Thyroid Basics & Tests - Gland Central
- Physiology: Thyroid synthesizes T4 (thyroxine) & T3 (triiodothyronine) from iodine & thyroglobulin. T4 is major circulating hormone; T3 is more potent (3-4x) & active, mostly from peripheral T4 conversion. C-cells: calcitonin.
- HPT Axis Regulation:
- Core Tests:
- TSH: Best initial. Normal: 0.4-4.0 mIU/L.
- ↑ TSH, ↓ fT4: Primary Hypothyroidism.
- ↓ TSH, ↑ fT4/fT3: Primary Hyperthyroidism.
- fT4, fT3: Unbound, metabolically active forms.
- Antibodies: Anti-TPO (Hashimoto’s), TRAb (Graves’).
- Imaging: USG (nodules), RAIU (differentiates hyperthyroidism causes).
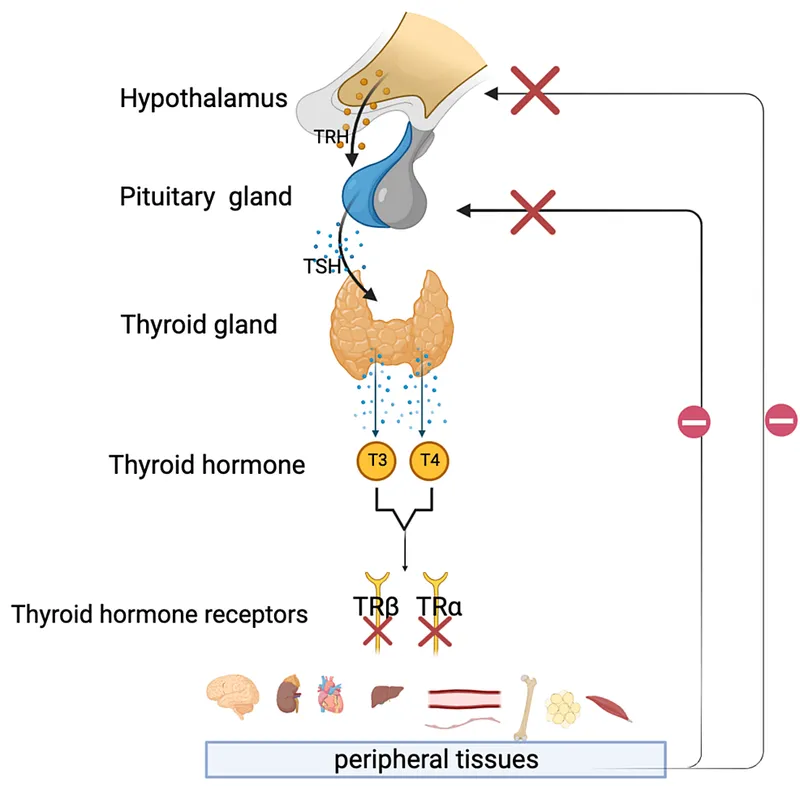
- TSH: Best initial. Normal: 0.4-4.0 mIU/L.
⭐ TSH is the most sensitive screening test for primary thyroid disorders.
Hypothyroidism - Slow & Low Show
- Definition: Clinical syndrome from ↓ thyroid hormone action.
- Etiology:
- Primary (thyroid failure): Hashimoto's (anti-TPO Ab+), iatrogenic (post-radioiodine/surgery), iodine deficiency, drugs (Li, amiodarone).
- Secondary: ↓ Pituitary TSH.
- Tertiary: ↓ Hypothalamic TRH.
- Clinical Features (Sx): Fatigue, weight gain, cold intolerance, constipation, hoarseness, dry skin, hair loss, bradycardia, delayed reflexes (Woltman sign).

- Diagnosis (Dx):
- Primary: ↑TSH, ↓FT4.
- Central: ↓/Normal TSH, ↓FT4.
- Management (Rx): Levothyroxine 1.6 mcg/kg/day. Monitor TSH (target 0.5-2.5 mIU/L).
- Complication: Myxedema coma: severe hypothyroidism → hypothermia, bradycardia, hypoglycemia, hyponatremia, altered mental status (AMS) ⚠️.
⭐ Subclinical hypothyroidism (↑TSH, normal FT4): Treat if TSH >10 mIU/L, or if symptomatic, pregnant, or goiter with TSH <10 mIU/L (e.g., TSH 7-9.9 mIU/L).
Hyperthyroidism - Fast & Furious Gland
- Etiology: Excess thyroid hormone (TH) production.
- Graves' Disease (most common; autoimmune, TRAb+)
- Toxic Multinodular Goiter (TMNG)
- Toxic Adenoma
- Thyroiditis (transient hyperthyroid phase, e.g., De Quervain's)
- Clinical Features: Weight ↓ despite ↑appetite, heat intolerance, palpitations, tachycardia, tremor, anxiety, goiter, lid lag/stare.
- Graves' Specific: Exophthalmos, pretibial myxedema, thyroid acropachy.
- Diagnosis:
- Screen: ↓TSH (often <0.01 mIU/L), ↑Free T4/T3.
