Environmental and Occupational Hazards

On this page
🏭 The Toxic Workplace: Environmental and Occupational Hazard Fundamentals
Every day, millions of workers encounter invisible threats-chemical vapors, heavy metals, particulates, and radiation-that can silently damage lungs, nerves, kidneys, and blood. This lesson equips you to identify occupational and environmental hazards, trace how toxins enter and harm the body, assess exposure levels like a detective, and implement prevention strategies that save lives. You'll connect toxicological mechanisms to clinical presentations across multiple organ systems, building the diagnostic and protective skills essential for any physician who encounters patients shaped by their work and environment.
📌 Remember: SHAPE - Source identification, Hazard assessment, Acute vs chronic effects, Prevention strategies, Exposure limits. Every occupational health evaluation follows this systematic approach with >95% diagnostic accuracy when properly applied.
The foundation of occupational health rests on understanding dose-response relationships, exposure pathways, and temporal patterns. While Threshold Limit Values (TLVs) developed by ACGIH are widely referenced as 8-hour time-weighted averages, India follows Permissible Exposure Limits (PELs) defined by DGFASLI under the Factories Act, 1948 and associated state rules. Short-Term Exposure Limits (STELs) define 15-minute maximum exposures that should never be exceeded.
| Exposure Type | Time Frame | Health Effect | Latency Period | Reversibility |
|---|---|---|---|---|
| Acute Chemical | Minutes-Hours | Immediate toxicity | <24 hours | Often reversible |
| Chronic Inhalation | Months-Years | Pneumoconiosis | 10-30 years | Usually irreversible |
| Carcinogenic | Years-Decades | Malignancy | 15-40 years | Irreversible |
| Ergonomic | Days-Months | Musculoskeletal | Weeks-months | Variable |
| Biological | Hours-Days | Infection/allergy | Hours-weeks | Usually reversible |
- Engineering controls: 85% effectiveness in reducing exposures
- Administrative controls: 60% effectiveness through policy
- Rotation schedules limiting exposure to <50% of PEL
- Training programs reducing incidents by 40%
- Secondary Prevention (Early detection)
- Biological monitoring with quarterly assessments per Factories Act requirements
- Medical surveillance detecting 70% of early disease
- Mandatory reporting of occupational diseases under BNS Section 106
- Forensic examination protocols for occupational fatalities
- Tertiary Prevention (Disease management)
- Disability prevention in 80% of cases with early intervention
- Workplace modifications enabling 90% return-to-work rates
⭐ Clinical Pearl: The "healthy worker effect" creates a 20-30% underestimation of occupational disease rates in India's large informal workforce, where workers leave hazardous jobs due to illness without formal documentation, further skewing epidemiological data.
💡 Master This: Occupational disease causation requires establishing temporal relationship (exposure precedes disease), dose-response (higher exposures cause more severe effects), and biological plausibility (known mechanism of action). Bradford Hill criteria provide scientific framework, though Indian courts under BSA require expert testimony correlating clinical findings with occupational history for legal causation in workmen's compensation cases.
Understanding exposure assessment principles enables precise risk stratification and targeted interventions that prevent both acute poisoning and chronic occupational diseases, with forensic medicine experts playing crucial roles in investigating occupational deaths and establishing medico-legal causation under India's updated legal framework.
🏭 The Toxic Workplace: Environmental and Occupational Hazard Fundamentals
⚗️ Chemical Exposure Pathways: The Toxic Highway System
📌 Remember: ADME - Absorption, Distribution, Metabolism, Excretion. Every chemical follows this sequence, with Phase I (oxidation) and Phase II (conjugation) metabolism determining both activation and detoxification pathways.
Dermal absorption varies dramatically by anatomical site: scrotal skin absorbs 42x faster than forearm, forehead absorbs 6x faster, and palm absorbs 0.1x compared to forearm baseline. Molecular weight <500 Da and lipophilicity (log P 1-3) optimize skin penetration.
