Physiology & Acclimatization - Thin Air Acclimation
- Altitude Zones: High (2500-3500m), Very High (3500-5500m), Extreme (>5500m). Illness risk >2500m.
- Initial Response (Hypobaric Hypoxia → $P_{IO_2}$ ↓; $P_{IO_2} = (P_B - P_{H_2O}) \times F_{IO_2}$): Peripheral chemoreceptors (carotid bodies) → Hyperventilation → Respiratory Alkalosis ($P_{aCO_2}$ ↓).
- Acclimatization (HIF-1α mediated):
- Hours: Renal $HCO_3^-$ excretion (compensates alkalosis).
- Days-Weeks: ↑EPO → ↑RBC mass; ↑2,3-DPG (ODC right shift); ↑capillary & mitochondrial density. 📌 Mnemonic ("HALEO"): Hyperventilation, Alkalosis (initial), Later renal compensation, EPO increase, Oxygen dissociation curve shifts right.

⭐ The primary stimulus for ventilation at high altitude is hypoxia, sensed by carotid bodies.
Acute Mountain Sickness (AMS) - Headache Heights
- Definition: Symptom complex (headache + others) occurring 6-12h after rapid ascent to altitudes >2500m (8000ft).
- Pathophysiology: Hypoxia → cerebral vasodilation → ↑cerebral blood flow → ↑intracranial pressure (ICP) / mild cerebral edema.
- Symptoms: Headache PLUS ≥1 of:
- Gastrointestinal upset (anorexia, nausea, vomiting)
- Fatigue or weakness
- Dizziness or lightheadedness
- Difficulty sleeping
- 📌 Mnemonic: "Altitude Sickness Is A DRAG" (Dizziness, Retreat/difficulty sleeping, Anorexia/Nausea, General malaise/fatigue)
- Diagnosis: Lake Louise Scoring System (LLSS). AMS if score ≥3 with headache.
- Headache (0-3)
- GI symptoms (0-3)
- Fatigue/weakness (0-3)
- Dizziness/lightheadedness (0-3)
- Difficulty sleeping (0-3)

- ⭐
Headache is the cardinal symptom of Acute Mountain Sickness.
Severe Altitude Illnesses - Brain Lung Alarms
- Critical, life-threatening conditions requiring rapid diagnosis and immediate descent.
| Feature | HACE (High Altitude Cerebral Edema) | HAPE (High Altitude Pulmonary Edema) |
|---|---|---|
| Nature/Onset | Severe AMS progression; brain swelling. Onset typically hours to days. | Non-cardiogenic pulmonary edema. Can be rapid (hours-days), may occur without preceding AMS. |
| Key Symptoms | Severe headache, nausea/vomiting, profound lethargy → ataxia, confusion, altered consciousness, coma. | Dyspnea at rest, persistent cough (frothy/pink sputum), chest tightness, extreme fatigue. |
| Key Signs | Ataxia (critical!), papilledema, retinal hemorrhages, ↓consciousness. 📌 "Can't Walk, Can't Talk" | Tachypnea, tachycardia, cyanosis, rales/crackles on auscultation. 📌 "Can't Breathe, Frothy Wreath" |
| Pathophysiology | Vasogenic/cytotoxic cerebral edema due to hypoxia. | Uneven hypoxic pulmonary vasoconstriction → ↑pulmonary artery pressure → capillary leakage. |
| Primary Treatment | Immediate Descent, Oxygen, Dexamethasone (8mg stat, then 4mg 6-hourly) | Immediate Descent, Oxygen, Nifedipine (30mg SR BD or 10mg stat then 20mg SR), CPAP/PEEP |
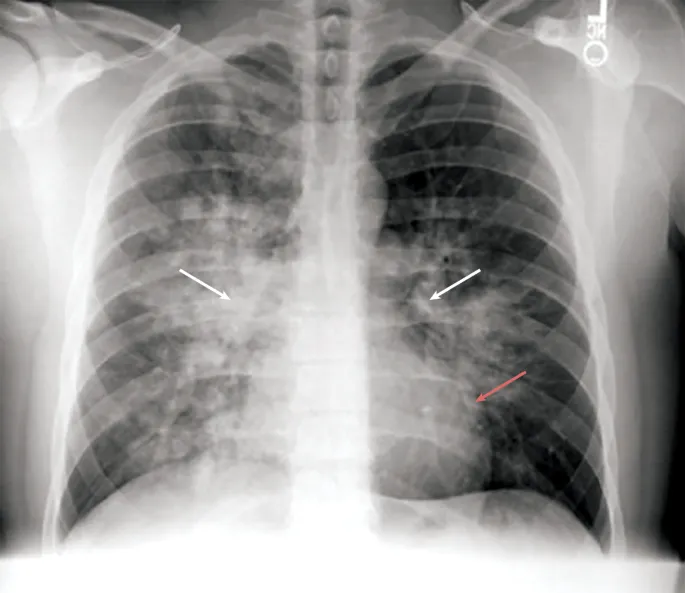
Prevention & Management - Summit Smartly
-
Prevention Strategies:
- Gradual ascent: Max 300-500m sleep altitude ↑ per day above 3000m.
- Rest days every 2-3 days. "Climb high, sleep low."
- Avoid alcohol & sedatives.
- 📌 Mnemonic: "Don't GO UP FAST" - Gradual ascent, Oxygen if needed, Understand symptoms, Prophylaxis, Fluids, Acclimatize, Sleep low, Take rest days.
-
Pharmacological Prophylaxis:
Drug Dose Indication MOA Summary (brief) Key Side Effects (brief) Acetazolamide 125mg BD (start 24h prior) Standard prophylaxis ↑Ventilation (via HCO₃⁻ diuresis) Paresthesias, polyuria Dexamethasone - Acetazolamide intolerant/allergic, rapid ascent Anti-inflammatory Hyperglycemia, mood changes Nifedipine - HAPE-susceptible ↓Pulm. artery pressure Hypotension, headache -
General Management Principles:
- ABCs. Descent is key for severe illness.
- Oxygen therapy.
- Gamow bag (portable hyperbaric chamber).
⭐ Acetazolamide speeds acclimatization by inducing bicarbonate diuresis and metabolic acidosis, stimulating ventilation.
High‑Yield Points - ⚡ Biggest Takeaways
- Acclimatization is key; gradual ascent and acetazolamide are prophylactic.
- AMS: headache, nausea; treat with descent, O2, acetazolamide.
- HACE: ataxia, altered mental status; immediate descent, dexamethasone.
- HAPE: dyspnea, cough, rales; immediate descent, O2, nifedipine.
- Prevent with staged ascent: sleep no >300-500m higher daily above 3000m.
- Acetazolamide: induces metabolic acidosis, stimulating ventilation for acclimatization.
- Gamow bag simulates descent, a temporizing measure for severe illness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

