CPAP: Mechanism & Principles - Airway's Best Friend
- CPAP: Delivers Continuous Positive Airway Pressure.
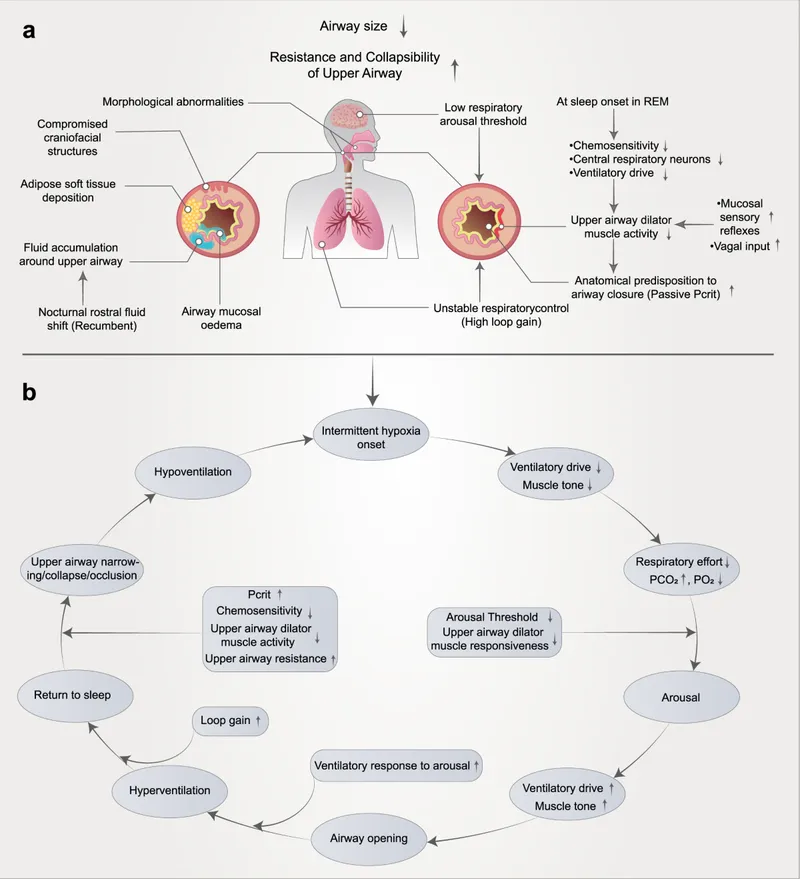
- Core Mechanism: Acts as a "pneumatic splint".
- Maintains constant air pressure to keep the upper airway patent during sleep.
- Prevents collapse of pharyngeal tissues, especially during inspiration.
- Ensures unobstructed airflow from nasopharynx to larynx.
- Therapeutic Principles:
- Positive pressure counteracts forces causing airway narrowing.
- Reduces/eliminates apneas, hypopneas, and snoring.
- Improves nocturnal oxygen saturation (SpO₂).
- Aids in restoring normal sleep stages.
⭐ CPAP is considered the gold standard therapy for patients with moderate to severe Obstructive Sleep Apnea (OSA).
CPAP: Indications & Contraindications - Green Lights & Red Flags
Indications (Green Lights):
- Obstructive Sleep Apnea (OSAHS):
- AHI > 15/hr (Moderate-Severe).
- AHI 5-15/hr (Mild) + significant EDS, HTN, CVD, or cognitive/mood issues.
- Obesity Hypoventilation Syndrome (OHS).
- Central Sleep Apnea (CSA): e.g., Cheyne-Stokes in HF (if primary Tx fails).
- Symptomatic Upper Airway Resistance Syndrome (UARS).
Contraindications (Red Flags):
- Absolute:
- Severe bullous lung disease (risk: pneumothorax).
- Untreated pneumothorax/pneumomediastinum.
- Recent facial/skull/esophageal/gastric surgery or trauma.
- Active CSF leak / recent neurosurgery.
- Relative (Caution):
- Severe hypotension.
- Severe uncorrected nasal obstruction.
- Marked claustrophobia/anxiety.
⭐ CPAP is gold standard for moderate-severe OSAHS (AHI >15), reducing AHI, EDS, and improving QoL & CV outcomes.