- Respiratory Absorption Factors
- Minute ventilation: 6-8 L/min at rest, >50 L/min during heavy work
- Alveolar surface area: 70 m² available for gas exchange
- Soluble gases: >90% absorption in upper airways
- Insoluble gases: >80% reach alveoli for systemic absorption
- Distribution Patterns
- Lipophilic compounds: adipose tissue concentration 10-100x plasma
- Hydrophilic compounds: extracellular fluid distribution
- Volume of distribution: 0.6 L/kg (total body water) for hydrophilic
- Volume of distribution: >10 L/kg for highly lipophilic compounds
| Chemical Class | Primary Route | Absorption Rate | Half-Life | Target Organs |
|---|---|---|---|---|
| Volatile Organics | Inhalation | 90% in 5 min | 2-24 hours | CNS, Liver |
| Heavy Metals | Ingestion/Inhalation | 10-50% absorbed | Days-years | Kidney, Brain |
| Pesticides | Dermal/Inhalation | 60-95% absorbed | Hours-days | Nervous System |
| Solvents | Inhalation/Dermal | 80-100% absorbed | 1-48 hours | CNS, Liver |
| Particulates | Inhalation | Size-dependent | Months-years | Lungs |
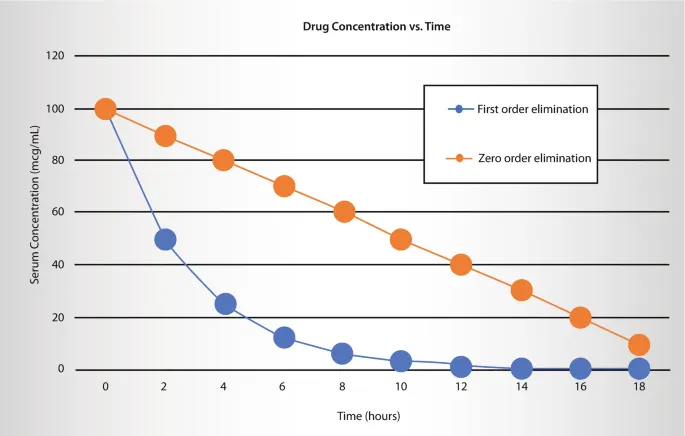
💡 Master This: First-order kinetics (constant percentage eliminated per unit time) applies to >95% of occupational exposures at typical workplace concentrations. Zero-order kinetics (constant amount eliminated) occurs only at very high exposures that saturate metabolic pathways.
Chemical exposure assessment requires understanding these fundamental pathways to predict both immediate health risks and long-term consequences of workplace exposures.
⚗️ Chemical Exposure Pathways: The Toxic Highway System
🎯 Exposure Assessment Mastery: The Detective's Toolkit
- Exposure Measurement Hierarchy
- Direct reading instruments: Real-time data with ±5% accuracy
- Personal dosimeters: Integrated 8-hour time-weighted averages
- Passive samplers: No power required, ±10% accuracy
- Active samplers: Pump-driven, ±2% accuracy for most compounds
- Biological monitoring: Internal dose assessment
- Blood levels: Acute exposure indicator (<24 hours)
- Urine metabolites: Integrated exposure over 2-7 days
- Exhaled breath: Real-time volatile compound assessment
📌 Remember: CHESS - Characterize exposure, Hazard identification, Exposure assessment, Source evaluation, Sampling strategy. This systematic approach ensures >90% accuracy in exposure determination.
Temporal exposure patterns critically influence health outcomes. Peak exposures often cause acute effects even when 8-hour TWA remains below limits. Ceiling limits represent concentrations that should never be exceeded, while STEL values define 15-minute maximum exposures.

