DM Basics - Sweet Definitions
- WHO Diagnostic Criteria (Any ONE):
- Fasting Plasma Glucose (FPG): $\geq$ 126 mg/dL (7.0 mmol/L)
- 2-hr Plasma Glucose (PG): $\geq$ 200 mg/dL (11.1 mmol/L) during OGTT (75g anhydrous glucose)
- HbA1c: $\geq$ 6.5% (48 mmol/mol)
- Random Plasma Glucose: $\geq$ 200 mg/dL (11.1 mmol/L) + symptoms of hyperglycemia
- Types:
- Type 1 DM (T1DM): Autoimmune $\beta$-cell destruction
- Type 2 DM (T2DM): Insulin resistance & relative deficiency
- Gestational DM (GDM): Diagnosed in 2nd/3rd trimester
- LADA (Latent Autoimmune Diabetes in Adults)
- MODY (Maturity-Onset Diabetes of the Young)
- Epidemiology (India): High prevalence, often undiagnosed. Second largest number of DM patients globally.
⭐ HbA1c reflects average plasma glucose over the preceding 8-12 weeks (lifespan of RBCs).
Sugar Breakdown - Pathophysiology Unpacked
- Type 1 DM (T1DM): Immune-mediated destruction of pancreatic β-cells, leading to absolute insulin deficiency.
- Genetic predisposition (e.g., HLA-DR3, HLA-DR4).
- Environmental triggers (e.g., viruses, toxins) initiate autoimmunity.
- Type 2 DM (T2DM): Characterized by a combination of:
- Insulin Resistance: Decreased peripheral tissue (muscle, fat) and hepatic response to insulin.
- β-cell Dysfunction: Progressive decline in insulin secretion, often with amyloid deposition in islets. Results in relative insulin deficiency.
⭐ Glucotoxicity and lipotoxicity contribute to progressive β-cell dysfunction in T2DM, worsening hyperglycemia.
Spotting Sugar - Signs & Tests
- Symptoms: 📌 Peeing (Polyuria), Parched (Polydipsia), Peckish (Polyphagia); weight loss (T1DM), fatigue, blurred vision, recurrent infections. Acanthosis nigricans (insulin resistance).
- Diagnosis (ADA/WHO criteria - any ONE):
- FPG $\ge$ 126 mg/dL
- 2-hr PG (75g OGTT) $\ge$ 200 mg/dL
- HbA1c $\ge$ 6.5%
- RPG $\ge$ 200 mg/dL + symptoms
- GDM Screening (24-28 wks):
- IADPSG (75g OGTT): F $\ge$ 92, 1hr $\ge$ 180, 2hr $\ge$ 153 mg/dL (any 1 needed).
⭐ DIPSI (India specific): Single 75g OGTT (any time), 2-hr PG $\ge$ 140 mg/dL is diagnostic.
Taming the Sugar - Treatment Toolkit
- Pillars: Lifestyle (diet, exercise) + Pharmacotherapy.
- Initial Rx: Metformin (↓Hepatic glucose output; GI SEs).
- Key OHAs:
- Sulfonylureas (Glimepiride): ↑Insulin secretion. Risk: Hypoglycemia, Wt gain.
- DPP-4 inhibitors (Sitagliptin): ↑Incretin levels. Weight neutral.
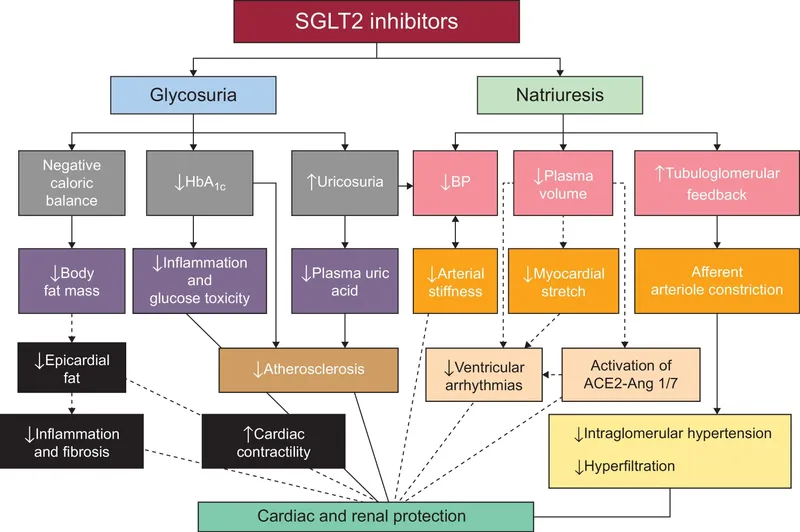
- SGLT2 inhibitors (Dapagliflozin, Empagliflozin): ↑Renal glucose excretion. CV & Renal benefits. 📌 "Flozin for flow out"
- Injectables:
- GLP-1 RAs (Liraglutide, Semaglutide): ↑Incretin, Wt loss. CV benefits.
- Insulin: Types (Rapid, Short, Intermediate, Long). Regimens (Basal, Basal-Bolus).
- Targets: HbA1c generally <7%. Individualize (<6.5% young/new, <8% elderly/comorbid).
⭐ SGLT2 inhibitors (e.g., Empagliflozin, Canagliflozin, Dapagliflozin) reduce MACE and progression of diabetic kidney disease.
Sugar's Sting - Complications Galore
- Acute: Diabetic Ketoacidosis (DKA), Hyperosmolar Hyperglycemic State (HHS) - emergencies.
- Chronic Microvascular:
- Retinopathy: Non-proliferative (NPDR), Proliferative (PDR); major cause of blindness.
- Nephropathy: Microalbuminuria (Urine Albumin-Creatinine Ratio 30-300 mg/g) → End-Stage Renal Disease (ESRD).
- Neuropathy: Peripheral (glove & stocking sensory loss), autonomic (gastroparesis, postural hypotension).
- Chronic Macrovascular: Accelerated atherosclerosis - Coronary Artery Disease (CAD), Cerebrovascular Disease (CVD), Peripheral Vascular Disease (PVD).
- Diabetic Foot: Ulcers, infections, Charcot arthropathy; risk of amputation.

⭐ Microalbuminuria (UACR 30-300 mg/g) is the earliest detectable stage of diabetic nephropathy and a key screening target.
High‑Yield Points - ⚡ Biggest Takeaways
- HbA1c ≥6.5% or FPG ≥126 mg/dL diagnoses Diabetes Mellitus.
- Metformin: first-line oral agent for Type 2 DM; inhibits hepatic gluconeogenesis.
- DKA: hyperglycemia, ketosis, anion gap metabolic acidosis; treat with IV fluids, insulin.
- HHS: severe hyperglycemia, hyperosmolality, dehydration; minimal ketosis.
- Diabetic retinopathy screening: at diagnosis for T2DM; 5 years post-diagnosis for T1DM.
- ACE inhibitors/ARBs: preferred for hypertension in diabetics; renoprotective with microalbuminuria.
- Dawn phenomenon vs. Somogyi effect: check 3 AM blood glucose to differentiate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

