Dyspnea: Definition & Pathophysiology - Breathless Beginnings
- Dyspnea: Subjective awareness of uncomfortable breathing.
- Types:
- Acute: <2-4 weeks; Chronic: >2-4 weeks.
- Orthopnea: Dyspnea supine.
- PND (Paroxysmal Nocturnal Dyspnea): Sudden nocturnal dyspnea.
- Trepopnea: Dyspnea in one lateral decubitus position.
- Pathophysiology:
- Respiratory center stimulation.
- Inputs from:
- Chemoreceptors: Central (medullary; $CO_2$, $H^+$); Peripheral (carotid/aortic bodies; $O_2$, $CO_2$, $H^+$).
- Mechanoreceptors: Lung (stretch, J-receptors); Chest wall (proprioceptors).
- Ventilation/Perfusion (V/Q) mismatch.
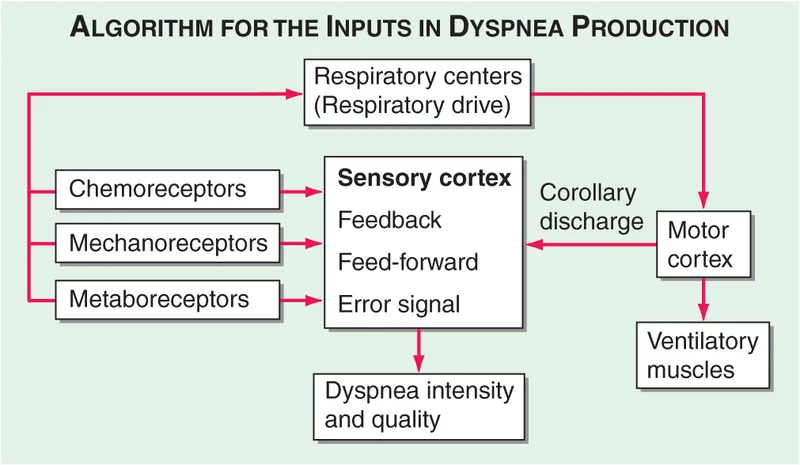
⭐ Orthopnea is a hallmark of left ventricular failure but can also occur in severe diaphragmatic weakness.
Dyspnea: Etiology - The Usual Suspects
Major Causes:
- Pulmonary: COPD, Asthma, Pneumonia, PE, Pneumothorax, ILD, Pleural effusion
- Cardiac: CHF, ACS, Arrhythmias, Pericardial (tamponade, constrictive), Valvular
- Neuromuscular: Myasthenia, GBS, Diaphragm paralysis
- Hematologic: Severe Anemia
- Metabolic: Acidosis (DKA - Kussmaul)
- Psychogenic: Anxiety, Panic
📌 Acute Dyspnea (4P+A+C):
- Pneumothorax
- Pulmonary Embolism (PE)
- Pneumonia
- Pulmonary Edema (APO)
- Asthma
- Cardiac (ACS/Arrhythmia)
Differentiating Acute Causes:
| Feature | PE | Pneumothorax | APO | Asthma |
|---|---|---|---|---|
| Onset | Sudden | Sudden | Sudden/Rapid | Gradual/Sudden |
| Chest Pain | Pleuritic | Pleuritic, ipsi. | +/- Pressure | Tightness |
| Breath Sounds | Normal/Crackles/Rub | ↓/Absent ipsi. | Bilat. crackles/wheezes | Bilat. wheezes |
| CXR | Normal/Hampton's/Westermark | Pleural line | Bilat. infiltrates/Kerley B | Hyperinflation/Normal |
| Key Assoc. | DVT risk | Tall, thin; trauma | Heart disease Hx | Asthma Hx, triggers |
Dyspnea: Clinical Evaluation - Unmasking Dyspnea
- History: Onset (sudden/gradual), duration, mMRC severity, character, aggravating/relieving factors. Associated: chest pain, cough, fever, wheeze, hemoptysis. PMH, meds, smoking.
- Physical Exam:
- General: Distress, cyanosis, accessory muscle use.
- Vitals: RR, SpO2 (< 90% critical), HR, BP.
- Respiratory: Palpation, percussion, auscultation (wheezes, crackles, rubs, ↓ breath sounds).
- Cardiac: JVP, S3, murmurs, edema.
- Signs of DVT.
- Initial Investigations: Pulse oximetry, CXR, ECG, ABG ($P(A-a)O_2$).
- Further: CBC, D-dimer, BNP/NT-proBNP, Troponins, Spirometry/PFTs, Echo, CT chest (CTPA, HRCT).
