Enhanced Recovery Protocols - Speedy Recovery Blueprint
- Aim: Optimize patient recovery, ↓ hospital stay, ↓ complications, ↓ costs.
- Multimodal, evidence-based strategy: Integrates care across preoperative, intraoperative, and postoperative phases.
- Key Pillars:
- Patient education & engagement.
- Preoperative nutrition (e.g., carbohydrate loading), avoiding prolonged fasting (clear fluids up to 2 hrs pre-op).
- Standardized anesthetic & analgesic plans (opioid-sparing, multimodal analgesia).
- Early mobilization & oral intake post-surgery (within hours).
- Avoidance of routine nasogastric tubes & drains.
- Outcomes: ↑ Patient satisfaction, ↓ morbidity, faster functional recovery.
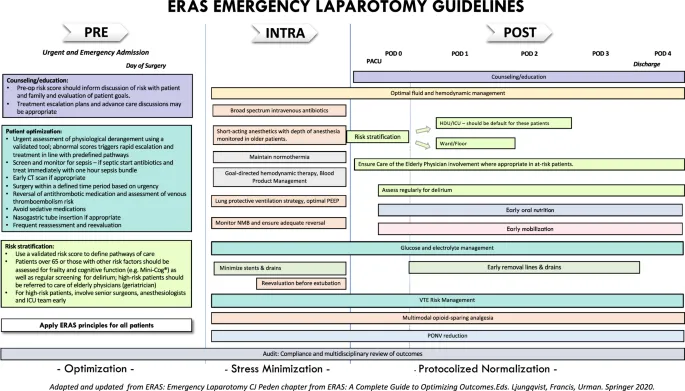
⭐ ERAS significantly reduces postoperative ileus and can shorten hospital length of stay by 30-50% or 2-3 days compared to traditional care pathways.
Enhanced Recovery Protocols - Pre-Op Power-Up
- Patient Education: Explain ERAS, active role, expectations.
- Nutritional Screening & Support:
- Correct malnutrition (e.g., Albumin <3 g/dL).
- Carbohydrate loading: 2-3 hrs pre-op (clear complex carbs, e.g., maltodextrin).
- Consider immunonutrition for high-risk (e.g., major GI surgery).
- Risk Reduction & Optimization:
- Smoking cessation: Aim ≥4 wks pre-op.
- Alcohol cessation: Advise ≥4 wks pre-op.
- Anemia correction: Target Hb >10 g/dL.
- Pre-habilitation: Structured exercise program to improve functional capacity.
- Fasting & Bowel Prep:
- No solids <6 hrs, clear fluids <2 hrs pre-op.
- Avoid routine mechanical bowel preparation unless specifically indicated.
⭐ Pre-operative carbohydrate loading (e.g., 50g in 400ml water 2-3 hrs prior) reduces post-operative insulin resistance, minimizes protein loss, and improves patient comfort and well-being.
Enhanced Recovery Protocols - Smooth Sailing Ops
- Intraoperative Care - Minimize Stress:
- Anesthesia: Short-acting agents, regional/neuraxial blocks (epidural) to ↓ opioid use.
- Fluid Management: Goal-Directed Fluid Therapy (GDFT); avoid overload, maintain euvolemia.
- Normothermia: Maintain core temperature > 36°C (active warming).
- PONV Prophylaxis: Multimodal (e.g., dexamethasone, ondansetron).
- Surgical Technique: Minimally invasive surgery (MIS) preferred.
- Selective use of NG tubes & drains.
- Postoperative Care - Accelerate Recovery:
- Analgesia: Multimodal, opioid-sparing (paracetamol, NSAIDs, local blocks).
- Early Mobilization: Ambulate within 24h post-op.
- Early Oral Nutrition: Liquids within hours, early diet advancement.
- Glycemic Control: Target blood glucose < 180 mg/dL.
- Early Catheter Removal: Urinary catheters, drains removed promptly (e.g., POD1).
- VTE Prophylaxis: Mechanical and/or pharmacological.
⭐ Early oral nutrition (within 24 hours post-op) is a cornerstone of ERAS, reducing ileus and improving nitrogen balance.
Enhanced Recovery Protocols - Road to Discharge
- Goal: Expedite safe recovery, reduce hospital stay, minimize readmissions.
- Key Post-Op Interventions (POD 1+):
- Mobilization: Early, frequent ambulation (e.g., >2-3 times/day).
- Nutrition: Resume oral diet promptly (target within 24h).
- Analgesia: Multimodal regimen, prioritize non-opioids.
- Catheters/Drains: Discontinue once indications cease (e.g., Foley by POD1).
- VTE Prophylaxis: Continue based on risk assessment.
- Discharge Readiness Checklist:
- Pain: Adequately controlled with oral analgesics.
- Diet: Tolerating sufficient oral intake.
- Mobility: Independent or at pre-op baseline.
- No unresolved issues (e.g., fever, uncontrolled nausea, wound concerns).
⭐ Early ambulation and oral feeding are pivotal in reducing postoperative ileus and overall length of hospital stay.
High‑Yield Points - ⚡ Biggest Takeaways
- ERAS protocols are multimodal, evidence-based pathways to accelerate recovery after surgery.
- Key preoperative elements: Patient education, nutritional optimization, carbohydrate loading, no prolonged fasting.
- Intraoperative strategies: Regional anesthesia, minimally invasive surgery (MIS), normothermia, euvolemia.
- Postoperative care: Early oral nutrition, early mobilization, multimodal opioid-sparing analgesia, timely catheter removal.
- Primary goals: Reduce surgical stress response, minimize organ dysfunction, improve outcomes.
- Benefits: Shorter hospital stay (LOS), fewer postoperative complications, enhanced patient satisfaction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

