Obesity - Sizing Up & Risks
- Definition: Excess body fat posing health risk. BMI ($kg/m^2$):
- WHO: Underweight <18.5; Normal 18.5-24.9; Overweight 25-29.9; Obesity I 30-34.9, II 35-39.9, III ≥40.
- Asian Indian: Overweight 23-24.9; Obesity ≥25.
- BMI Formula: $BMI = \text{weight (kg)} / (\text{height (m)})^2$.
- Etiology: Multifactorial (genetics, lifestyle, endocrine e.g., hypothyroidism, Cushing's).
- Assessment:
- BMI.
- Waist Circumference (WC) (Indian): M >90cm, F >80cm (Central Obesity).
- Waist-to-Hip Ratio (WHR): ↑Risk M >0.90, F >0.85.
⭐ Central obesity (↑ WC) is a better predictor of metabolic risk than BMI alone, especially in Asian populations.
- Major Complications: T2DM, CVD, HTN, Dyslipidemia, OSA, NAFLD, PCOS, Cancers (e.g., endometrial, breast, colon).
Obesity Management - The Battle Plan
- 1. Lifestyle Modification (Cornerstone)
- Diet: Calorie deficit (↓500-750 kcal/day).
- Exercise: ≥150 min/week moderate-intensity aerobic activity.
- Behavioral Therapy: CBT, motivational interviewing.
- 2. Pharmacotherapy
- Indications: BMI ≥30 or ≥27 with comorbidities.
- Orlistat: Lipase inhibitor; MOA: ↓fat absorption; S/E: steatorrhea, flatus with discharge.
- Liraglutide (3mg): GLP-1 agonist; MOA: ↑satiety; S/E: nausea, pancreatitis (rare).
- 3. Bariatric Surgery (Severe Obesity)
- Indications: BMI ≥40 or ≥35 with comorbidities.
- Asian (Indian): BMI >37.5 or >32.5 with comorbidities.
- Types: Sleeve Gastrectomy (LSG - restrictive), Roux-en-Y Gastric Bypass (LRYGB - restrictive & malabsorptive).
- Outcomes: Weight loss, T2DM remission. Complications: Dumping syndrome, nutritional deficiencies.
⭐ Liraglutide for obesity (Saxenda, 3.0 mg) is higher dose than for diabetes (Victoza, up to 1.8 mg).
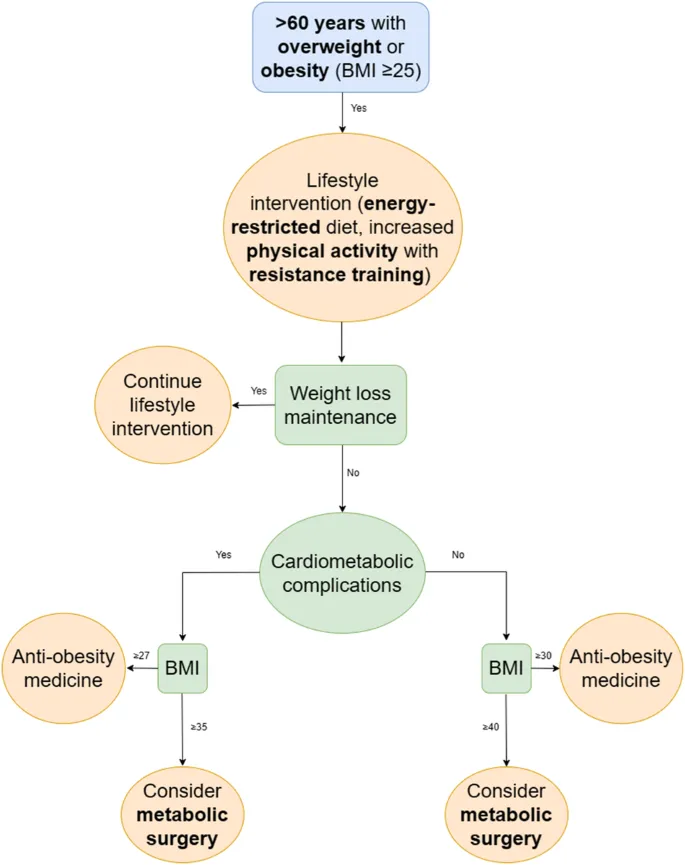
Metabolic Syndrome - The Risky Quintet
Metabolic Syndrome (MetS): a cluster of risk factors significantly ↑ risk of Cardiovascular Disease (CVD) & Type 2 Diabetes (T2DM). Diagnosis: $\ge$3 of 5 criteria (NCEP ATP III/IDF, Indian adaptations):
- Abdominal Obesity (Waist Circumference):
- Men: >90 cm (South Asian/Indian)
- Women: >80 cm (South Asian/Indian)
- Hypertriglyceridemia: TG $\ge$150 mg/dL or on drug therapy.
- Low HDL-C:
- Men: <40 mg/dL or on drug therapy.
- Women: <50 mg/dL or on drug therapy.
- Hypertension: BP $\ge$130/85 mmHg or on antihypertensive drug.
- Impaired Fasting Glucose: FG $\ge$100 mg/dL or on drug therapy for hyperglycemia.
Pathophysiology: Core is Insulin Resistance linked to central obesity. Leads to altered adipokine release (↓adiponectin, ↑leptin resistance) & chronic low-grade inflammation.
⭐ Non-alcoholic fatty liver disease (NAFLD) is often considered the hepatic manifestation of MetS.
MetS Management - Holistic Harmony
Primary goals: ↓ ASCVD risk, prevent T2DM. Cornerstone: Lifestyle modification.
- Lifestyle First
- Weight reduction: 5-10% body weight
- Diet: DASH, Mediterranean
- Physical activity: ≥150 min/wk moderate
- Pharmacotherapy (Individual components)
- Hypertension: ACEi/ARB (often preferred)
- Dyslipidemia: Statins, Fibrates
- Hyperglycemia: Metformin
- High CVD risk: Aspirin
⭐ Weight loss of 5-10% is the primary target of lifestyle modification and significantly improves MetS components.
High‑Yield Points - ⚡ Biggest Takeaways
- Metabolic Syndrome: ≥3 criteria - Abdominal obesity, ↑ Triglycerides (≥150 mg/dL), ↓ HDL-C (<40 men, <50 women), ↑ BP (≥130/85 mmHg), ↑ Fasting Glucose (≥100 mg/dL).
- Indian waist cut-offs for abdominal obesity: Men ≥90 cm, Women ≥80 cm.
- Leptin resistance (satiety hormone) and altered Ghrelin (hunger hormone) contribute to obesity.
- ↓ Adiponectin (insulin-sensitizing adipokine) in obesity is linked to insulin resistance, a core defect.
- Orlistat: A pancreatic lipase inhibitor used for weight loss; common side effect is steatorrhea.
- Bariatric surgery is considered for BMI ≥40 kg/m² or BMI ≥35 kg/m² with significant comorbidities.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

