Other Surgical Procedures for OSA - Beyond UPPP Basics
- Indicated for CPAP/UPPP failure or intolerance.
- Aim: Enlarge airway at specific obstruction sites; often multi-level surgery.
- Selection Criteria:
- Site(s) of collapse (tongue base, lateral pharyngeal walls, epiglottis).
- OSA severity (AHI >15).
- BMI <40 kg/m², comorbidities.
- Procedures:
- Genioglossus Advancement (GA).
- Hyoid Suspension.
- Maxillomandibular Advancement (MMA).
- Tracheostomy (severe/refractory OSA).
⭐ Maxillomandibular Advancement (MMA) has the highest success rate (~86%) for OSA among non-tracheostomy procedures, especially for AHI >30.
Other Surgical Procedures for OSA - Tongue Taming Tactics
Addresses retrolingual/hypopharyngeal collapse. Often adjunctive to UPPP. 📌 Mnemonic: Geniuses Hang Radios Subtly (GA, HS, RFBT, Submucosal Lingual Resection)
- Genioglossus Advancement (GA)
- Indication: Retrolingual collapse.
- Technique: Mandibular osteotomy, advances genial tubercle & genioglossus.
- Outcome: AHI ↓ ~50-60%.
- Complications: Chin numbness, dental injury.
- Hyoid Suspension (HS)
- Indication: Hypopharyngeal collapse.
- Technique: Hyoid bone repositioned anteriorly/superiorly.
- Outcome: AHI ↓ ~40-50%.
- Complications: Dysphagia, neck pain.
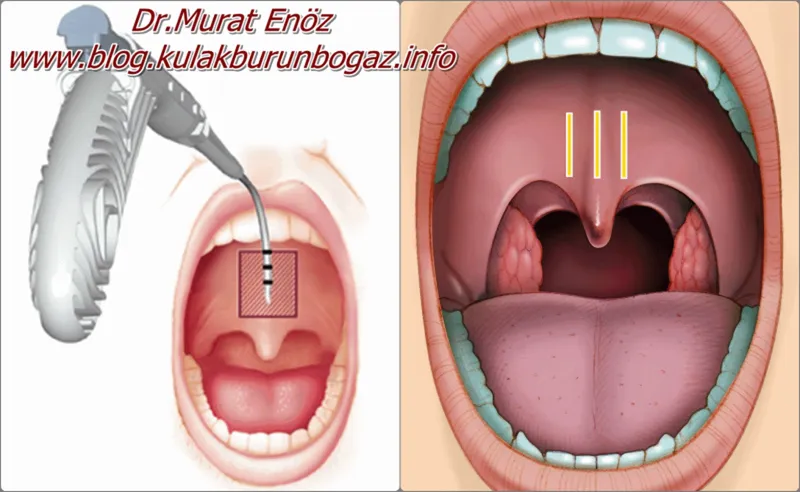
- Radiofrequency Ablation of Tongue Base (RFBT)
- Indication: Tongue base hypertrophy, mild-moderate OSA.
- Technique: Thermal injury reduces tongue volume; multiple sessions.
- Outcome: AHI ↓ ~30-60%.
- Complications: Pain, swelling, temporary dysarthria.
- Submucosal Lingual Resection / Lingualplasty
- Indication: Significant tongue base hypertrophy.
- Technique: Surgical debulking of tongue base tissue.
- Outcome: AHI ↓ ~60-70%.
- Complications: Bleeding, edema, taste disturbance.
⭐ Hyoid suspension is particularly effective for patients with isolated hypopharyngeal collapse or retroepiglottic obstruction.
