Headache Basics & Classification - Head Start
- Primary Headaches: Headache is the illness; no underlying cause. 📌 P: Problem is the headache.
- Types: Migraine, Tension-Type (TTH), Trigeminal Autonomic Cephalalgias (e.g., Cluster).
- Secondary Headaches: Symptom of another condition (e.g., infection, tumor, bleed). 📌 S: Symptom of something else.
- Requires identifying and treating the underlying pathology.
- IHS Classification: International Classification of Headache Disorders (ICHD by IHS) is the standard.
⭐ Most common type of primary headache is Tension-Type Headache.
Primary Headaches: Migraine & TTH - Brain Pain Duo
-
Migraine:
- Diagnosis: ≥5 attacks (no aura), ≥2 (aura). Duration 4-72h.
- 📌 POUND: Pulsatile, Often unilateral, Usually 4-72h, Nausea/vomiting, Disabling.
- Aura: Reversible CNS sx (visual common); develop ≥5 min, last 5-60 min.
- Chronic: ≥15 headache days/month (>3 months); migraine on ≥8 days.
⭐ Status migrainosus: debilitating migraine >72 hours.
-
Tension-Type Headache (TTH):
- Most common. Bilateral, pressing/tightening (non-pulsatile), mild-moderate. Not aggravated by activity.
- Duration 30 min-7 days. No N/V; photophobia OR phonophobia (not both).
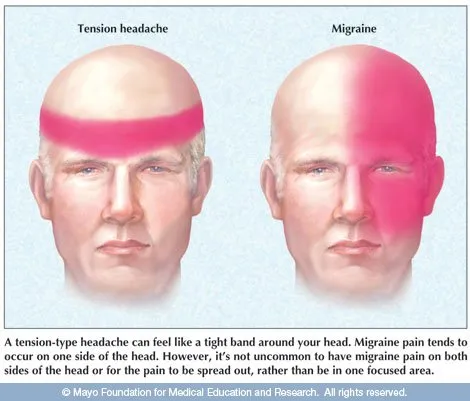
Migraine vs. TTH Comparison
| Feature | Migraine | Tension-Type Headache (TTH) |
|---|---|---|
| Location | Unilateral | Bilateral |
| Character | Pulsatile | Pressing/Tightening |
| Duration | 4-72h | 30 min-7 days |
| Associated Sx | N/V, Photo & Phonophobia | Photo OR Phono (not both), No N/V |
| Severity | Mod-Severe, Disabling | Mild-Mod, Not disabling |
Primary Headaches: TACs - TACs Attack
- Cluster Headache: Severe unilateral orbital/temporal pain, 15-180 min, up to 8/day.
- 📌 CLUSTER: Conjunctival injection, Lacrimation, Unilateral, Sweating/autonomic sx, Temporal/orbital, Eight/day, Restlessness.

- 📌 CLUSTER: Conjunctival injection, Lacrimation, Unilateral, Sweating/autonomic sx, Temporal/orbital, Eight/day, Restlessness.
- Paroxysmal Hemicrania: Shorter (2-30 min), frequent attacks.
- ⭐ > Absolute indomethacin response (e.g., 25-75 mg tid) is diagnostic.
- SUNCT/SUNA: Shortest (1-600 sec), very frequent, stabbing pain. SUNCT: +conjunctival injection & tearing.
| Feature | Cluster Headache | Paroxysmal Hemicrania | SUNCT/SUNA |
|---|---|---|---|
| Duration | 15-180 min | 2-30 min | 1-600 sec |
| Freq./day | ≤8 | >5 (often many) | ≥1 (up to 200) |
| Autonomic Sx | Yes (prominent) | Yes (prominent) | Yes (defining) |
| Indomethacin Resp. | No | Absolute | No |
Secondary Headaches & Red Flags - Danger Signals
- 📌 SNOOPPP Red Flags: Systemic symptoms/Secondary risk factors, Neurologic symptoms/signs, Onset sudden/abrupt, Older age of onset >50 years, Pattern change or recent onset, Positional, Precipitated by cough/sneeze/exercise, Papilledema.
- Key Secondary Causes:
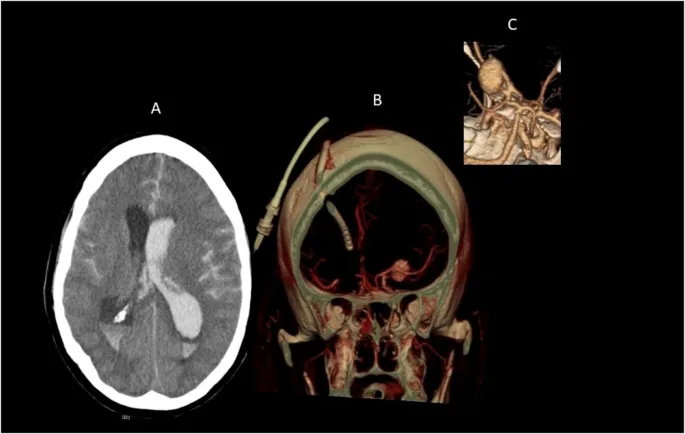
- Subarachnoid Hemorrhage (SAH): Thunderclap headache, neck stiffness.
- Meningitis/Encephalitis: Fever, nuchal rigidity, altered mental status.
- Giant Cell Arteritis (GCA): Age >50 years, new headache, jaw claudication, visual sx, tender temporal artery, ↑ESR/CRP.
- Brain Tumor: Progressive, focal deficits, morning headache, papilledema.
- Idiopathic Intracranial Hypertension (IIH): Obese young women, papilledema, visual changes, pulsatile tinnitus.
⭐ The 'worst headache of life' or 'thunderclap headache' is a classic presentation of subarachnoid hemorrhage and requires urgent neuroimaging.
Headache Management Approaches - Relief Roadmap
- Principles: Diagnosis, education, lifestyle modification.
- Migraine Management:
- Acute: NSAIDs, triptans (e.g., **sumatriptan 50-100mg PO**), CGRP antagonists (-gepants).
- Prophylactic: β-blockers (propranolol), TCAs (amitriptyline), anticonvulsants (topiramate, valproate), CGRP mAbs (-mabs), Botox (chronic).
- Cluster: Acute (100% O₂ 12-15L/min 15-20min, sumatriptan 6mg SC). Prophylactic: verapamil (1st line), corticosteroids, lithium.
- Tension-Type: Acute (analgesics, NSAIDs). Prophylactic: amitriptyline.
⭐ Verapamil is the first-line prophylactic agent for cluster headache and requires ECG monitoring.
High‑Yield Points - ⚡ Biggest Takeaways
- Tension-type headache (TTH): Most common; bilateral, non-pulsating. NSAIDs first-line.
- Migraine: Unilateral, pulsating, aura. Acute: Triptans, NSAIDs. Prophylaxis: Propranolol.
- Cluster headache: Severe, unilateral, periorbital pain, autonomic features. Acute: 100% Oxygen, Sumatriptan SC.
- Red flags (SNOOP4): Identify secondary headaches; e.g., sudden onset ("thunderclap"), neurological deficits.
- Subarachnoid hemorrhage (SAH): "Worst headache of life"; CT scan is key.
- Medication Overuse Headache (MOH): From frequent acute drug use (>10-15 days/month).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