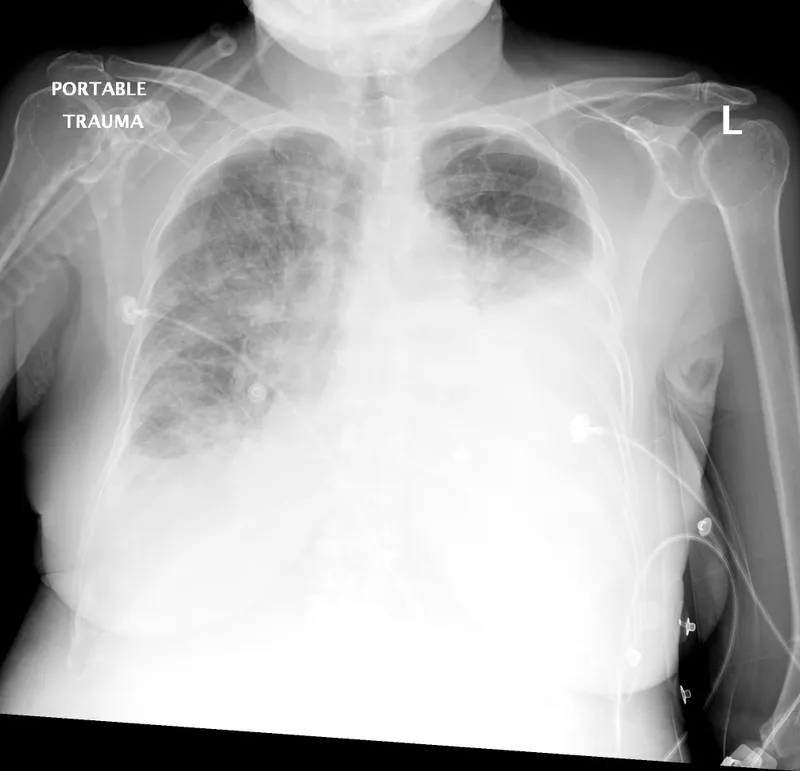
⭐ Pulsus paradoxus >10 mmHg is a key finding in cardiac tamponade and severe asthma/COPD.
Dyspnea: Management Principles - Breathing Easier
- General Approach: ABCDE (Airway, Breathing, Circulation, Disability, Exposure). Secure airway, administer Oxygen.
- Target SpO2: 94-98% (general); 88-92% in COPD with hypercapnic failure.
-
Non-Invasive Ventilation (NIV - CPAP/BiPAP):
- Indications: COPD exacerbation (respiratory acidosis), cardiogenic pulmonary edema.
- Contraindications: Facial trauma, undrained pneumothorax, hemodynamic instability, GCS < 8.
-
Life-Threatening Causes: Quick Management
- Acute Pulmonary Edema: Diuretics, Nitrates, NIV. 📌 LMNOP (Lasix, Morphine, Nitrates, Oxygen, Position).
- Acute Severe Asthma/COPD: Bronchodilators (SABA, SAMA), Corticosteroids, O2. Consider MgSO4 for asthma.
- Tension Pneumothorax: Immediate needle decompression → chest tube.
- Massive Pulmonary Embolism: Anticoagulation; Thrombolysis/embolectomy if unstable.
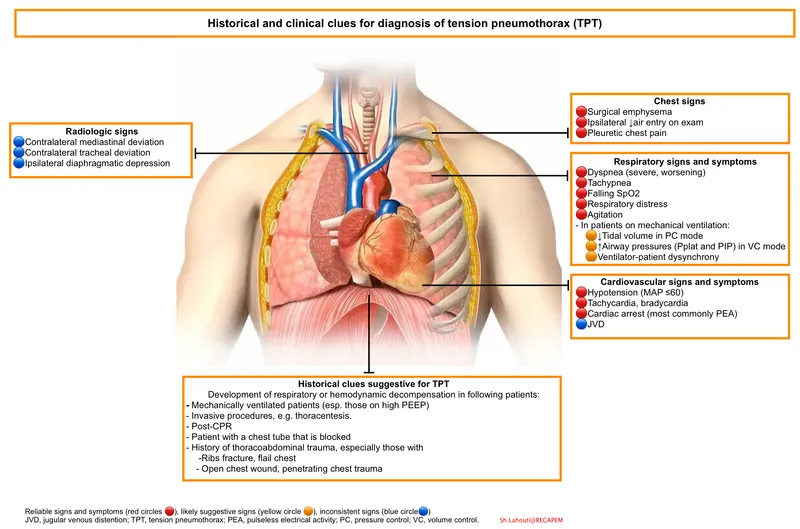
⭐ In tension pneumothorax, needle thoracostomy should be performed in the 2nd intercostal space, mid-clavicular line, or the 5th intercostal space, anterior axillary line, over the superior border of the rib below to avoid neurovascular bundle.
High‑Yield Points - ⚡ Biggest Takeaways
- Key acute dyspnea causes: PE, pneumothorax, ACS, asthma/COPD exacerbation.
- Key chronic dyspnea causes: COPD, heart failure, ILD, anemia.
- Orthopnea & PND: hallmarks of left ventricular failure (LVF).
- Platypnea-orthodeoxia: linked to hepatopulmonary syndrome, R-L shunts.
- Kussmaul's respiration: signifies severe metabolic acidosis (e.g., DKA).
- Pulsus paradoxus >10 mmHg: points to cardiac tamponade, severe asthma/COPD.
- Acute respiratory distress immediate management: prioritize ABC (Airway, Breathing, Circulation) and administer supplemental oxygen.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