- Etiology: Thyroid autoantibodies (TRAb for Graves').
- Radioiodine Uptake (RAIU): Graves' (diffuse ↑), TMNG/Adenoma (nodular ↑), Thyroiditis (↓).
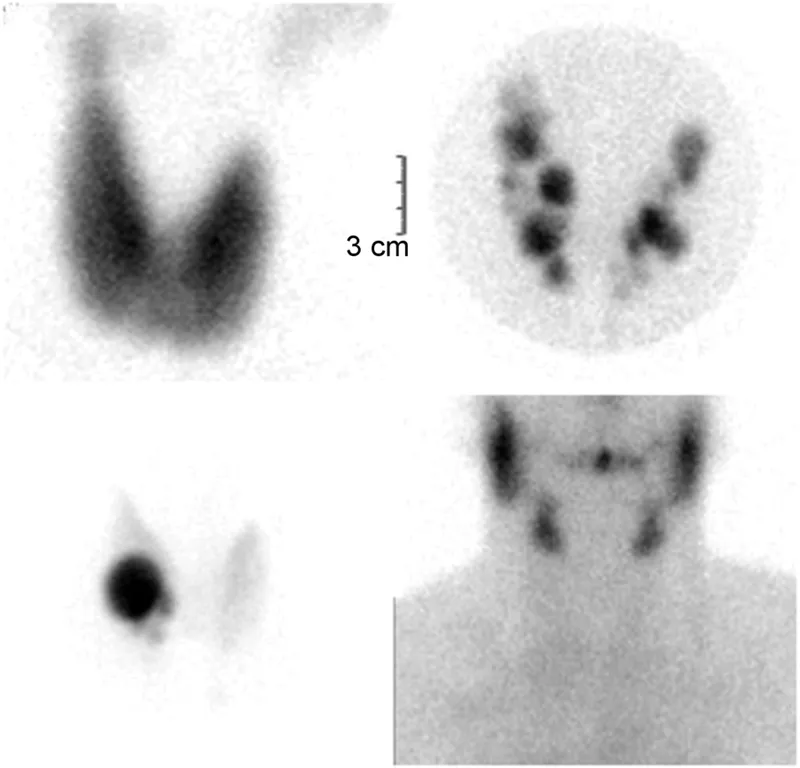
- Management:
- Symptomatic: β-blockers (e.g., Propranolol).
- Antithyroid Drugs (ATDs): Methimazole (MMI), Propylthiouracil (PTU).
- Radioactive Iodine ($^{131}I$) Ablation.
- Thyroidectomy.
- Thyroid Storm: Acute, life-threatening. Fever, tachycardia, delirium. Tx: PTU, iodides, steroids, β-blockers.
⭐ Propylthiouracil (PTU) is preferred over Methimazole in the 1st trimester of pregnancy and in thyroid storm due to MMI's teratogenicity and PTU's additional effect of blocking peripheral T4 to T3 conversion (in storm).
Thyroiditis, Nodules & Cancers - Inflamed & Lumpy Gland
- Thyroiditis:
- Subacute (De Quervain's): Post-viral; painful, tender goitre; ↑ESR. Triphasic course. Rx: NSAIDs/steroids.
- Hashimoto's: Autoimmune (Anti-TPO Ab); painless goitre, commonest hypothyroidism. Risk: Lymphoma.
- Riedel's: IgG4-related; "woody" hard, fixed, painless thyroid. Compressive.
- Thyroid Nodules:
- Eval: TSH. Low → Scintigraphy. Normal/High or Cold Nodule → USG → FNA.
- Suspicious USG: Microcalcifications, hypoechoic, irregular margins, taller-than-wide.
- FNA: Bethesda system guides management.
- Thyroid Cancers:
- Papillary (PTC): ~80%, psammoma bodies, Orphan Annie nuclei. Lymphatic spread. Good prognosis. 📌 Popular.
- Follicular (FTC): ~10-15%, hematogenous spread. Capsular/vascular invasion for malignancy.
- Medullary (MTC): ~5%, from C-cells (↑calcitonin). MEN2A/2B (RET). Amyloid.
- Anaplastic: <5%, elderly, aggressive, poor prognosis.

⭐ Psammoma bodies in Papillary Thyroid Carcinoma are concentrically laminated calcifications, an exam favourite.
High‑Yield Points - ⚡ Biggest Takeaways
- Hashimoto's thyroiditis: Most common cause of hypothyroidism; anti-TPO Ab.
- Graves' disease: Most common cause of hyperthyroidism; TSH-receptor Ab (TRAb).
- Thyroid storm: Life-threatening; treat: PTU/methimazole, β-blockers, iodine, steroids.
- Myxedema coma: Severe hypothyroidism; treat: IV levothyroxine, hydrocortisone.
- Amiodarone: Can cause both hypo- & hyperthyroidism.
- Subacute (de Quervain's) thyroiditis: Painful gland, ↑ESR, triphasic thyroid function.
- Papillary carcinoma: Most common thyroid cancer; Orphan Annie eye nuclei, psammoma bodies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