| Sampling Method | Duration | Accuracy | Cost | Applications |
|---|---|---|---|---|
| Real-time monitors | Continuous | ±5-10% | High | Peak detection |
| Personal pumps | 8-hour TWA | ±2-5% | Moderate | Compliance |
| Passive badges | 8-hour TWA | ±10-15% | Low | Screening |
| Biological samples | Variable | ±5-20% | Moderate | Internal dose |
| Wipe samples | Point-in-time | ±10% | Low | Surface contamination |
- Field blanks: 10% of total samples to detect contamination
- Duplicate samples: 10% of samples for precision assessment
- Coefficient of variation should be <15% for acceptable precision
- Spike recovery should be 85-115% for analytical accuracy
- Chain of custody: Documented sample handling preventing legal challenges
⭐ Clinical Pearl: Skin notation chemicals (like aniline, phenol, organophosphates) can contribute >50% of total body burden through dermal absorption, making air sampling alone inadequate for exposure assessment.
💡 Master This: Occupational Exposure Limits (OELs) protect 95% of healthy workers but may not protect hypersusceptible individuals (pregnant women, those with genetic polymorphisms, pre-existing disease). Clinical judgment must consider individual risk factors beyond population-based limits.
Exposure assessment provides the quantitative foundation for all occupational health decisions, from immediate hazard control to long-term epidemiological studies.
🎯 Exposure Assessment Mastery: The Detective's Toolkit
🔬 Toxicological Mechanisms: The Cellular Battlefield
Cytochrome P450 enzymes both detoxify and activate chemicals through Phase I metabolism. CYP2E1 activation can significantly increase with chronic alcohol use, dramatically enhancing susceptibility to carbon tetrachloride, acetaminophen, and vinyl chloride toxicity. Genetic polymorphisms in CYP enzymes create significant differences in individual susceptibility.
- Cellular Injury Mechanisms
- Membrane disruption: Lipid peroxidation altering membrane fluidity
- Protein denaturation: Sulfhydryl group oxidation disrupting enzyme function
- Critical protein targets: A wide range of essential enzymes affected
- Threshold effect: Significant enzyme inhibition required for clinical symptoms
- DNA damage: Adduct formation leading to mutagenesis
- Base modifications: Numerous types of DNA adducts identified
- Repair capacity: DNA repair mechanisms are highly efficient but vary by damage type
📌 Remember: REDOX - Reactive species generation, Enzyme inhibition, DNA damage, Organelle dysfunction, Xenobiotic metabolism. These interconnected pathways determine cellular fate following toxic exposure (simplified representation of complex processes).
Target organ selectivity depends on tissue-specific metabolism, blood flow patterns, and cellular defense mechanisms. The liver receives approximately 25% of cardiac output and contains highest concentrations of metabolizing enzymes, making it highly susceptible to chemical-induced injury.
| Mechanism | Examples | Time Course | Reversibility | Biomarkers |
|---|---|---|---|---|
| Enzyme inhibition | Organophosphates | Minutes-hours | Reversible | Cholinesterase |
| Membrane damage | Solvents | Hours-days | Variable | LDH, ALT |
| DNA alkylation | Alkylating agents | Days-weeks | Irreversible | DNA adducts |
| Oxidative stress | Metals, quinones | Hours-days | Variable | MDA, 8-OHdG |
| Protein binding | Heavy metals | Days-months | Irreversible | Metallothionein |
Biomarkers of exposure detect internal dose, while biomarkers of effect identify early biological changes preceding clinical disease. Urinary metabolites provide integrated exposure assessment with variable detection windows, while DNA adducts indicate genotoxic exposure with persistence varying by adduct type and repair efficiency.
💡 Master This: Threshold effects characterize most toxic responses, with No Observed Adverse Effect Levels (NOAELs) providing the basis for occupational exposure limits. Non-threshold effects (primarily carcinogenesis) assume any exposure carries some risk, requiring ALARA (As Low As Reasonably Achievable) principles.
Understanding toxicological mechanisms enables prediction of individual susceptibility, selection of appropriate biomarkers, and development of targeted therapeutic interventions for occupational exposures.
