Nutritional Assessment - Sizing Up Situation
- Goal: ICU nutrition ↓morbidity, ↓mortality, ↓LOS.
- Key Tools:
- SGA (Subjective Global Assessment): Subjective.
- NRS-2002 (Nutritional Risk Screening): Score ≥3 = risk.
- NUTRIC Score: ICU-specific. Score 5-9 = high risk, benefit from nutrition.
- Limitations:
- Biomarkers (Albumin, Prealbumin): Unreliable (APR, fluid shifts).
- Anthropometry: Fluid shifts limit use in ICU.
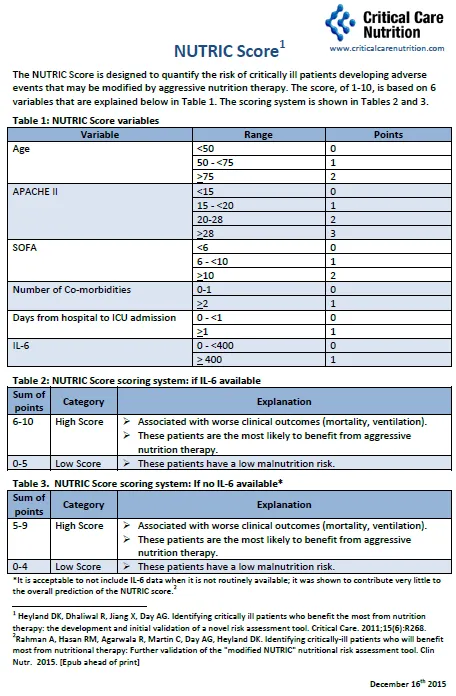
⭐ NUTRIC score components: Age, APACHE II, SOFA, #Comorbidities, Days hosp to ICU, IL-6. Score ≥5 = high risk; consider aggressive nutrition therapy.
Caloric & Protein Needs - Fueling the Fight
- Energy Target: 20-25 kcal/kg/day.
- Use actual body weight (ABW) for non-obese; adjusted BW for obese.
- Gold Standard: Indirect calorimetry (IC).
- Predictive equations (e.g., Harris-Benedict, Penn State) have limitations.
- Protein: 1.2-2.0 g/kg/day (↑ burns, trauma).
⭐ Protein target for most critically ill patients: 1.2-2.0 g/kg/day.
- Carbs: 50-70% non-protein calories; $GIR_{max}$ 4-5 mg/kg/min.
- Fats: 30-50% non-protein calories.
Enteral Nutrition - Gut Instincts First
- Indications: Functional GIT, inadequate oral intake.
- Contraindications: Ileus, obstruction, severe shock, high-output fistula (distal).
- Timing: Early EN (within 24-48 hours).
⭐ Early EN (within 24-48h) preserves gut integrity, ↓bacterial translocation & sepsis.
- Access Routes:
- NG/NJ: Short-term; NG (↑aspiration), NJ (↓aspiration).
- PEG/PEJ: Long-term; PEG (gastric), PEJ (jejunal, ↓aspiration).

- Formulas: Standard polymeric, fiber, high-protein.
- Initiation: Start 10-20 mL/hr, advance to goal.
- Complications:
- GI: Diarrhea, GRV > 500ml (hold EN).
- Mechanical: Tube issues.
- Metabolic: Refeeding syndrome.
Parenteral Nutrition - Vein Victory Plan
- Indications: Non-functional GIT; EN contraindicated; EN failure to meet needs.
- Timing:
- No EN: Start after 7 days (well-nourished), earlier (malnourished).
- Supplemental PN: If EN <60% needs by day 7-10.
- Access:
- Central (TPN): Preferred, high osmolarity.
- Peripheral (PPN): Short-term, osmolarity <900 mOsm/L.
- Components: Dextrose, amino acids, lipid emulsions, electrolytes, vitamins, trace elements.
- Complications: Catheter-related (infection, thrombosis); metabolic (hyperglycemia, refeeding, PNALD); overfeeding.

