Clinical Evaluation of Sleep Apnea - Defining the Disruption
- Core Principle: Identify type & severity for effective management.
- Sleep Apnea Types:
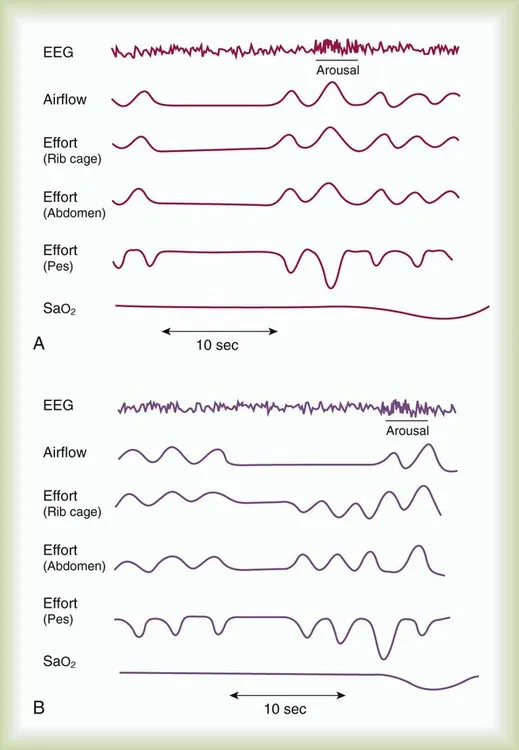
- Obstructive (OSA): Most common; upper airway collapse despite respiratory effort.
- Key feature: Paradoxical chest/abdominal movement during events.
- Central (CSA): Absent respiratory effort due to ↓ central ventilatory drive.
- Often linked to heart failure (e.g., Cheyne-Stokes), stroke, or opioid use.
- Mixed: Begins as central, then transitions to obstructive pattern during an event.
- Obstructive (OSA): Most common; upper airway collapse despite respiratory effort.
- Significance: Differentiating OSA vs. CSA is crucial as treatments vary significantly.
⭐ Apnea-Hypopnea Index (AHI) > 5 events/hour is diagnostic for sleep apnea when accompanied by symptoms.
Clinical Evaluation of Sleep Apnea - Symptom Sleuthing
- Key Symptoms (Patient/Partner Reported):
- Loud, habitual snoring (often with pauses/gasps).
- Witnessed apneas or choking episodes during sleep.
- Excessive Daytime Sleepiness (EDS) despite adequate sleep duration.
- Morning headaches, unrefreshing sleep, fatigue.
- Nocturia, difficulty concentrating, irritability.
- Pertinent Risk Factors (Inquire Actively):
- Obesity (BMI > 30 kg/m²).
- Large neck circumference: > 17 inches (Men), > 16 inches (Women).
- Male gender; Age > 40 years.
- Family history of OSA; craniofacial abnormalities.
- Alcohol/sedative use, especially before bedtime.
- Epworth Sleepiness Scale (ESS):
- Standardized questionnaire to quantify average daytime sleepiness.
- Score > 10 indicates significant/pathological sleepiness, warranting further investigation.
⭐ Witnessed apneas by a bed partner are a highly specific indicator for Obstructive Sleep Apnea.
Clinical Evaluation of Sleep Apnea - Examining the Airway
- General:
- BMI: >30 kg/m² (obesity)
- Neck circumference: >43 cm (men), >40 cm (women)
- Craniofacial Features:
- Retrognathia, micrognathia
- Midface hypoplasia
- High-arched palate
- Macroglossia
- Oropharyngeal Examination:
- Mallampati Score: Class III or IV (↓ posterior airway space)
- 📌 My Little Pony Tongue (Mallampati, Lingual tonsil, Palatine tonsil, Tongue base)
- Tonsillar hypertrophy (Grades 3+, 4+)
- Elongated/thickened uvula
- Friedman Tongue Position (FTP) & Palate Position (FPP)
- FTP I-IV based on tongue relative to palate & uvula.
