as an integrated network system where functional connectivity between distant regions creates emergent properties that exceed individual component capabilities. Resting-state networks, task-positive networks, and network switching mechanisms explain both normal cognition and neuropsychiatric disorders.
Default Mode Network Architecture
-
Core Hubs (high connectivity nodes)
- Posterior cingulate cortex: central hub with highest connectivity
- Medial prefrontal cortex: self-referential processing
- Angular gyrus: conceptual processing and memory retrieval
- Precuneus: consciousness and self-awareness
- Hippocampus: memory encoding and retrieval
- Network deactivation: occurs during focused tasks
- Task-negative correlation: r = -0.6 to -0.8
-
Clinical Significance (network dysfunction)
- Alzheimer's disease: early DMN disruption in 80% of cases
- Depression: hyperconnectivity within DMN (rumination)
- ADHD: reduced DMN suppression during tasks
- Meditation effects: increased DMN regulation after 8 weeks
- Psychedelics: DMN suppression correlates with ego dissolution
📌 Remember: DMN-TPN switching - Default Mode Network active at rest, Task-Positive Networks active during focused attention. Salience network mediates switching between these states. Network dysfunction underlies cognitive disorders: DMN hyperactivity in depression, reduced switching in ADHD, network fragmentation in schizophrenia.
Executive Control Network Integration
| Network | Key Regions | Primary Function | Connectivity Strength | Clinical Disorders |
|---|---|---|---|---|
| Central Executive | dlPFC, PPC | Working memory, attention | r = 0.4-0.6 | ADHD, schizophrenia |
| Salience | AI, dACC | Network switching | r = 0.5-0.7 | Autism, psychosis |
| Dorsal Attention | FEF, IPS | Top-down attention | r = 0.3-0.5 | Neglect, ADHD |
| Ventral Attention | TPJ, VFC | Bottom-up attention | r = 0.2-0.4 | Spatial neglect |
| Language | Broca's, Wernicke's | Language processing | r = 0.6-0.8 | Aphasia, dyslexia |
Neurotransmitter Network Modulation
-
Dopaminergic System (reward and motivation)
- Ventral tegmental area: reward prediction signaling
- Substantia nigra: movement initiation control
- Striatal projections: goal-directed behavior
- Phasic dopamine: reward prediction error (15% above baseline)
- Tonic dopamine: motivational state maintenance
- Network effects: enhances signal-to-noise ratio by 200-300%
-
Cholinergic System (attention and learning)
- Basal forebrain: cortical arousal and attention
- Brainstem nuclei: REM sleep and memory consolidation
- Nicotinic receptors: fast synaptic transmission (<5ms)
- Muscarinic receptors: slow modulation (100-1000ms)
- Attention enhancement: acetylcholine increases cortical gamma by 40-60%
-
Noradrenergic System (arousal and stress response)
- Locus coeruleus: global arousal regulation
- Network-wide effects: modulates all major networks
- Inverted-U function: optimal performance at moderate levels
- Stress response: norepinephrine increases network switching by 50-100%
- Cognitive flexibility: enhanced at moderate arousal, impaired at extremes
💡 Master This: Neurotransmitter systems create network states that determine cognitive capacity. Dopamine enhances reward networks and executive control, acetylcholine sharpens attention networks, and norepinephrine modulates arousal and network flexibility. Pharmacological interventions targeting these systems can restore network function in psychiatric disorders.
📌 Remember: DANCE for neurotransmitter network effects - Dopamine (reward/executive), Acetylcholine (attention/learning), Norepinephrine (arousal/flexibility), Cortisol (stress/memory), Endorphins (pain/mood). Each system has specific network targets and therapeutic windows for optimal cognitive enhancement.
Understanding neural network integration reveals how distributed brain systems create complex behaviors and how network dysfunction underlies neurological and psychiatric disorders, providing targets for precision therapeutic interventions.
🎖️ Clinical Command Center: Rapid Neurological Mastery Arsenal
Essential Clinical Arsenal
- Rapid Assessment Framework (<5 minutes)
- ABCDE approach: Airway, Breathing, Circulation, Disability, Exposure
- Glasgow Coma Scale: Eye (4) + Verbal (5) + Motor (6) = 15
- NIHSS stroke scale: 42-point scale, >15 = severe stroke
- Time windows: tPA <4.5 hours, thrombectomy <6-24 hours
- Blood pressure: maintain <185/110 for thrombolysis
- Seizure protocol: lorazepam 0.1 mg/kg, max 4mg IV push
📌 Remember: TIME-BRAIN for stroke urgency - Time is brain (1.9 million neurons/minute), Imaging immediately, Medications ready, Endovascular team alert. Blood pressure control, Rapid assessment, Anticoagulation reversal, Intensive monitoring, Neurological checks hourly.
Critical Threshold Reference
| Parameter | Normal Range | Mild Abnormal | Severe Abnormal | Action Required |
|---|---|---|---|---|
| ICP | 5-15 mmHg | 16-20 mmHg | >20 mmHg | Immediate intervention |
| CPP | 60-70 mmHg | 50-59 mmHg | <50 mmHg | Vasopressor support |
| GCS | 13-15 | 9-12 | <9 | Intubation consideration |
| Glucose | 70-140 mg/dL | 50-69, 141-180 | <50, >180 | Immediate correction |
| Sodium | 135-145 mEq/L | 130-134, 146-150 | <130, >150 | Gradual correction |
💡 Master This: Neurological emergencies follow time-critical protocols where minutes determine outcomes. Status epilepticus requires benzodiazepines within 5 minutes, antiepileptics within 20 minutes, and anesthesia within 40 minutes if seizures persist. Stroke intervention success rates decline 10-15% for every 15-minute delay.
Master these frameworks, and you possess the clinical command center for neurological excellence - transforming complex presentations into systematic, evidence-based care that optimizes patient outcomes through precision medicine approaches.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app












