Frailty and Sarcopenia - Defining Decline
- Frailty: Clinical syndrome; ↑vulnerability to stressors from multisystem physiological decline.
- Fried Phenotype: ≥3 criteria (weight loss >4.5kg/yr, exhaustion, weakness, slowness, low activity).
- Sarcopenia: Age-related loss of muscle mass, strength (e.g. handgrip), and/or physical performance (gait speed <0.8 m/s).
| Frailty | Sarcopenia | |
|---|---|---|
| Core Defect | Multisystem reserve loss | ↓Muscle mass, strength, function |
| Impact | ↑Vulnerability, poor stress recovery | ↑Falls, disability, ↓QoL |
Frailty and Sarcopenia - Roots of Weakness
Underlying mechanisms driving age-related decline:
- Inflammation: Chronic low-grade ("inflammaging") with ↑ IL-6, TNF-α promoting muscle breakdown.
- Anabolic Resistance: Impaired muscle protein synthesis despite adequate stimuli.
- Neuromuscular Degeneration: Loss of motor units, ↓ nerve conduction velocity.
- Mitochondrial Dysfunction: ↓ ATP, ↑ reactive oxygen species (ROS) damaging muscle cells.
- Hormonal Dysregulation: ↓ anabolic hormones (testosterone, IGF-1), ↑ catabolic hormones (cortisol).
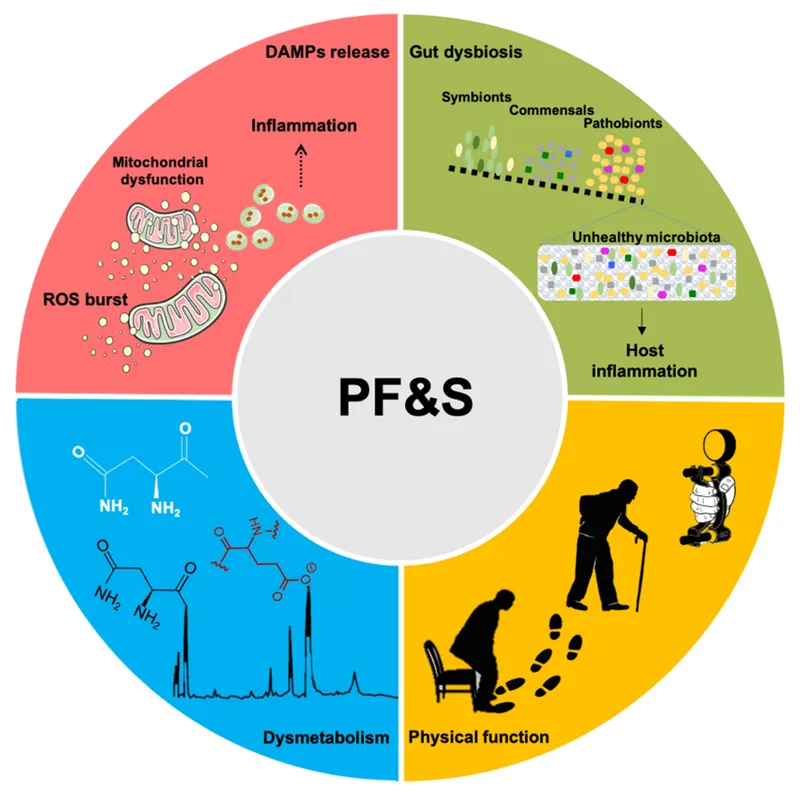
⭐ Sarcopenia is defined by low muscle mass, plus low muscle strength or low physical performance. Gait speed < 0.8 m/s is a critical threshold for assessing physical performance_._
Frailty and Sarcopenia - Clinical Clues & Criteria
- Frailty Clues: Weakness, fatigue, unintentional wt. loss, slow gait, ↓ physical activity.
- Sarcopenia Clues: ↓ Muscle mass, strength & performance; increased falls, slow gait.
Diagnostic Criteria:
| Condition | Criteria (Abbr.) | Diagnosis |
|---|---|---|
| Frailty | Fried's Phenotype: - Unintentional Wt. Loss (≥4.5kg or >5%/yr) - Exhaustion - Weakness (grip) - Slow Walk Speed - Low Physical Activity | Frail: ≥3 criteria Pre-frail: 1-2 criteria |
| Sarcopenia | EWGSOP2: 1. Low Muscle Strength 2. Low Muscle Quantity/Quality 3. Low Physical Performance (for severe) | Probable: 1 Confirmed: 1+2 Severe: 1+2+3 |
Sarcopenia Diagnosis (EWGSOP2 Algorithm):
⭐ Sarcopenia (low muscle strength + low muscle quantity/quality) is a strong predictor of disability, morbidity, and mortality in older adults.