⭐ Major risk with PN: Catheter-Related Bloodstream Infection (CRBSI).
Special Considerations - Tricky Patient Tactics
- Immunonutrition: Arginine, glutamine, omega-3 FAs; controversial.
- Sepsis: Early EN; avoid overfeeding.
- ARDS: Consider omega-3 FAs/antioxidants (limited evidence).
- Pancreatitis (Severe): Early EN (NJ preferred).
- Obesity: Hypocaloric, high-protein: 11-14 kcal/kg actual weight. Protein: >2.0 g/kg IBW (BMI 30-40), >2.5 g/kg IBW (BMI >40).
⭐ Protein for BMI >40: >2.5 g/kg IBW.
Monitoring & Pitfalls - Watching for Trouble
- Adequacy: Clinical signs, nitrogen balance (limited), indirect calorimetry (measures energy expenditure).
- Complications: Monitor glucose (target 140-180 mg/dL), electrolytes (K, Mg, PO₄), LFTs, triglycerides.
- Refeeding Syndrome (RFS):
- Patho: Insulin surge → intracellular electrolyte shifts. 📌 PIMP: ↓Phosphate, ↓Potassium, ↓Magnesium.
- Risks: Malnutrition, alcoholism. Prevent: Thiamine, slow refeed. Manage: Correct electrolytes.
- ⭐ > Key electrolyte abnormalities in refeeding syndrome are hypophosphatemia, hypokalemia, and hypomagnesemia.

-
%%{init: {'flowchart': {'htmlLabels': true}}}%% flowchart TD
Start["📋 At-Risk Patient?
• Identify risk level• Prepare nutrition"]
Nutrition{"💊 Start Nutrition
• Initiate feeding• Assess tolerance"}
LowRisk["✅ Low Risk
• Start 75% target• Ongoing monitoring"]
HighRisk["⚠️ High Risk
• Give Thiamine• 5-10 kcal/kg/day"]
Monitor["🔬 Lab Monitor
• PO4, K, Mg levels• Close observation"]
Correct["🚨 Electrolytes ⬇️
• Correct labs• Slow/Pause feed"]
Gradual["👁️ Monitoring
• Gradual ⬆️ Feed• Goal achievement"]
Start --> Nutrition Nutrition -->|No| LowRisk Nutrition -->|Yes| HighRisk HighRisk --> Monitor Monitor -->|Stable| Gradual Monitor -->|⬇️ Electrolytes| Correct Correct --> Gradual
style Start fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style Nutrition fill:#FEF8EC, stroke:#FBECCA, stroke-width:1.5px, rx:12, ry:12, color:#854D0E style LowRisk fill:#F6F5F5, stroke:#E7E6E6, stroke-width:1.5px, rx:12, ry:12, color:#525252 style HighRisk fill:#FDF4F3, stroke:#FCE6E4, stroke-width:1.5px, rx:12, ry:12, color:#B91C1C style Monitor fill:#FFF7ED, stroke:#FFEED5, stroke-width:1.5px, rx:12, ry:12, color:#C2410C style Correct fill:#FDF4F3, stroke:#FCE6E4, stroke-width:1.5px, rx:12, ry:12, color:#B91C1C style Gradual fill:#EEFAFF, stroke:#DAF3FF, stroke-width:1.5px, rx:12, ry:12, color:#0369A1
* **Overfeeding:** Hyperglycemia, hepatic steatosis, ↑$CO_2$ production (difficult weaning).
## High‑Yield Points - ⚡ Biggest Takeaways
> * **Early Enteral Nutrition (EEN)** within **24-48 hours** is preferred in critical illness.
> * Use **Parenteral Nutrition (PN)** if EN contraindicated or inadequate by day **7**.
> * Caloric goal: **25-30 kcal/kg/day**; Protein: **1.2-2.0 g/kg/day**.
> * Watch for **Refeeding Syndrome**: monitor **K, PO4, Mg**; give **thiamine** pre-feeding.
> * **Immunonutrition** (arginine, glutamine) has specific roles, not for routine sepsis.
> * High **Gastric Residual Volumes (GRVs)** alone don't mandate stopping EN.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

