Disability Evaluation - Defining the Damage
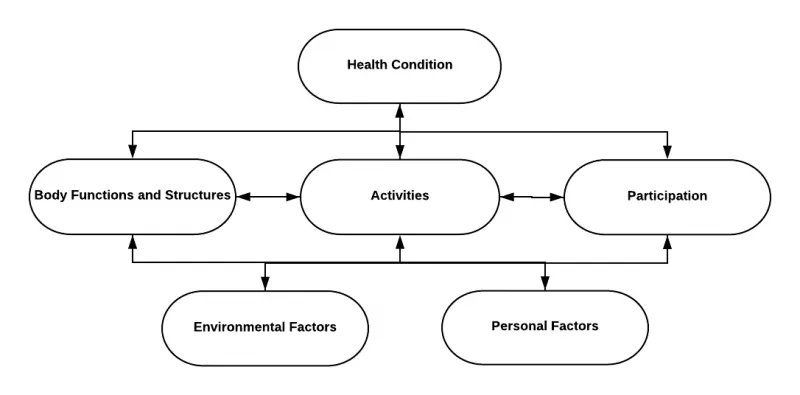
- Core Concepts (WHO ICF Model):
- Impairment: Problem in body function/structure (e.g., loss of limb).
- Activity Limitation: Difficulty executing a task/action (e.g., unable to walk).
- Participation Restriction: Problem experiencing involvement in life situations (e.g., unable to work).
- Disability: Umbrella term for impairments, activity limitations, & participation restrictions.
- Participation Restriction: Disadvantage from impairment/disability, limiting fulfillment of a normal role (depends on age, sex, social, cultural factors).
- Types: Physical, sensory, intellectual, mental illness, chronic neurological conditions, blood disorders.
⭐ The Rights of Persons with Disabilities (RPWD) Act, 2016, expanded the list of recognized disabilities from 7 to 21. Key provisions include non-discrimination, accessibility, and inclusive education.
Assessment Protocols - Gauging the Gap
- Goal: Objectively quantify functional impairment and its impact.
- Core Principles: Impartiality, thoroughness, meticulous documentation.
- Systematic Approach:
- Detailed History: Injury/illness mechanism, onset, progression, treatment, occupational impact, pre-existing conditions.
- Comprehensive Clinical Exam: General, systemic, and disability-specific findings.
- Corroborative Investigations: X-rays, MRI, nerve conduction studies, audiometry, perimetry.
- Standardized Objective Tools: WHO DAS 2.0, AMA Guides to the Evaluation of Permanent Impairment (Sixth Edition, 2022), specific disability scales/questionnaires.
- Medical Board Adjudication: Multidisciplinary team (relevant specialists) for final assessment and certification. Essential for medico-legal validity under BSA evidence standards.
⭐ A Medical Board, typically comprising specialists relevant to the disability (e.g., orthopedician, ophthalmologist, psychiatrist), is essential for comprehensive and objective disability assessment in medico-legal cases under BSA evidence standards.
Quantification Methods - Counting the Cost
- Disability percentage is quantified using standardized guidelines, primarily from Gazette of India notifications under the RPWD Act, 2016.
- Assessment relies on specific schedules and criteria detailed for various conditions (e.g., locomotor, sensory, intellectual disabilities).
- Key Principle: To assign a numerical value (%) to the extent of impairment.
- Combining Multiple Disabilities:
- Calculated using a specific formula: $C = A + B(100-A)/100$, where A is the higher disability percentage and B is the lower.
- Thresholds:
- A disability of <40% is considered mild.
- A disability of ≥40% is termed a 'benchmark disability', qualifying for benefits.
- Purpose: Ensures objectivity, uniformity, and legal validity for accessing support, aids, appliances, and reservations.
⭐ A person with 40% or more of a specified disability is generally considered a 'person with benchmark disability' under the Rights of Persons with Disabilities (RPWD) Act, 2016, making them eligible for certain benefits and reservations.
Certification & Caveats - Sealing the Deal (Carefully!)
-
Disability Certificate:
- Issued by a designated medical authority/board as per Rights of Persons with Disabilities (RPWD) Act, 2016 guidelines.
- Specifies: type of disability, extent (percentage), duration (permanent/temporary), and need for assistive devices.
- Temporary certificates require reassessment after a specified period.
-
Unique Disability ID (UDID) Card:
- A single, unique identity card for Persons with Disabilities (PwDs).
- Aims to streamline access to government benefits and schemes.
-
Addressing Malingering/Exaggeration:
- Requires careful clinical examination, observation, and objective testing.
- Corroborate with collateral history if possible.
-
Medico-legal & Ethical Responsibilities:
- Utmost honesty, objectivity, and impartiality in assessment.
- Maintain strict confidentiality.
- Thorough documentation is crucial.
⭐ Issuing a false or improper disability certificate can lead to disciplinary action by the State Medical Council and legal penalties under the RPWD Act or Indian Penal Code (IPC).
-
Important Caveats:
- Clearly document all findings and reasoning.
- Explicitly state any limitations encountered during the assessment process.
- Ensure the certificate is unambiguous and complete before issuance and sealing.
High‑Yield Points - ⚡ Biggest Takeaways
- Disability involves restriction or lack of ability to perform an activity in a manner considered normal.
- Governed by the Rights of Persons with Disabilities (RPWD) Act, 2016.
- Permanent disability is non-progressive; temporary disability requires re-assessment.
- Disability percentage is crucial; ≥40% often required for benefits.
- Medical Boards are constituted for assessment and certification.
- UDID (Unique Disability ID) card is a key document.
- Common types include locomotor, visual, hearing, and intellectual disabilities.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