🔬 Toxicological Mechanisms: The Cellular Battlefield
🛡️ Prevention and Control Strategies: The Hierarchy of Protection
- Hierarchy of Controls (Most to Least Effective)
- Elimination: Complete hazard removal through process changes
- Substitution: Significant risk reduction using safer alternatives
- Green chemistry: Safer solvents with potential for substantial toxicity reduction
- Material substitution: Non-toxic alternatives available for many hazardous chemicals
- Engineering Controls: Substantial exposure reduction potential
- Local exhaust ventilation: High capture efficiency at source when properly designed
- Isolation/enclosure: Effective containment of hazardous processes
- Administrative Controls: Moderate risk reduction potential
- Job rotation: Limiting individual exposure below regulatory limits
- Training programs: Potential for significant reduction in incident rates
- Personal Protective Equipment: Variable protection depending on proper use
- Respirator protection factors: Range from 10-10,000x depending on type
- Actual workplace protection: Often significantly lower due to improper use
📌 Remember: The standard hierarchy follows Elimination, Substitution, Engineering Controls, Administrative Controls, Personal Protective Equipment. This hierarchy ensures maximum protection with minimum reliance on worker behavior.
Ventilation design requires understanding capture velocities specific to contaminant generation patterns. Welding fumes and grinding operations require specific capture velocities that vary based on equipment and materials - consult ACGIH Industrial Ventilation Manual for specific requirements. Dilution ventilation provides general air changes but requires substantially more air volume than local exhaust.
| Control Method | Effectiveness | Cost | Maintenance | Worker Dependence |
|---|---|---|---|---|
| Elimination | Highest | Variable | None | None |
| Substitution | High | Moderate | Low | None |
| Engineering | High | High | Moderate | Low |
| Administrative | Moderate | Low | High | High |
| PPE | Variable | Low | Moderate | Very High |
Medical surveillance programs aim to detect early health effects when properly designed. Biological monitoring provides objective exposure assessment, while health screening identifies susceptible individuals and early disease. Periodic examinations should occur at intervals based on latency periods and exposure levels.
💡 Master This: Multiple control strategies used simultaneously can provide enhanced protection. Combining engineering controls with administrative controls and PPE yields improved overall protection when systems function properly and independently.
Prevention and control strategies must be tailored to specific hazards, workplace conditions, and worker populations to achieve maximum effectiveness in protecting occupational health.
🛡️ Prevention and Control Strategies: The Hierarchy of Protection
🔗 Multi-System Integration: The Occupational Health Network
Gene-environment interactions create dramatic individual variability in occupational disease susceptibility. GSTM1-null genotype affects 50% of populations and increases lung cancer risk by 2-3 fold in workers exposed to polycyclic aromatic hydrocarbons. Slow acetylator phenotype (NAT2 polymorphism) increases bladder cancer risk by 3-5 fold in workers exposed to aromatic amines.
- Multi-System Exposure Effects
- Neurotoxic-hepatotoxic combinations: Alcohol + solvents increase liver damage 5-10 fold
- Respiratory-cardiovascular interactions: Particulate matter increases MI risk by 2-3% per 10 μg/m³ increase
- Inflammatory mediators: IL-6, TNF-α elevated 2-5 fold after exposure
- Autonomic dysfunction: Heart rate variability decreased 20-40%
- Endocrine disruption: >200 workplace chemicals affect hormone systems
- Reproductive effects: Fertility reduction of 20-50% in exposed workers
- Thyroid disruption: TSH changes in 30-60% of exposed populations
📌 Remember: TEAMS - Toxicokinetic interactions, Endocrine disruption, Allergic sensitization, Multiple organ effects, Synergistic toxicity. These interconnected mechanisms require comprehensive health assessment approaches under BNS Section 125 for negligent acts causing harm.
Emerging occupational hazards include nanoparticles, endocrine disruptors, and shift work effects. Engineered nanoparticles penetrate cellular barriers and accumulate in brain, liver, and lungs with unknown long-term effects. Night shift work increases breast cancer risk by 40-50% and cardiovascular disease by 20-30%.
| Exposure Combination | Interaction Type | Risk Multiplier | Mechanism | Prevention Strategy |
|---|---|---|---|---|
| Alcohol + Solvents | Synergistic | 5-10x | CYP2E1 induction | Alcohol screening |
| Asbestos + Smoking | Multiplicative | 50-90x | DNA damage | Smoking cessation |
| Heat + Dehydration | Additive | 2-3x | Thermoregulation | Hydration programs |
| Noise + Ototoxins | Synergistic | 3-5x | Cochlear damage | Hearing conservation |
| Stress + Chemicals | Potentiating | 2-4x | Immune suppression | Stress management |
Precision occupational health represents the future direction, using genetic testing, biomarker panels, and wearable sensors to provide individualized risk assessment and personalized protection strategies. Pharmacogenomic testing can identify workers at 10-100 fold higher risk for specific chemical exposures, with findings admissible under BSA Section 45.