Frailty and Sarcopenia - Geriatric Gauges
- Key Assessment Tools:
- Handgrip Strength: Measured by dynamometer (e.g., < 27 kg men, < 16 kg women - EWGSOP2 criteria for probable sarcopenia).
- Gait Speed: Time to walk 4 meters; < 0.8 m/s indicates frailty/sarcopenia.
- Short Physical Performance Battery (SPPB): Assesses balance, gait, chair stands; score ≤ 8 suggests frailty.
- Chair Stand Test: Time for 5 sit-to-stand repetitions; > 15 seconds indicates poor function.
- Muscle Mass: DXA (gold standard), BIA, CT/MRI.
⭐ Sarcopenia (EWGSOP2): Low muscle strength (e.g., grip strength) is the primary parameter. If low strength is present, assess for low muscle quantity/quality. If both are present, sarcopenia is confirmed. Severe sarcopenia includes low physical performance (e.g., gait speed).
Frailty and Sarcopenia - Intervention Strategies
- Exercise: Cornerstone; multi-component programs most effective.
- Resistance training: Builds muscle mass & strength.
- Aerobic exercise: Improves cardiovascular fitness.
- Balance & flexibility: Reduces fall risk.
- Nutrition: Crucial for muscle health.
- Protein intake: Target $1.2-1.5 \text{ g/kg/day}$.
- Vitamin D: Supplement if levels low ($< \textbf{20 ng/mL}$ or $< \textbf{50 nmol/L}$).
- Omega-3 fatty acids: Consider for anti-inflammatory effects.
- Medication Review:
- Reduce polypharmacy; deprescribe non-essential/harmful drugs.
- Psychosocial Support:
- Address depression, anxiety, social isolation.
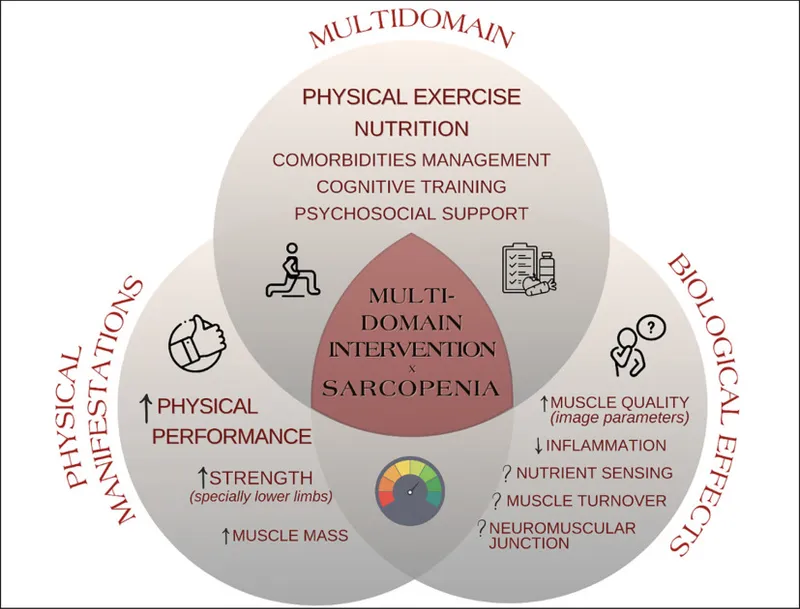
⭐ Resistance exercise is the most effective single intervention to counteract sarcopenia and improve muscle strength in older adults.
High‑Yield Points - ⚡ Biggest Takeaways
- Frailty is ↑ vulnerability to stressors from ↓ physiological reserves.
- Clinical Frailty Scale (CFS) is a common tool (1-Very Fit to 9-Terminally Ill).
- Sarcopenia is age-related loss of muscle mass, strength, and function.
- Sarcopenia diagnosis: Low muscle mass plus low strength OR low physical performance.
- EWGSOP2 criteria guide sarcopenia diagnosis, prioritizing muscle strength.
- Management: Optimal protein (1.2-1.5 g/kg/day) and resistance exercise.
- Both conditions ↑ risk of falls, disability, hospitalization, and mortality.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