CPAP: Equipment & Titration - Gear, Gauges, & Goals
- CPAP Device (Generator): Delivers constant, positive airflow.
- Types: Fixed-pressure (standard CPAP), Auto-titrating (APAP).
- Humidifier: Adds moisture to air; prevents nasopharyngeal dryness. Heated vs. Passover.
- Tubing & Mask Interface: Critical for effective seal & patient comfort.
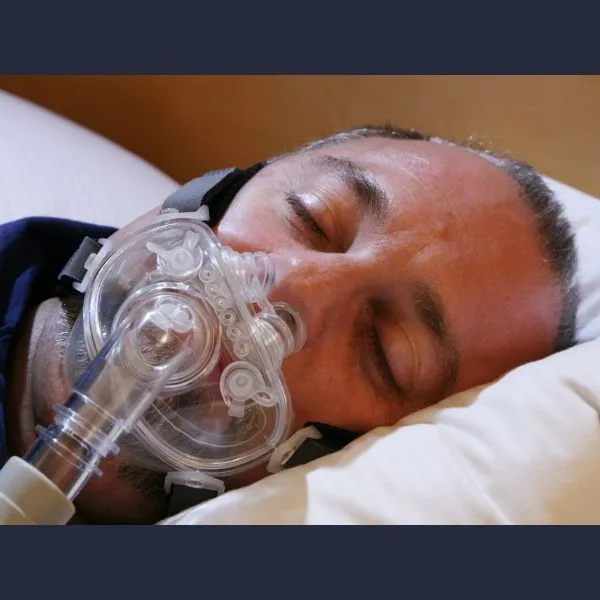
- Nasal Pillows: Minimal contact; good for claustrophobia, allows glasses. Cons: potential nasal irritation, mouth leaks.
- Nasal Mask: Covers nose; good seal. Cons: forehead pressure, mouth leaks if edentulous or mouth breather.
- Oronasal (Full Face) Mask: Covers nose & mouth; for mouth breathers or nasal obstruction. Cons: larger, aspiration risk, claustrophobia.
- Titration: Process to determine optimal pressure.
- Goal: Eliminate apneas, hypopneas, snoring, O2 desaturations. Target AHI < 5/hr.
- Methods: In-lab Polysomnography (PSG) - gold standard. APAP device for home titration (often uses 90th or 95th percentile pressure).
- Pressure Range: Typically 4-20 cm H2O.
⭐ APAP devices can be used for initial titration, especially if PSG is unavailable or delayed, and for long-term management to adapt to changing patient needs (e.g., weight fluctuations).
CPAP: Benefits & Challenges - Perks, Problems, Persistence
- Perks (Benefits):
- Improved sleep quality & daytime alertness; ↓somnolence
- Significant ↓ in Apnea-Hypopnea Index (AHI)
- Better blood pressure control; ↓ long-term cardiovascular morbidity
- Enhanced cognitive function, mood, and quality of life (QoL)
- Problems (Challenges):
- Mask interface: discomfort, air leaks, pressure sores, skin irritation
- Nasal symptoms: dryness, congestion, rhinorrhea, epistaxis
- Pressure-related: aerophagia, bloating, chest discomfort
- Other: claustrophobia, machine/mask noise, partner disturbance
- Persistence (Adherence):
- Critical for efficacy; often a major hurdle
- Key factors: patient education, mask selection/fit, humidification, psychosocial support, regular follow-up
⭐ Good adherence, defined as >4 hours of use per night on >70% of nights, is essential for achieving significant clinical benefits.
High‑Yield Points - ⚡ Biggest Takeaways
- CPAP is gold standard for moderate to severe Obstructive Sleep Apnea (OSA).
- Acts as a pneumatic splint, maintaining upper airway patency during sleep.
- Indicated for AHI >15/hr, or AHI >5/hr with comorbidities/symptoms.
- Pressure titration via polysomnography (PSG) is essential for optimal therapy.
- Patient compliance is the primary challenge and key to successful outcomes.
- Common issues: mask leak, nasal dryness/congestion, skin irritation.
- Significantly improves AHI, daytime somnolence, BP, and quality of life.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