💡 Master This: Systems thinking in occupational health requires understanding that workplace exposures create cascading effects through multiple biological pathways. Single-chemical risk assessments may underestimate real-world risks by 2-10 fold when multiple exposures and individual susceptibility factors are considered. Legal documentation must follow BNSS Section 183 for medical examination procedures.
Multi-system integration approaches enable more accurate risk assessment, better protection strategies, and personalized interventions that account for the complex reality of modern workplace exposures under the BNS 2023 framework for occupational safety violations.
🔗 Multi-System Integration: The Occupational Health Network
🎯 Clinical Mastery Arsenal: Your Occupational Health Command Center
📌 Essential Recognition Patterns: TOXICS - Temporal relationship (exposure precedes symptoms), Occupational clustering (multiple workers affected), Xenobiotic detection (biological monitoring), Improvement away from work, Consistent clinical syndrome, Specific exposure history. These patterns identify >95% of occupational diseases when systematically applied.
Critical Threshold Arsenal for immediate clinical decision-making:
- Emergency Exposure Limits
- IDLH (Immediately Dangerous to Life/Health): An atmospheric concentration of any toxic, corrosive or asphyxiant substance that poses an immediate threat to life or would cause irreversible or delayed adverse health effects or would interfere with an individual's ability to escape from a dangerous atmosphere (29 CFR 1910.120)
- Carboxyhemoglobin >25%: Immediate hyperbaric oxygen consideration
- >40%: Life-threatening, requires 100% oxygen and ICU monitoring
- >60%: Usually fatal without immediate intervention
- Methemoglobin >20%: Methylene blue 1-2 mg/kg IV indicated
- Cholinesterase <50% of baseline: Moderate organophosphate poisoning
- <25%: Severe poisoning requiring atropine and pralidoxime
⭐ Master This: Biological Exposure Indices (BEIs) are guidance values for assessing biological monitoring results representing internal dose corresponding to TLV exposure. The ACGIH states that BEI interpretation requires professional experience in occupational health. Overexposure is indicated when a BEI is exceeded, but the degree of overexposure and clinical implications are complex and substance-specific, requiring expert interpretation rather than fixed multipliers.
| Clinical Scenario | Key Biomarker | Critical Threshold | Immediate Action | Follow-up Interval |
|---|---|---|---|---|
| Lead exposure | Blood lead | >40 μg/dL | Remove from exposure | Weekly monitoring |
| Mercury exposure | Urine mercury | >50 μg/L | Chelation consideration | Monthly monitoring |
| Solvent exposure | Breath analysis | >50% of TLV | Ventilation check | Daily monitoring |
| Pesticide exposure | Cholinesterase | <70% baseline | Medical evaluation | Weekly monitoring |
| Asbestos exposure | Chest X-ray | Pleural changes | Pulmonary referral | Annual monitoring |
Rapid Assessment Protocol for suspected occupational disease:
- Exposure history: Detailed job tasks and chemical inventory
- Temporal patterns: Symptom timing relative to work schedule
- Coworker effects: Similar symptoms in workplace colleagues
- Biological monitoring: Appropriate biomarkers for suspected exposures
- Environmental assessment: Workplace measurements and control evaluation
This clinical mastery framework enables rapid recognition, accurate diagnosis, and effective management of occupational health emergencies while establishing systematic approaches for long-term worker protection and health surveillance.
🎯 Clinical Mastery Arsenal: Your Occupational Health Command Center
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























