Fever - Burning Questions
- Definition: Core body temp > 38.3°C (101°F) or sustained > 38°C (100.4°F) over 1 hour.
- Mechanism: Pyrogens (exogenous/endogenous) → Hypothalamic PGE2 ↑ → ↑ thermoregulatory set point.
- Key Patterns (Clinical clues, not diagnostic):
- Continuous: Typhoid, lobar pneumonia. Fluctuates < 1°C/24h.
- Remittent: Infective endocarditis. Fluctuates > 1°C/24h, always above normal.
- Intermittent: Malaria, pyemia. Fever spikes with return to normal.
- Pel-Ebstein: Hodgkin's lymphoma. Cyclical fever for days/weeks.
- Fever of Unknown Origin (FUO): Temp > 38.3°C for ≥ 3 weeks; no diagnosis after 1 week inpatient workup (classic definition).
- Common causes: Infections (e.g., TB, endocarditis), Malignancies (e.g., lymphoma), Autoimmune (e.g., Still's disease).
- Other types: Nosocomial, Neutropenic (ANC < 500/µL), HIV-associated.
- Initial Workup Approach:
- Red Flags: Immunocompromise, new cardiac murmur, petechiae/purpura, altered sensorium, severe headache.

⭐ Pel-Ebstein fever, a cyclical pattern of fever lasting for days to weeks followed by afebrile periods, is classically associated with Hodgkin's lymphoma.
Pain - Agony Aunt
Pain: Unpleasant sensory & emotional experience associated with actual or potential tissue damage. Often considered the fifth vital sign.
-
Assessment: 📌 SOCRATES
- Site: Where? Localized/diffuse?
- Onset: When? Sudden/gradual?
- Character: What type? (e.g., Sharp, dull, burning, throbbing)
- Radiation: Does it spread?
- Associated symptoms: Nausea, vomiting, fever, neurological deficits?
- Timing/Duration: Constant/intermittent? Pattern?
- Exacerbating/Relieving factors: What makes it better/worse?
- Severity: Pain scales (e.g., Visual Analog Scale 0-10, Numeric Rating Scale 0-10, Wong-Baker FACES for children).
-
Types of Pain:
- Nociceptive: Due to tissue injury.
- Somatic: Musculoskeletal (well-localized, aching, throbbing).
- Visceral: Internal organs (poorly localized, deep, cramping, squeezing).
- Neuropathic: Due to nerve lesion/dysfunction (burning, tingling, shooting, electric shock-like).
- Nociplastic: Altered nociception without clear evidence of actual or threatened tissue damage (e.g., fibromyalgia).
- Nociceptive: Due to tissue injury.
-
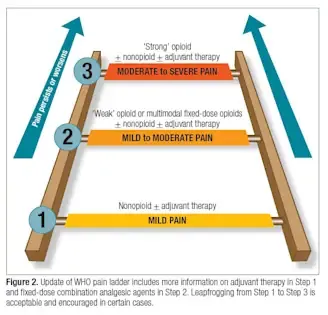
Management Principles (WHO Analgesic Ladder):
- Step 1: Non-opioid (e.g., Paracetamol, NSAIDs) ± Adjuvant.
- Step 2: Weak opioid (e.g., Codeine, Tramadol) ± Non-opioid ± Adjuvant.
- Step 3: Strong opioid (e.g., Morphine, Fentanyl) ± Non-opioid ± Adjuvant.
- Address underlying cause; consider non-pharmacological therapies (physio, TENS, CBT).
⭐ Neuropathic pain often responds poorly to traditional analgesics but may improve with anticonvulsants (e.g., gabapentin, pregabalin) or tricyclic antidepressants (e.g., amitriptyline).
Fatigue - Energy Crisis
- Definition: Subjective lack of physical and/or mental energy, distinct from weakness or somnolence.
- Duration Criteria:
- Acute: < 1 month
- Chronic: > 6 months (significant impact on daily life)
- Etiology: Broad differential.
- Medical: Anemia, hypothyroidism, Diabetes Mellitus, infections (e.g., TB, HIV, EBV), malignancy, autoimmune (SLE, RA), cardiac/pulmonary/renal insufficiency.
- Psychiatric: Depression, anxiety disorders.
- Lifestyle/Medications: Poor sleep, deconditioning, stress, alcohol/substance abuse, beta-blockers, antihistamines.
- Chronic Fatigue Syndrome (CFS/ME).
- Red Flags: Unexplained weight loss (>5% body weight), persistent fever (>38.3°C), generalized lymphadenopathy (>2cm), focal neurological signs, unexplained bleeding, drenching night sweats.
- Initial Workup: Detailed history (including psychosocial), physical exam, CBC with differential, ESR/CRP, TSH, random blood sugar, electrolytes, LFTs, RFTs, urinalysis. Consider HIV, CXR based on risk factors/symptoms.
⭐ A hallmark of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) is post-exertional malaise (PEM), where symptoms worsen significantly after minimal physical or mental exertion, typically lasting >24 hours and being disproportionate to the activity.
High‑Yield Points - ⚡ Biggest Takeaways
- Fever of Unknown Origin (FUO): Temperature >38.3°C for >3 weeks, undiagnosed after 1 week of inpatient evaluation.
- Pain Assessment: Systematically use OPQRST (Onset, Palliative/Provocative, Quality, Radiation, Severity, Timing) or SOCRATES for comprehensive characterization.
- Fatigue Red Flags: Unexplained weight loss, lymphadenopathy, and focal neurological deficits warrant urgent investigation.
- Drug Fever: Often presents with rash and eosinophilia; common culprits include beta-lactams and sulfonamides.
- Key Fever Patterns: Continuous (typhoid), intermittent (malaria), Pel-Ebstein (Hodgkin's lymphoma) are diagnostically crucial.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

