Epidemiology & Impact - Geriatric Ground Zero
- Prevalence: 1 in 3 adults >65 years fall each year; rates ↑ with age & in long-term care.
- Common Injuries: Hip fractures (high morbidity/mortality), traumatic brain injuries (TBI), wrist & vertebral fractures.
- Consequences:
- Significant cause of hospitalization & ↑ healthcare utilization.
- Leads to disability, loss of independence, premature institutionalization.
- Fear of Falling (FoF) cycle: ↓ activity → deconditioning → ↑ fall risk.
- Major contributor to injury-related death in the elderly.

⭐ Falls are a leading cause of non-fatal injuries and hospital admissions for trauma in older adults.
Risk Factors - Stumble Suspects
| Category | Examples |
|---|---|
| Intrinsic | Age-related changes (gait, balance, vision ↓, proprioception ↓), chronic diseases (arthritis, Parkinson's, stroke, dementia, postural hypotension), polypharmacy (≥4-5 medications) |
| Extrinsic | Environmental hazards (poor lighting, loose rugs, clutter, unsafe stairs), improper footwear |
- Illumination (poor)
- Hazards (environmental)
- Assistive devices (lack/improper use)
- Transfer techniques (unsafe)
- Education (lack of awareness)
- Footwear (inappropriate)
- Age-related changes
- Low blood pressure (postural hypotension)
- Locomotor problems (gait/balance)
- Incontinence (urgency leading to rush)
- Nutrition (malnutrition, vitamin D deficiency)
- General debility/frailty
⭐ Postural hypotension (a drop of ≥20 mmHg systolic or ≥10 mmHg diastolic BP within 3 mins of standing) is a common, often reversible, cause of falls in the elderly and frequently linked to medications like antihypertensives and diuretics. Polypharmacy significantly elevates this risk when ≥4-5 medications are used concurrently, especially sedatives and psychotropics.
Assessment & Screening - Tumble Detectives
- Comprehensive Geriatric Assessment (CGA): Holistic evaluation to identify risk factors.
- Fall History: Detailed account of fall circumstances.
- 📌 SPLATT Mnemonic:
- Symptoms at time of fall
- Previous falls
- Location of fall
- Activity at time of fall
- Time of day
- Trauma post-fall
- 📌 SPLATT Mnemonic:
- Medication Review: Identify polypharmacy & high-risk drugs (e.g., sedatives, antihypertensives).
- Physical Examination:
- Vision & hearing acuity.
- Cardiovascular: Orthostatic hypotension (check BP lying & standing).
- Neurological: Cognition, peripheral neuropathy, reflexes.
- Musculoskeletal: Gait, balance (e.g., Romberg), muscle strength (e.g., chair stand test).
- Functional Assessment Tools:
- Timed Up and Go (TUG) Test: >12-14 seconds indicates ↑ fall risk.
- Berg Balance Scale (BBS).
- Tinetti Performance Oriented Mobility Assessment (POMA).
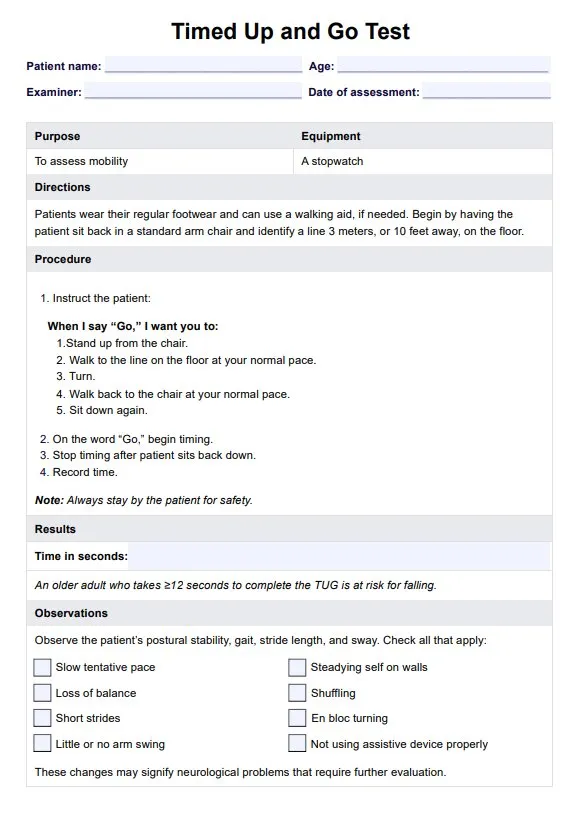
⭐ The 'Timed Up and Go' (TUG) test is a simple, widely used tool to assess mobility and predict fall risk; a time >12-14 seconds indicates a high risk of falling and warrants further assessment.
Prevention & Management - Safety Shield Plan
Key interventions:
- Additional Fall Prevention:
- Vision Correction: Regular eye exams, updated eyewear.
- Footwear Advice: Proper fit, low heel, non-slip soles.
Core Intervention Domains Table:
| Domain | Key Actions & Recommendations |
|---|---|
| Exercise Programs | Balance, strength, gait training (e.g., Tai Chi). Regular participation. |
| Medication Review | Reduce/stop high-risk drugs (psychotropics, sedatives); address polypharmacy. |
| Environmental Modification | Home safety: improve lighting, remove hazards (rugs), install grab bars, non-slip surfaces. |
| Osteoporosis Management | Screen: DEXA (T-score ≤ -2.5), FRAX. Supplements: Calcium (1000-1200 mg/day), Vit D (800-1000 IU/day). Meds: Bisphosphonates, Denosumab, Teriparatide. |
Simplified Osteoporosis Management Post-Fall:
High‑Yield Points - ⚡ Biggest Takeaways
- Multifactorial risk assessment is crucial for preventing falls in older adults.
- The Timed Up and Go (TUG) test; >12 seconds indicates an increased fall risk.
- Vitamin D (800-1000 IU/day) and Calcium (1000-1200 mg/day) supplementation is vital for bone health.
- Bisphosphonates (e.g., Alendronate, Zoledronic acid) are first-line pharmacological therapy for osteoporosis.
- Regular exercise programs incorporating balance, strength, and gait training significantly reduce fall incidence.
- Conduct a thorough medication review to identify and minimize high-risk drugs (e.g., psychotropics, polypharmacy).
- Home environment assessment and modification can substantially reduce extrinsic fall hazards for elderly patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