Other Surgical Procedures for OSA - Jaw & Zap Fixes
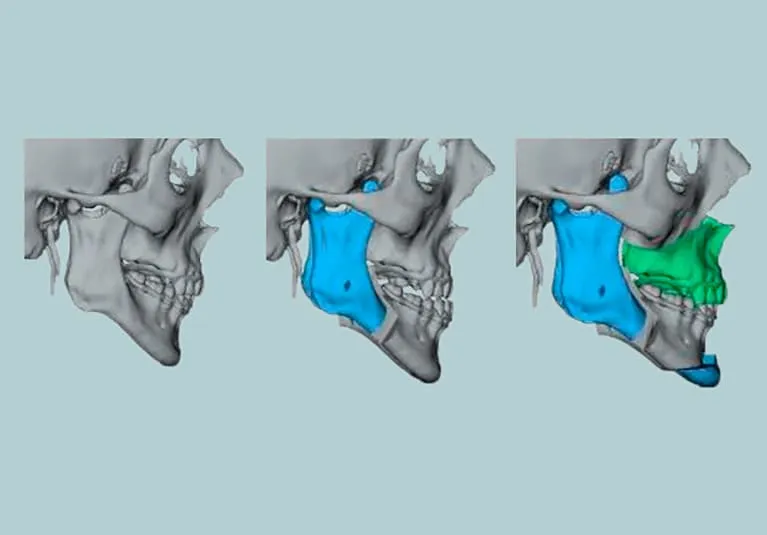
- Maxillomandibular Advancement (MMA)
- Surgical advancement of maxilla & mandible, typically >10mm.
- Indications: Severe OSA, retrognathia, craniofacial abnormalities.
- Outcomes: High success rates (often >80%), significant facial profile alteration.
- Complications: Nerve injury (V3 sensory changes), malocclusion, TMJ pain.
- Hypoglossal Nerve Stimulation (HGNS)
- Mechanism: Implanted neurostimulator activates hypoglossal nerve → tongue protrusion → maintains airway patency during sleep.
- Patient Selection:
- Moderate to severe OSA (AHI 15-100).
- BMI < 35 kg/m² (some devices up to 40 kg/m²).
- DISE: No complete concentric collapse (CCC) at velum/palate.
- Components: Implantable pulse generator (IPG), sensing lead (respiratory effort), stimulation lead (hypoglossal nerve).
- Outcomes: ↓AHI, ↓daytime sleepiness, ↑Quality of Life.
⭐ HGNS is contraindicated in patients with complete concentric collapse (CCC) of the soft palate identified during Drug-Induced Sleep Endoscopy (DISE).
Other Surgical Procedures for OSA - Varied Airway Aids
- Palatal Implants (e.g., Pillar Procedure)
- Minimally invasive option for mild OSA and primary snoring.
- Mechanism: Polyester implants stiffen the soft palate, reducing vibration and collapse.
- Nasal Surgery (Septoplasty, Turbinate Reduction)
- Primarily adjunctive; rarely a standalone OSA treatment.
- Aims to improve nasal airflow, potentially enhancing CPAP tolerance.
- Often part of multi-level surgical approaches.
- Tracheostomy
- Most definitive treatment; bypasses entire upper airway obstruction.
- Highest efficacy (near 100% resolution of OSA).
- Indications: Life-threatening OSA unresponsive to other treatments, severe craniofacial anomalies, or failure of all other therapies.
⭐ Tracheostomy offers the highest success rate for OSA but is considered a last resort due to its impact on quality of life and associated morbidity, bypassing all levels of upper airway obstruction directly.
High‑Yield Points - ⚡ Biggest Takeaways
- Maxillomandibular advancement (MMA): Most effective surgical treatment for OSA, especially with retrognathia.
- Genioglossus advancement (GA): Targets tongue base collapse by anteriorly moving the genioglossus muscle.
- Hyoid suspension: Expands hypopharyngeal airway by elevating and advancing the hyoid bone.
- Radiofrequency tongue base reduction (RFTBR): Reduces tongue volume, for mild-moderate OSA or multilevel approaches.
- Tracheostomy: Definitive treatment for severe, refractory OSA, bypassing upper airway obstruction.
- Bariatric surgery: Crucial for obese OSA patients, significantly improving AHI and overall health.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

