CGA Fundamentals - Geriatric Super‑Scan
- Definition: Multidimensional, interdisciplinary diagnostic process to identify care needs & develop a coordinated plan for frail older adults.
- Goal: Improve health outcomes, functional status, & quality of life.
- Core Components (The "5 M's" 📌):
- Mobility (gait, balance, falls)
- Mind (cognition, mood)
- Medications (polypharmacy, appropriateness)
- Multicomplexity (comorbidities, social support, environment)
- Matters Most (patient goals, advance care planning)
- Key Indications:
- Age >75-80 years with functional decline
- Multiple comorbidities or frailty
- Geriatric syndromes (e.g., falls, dementia, delirium, incontinence)
- Recent significant hospitalization or change in living situation
- Benefits: ↓ mortality, ↓ hospital readmission & length of stay, ↑ functional independence, ↑ diagnostic accuracy, improved quality of life.
⭐ CGA is most effective for frail older adults at high risk of adverse outcomes (e.g., functional decline, institutionalization), not universally for all older individuals.
CGA Domains - The Geriatric Checkpoints
- Systematic evaluation of medical, functional, psychosocial, & environmental issues to inform care plans.
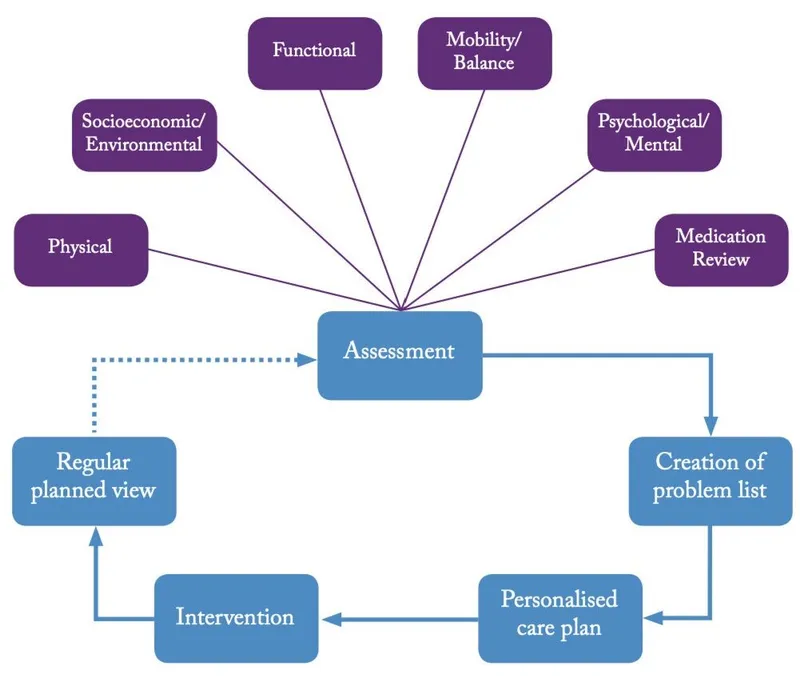
- 1. Medical & Physical Health:
- Disease burden, co-morbidities; medication review (polypharmacy: ≥5 drugs).
- Nutritional status (e.g., MNA, weight loss).
- Sensory function (vision, hearing deficits).
- Pain (acute/chronic, functional impact).
- Urinary continence.
- Fall risk (history; TUG >12s = high risk).
- 2. Functional Status:
- Activities of Daily Living (ADLs) (Katz Index: e.g., bathing, dressing, toileting, transfers).
- Instrumental ADLs (IADLs) (Lawton Scale: e.g., finances, meds, shopping, transport).
- Mobility & Gait (Gait speed <0.8 m/s = poor outcome; balance).
- 3. Psychological & Cognitive Health:
- Cognition (e.g., MMSE, MoCA, Mini-Cog for dementia/MCI).
- Mood (e.g., GDS >5 = depression; anxiety).
- Delirium (e.g., CAM for acute confusion).
- 4. Socio-environmental Factors:
- Social support, caregiver well-being.
- Home environment (safety, suitability).
- Financial resources.
- Access to services & healthcare.
⭐ Functional ability (ADLs/IADLs) robustly predicts mortality & institutionalization, often more than specific medical diagnoses.
CGA Toolkit & Action - Assess & Address
- Goal: Develop coordinated care plan to optimize health & functional independence.
- Key Assessment Tools (Domains):
- Mobility: Timed Up and Go (TUG; >12s ↑fall risk), Gait speed (<0.8m/s frailty marker)
- Cognition: MMSE (<24 suggests impairment), Mini-Cog, MoCA
- Mood: Geriatric Depression Scale (GDS-15; >5 indicative)
- Nutrition: MNA-SF (≤11 malnutrition risk)
- Function: ADL (Katz - basic), IADL (Lawton - complex)
- Polypharmacy: Beers criteria, STOPP/START tools
- Sensory: Vision (Snellen chart), Hearing (Whisper test, audioscopy)
- Social & Environmental: Support systems, home safety
- Interdisciplinary Team (IDT): Geriatrician, nurse, physiotherapist, occupational therapist, pharmacist, social worker, dietitian.
- CGA Workflow & Key Outcomes:
⭐ CGA is proven to reduce hospital admissions, length of stay, institutionalization, and mortality, while improving diagnostic accuracy and functional status.
High‑Yield Points - ⚡ Biggest Takeaways
- CGA (Comprehensive Geriatric Assessment) is a multidimensional, interdisciplinary process assessing medical, psychosocial, and functional capabilities in frail elderly.
- Key domains include: medical conditions, cognitive status (e.g., MMSE), functional status (ADLs, IADLs), mood (e.g., GDS), nutritional status (e.g., MNA), polypharmacy, and social support.
- Functional decline (impairment in ADLs/IADLs) and polypharmacy (≥5 medications) are major targets, strongly predicting adverse outcomes.
- Gait speed (often called the "sixth vital sign") and the Timed Up and Go (TUG) test are crucial for assessing mobility and fall risk.
- CGA aims to improve functional status, quality of life, reduce hospitalization and institutionalization, and effectively manage geriatric syndromes (e.g., falls, delirium, frailty, incontinence).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

