IPC Fundamentals - Teamwork Makes Dream Work
- Definition: Multiple health workers from different professional backgrounds provide comprehensive services by working with patients, their families, carers, and communities to deliver the highest quality of care across settings (WHO).
- Core Components & Principles:
- Values & Ethics: Mutual respect, shared trust, patient-centeredness.
- Roles & Responsibilities: Clarity of own and others' roles; recognizing legal boundaries.
- Interprofessional Communication: Active listening, timely, accurate information sharing. (📌 Use SBAR: Situation, Background, Assessment, Recommendation for structured handoffs).
- Teams & Teamwork: Shared leadership, collaborative problem-solving, joint decision-making.
- Significance & Benefits:
- ↑ Patient safety & quality of care.
- ↓ Medical errors & length of hospital stay.
- ↑ Efficiency, care coordination, and resource utilization.
- ↑ Patient & provider satisfaction.
⭐ Effective Interprofessional Collaboration (IPC) is a core competency emphasized by the National Medical Commission (NMC) for Indian Medical Graduates, crucial for addressing complex health needs and improving patient outcomes in diverse settings like primary health centres (PHCs) and tertiary hospitals alike.
IPC Team Dynamics - Playing Your Part
-
Core Elements for Success:
- Defined Roles & Responsibilities: Understand your scope and others'.
- Open Communication: Essential for safety and coordination. Use tools like SBAR.
- Shared Patient-Centered Goals: Unified team vision.
- Mutual Respect & Trust: Forms the bedrock of collaboration.
- Collaborative Decision-Making: Involve all relevant expertise.
-
Playing Your Part Effectively:
- Be Accountable, Proactive, and Reliable.
- Communicate Clearly & Concisely (e.g., SBAR, closed-loop).
- Practice Active Listening & Value Diverse Inputs.
- Offer & Accept Constructive Feedback and Support.
- Engage in Conflict Resolution constructively.

⭐ Studies show effective IPC significantly reduces medical errors by improving communication and coordination, directly impacting patient safety.
📌 TEAM for high-functioning teams:
- Trust: Build and maintain.
- Effective Communication: Clear, timely, respectful.
- Accountability: Individual and shared.
- Mutual Support: Assist and empower colleagues.
IPC Challenges & Solutions - Hurdles & Handshakes
- Hurdles (Barriers):
- Traditional hierarchies, power imbalances
- Communication gaps: discipline-specific jargon, differing styles
- Ambiguous roles, unclear responsibilities
- Time pressures, heavy clinical workloads
- Insufficient interprofessional education (IPE)
- Resistance to change, entrenched professional silos
- Handshakes (Solutions):
- Define clear roles, establish shared patient-centered goals
- Utilize standardized communication tools (e.g., SBAR, ISBAR)
- Conduct regular team meetings, briefings, and debriefings
- Implement joint training: Interprofessional Education (IPE)
- Foster leadership support, mutual respect, and trust
- Develop structured conflict resolution pathways
⭐ Studies show effective IPC significantly reduces preventable medical errors and improves patient safety outcomes.
IPC Impact & Models - Better Care Together
- Impact of Effective IPC:
- Enhanced patient safety: ↓ medical errors, ↓ preventable adverse events.
- Improved patient outcomes: Better chronic disease management, ↑ treatment adherence.
- Increased patient satisfaction: Holistic, coordinated, patient-centered care.
- Optimized resource utilization: ↓ hospital readmissions, ↓ length of stay, ↓ healthcare costs.
- Improved healthcare provider well-being: ↑ job satisfaction, ↓ burnout, shared responsibility.
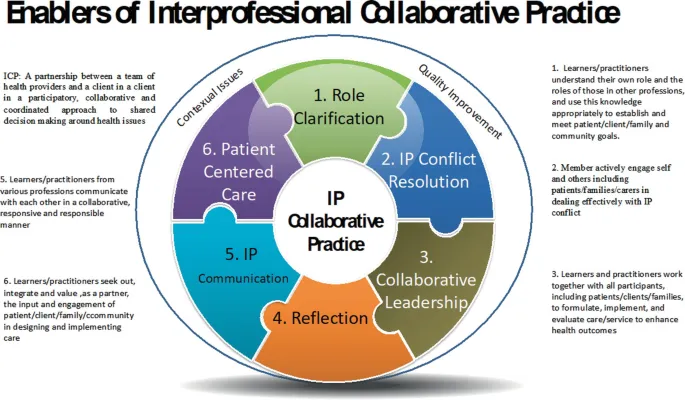
- Key IPC Models & Principles:
- WHO Framework for Action on IPE & Collaborative Practice: Focuses on mechanisms, context, and outcomes for collaborative practice.
- Interprofessional Education Collaborative (IPEC) Core Competencies: Values/Ethics, Roles/Responsibilities, Interprofessional Communication, Teams/Teamwork.
- Underlying principles: Shared goals, mutual respect, clear roles, effective communication, shared decision-making.
⭐ Effective interprofessional collaboration has been shown to reduce patient mortality rates by up to 20% in specific acute care settings and significantly decrease medical errors related to miscommunication during patient handoffs (e.g., SBAR implementation).
High‑Yield Points - ⚡ Biggest Takeaways
- Interprofessional Collaboration (IPC) is essential for optimal patient outcomes and safety.
- Effective teams require mutual respect, shared goals, and clear communication.
- Key members include doctors, nurses, pharmacists, and other allied health professionals.
- SBAR (Situation, Background, Assessment, Recommendation) is a crucial communication tool.
- Common barriers: hierarchical attitudes, poor communication, and undefined roles.
- Successful IPC improves patient satisfaction, reduces errors, and enhances team morale.
- Shared decision-making and accountability are central to effective teamwork.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

