Cardiovascular Complications - Heart Under Pressure
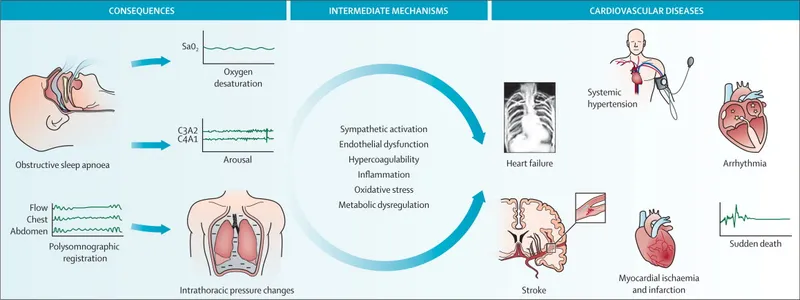
OSA chronically stresses the heart via intermittent hypoxia/hypercapnia, sympathetic overdrive, oxidative stress, and systemic inflammation.
- Hypertension:
- Systemic: OSA is a key secondary cause; often treatment-resistant. Prevalence: 30-70% in OSA.
- Pulmonary: Due to hypoxic vasoconstriction; can lead to Cor Pulmonale (Right Heart Failure).
- Coronary Artery Disease (CAD):
- ↑ Risk of angina, Myocardial Infarction (MI), especially nocturnal.
- Mechanisms: Endothelial dysfunction, pro-inflammatory state, pro-thrombotic state.
- Cardiac Arrhythmias:
- Atrial Fibrillation (AF): Most common; OSA ↑ recurrence post-ablation.
- Bradyarrhythmias: Sinus bradycardia, AV blocks during apneic events.
- Ventricular Tachycardia/Fibrillation: ↑ Risk of Sudden Cardiac Death (SCD), particularly during sleep.
- Heart Failure (HF):
- Both Left Ventricular (LV) systolic & diastolic dysfunction.
- OSA can worsen pre-existing HF and contribute to new-onset HF.
- Cerebrovascular Accidents (CVA):
- ↑ Risk of Stroke and Transient Ischemic Attacks (TIA).
- Associated with AF, hypertension, and accelerated atherosclerosis.
⭐ Patients with OSA have a 2-4 fold increased risk of developing hypertension compared to the general population.
Neurocognitive & Metabolic Issues - Mind & Metabolism
- Neurocognitive Manifestations:
- Persistent daytime hypersomnolence, overwhelming fatigue.
- Cognitive deficits: impaired attention span, poor concentration, memory lapses (short-term), compromised executive functions (planning, decision-making).
- Mood disturbances: increased incidence of depression, anxiety disorders, irritability.
- Characteristic morning headaches.
- Significantly ↑ risk of motor vehicle accidents (MVA) & workplace injuries.
- Overall ↓ quality of life.
- Metabolic Dysregulation:
- Insulin Resistance: Key factor, significantly ↑ risk for Type 2 Diabetes Mellitus.
- Dyslipidemia: Characterized by ↑ triglycerides (TG) & ↓ High-Density Lipoprotein (HDL) cholesterol.
- Metabolic Syndrome: OSA is a strong independent risk factor; clustering of (central obesity, HTN, dyslipidemia, IR).
- Non-Alcoholic Fatty Liver Disease (NAFLD) & Non-Alcoholic Steatohepatitis (NASH): common comorbidities.
- Chronic low-grade systemic inflammation: evidenced by ↑ C-Reactive Protein (CRP), IL-6.
- Hyperuricemia: may contribute to ↑ gout incidence.
⭐ Patients with moderate to severe OSA have a significantly higher likelihood of developing insulin resistance and subsequent Type 2 Diabetes, independent of obesity.
Other Systemic Effects - Beyond Heart & Head
- Gastrointestinal:
- ↑ GERD: Negative intrathoracic pressure promotes nocturnal acid reflux.
- NAFLD (Non-alcoholic Fatty Liver Disease): OSA = independent risk; linked to intermittent hypoxia, systemic inflammation.
- Renal:
- Nocturnal Polyuria: ↑ ANP (hypoxemia, intrathoracic pressure changes), ↓ ADH effect.
- CKD progression: Worsened by chronic hypoxia, sympathetic activation, inflammation.
- Endocrine:
- ↓ Growth Hormone (GH) secretion: Disrupted slow-wave sleep impairs pulsatile release.
- Hematological:
- Secondary Polycythemia: Chronic hypoxemia stimulates erythropoietin.
- Hypercoagulability: Endothelial dysfunction, ↑ platelet activation, ↑ fibrinogen.
- Ophthalmological:
- NAION (Non-arteritic Anterior Ischemic Optic Neuropathy): Strong association.
- Floppy Eyelid Syndrome (FES): Common co-morbidity.
- ↑ Glaucoma risk (Open-angle, Normal Tension).
- Perioperative:
- Increased risk: difficult intubation, airway obstruction.
- Higher post-op risk: respiratory depression, atelectasis, hypoxemia.
- Other:
- Erectile Dysfunction: Common; hypoxia, endothelial dysfunction, autonomic dysregulation.
- Sensorineural Hearing Loss: Potential link via cochlear hypoxia.
⭐ OSA is a key risk factor for Non-arteritic Anterior Ischemic Optic Neuropathy (NAION), causing sudden, painless, monocular vision loss, often on waking.
High-Yield Points - ⚡ Biggest Takeaways
- Systemic hypertension is a primary cardiovascular risk; pulmonary hypertension also occurs.
- Increased risk of cardiac arrhythmias (e.g., AF), myocardial infarction (MI), and stroke.
- Strong association with insulin resistance, increasing Type 2 Diabetes Mellitus risk.
- Neurocognitive impacts: excessive daytime somnolence, impaired concentration, mood changes.
- Higher perioperative complication rates and increased risk of motor vehicle accidents.
- Linked to Non-Alcoholic Fatty Liver Disease (NAFLD) and can worsen GERD.
- Untreated OSA significantly elevates all-cause mortality.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