- Mallampati Score: Class III or IV (↓ posterior airway space)
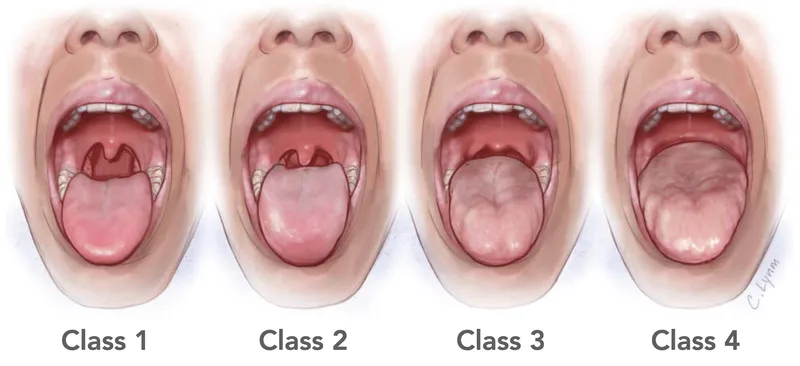
⭐ Friedman Staging System (combining Mallampati, tonsil size, BMI) predicts OSA severity & surgical success. Stage I has highest success rate with UPPP (~80%).
Clinical Evaluation of Sleep Apnea - Sleep Study Deep Dive
- Polysomnography (PSG): Gold Standard
- In-lab, attended (Type 1).
- Monitors: EEG, EOG, EMG, ECG, airflow, respiratory effort, SaO2, snoring.

- Home Sleep Apnea Testing (HSAT)
- Portable, unattended (Types 2, 3, 4).
- Fewer channels (e.g., airflow, effort, SaO2).
- For high pre-test probability OSA, no major comorbidities.
- Key Metrics:
- Apnea-Hypopnea Index (AHI): $AHI = \frac{\text{Apneas + Hypopneas}}{\text{Total Sleep Time (hrs)}}$
- Normal: < 5/hr
- Mild: 5-14/hr
- Moderate: 15-29/hr
- Severe: ≥ 30/hr
- Oxygen Desaturation Index (ODI): Desaturations (≥3-4%) per hour.
- Respiratory Disturbance Index (RDI): AHI + RERAs (Respiratory Effort Related Arousals).
- Apnea-Hypopnea Index (AHI): $AHI = \frac{\text{Apneas + Hypopneas}}{\text{Total Sleep Time (hrs)}}$
⭐ AHI is the primary metric for diagnosing Obstructive Sleep Apnea (OSA) and grading its severity.
Clinical Evaluation of Sleep Apnea - Grading Severity & Risks
- Severity (AHI/hr): Normal <5, Mild 5-15, Moderate 15-30, Severe >30.
- Risks:
- Cardiovascular: Hypertension (HTN), MI, stroke.
- Metabolic: Insulin resistance, Type 2 DM.
- Neurocognitive: Somnolence, ↓concentration, mood changes.
⭐ OSA is an independent risk factor for systemic hypertension.
High‑Yield Points - ⚡ Biggest Takeaways
- Polysomnography (PSG) remains the gold standard diagnostic test for OSA.
- Apnea-Hypopnea Index (AHI) quantifies severity: Mild (5-15 events/hr), Moderate (15-30), Severe (>30).
- Epworth Sleepiness Scale (ESS) is crucial for evaluating daytime hypersomnolence.
- STOP-BANG questionnaire is a validated screening tool for high-risk patients.
- Clinical triad: loud habitual snoring, witnessed apneas, and excessive daytime sleepiness.
- Physical exam: focus on BMI, neck circumference (>40cm), tonsillar hypertrophy, retrognathia.
- Muller’s maneuver assesses upper airway collapsibility and potential obstruction site during wakefulness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

